Last updated: April 2026
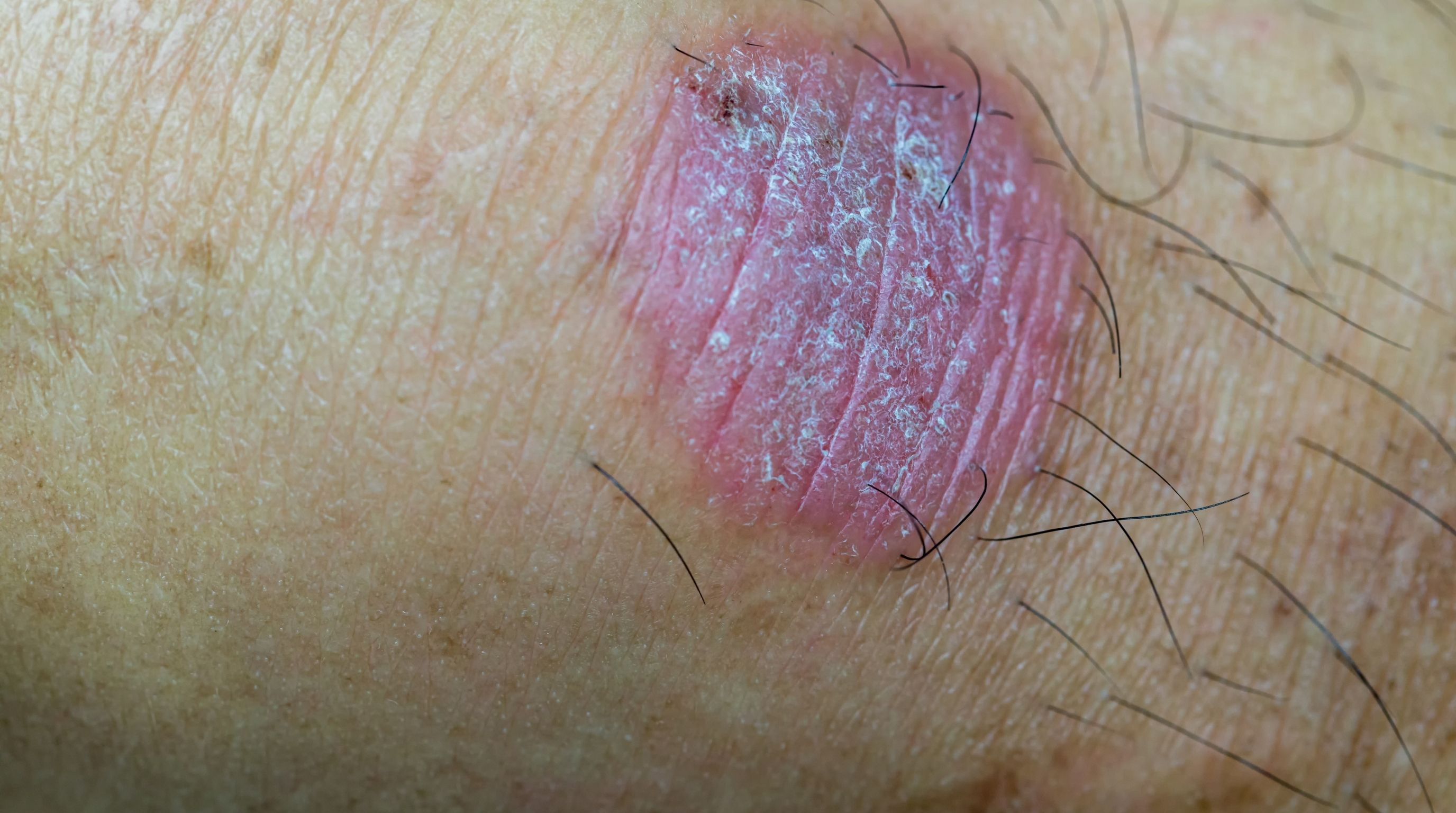
A chancre is a round, firm, painless ulcer with raised, defined edges and a clean base, ranging from 1 to 2 centimeters in diameter. It is the first visible sign of syphilis, the point at which Treponema pallidum, the bacterium that causes the infection, has entered the body and triggered a localized immune response at the site of contact. The painless part is what throws people.
