Last updated: April 2026
If you're pregnant and just got a trichomoniasis diagnosis, the first thing running through your mind is probably your baby, not yourself. That's completely normal. The good news is that trich passing to a newborn during vaginal delivery is uncommon, and when it does happen, it is treatable. This article explains exactly how transmission works, what doctors look for in a newborn who may have been exposed, and, most importantly, how testing and treatment before labor can eliminate the risk entirely.
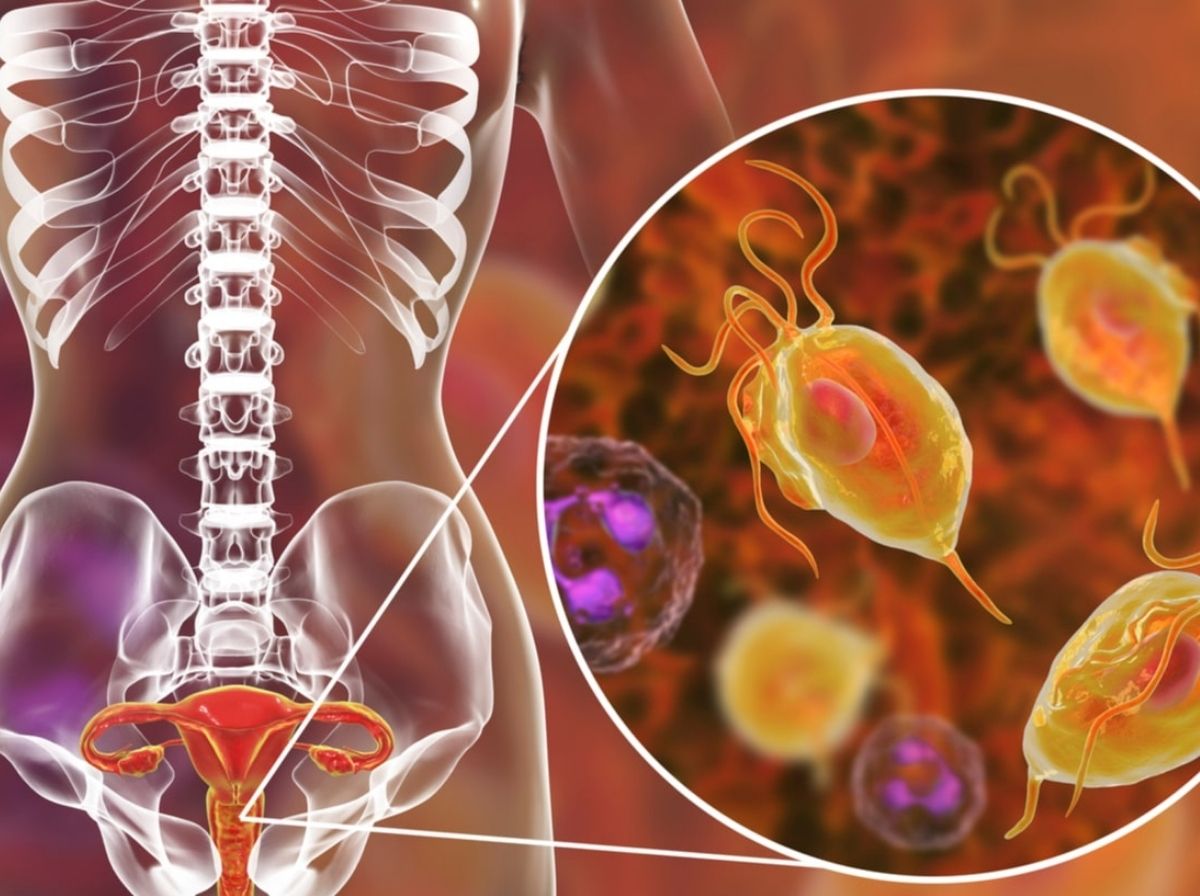
Yes, it is possible for a baby to contract trichomoniasis during birth, but it is genuinely rare. The parasite Trichomonas vaginalis lives in the vaginal tract, and when a baby passes through an infected birth canal during vaginal delivery, contact with infected secretions can, in some cases, lead to neonatal infection. Most newborns who are exposed do not become infected, and the ones who do are treatable. But the biology behind how and why transmission sometimes occurs is worth understanding, especially if you're currently pregnant and trich-positive.
