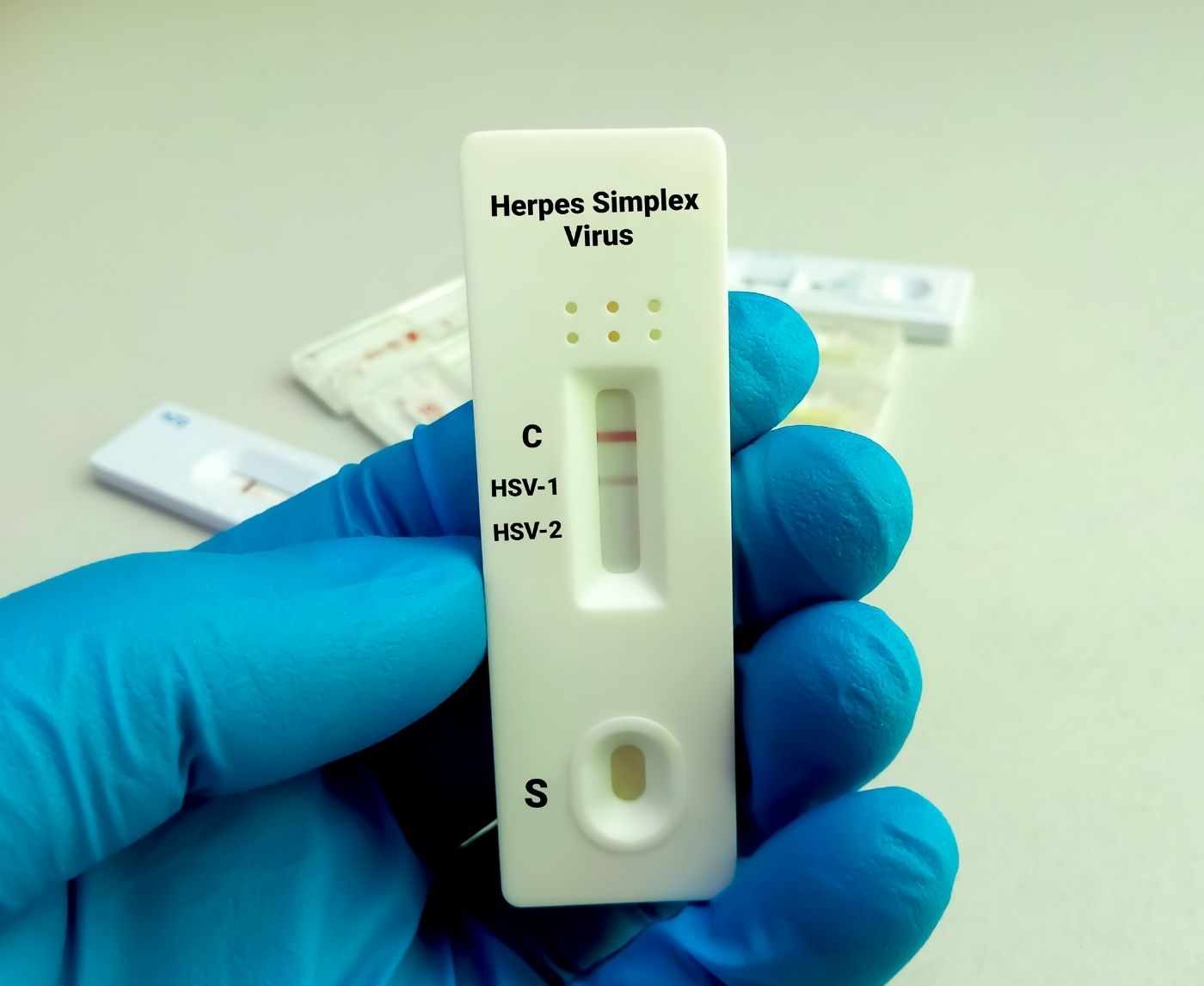
Quick Answer: HSV-2 can be misdiagnosed when symptoms are guessed without testing, when blood tests are used in the wrong situation, or when people test too early and trust a low positive or false negative result too quickly. The most reliable next step depends on whether you have visible sores, when the possible exposure happened, and whether confirmatory testing is needed.