You're looking for a sore that doesn't hurt the way you'd expect a wound to hurt. It appears between 10 and 90 days after exposure, with the average onset at 21 days, and heals on its own in 3 to 6 weeks. That disappearance means nothing. The infection does not leave with the sore.
People are also reading: Herpes Isn’t That Simple: The Truth Behind the 3 M’s Rule
What a Syphilis Chancre Actually Looks Like
The clinical description of a chancre is a painless ulcer with an indurated border, meaning the edges feel firm and hardened, slightly raised above the surrounding skin, almost like a rim around a shallow crater. The base of the ulcer is smooth rather than ragged, without pus or heavy discharge, though it oozes a small amount of clear or slightly yellowish fluid containing live bacteria. The surface itself looks flat or slightly sunken. It is not blistered, not crusty, and not fluid-filled the way a herpes sore is.
Size matters here: chancres fall in the 1 to 2 centimeter range, roughly the size of a pencil eraser. They can be smaller, a few millimeters, or, less commonly, larger. There is usually one, though NCBI's clinical review of syphilis notes that multiple chancres occur more frequently in people with HIV. The sore appears at exactly the site where the bacteria entered your body, which is why chancres are found on the penis, scrotum, vulva, vaginal walls, cervix, anus, rectum, lips, or mouth, depending on what kind of sexual contact occurred.
What makes chancres genuinely difficult to catch is the combination of painlessness and location. A chancre inside the vagina, on the cervix, inside the rectum, or under the foreskin can be present for its entire 3 to 6 week lifespan without the person ever seeing or feeling it. Because Treponema pallidum triggers an inflammatory response in regional lymph nodes as it disseminates from the initial infection site, the first sign people notice is not the sore itself but slightly swollen, rubbery lymph nodes near the groin, also painless, and easily mistaken for nothing.