People are also reading: Trichomoniasis Symptoms During Pregnancy, Or Why You Probably Won't Have Any
How Does Trichomoniasis Spread from Mother to Baby?
Trichomoniasis is caused by a single-celled parasite called Trichomonas vaginalis. In adults, it spreads through skin-to-skin contact during sexual activity, primarily vaginal sex, though contact with infected genital secretions is the key mechanism. During pregnancy, the parasite establishes itself in the vaginal tract, often without causing noticeable symptoms. According to the CDC, roughly 70–85% of people with trichomoniasis have no symptoms at all, which is part of what makes it so likely to go undetected during pregnancy.
When a baby is born vaginally, it travels through the birth canal and comes into direct contact with vaginal secretions. If those secretions contain T. vaginalis, there's a window for exposure. The critical distinction here is exposure versus infection: most exposed babies clear the parasite on their own or never develop a sustained infection. The newborn immune system, while still developing, manages to resist the parasite in the majority of cases. Perinatal transmission, meaning infection passed from mother to baby around the time of birth, is documented in medical literature but categorized as uncommon by both the CDC and published clinical guidelines.
One reason transmission remains relatively rare is timing. The parasite needs sustained contact with mucosal surfaces to establish infection. The brief passage through the birth canal doesn't always provide enough time or exposure for the parasite to take hold. Additionally, babies born at term to mothers who received treatment during pregnancy and cleared the infection before labor face essentially no transmission risk at all; the parasite simply isn't there to pass on.
What Are the Risk Factors for Transmission?
Not all pregnancies with trichomoniasis carry the same transmission risk. Several factors affect how likely it is that an infection passes to the baby during delivery. The most significant is whether the infection is active and untreated at the time of labor. A pregnant person who received treatment and cleared the infection before 37 weeks faces a fundamentally different situation than someone who goes into labor with an active, untreated infection.
Preterm birth is another factor worth understanding. A systematic review published in PMC on neonatal trichomoniasis found that the majority of documented neonatal infections occurred in preterm infants, nine out of eleven reported cases in the review were preterm births. This matters for two reasons: first, trichomoniasis itself is associated with a higher risk of preterm labor, which means the two conditions can co-occur; second, premature babies have less developed immune defenses, making them more vulnerable if exposure does occur.
Untreated infection at delivery also means higher parasite load in vaginal secretions, which increases the likelihood of exposure leading to actual infection. A person who has been symptomatic but undiagnosed through the entire pregnancy, which happens because trichomoniasis is not routinely screened for at standard OB appointments, is at greater risk of transmitting the infection than someone who was diagnosed and treated early. This is one of the strongest arguments for proactive testing during pregnancy, particularly for anyone who has had unprotected sex, a new partner, or symptoms such as unusual discharge or odor during the pregnancy.
For more information on how trichomoniasis can negatively impact your pregnancy, make sure to read our guide: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
What Happens If a Baby Is Infected?
When neonatal trichomoniasis does occur, the symptoms are not what most people would expect. Because T. vaginalis typically causes genital infections in adults, the assumption is that a newborn would show similar genital symptoms. In reality, the most documented site of neonatal infection is the respiratory tract, not the genitalia. This happens because during delivery, babies inhale small amounts of secretions, including any organisms present in the birth canal, as they take their first breaths.
The PMC systematic review on neonatal trichomoniasis found that respiratory symptoms were the most common presentation in documented cases. Affected newborns showed signs including breathing difficulties, periods of abnormal heart rate, nasal discharge, and in more serious cases, pneumonia. These symptoms often look indistinguishable from other neonatal respiratory conditions, which is one reason trichomoniasis in newborns is frequently missed or diagnosed late. In several documented cases, infants were initially treated for sepsis or other infections before trichomoniasis was identified as the actual cause.
In female infants, the urogenital tract may become infected, occasionally manifesting as vaginal discharge during infancy. This is uncommon and usually goes away with treatment. Infection disseminating beyond the respiratory and genital tracts is even more uncommon, yet recorded in medical literature. A 2018 case report in Clinical Infectious Diseases told the story of a premature baby who got a brain abscess from T. vaginalis. This was an unusual case that showed how far the parasite can travel when the defenses of a newborn are very weak. That level of severity is very rare, but it shows why finding and treating maternal trichomoniasis before delivery is not just a precaution; it is important.