Why HSV-2 Gets Misdiagnosed in the First Place
HSV-2 is not hard only because of the virus itself. It is hard because real life is messy. A lot of people never show the classic clusters of blisters that the internet loves to use in every frightening image search, and the CDC says clinical diagnosis can be difficult because many infected people do not have the typical lesions when they are evaluated. When symptoms do show up, they can overlap with friction irritation, razor burn, yeast irritation, folliculitis, hemorrhoids, allergic reactions, or other causes of genital ulcers.
This is where the first big mistake happens: someone looks at a sore, a clinician makes a visual guess, or a patient assumes every sting, itch, or bump must be herpes. That is not how sexual health works. The internet loves to call everything herpes, but real bodies are not that dramatic all the time. Sometimes a person is convinced they have HSV-2 and it turns out to be an ingrown hair. Other times someone dismisses a sore as shaving irritation and misses an actual outbreak.
The second big issue is that people often think “positive is positive” and “negative is negative” without asking what kind of test they had. That sounds logical, but it is not always true. Herpes testing has context, and if you skip that part, you can end up with a label that is incomplete, misleading, or just plain wrong. That is why a calm, evidence-based read of the result matters more than panic.

People are also reading: How Long After Exposure Can Chlamydia Be Detected?
The Test Itself Is Not the Whole Story
One of the most common testing mistakes is using the wrong test for the wrong situation. If you have visible sores or blisters, CDC guidance says the diagnosis should be confirmed with a type-specific virologic test from the lesion, usually a NAAT or culture. In plain language, that means an actual swab from the sore is usually the smartest starting point when symptoms are present.
Blood tests are a different story. They look for antibodies, not the virus itself. That can be useful in certain situations, like if symptoms are recurrent but no lesion is available to swab, if a partner has genital herpes, or if a clinician strongly suspects herpes and wants more information. But CDC does not recommend herpes blood testing for most people without symptoms because wrong results are more likely in low-risk populations.
There is also a quality issue inside blood testing. The FDA warned in 2023 that HSV-2 serologic tests can produce false-reactive results, especially when a person has a low risk of infection, gets tested too soon, or receives a result near the cutoff value. That is exactly why a low positive should not be treated like a dramatic final verdict without context.
A lot of confusion clears up the minute you ask a simple question: was this a swab from a sore, a PCR, a culture, or a blood antibody test? Once you know that, the result starts to make more sense. If you want a private starting point while you sort out next steps, the Genital & Oral Herpes 2-in-1 At-Home Test Kit gives readers a discreet option to begin that process from home.
Timing Mistakes Are a Huge Reason Results Get Misread
Someone has sex on Saturday, starts spiraling on Sunday, and wants a blood test by Tuesday. That instinct is deeply human, but biology is rude like that. Antibody blood tests need time after infection before the body makes enough detectable antibodies, so testing too soon can create a false negative. The FDA specifically notes that testing too soon after infection raises the chance of a false result.
The timing issue works both ways. A lesion swab is usually most useful when the sore is fresh and active. If someone waits until the area is nearly healed, the sample may not capture enough virus, especially with culture-based methods. NHS guidance explains that testing is often done by swabbing a blister or sore, and if no visible sore is there, that changes what testing is possible.
This is why people walk away with opposite stories from the same virus. One person tests negative too early and believes they are clear. Another person gets a low positive blood test after an anxious screening panel and believes their life just exploded. Neither situation should be read in isolation. Timing is not a side detail. It is the frame around the whole picture.
If your brain is stuck in the loop of “I need answers right now,” that makes sense. But herpes testing rewards timing, not urgency. Sometimes the most accurate move is not doing more random testing today. It is choosing the right test at the right moment.