The honest reality is that visual diagnosis of a chancre, by yourself, from a photo, or by image-matching on Google, is unreliable. The appearance overlaps with too many other conditions. What you need is a test, not an image match. The table above describes the classic presentation, but atypical chancres exist, and the only way to confirm syphilis is serology.
Is This a Chancre, Herpes, or Something Else? Here's How to Tell Them Apart
The question most people are actually asking when they search for chancre information is: could this be something less serious? The conditions that look like chancres are common, and the distinctions matter, not to avoid testing, but to understand what you're looking at.
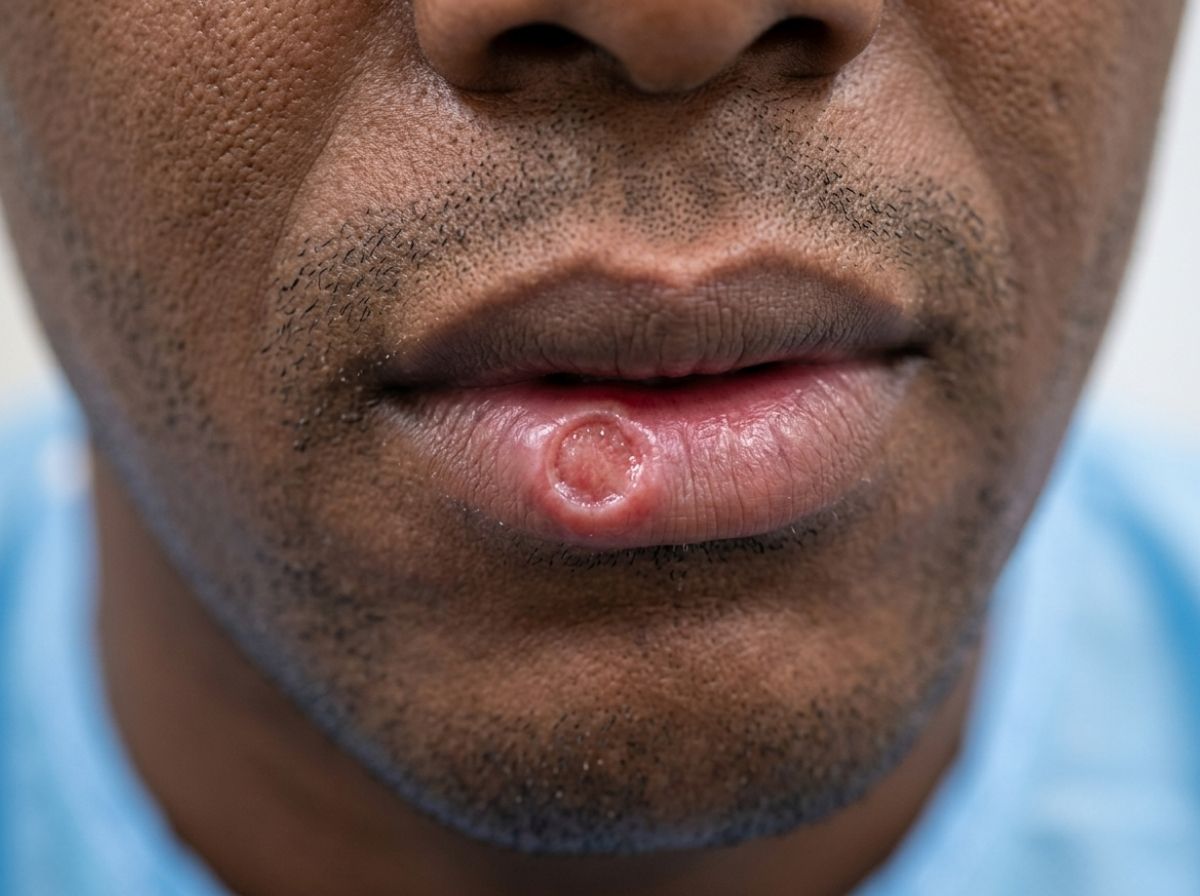
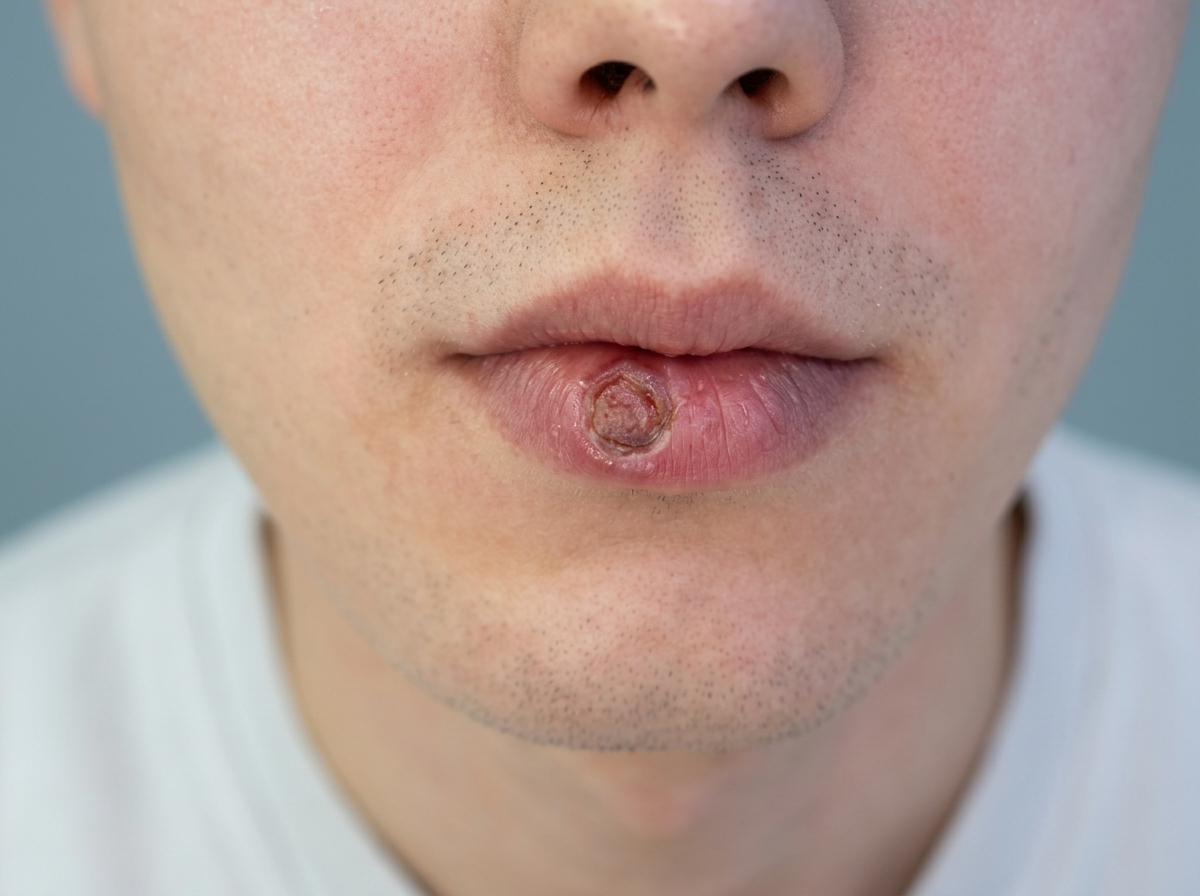
The most important comparison is chancre versus herpes sore. Herpes lesions from HSV-1 or HSV-2 begin as small, fluid-filled blisters clustered together, which then rupture to form shallow, raw-looking ulcers. They hurt, during a first outbreak, the pain is pronounced and is accompanied by a prodrome of tingling or burning before the blisters appear, plus fever, muscle aches, and swollen glands in some cases. A herpes outbreak involves several small sores in a cluster rather than one larger, isolated ulcer.
The edges are irregular and look torn, rather than the clean, firm rim of a chancre. Pain is the single most useful distinguishing feature: if the sore hurts when you sit down, when fabric brushes it, or when anything makes contact with it, that is more consistent with herpes than syphilis. A chancre that is genuinely painless is not herpes.
An ingrown hair or folliculitis can look like an early chancre, a small, raised bump with a defined border in the pubic area. The differences: folliculitis has a white or yellow pustule at the center, is surrounded by warmth and inflammation, and resolves within a few days.
A chancre has no white tip, does not feel warm and inflamed, and does not resolve within days. A razor bump or contact irritation clears within 24 to 72 hours and appears across a shaved area rather than as one isolated sore. A traumatic ulcer from friction during sex heals within a week and correlates directly with physical trauma. A chancre persists for 3 to 6 weeks regardless of what you do to it.