People are also reading: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
How Do Doctors Test and Treat Trichomoniasis in a Newborn?
If a baby is born to a mother who has an active trichomoniasis infection, the delivery team will keep an eye out for signs of infection in the days after the baby is born. There is no standard universal screening protocol for newborns of trich-positive mothers; however, any respiratory symptoms, abnormal discharge, or other indicators will necessitate further investigation. To find the parasite directly, doctors usually do lab tests on a newborn's secretions from the respiratory tract, nasal passages, or genital area. They do this by looking at them under a microscope or by growing them in a culture.
Treatment in confirmed neonatal cases uses the same antibiotic that treats trichomoniasis in adults, adjusted for the baby's weight and age. Medical literature consistently reports that respiratory status improves after treatment and the parasite becomes undetectable in subsequent specimens. The keyword here is "confirmed", treatment is not given prophylactically to every baby born to an infected mother, only to those showing signs of actual infection after testing confirms the parasite is present.
The most important thing to understand about neonatal trichomoniasis from a practical standpoint: it is treatable and, when caught, responds well to appropriate antibiotic therapy. The bigger concern isn't what happens if a baby does get it, it's making sure the infection isn't silently present in the mother during delivery in the first place, which brings everything back to testing during pregnancy.
Testing for Trichomoniasis During Pregnancy: When and Why It Matters
Here's something most people don't realize until they're already pregnant: trichomoniasis is not part of standard prenatal STI screening in the United States. Your OB will typically test for chlamydia, gonorrhea, syphilis, HIV, and hepatitis B at your first prenatal visit, but trich is not on that routine list unless you have symptoms or are considered high-risk. According to the CDC's STI Treatment Guidelines, routine screening for asymptomatic pregnant individuals has not been established as having a clear benefit, though symptomatic pregnant people should be tested and treated regardless of trimester.
What this means in practice is that a significant number of pregnant people are carrying trichomoniasis without knowing it. The CDC estimates over two million trichomoniasis infections in the US, with the majority of infected individuals experiencing no symptoms. During pregnancy, discharge and vaginal changes are already common, making it even easier to dismiss symptoms that might actually be trich. If you have had a new partner during pregnancy, a partner who hasn't been tested, or you've noticed unusual discharge, odor, or irritation, asking specifically to be tested for trichomoniasis is completely reasonable and worth doing.
If you want to test from home, the Trichomoniasis At-Home STD Test Kit (98%+) available at STD Test Kits gives you results without a clinic visit. Testing from home is discreet, fast, and takes the guesswork out of whether you need to follow up with your doctor. For trichomoniasis, the testing window is 5–28 days after exposure. This reflects the incubation period of the parasite, meaning you can test reliably once symptoms have had time to develop.
If you believe you were recently exposed and your result is negative, retesting at the end of the 28-day window confirms a true negative. For more information on trichomoniasis symptoms and treatment, and whether or not you can treat it during your pregnancy, make sure to read this guide: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
What Can a Pregnant Person Do to Reduce the Risk?
The clearest answer to "how do I make sure my baby doesn't get trich at birth" is also the most straightforward: know your status before labor begins and treat any active infection. If trichomoniasis is identified and treated during pregnancy, and the infection is confirmed cleared before delivery, the parasite is simply not present to transmit. The transmission risk at birth drops to essentially zero when there's no active infection.
Testing during the second trimester, or earlier if symptoms appear, gives the most time to treat and confirm clearance before labor. Treatment during pregnancy is safe and effective, and clearing the infection before 37 weeks is considered ideal. Even treatment closer to the due date still reduces parasite load and lowers transmission risk, though earlier is always better when it comes to protecting both mother and baby.
Partner treatment matters here too. One of the most common reasons trichomoniasis returns after treatment is reinfection from an untreated partner. If you treat during pregnancy but your partner doesn't, the infection can come back before delivery, putting you right back where you started. Both partners should be tested and treated at the same time, and sexual activity should pause until both confirm clearance. This is not just about the relationship, it's directly about your baby's health at delivery.