Sample Mix-Ups, Type Confusion, and the HSV-1 vs HSV-2 Problem
Another classic mistake is treating all herpes results like they mean the same thing. They do not. HSV-1 and HSV-2 are related viruses, but they are not interchangeable labels. A person may already carry HSV-1 from oral infection, sometimes from childhood, and then misunderstand later blood work as if it proves a new genital HSV-2 infection. That is one reason type-specific testing matters so much.
Then there is the IgM problem. ASHA notes that IgM tests are not reliable for distinguishing HSV-1 from HSV-2 and can easily create misleading HSV-2 false positives. This matters because people still show up online saying, “My IgM was positive, so I definitely just got herpes.” That is not a safe interpretation.
The emotional cost of this confusion is real. People tell partners things before the diagnosis is stable. They assume cheating, recent transmission, or certainty about timing that the test simply cannot provide. Even NHS guidance reminds readers that herpes testing cannot tell you how long you have had herpes or who you got it from. That one sentence would save a lot of unnecessary relationship damage if more people heard it sooner.
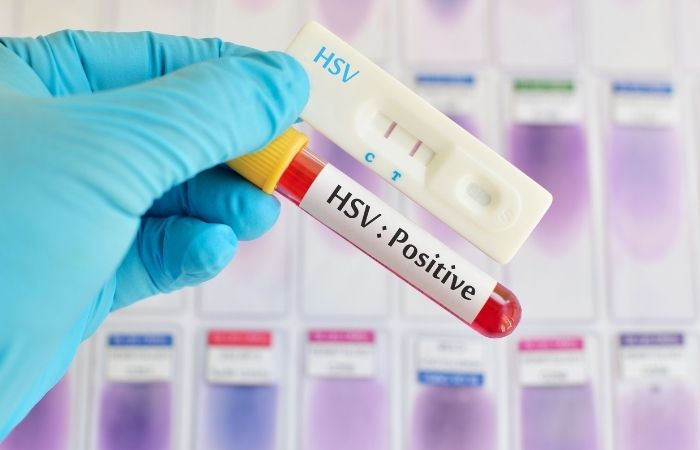
People are also reading: How Long After Exposure Can Chlamydia Be Detected?
Low Positive HSV-2 Blood Tests Are Where a Lot of Panic Starts
This is probably the biggest real-world source of HSV-2 misdiagnosis in asymptomatic people. A person gets screened, often without symptoms, sees a positive HSV-2 IgG result, and assumes the case is closed. But current guidance says false-reactive results are more likely when someone is low risk or when the result is near the cutoff. The FDA warning and USPSTF evidence both point to this problem.
The USPSTF recommends against routine serologic screening for genital herpes in asymptomatic adolescents and adults, including pregnant persons, because the harms of screening can outweigh the benefits in that setting. A big reason is poor positive predictive value in lower-prevalence populations, which is a technical way of saying the test can look more certain than it really is when the person being tested was not a strong fit for screening in the first place.
That does not mean every positive is wrong. It means some positives need a second look before they become part of someone’s identity. If you have a low positive, no symptoms, and no clear exposure history, it is reasonable to ask about confirmatory testing instead of jumping straight to certainty. That is not denial. That is good diagnostics.
What to Do After a Confusing HSV-2 Result
First, match the next step to the situation you are actually in. If you have an active sore, push for a proper lesion test instead of relying only on blood work. If you have no symptoms and got a low positive blood result, ask for the index value and discuss confirmatory testing rather than assuming the first answer is the final one. If you tested too early after an exposure, recognize that a negative may simply be early, not definitive.
Second, do not let shame make the decision for you. Herpes is common, manageable, and surrounded by far more social drama than medical mystery. The goal is not to “win” by proving you do or do not have it in one emotional afternoon. The goal is to get the clearest answer possible using the right method. That may mean retesting, confirming, or comparing a home result with clinic-based follow-up.