None of these alternatives can be confirmed or ruled out by looking. A painless, firm, persistent ulcer warrants a syphilis test even if you have a competing explanation ready. The competing explanation might be correct, but you won't know without testing, and syphilis caught at the primary stage is one of the most treatable infections that exists.
When and Where Chancres Appear, and Why Timing Matters So Much
The incubation period for syphilis runs from 10 to 90 days between exposure and the appearance of the first sore, with the average onset at 21 days. That variability is one of the reasons people struggle to connect a chancre to a specific encounter. If a sore appeared 6 weeks after a sexual encounter you were uncertain about, you might reasonably not associate the two, especially if there were other encounters in between. The timeline doesn't always feel obvious from the inside.
This matters directly for testing. Syphilis is detected through blood tests that identify the antibodies your immune system produces in response to Treponema pallidum. In the first week or two after a chancre appears, blood tests can return a false negative, not because the test is faulty, but because the immune system has not yet produced a detectable level of antibodies. According to CDC guidance on syphilis testing, the reliable testing window is 6 weeks after exposure. A negative result before that point does not confirm you are clear. A negative result at or after 6 weeks does.
If you are looking at a sore right now and trying to work out when you were exposed: the sore has likely been present for anywhere from a few days to a few weeks. Add that to the 10 to 90 day incubation window, and your most probable exposure falls within that range before the sore appeared. If your last sexual contact was well over 90 days before the sore appeared, syphilis is less likely, but atypical incubation occurs, and testing is still the right move when any doubt exists.