For those who want to be thorough, the Women's 10-in-1 At-Home STD Test Kit covers trichomoniasis alongside nine other infections including chlamydia, gonorrhea, syphilis, HIV, hepatitis B and C, both herpes strains, and HPV, a complete picture for anyone wanting to know their full STI status during pregnancy. Testing is empowerment, not alarm. Knowing where you stand is how you protect both yourself and your baby.
Does a C-Section Eliminate the Transmission Risk?
It's a logical question: if the birth canal is the route of exposure, does skipping it entirely remove the risk? In theory, yes, a cesarean delivery means the baby never passes through the vaginal tract, which eliminates the primary transmission pathway for T. vaginalis. But that theoretical protection comes with an important clinical caveat: no guidelines recommend cesarean delivery as a strategy for preventing trichomoniasis transmission, and no obstetrician would suggest one for this reason alone.
The reason is straightforward: transmission during birth is already uncommon, and cesarean delivery carries its own meaningful risks for both mother and baby, longer recovery, surgical complications, and implications for future pregnancies. Recommending major abdominal surgery to prevent an infection that responds reliably to a course of antibiotics would be a significant mismatch between intervention and risk. The far more appropriate response to a trichomoniasis diagnosis during pregnancy is treatment, confirmation of clearance, and proceeding with the planned delivery.
If a cesarean is already planned for other obstetric reasons, it may incidentally reduce the trich transmission risk, that's a secondary benefit, not a justification. For the vast majority of pregnant people with trichomoniasis, the path forward is straightforward: test, treat, confirm the infection is gone, and deliver as planned. The goal is an infection-free birth canal, not a different route around it.
The Bigger Picture: Trichomoniasis and Pregnancy Outcomes Beyond Birth Transmission
For most people who test positive during pregnancy, the immediate fear is passing the infection to the baby at delivery. That's a real concern worth addressing, but it's not the only way trichomoniasis affects pregnancy outcomes. A meta-analysis published in PMC found that trichomoniasis in pregnant women was independently associated with preterm birth, premature rupture of membranes, and low birth weight, three complications that carry their own serious downstream risks for the newborn, regardless of whether any transmission occurs at delivery. Preterm birth increases the risk of neonatal respiratory distress. Low birth weight is associated with higher infant mortality. Both can occur without any direct infection of the baby.
The mechanism isn't fully understood, but the leading hypothesis is that the inflammatory response T. vaginalis triggers in the vaginal tract can weaken the membranes surrounding the fetus, increasing the risk of early rupture and labor. There are also documented cases of ascending infection, the parasite traveling upward into the uterus, though this is less common than cervicovaginal infection. The practical implication is that trichomoniasis during pregnancy isn't a problem that stays contained to the birth canal. It can influence the course of the entire pregnancy.
A 2025 study published in Frontiers in Public Health on the global burden of trichomoniasis identified inadequate screening as one of the key drivers of ongoing harm, particularly in women of reproductive age. In the United States, trichomoniasis is not a reportable disease, which means the actual infection burden is almost certainly higher than surveillance data captures. For pregnant people specifically, that screening gap is consequential: an infection that isn't diagnosed can't be treated, and the pregnancy and delivery risks outlined in this article compound the longer it goes undetected. Testing during pregnancy isn't a precaution for edge cases, it's how you get ahead of a very common infection that the standard prenatal panel won't catch.

People are also reading: Can Trichomoniasis Cause a Miscarriage or Preterm Birth?
FAQs
1. Can a baby get trichomoniasis if I have a vaginal delivery?
Yes, it's possible, though it's genuinely uncommon. The baby passes through the birth canal and comes into contact with vaginal secretions, if those secretions contain Trichomonas vaginalis, exposure can occur. Most exposed babies don't develop a sustained infection, and those that do are treatable with antibiotics. The best way to prevent this entirely is to test and treat during pregnancy so the infection is cleared before labor begins.
2. What are the signs of trichomoniasis in a newborn?
The most common presentation in documented neonatal cases is respiratory symptoms, breathing difficulty, nasal discharge, and in more serious cases, pneumonia. This happens because babies inhale birth canal secretions during delivery. Female infants may also develop vaginal discharge. These symptoms often look similar to other neonatal conditions, which is why trich in newborns is sometimes missed initially. Any respiratory issues in a baby born to a trich-positive mother should be flagged to the care team.