A practical next step is to start with privacy and accuracy in mind. You can review testing options at STD Test Kits, use the Herpes 2-in-1 home kit if a discreet at-home option fits your situation, or consider a broader panel like the combo STD home test kits if the issue may not be herpes at all. The point is to stop guessing and move toward a cleaner answer
FAQs
1. Can HSV-2 really be misdiagnosed?
Yes. HSV-2 can be misdiagnosed when symptoms are judged visually without testing, when blood tests are used in the wrong setting, or when low-positive results are treated as definitive without confirmation. The CDC and FDA both acknowledge limits in herpes testing, especially around blood tests and timing.
2. What is the most common HSV-2 testing mistake?
One of the biggest mistakes is relying on a blood test alone when a fresh lesion is available to swab. Another common problem is overreacting to a low-positive HSV-2 IgG result without confirmatory testing.
3. Can a herpes blood test be falsely positive?
Yes. FDA warns that HSV-2 serology can produce false-reactive results, especially in people with low risk, people tested too early, and people with results near the cutoff. That is why context and confirmatory testing matter.
4. Can a herpes test be falsely negative?
Yes. A blood test can be negative if it is done before antibodies have developed, and a lesion test can miss infection if the sore is old, dry, or healing. A negative result always has to be read alongside timing and symptoms.
5. Is a swab better than a blood test for herpes?
If you have a visible sore, a swab-based lesion test is usually the better first move because it looks for the virus directly. Blood tests can help in selective situations, but they are not the ideal choice for every person or every moment.
6. Does a low positive HSV-2 result mean I definitely have herpes?
Not necessarily. A low positive can sometimes be a false-reactive result, particularly in asymptomatic people or low-risk settings. That kind of result often deserves a deeper review rather than immediate certainty.
7. Can doctors mistake something else for herpes?
Absolutely. Ingrown hairs, razor burn, friction irritation, folliculitis, allergic reactions, yeast-related irritation, and some other causes of genital ulcers can resemble herpes. That is why guessing from appearance alone can go sideways fast.
8. Can herpes testing tell me who gave it to me or when I got it?
No. Even when testing confirms herpes, it usually cannot tell you exactly when the infection was acquired or who transmitted it. That limitation is important because people often try to use test results as relationship timelines when the science cannot support that.
9. Should people without symptoms get screened for HSV-2?
In most situations, routine screening of asymptomatic people is not recommended. USPSTF recommends against routine serologic screening in asymptomatic adolescents and adults because of the balance of harms and the risk of false positives.
10. What should I do if my HSV-2 result feels confusing?
Pause before making big conclusions. Find out what kind of test you had, how long after exposure it was done, whether there were symptoms to swab, and whether the result was low positive or clearly positive. Then talk through confirmatory testing or retesting based on the actual situation.
How to Protect Yourself From an HSV-2 Misdiagnosis
The smartest way to avoid misdiagnosis is to stop treating herpes testing like a single yes-or-no event. Think of it more like a decision tree. Do you have sores right now? How long since exposure? Was this a blood test or a swab? Was the result clearly positive, low positive, or negative despite symptoms? Those details are not technical trivia. They determine whether the result is trustworthy.
A good rule is simple: visible lesion means swab if possible, recent exposure means be careful about early negatives, and low-positive blood results deserve context. Also, do not lean on IgM as the thing that settles the whole story. That test has caused too much confusion for too many people. Better science usually feels less dramatic and more annoyingly careful, which is exactly why it is better science.
The good news is that confusion is fixable. Most herpes testing mistakes come from rushing, mixing up test types, or reading a borderline result like a verdict from heaven. Once you know the weak spots, you can ask sharper questions, get better follow-up, and make decisions with a lot less fear and a lot more clarity.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it “came back.” In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC STI Treatment Guidelines: Genital Herpes
2. CDC: Screening for Genital Herpes
3. FDA: HSV-2 Tests for Genital Herpes Can Produce False-Reactive Results
4. USPSTF: Serologic Screening for Genital Herpes Infection
6. American Sexual Health Association: Herpes Testing
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Dr. Riley Santos, MPH | Last medically reviewed: March 2026
This article is for informational purposes and does not replace medical advice.