Chancres in women deserve specific attention because they are so consistently missed. A chancre on the cervix or inside the vaginal walls produces no external sign, causes no pain, and heals within 3 to 6 weeks without the person knowing it existed. Because Treponema pallidum enters a dissemination phase during primary infection, spreading through the bloodstream while the visible sore is still present, the damage begins before a single symptom appears.
This is why syphilis in women is diagnosed later on average than in men, and why routine testing matters regardless of whether anything has been noticed.
People are also reading: No Pain, Just Discharge, Is It Chlamydia or Something Else?
What Happens If You Ignore a Chancre and Wait for It to Heal
The chancre heals on its own. That is not a reason to wait, it is one of the most biologically misleading things about syphilis. The visible sore disappears in 3 to 6 weeks and the skin returns to normal. Nothing hurts. Most people who didn't recognize the sore for what it was conclude at this point that whatever it was, it resolved. It did not. Treponema pallidum is still present, still replicating, and now more widely distributed through the body, including the bloodstream and cerebrospinal fluid, even with no external evidence.
What follows the healed chancre, in untreated infection, is the secondary stage. This develops 2 to 8 weeks after the chancre disappears, as the bacteria reach high enough systemic concentrations to trigger a broader immune response. Secondary syphilis produces a non-itchy rash that characteristically appears on the palms and soles of the feet, a presentation specific enough that it is used as a clinical indicator, alongside fever, fatigue, muscle aches, sore throat, and swollen lymph nodes throughout the body. Mucous patches form inside the mouth, and flat wart-like growths can appear in the groin. These symptoms also resolve without treatment, after which syphilis enters the latent stage: months or years of no visible symptoms, while the bacteria continue their slow progression through internal structures.
Tertiary syphilis develops in a subset of untreated cases, typically 10 to 30 years after the initial infection. At this stage the damage is serious and frequently irreversible: cardiovascular involvement, including aortic aneurysm, neurological deterioration including dementia and loss of motor coordination, and gummatous lesions, granulomatous growths driven by chronic immune activation, affecting bones, skin, and organs. None of this is inevitable. Every stage of that progression is prevented by identifying and treating the infection at the primary stage, when a sore is still present and the bacterial load is still localized.
There is also the transmission consideration. The fluid that oozes from a chancre contains live Treponema pallidum. Skin-to-skin contact with that sore during sexual activity transmits the infection directly, unlike STIs that require internal fluid exchange, syphilis at the primary stage transmits on surface contact with the lesion. Condoms reduce but do not eliminate this risk if the sore falls outside the area the condom covers. Sexual contact while a chancre is present and untested puts partners at direct risk of primary syphilis infection.
How to Test for Syphilis After Seeing a Potential Chancre
The standard test for syphilis is a blood test. It does not require a swab of the sore, a urine sample, or any examination of the lesion itself, a finger-prick blood sample is enough to detect the antibodies your immune system produces in response to Treponema pallidum. At-home syphilis tests use this method and deliver results in 15 minutes.
The exact timing to follow: test from 6 weeks after the exposure you believe caused the sore. If the sore has been present for several weeks and you have a clear sense of when the exposure occurred, testing now is appropriate. If the sore appeared very recently and your exposure was less than 6 weeks ago, a negative result at this point is not fully reliable, the immune system has not yet produced detectable antibodies. Test now for a baseline, and retest at the 6-week mark from exposure if the first result is negative. A positive result at any point is actionable immediately.
A negative result means no detectable antibodies to Treponema pallidum were found at the time of testing. Before 6 weeks, this can mean the infection is present but not yet detectable, which is why retesting at the window matters. At or after 6 weeks, a negative result is reliable. A positive result means syphilis antibodies were detected; follow up with a healthcare provider for confirmatory testing. Syphilis at the primary stage is fully curable with prompt treatment.
If the circumstances of your exposure make it worth ruling out additional infections alongside syphilis, HIV, gonorrhea, herpes, hepatitis B and C, the 7-in-1 Complete At-Home STD Test Kit covers all of those in one package. If syphilis is your primary concern right now, the Syphilis At-Home STD Test Kit gives you a focused result with 99% accuracy from a simple finger-prick sample.