3. Is neonatal trichomoniasis treatable?
Yes, completely. When trichomoniasis is confirmed in a newborn through laboratory testing, it is treated with an antibiotic appropriate for the baby's size and age. Medical records consistently show that symptoms improve and the parasite becomes undetectable after treatment. It's a treatable infection, the key is catching it.
4. Does having trichomoniasis during pregnancy mean I'll definitely pass it to my baby?
No. Transmission is rare even when a mother has an active infection at delivery. The risk goes up with untreated infection, high parasite load, and preterm birth, but the majority of babies born to trich-positive mothers are not infected. That said, "rare" is still a risk worth eliminating, treating during pregnancy removes it entirely.
5. I was treated for trich during pregnancy. Is my baby still at risk?
If the infection was confirmed cleared before delivery, the risk is essentially zero, there's no parasite left to transmit. It's worth retesting after treatment to confirm clearance, and making sure your partner was also treated to prevent reinfection. If both of those boxes are checked, you're in a good position heading into labor.
6. Does trichomoniasis affect the baby before birth, not just at delivery?
The primary risks during pregnancy are to the pregnancy itself rather than direct fetal infection in the womb. Trichomoniasis is associated with preterm birth, low birth weight, and premature rupture of membranes, all of which can affect the baby's health. Ascending infection into the uterus is documented but less common. The concern at delivery is the birth canal transmission route specifically.
7. Why isn't trichomoniasis part of standard prenatal screening?
The CDC has not established routine screening for asymptomatic pregnant people because evidence hasn't yet confirmed that universal screening and treatment improves overall birth outcomes. The complication is that one study raised concerns about treatment in asymptomatic pregnant women potentially increasing preterm risk, which complicated the picture. That said, symptomatic pregnant people should absolutely be tested and treated. If you have any concerns or risk factors, ask your provider directly.
8. Can I test for trichomoniasis at home while pregnant?
Yes. An at-home rapid test is a practical, discreet option that gives you results quickly without a clinic appointment. The testing window for trichomoniasis is 5–28 days after exposure. If you're currently pregnant and haven't been tested for trich, an at-home test is a fast way to get clarity, and if the result is positive, you have time to act before delivery.
9. My partner hasn't been tested. Does that matter for my baby's risk?
It matters a lot. If your partner has trichomoniasis and you treat while your partner doesn't, reinfection before delivery is a real possibility. Both partners need to test and treat simultaneously, and sexual contact should pause until both confirm clearance. This is how you make sure the infection is genuinely gone, not just temporarily reduced.
10. How long after treatment before the infection is confirmed cleared?
Trichomoniasis typically responds to treatment within a week. Retesting about two to four weeks after completing treatment is recommended to confirm clearance. This timeline matters during pregnancy because it gives you a window to act: treat, wait, retest, confirm. If you're in the third trimester, talk to your OB about timing, there's usually still time to treat and confirm clearance before your due date.
Test Before Labor, Your Baby's Risk Starts With Your Status
The most effective thing you can do to protect your newborn from trichomoniasis is to know your status before you go into labor. Trich can't pass through a birth canal that doesn't have it. If you're pregnant, haven't been specifically tested for trichomoniasis, and have any reason to wonder, a new partner, unusual discharge, or simply wanting certainty, testing is the fastest way to get there.
The Trichomoniasis At-Home STD Test Kit (98%+) delivers results without the wait of a clinic appointment. For a more complete pregnancy STI picture, the Women's 10-in-1 At-Home STD Test Kit covers trichomoniasis alongside chlamydia, gonorrhea, syphilis, HIV, hepatitis B and C, herpes HSV-1 and HSV-2, and HPV, everything in one kit, at home, on your schedule. And if you'd like to explore the full range of individual and combination tests available, the complete selection is at STD Test Kits.
Testing is straightforward. The infection is treatable. The risk to your baby is preventable. That's the whole picture, and it starts with knowing where you stand.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
2. CDC STI Treatment Guidelines, Trichomoniasis
3. PMC, Clinical Manifestation of Trichomonas vaginalis in Neonates: A Systematic Review
4. PMC, Trichomoniasis and Adverse Birth Outcomes: A Systematic Review and Meta-Analysis
5. Clinical Infectious Diseases, Trichomonas vaginalis Brain Abscess in a Neonate
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.