What the Syphilis Landscape Looks Like Right Now, And Why This Matters
If you've found a sore and are wondering whether syphilis is even a realistic possibility for someone like you, it is more realistic than it used to be, and across a wider population than is commonly understood. Provisional CDC surveillance data released in September 2025 show that while primary and secondary syphilis cases declined by 22% in 2024 compared to 2023, the second consecutive year of decreases after more than two decades of sustained increases, the overall burden remains substantial. The 2023 total of over 209,000 syphilis cases was the highest annual figure in the United States since 1950, and more than 2.2 million STIs were reported in 2024 across all categories.
Perhaps more relevant to how you're reading this: a study published in the American Journal of Preventive Medicine in April 2025, analyzing electronic health records from nearly 57 million US adults, found that syphilis incidence declined among historically high-burden groups while rising among people without typical risk factors, those not using PrEP, not living with HIV, and not reporting behaviors previously associated with STI acquisition. In plain terms: the people who don't consider themselves at risk are increasingly the ones being diagnosed. Being sexually active with new or multiple partners places you in the exposure window regardless of how you identify your risk level.
Congenital syphilis, transmission from mother to baby during pregnancy, increased for the 12th consecutive year in 2024, reaching nearly 4,000 cases, a rise of nearly 700% since 2015 according to the CDC's provisional data. That figure exists almost entirely because primary syphilis went undetected: chancres that were missed, misidentified, or never tested. Testing at the primary stage, when a sore is still present, is the exact intervention that prevents that downstream harm.
Partner Notification and What Comes Next
If your test returns positive, the next step is determining who needs to know. For a primary-stage infection, partner notification covers the 90 days prior to your positive result, the window during which transmission from a chancre is most probable. For secondary-stage cases, the lookback period extends to 6 months. For latent syphilis of unknown duration, the recommended window extends to a year or more.
Telling a partner you've tested positive is uncomfortable. The realistic framing to offer them: syphilis is bacterial and fully treatable at every stage except tertiary, and your notification gives them the opportunity to test and treat before any complications develop. Many sexual health clinics and local health departments offer anonymous partner notification services, they contact partners on your behalf without identifying you. That option is available and worth using if a direct conversation feels unmanageable.
Avoid sexual contact from the point of a positive test until both you and any partners have been confirmed clear. The reason is biological, not precautionary: a person in the primary or secondary stage of syphilis is actively infectious, and the risk of transmission persists even with condom use if the sore falls in an area the condom does not cover.
Follow-up blood testing after treatment, at 6 and 12 months, confirms that antibody levels are declining as expected, which is how providers verify the treatment worked. Syphilis does not confer immunity; reinfection from a new exposure is possible after successful treatment, which is why ongoing routine testing makes sense if re-exposure is plausible.
FAQs
1. What does a syphilis chancre feel like when you touch it?
The defining feature is firmness. The border of a chancre feels indurated, harder and more raised than the surrounding skin, like a firm rim around a slightly sunken center. The sore itself is painless when touched, which is what distinguishes it from most other genital ulcers. If pressing on it causes significant pain, herpes or a traumatic sore is more consistent with that presentation.
2. Can a chancre appear inside the vagina or rectum where you can't see it?
Yes, and this is a common presentation. Internal chancres on the cervix, inside the vaginal walls, inside the rectum, or under the foreskin go unnoticed throughout their full 3 to 6 week lifespan in many cases. Treponema pallidum disseminates through the bloodstream during this period regardless of whether the sore is visible, which means the infection is active and transmissible even when there is nothing to see.
3. If the sore is painful, does that rule out syphilis?
Not entirely. The classic chancre is painless, and that is the most common presentation. However, CDC treatment guidelines note that chancres can be painful in atypical presentations and particularly in anal locations. Multiple chancres are also more likely to cause discomfort. A painful genital ulcer still warrants testing for syphilis alongside herpes and other possibilities, pain level alone is not a reliable way to rule it out.
4. How long does a chancre last before it heals?
Between 3 and 6 weeks, after which it heals without treatment and without leaving a visible mark in most cases. This spontaneous resolution is consistently misread as the infection clearing. It does not clear. The bacteria remain present, the disease progresses to secondary syphilis 2 to 8 weeks after the chancre disappears, and then enters a latent phase with no visible symptoms, all while the infection continues.
5. Can I test for syphilis right now if I think I have a chancre?
Yes, and you should. If your exposure was 6 or more weeks ago, the result is reliable. If the sore appeared recently and your exposure was less than 6 weeks ago, a negative result at this point may reflect a window period false negative rather than a true absence of infection. Test now for a baseline, and retest at the 6-week mark from exposure if the first result is negative.
6. Can a chancre heal without treatment and not come back?
The visible sore heals on its own whether or not any treatment is received. The infection does not. The disease moves from primary to secondary stage, producing a rash, fever, and swollen lymph nodes, and then enters a latent phase with no symptoms. Tertiary syphilis, which causes serious organ damage, can develop years or decades later in untreated cases. The healing of the chancre is not recovery.
7. Is a chancre always on the genitals?
No. Chancres appear at the site where Treponema pallidum entered the body, which depends on the type of sexual contact. Oral sex can produce chancres on the lips, inside the mouth, or on the tongue. Anal sex produces them in or around the rectum. A sore on the lip or inside the mouth that is painless, firm-edged, and not healing after 7 to 10 days belongs on the list of things to test for.
8. Can I have syphilis without ever seeing a chancre?
Yes. People with internal chancres, on the cervix, vaginal walls, inside the rectum, go through the entire primary stage without seeing or feeling anything. For these individuals, the first detectable sign of infection is the secondary stage rash or systemic symptoms that appear weeks after the chancre has already healed. This is one of the clearest reasons routine testing matters independently of whether any symptoms have appeared.
9. Does a syphilis test check the sore itself, or is it a blood test?
Standard syphilis testing is a blood test that detects antibodies your immune system produces in response to Treponema pallidum. At-home tests use a finger-prick blood sample. Swab-based direct detection using darkfield microscopy exists in clinical settings but is not the routine approach. The blood test is the standard method and is what at-home kits use.
10. What happens if I go to a doctor with a suspected chancre?
A clinician will examine the sore, take a sexual history, and order serologic blood testing for syphilis. Depending on the presentation, they will also test for other STIs that co-occur with syphilis at higher rates, including HIV, gonorrhea, and herpes. If syphilis is confirmed, appropriate treatment is prescribed. At the primary stage, outcomes with prompt treatment are excellent.
If There's a Sore and You're Not Sure, Test Today
A sore that appeared without obvious cause, doesn't hurt the way a wound should hurt, and hasn't resolved within a few days deserves more than a wait-and-see approach. It might be a chancre. It might be something far less significant. The only way to know is a test, and at the primary stage, syphilis is among the most treatable infections that exists. What makes it dangerous is not the biology but the gap between a sore appearing and a person doing something about it.
The Syphilis At-Home STD Test Kit from STD Test Kits delivers a result from a simple finger-prick blood sample with 99% accuracy in 15 minutes, no clinic appointment, no waiting room, no conversation with anyone required. If the exposure warrants a broader screen, the 7-in-1 Complete At-Home STD Test Kit covers syphilis, HIV, gonorrhea, herpes HSV-2, hepatitis B, and hepatitis C in one package. For a complete panel that adds HSV-1, trichomoniasis, and HPV, the Women's 10-in-1 At-Home STD Test Kit covers all of those in a single test.
Testing is the step that turns uncertainty into a clear answer and a clear next move. Visit STD Test Kits to find the right test for your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, About Syphilis, Stages, Symptoms, and Testing
2. NCBI StatPearls, Syphilis: Clinical Review and Management
3. CDC MMWR, Laboratory Recommendations for Syphilis Testing, United States, 2024
4. CDC, Sexually Transmitted Infections Surveillance, 2024 (Provisional)
6. Cleveland Clinic, Syphilis: Cause, Symptoms, Diagnosis, Treatment and Prevention
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.