Last updated: April 2026
You just found out you're pregnant, and somewhere in the anxiety-spiral of prenatal appointments and first-trimester symptoms, a trichomoniasis diagnosis lands. The first question most people ask isn't about themselves; it's about the baby. Can trich cause a miscarriage? Could it trigger early labor? Here's what the science actually says, what the risks look like in real terms, and why getting tested and treated promptly makes a meaningful difference.
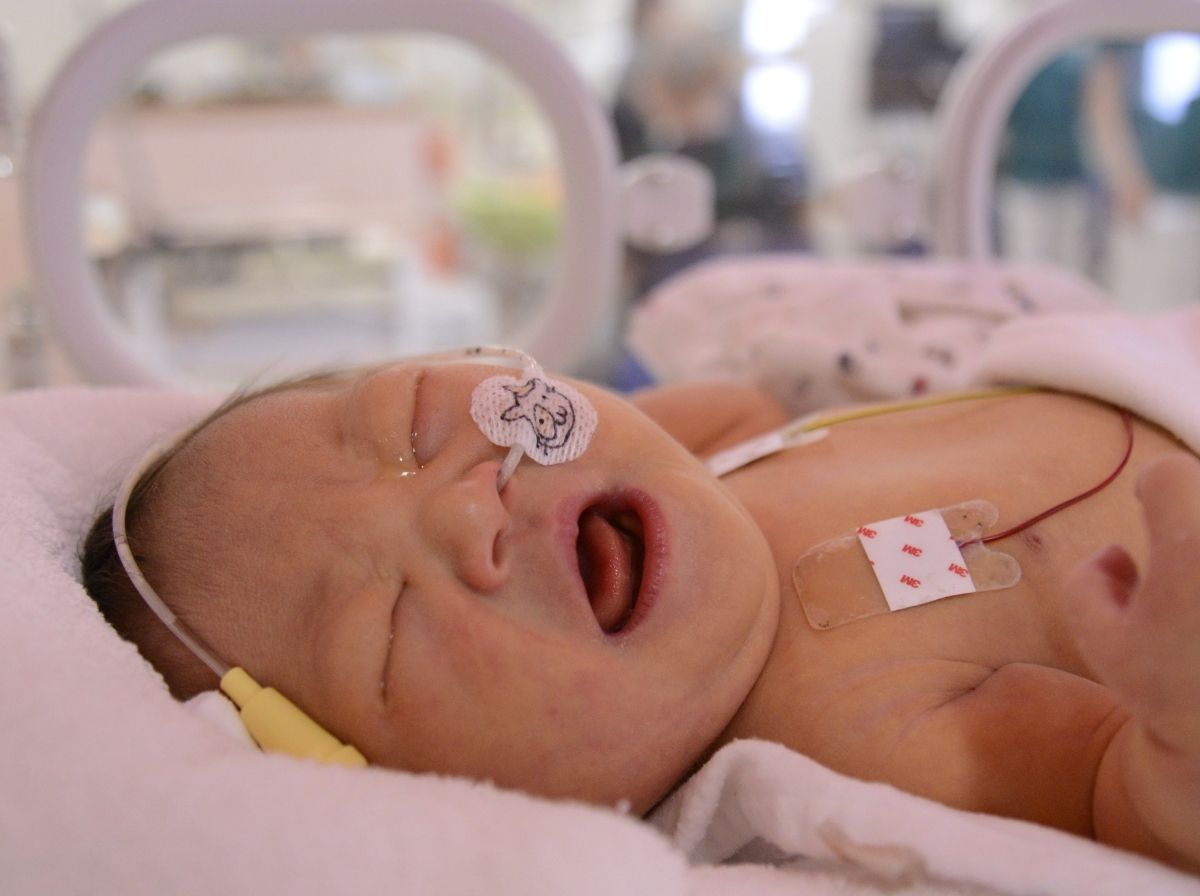
People are also reading: Can a Baby Get Trichomoniasis During Birth? What Happens and What to Do
Does Trichomoniasis Cause Miscarriage? The Direct Answer
No, trichomoniasis is not directly associated with miscarriage. Research published in BJOG and current CDC guidance both confirm that there is no established causal link between Trichomonas vaginalis infection and first-trimester pregnancy loss. What trich is associated with is different and still important: preterm birth, low birth weight, and premature rupture of membranes. Those are not the same thing as miscarriage, and that distinction matters enormously to anyone sitting with a positive test result and a growing baby.
What the evidence does show is something different, and it still matters: trichomoniasis in pregnancy is linked to a set of complications that can affect how and when your baby arrives. These are not the same thing as miscarriage, but they're worth understanding clearly. The distinction between "can cause miscarriage" and "is associated with preterm birth and low birth weight" is not just semantics; it changes the conversation significantly.
The internet, unsurprisingly, tends to blur this line. A search for "trichomoniasis and pregnancy" will return results ranging from calm to alarming, often presenting preterm birth risk and miscarriage as if they're interchangeable. They're not. Miscarriage, typically defined as pregnancy loss before 20 weeks, is a different outcome from preterm birth, which is delivery before 37 weeks of gestation. Trich has a documented association with the latter. Its connection to the former is not established in the medical literature.
That said, one area worth noting: some research has observed higher rates of trich infection among women who have experienced pregnancy loss. The mechanism isn't clear, and researchers are careful not to draw causal conclusions from correlational data. What's most likely is that trich creates a pro-inflammatory environment in the vaginal tract that can contribute to other complications, and that environment, not the parasite itself, may be the underlying factor in various adverse outcomes. The bottom line: trich doesn't cause miscarriages, but it can disrupt the conditions that support a healthy pregnancy.
Does Trichomoniasis Cause Premature Birth? What the Research Actually Shows
Here's where the evidence is genuinely significant. A 2021 systematic review and meta-analysis published in BJOG: An International Journal of Obstetrics and Gynaecology, one of the most comprehensive analyses of this topic to date, pooled data from multiple studies involving tens of thousands of pregnant women. According to that research, women with trichomoniasis during pregnancy had 1.27 times the odds of preterm delivery, nearly twice the odds of premature rupture of membranes (PROM), and more than double the odds of delivering a low birth weight baby compared to uninfected women. The CDC's own treatment guidelines acknowledge the association between T. vaginalis infection and adverse pregnancy outcomes, including premature rupture of membranes and preterm delivery as an established clinical concern.
Those numbers need to be put into plain English. Preterm delivery means giving birth before 37 weeks, which is when babies can have a lot of trouble with their lungs, keeping their body temperature stable, and eating. One of the best signs of how healthy a newborn will be is if they have a low birth weight, which is less than 2,500 grams (about 5.5 pounds). Premature rupture of membranes, which happens when the amniotic sac breaks before labor starts, can cause early labor or put the baby at risk of infection. None of these are certain, but the link is real and has been shown in many studies.
Scientists don't fully understand how this works, but they have a working theory. When you get trichomonas vaginalis, it makes your immune system react by causing inflammation in the cervical and vaginal tissue. This response includes higher amounts of certain inflammatory molecules, like interleukin-8 and vaginal defensins, which are also signs that neutrophils are active. That activation is linked to cervical ripening, which can lead to labor starting sooner than planned. To put it another way, the immune system's reaction to the infection may be more harmful to the pregnancy than the parasite itself.
It's also a good idea to put the numbers in context. A 1.27-fold higher chance of giving birth too soon means the risk is higher, not terrible. Most pregnant women who have trichomoniasis and don't get treatment don't give birth early. But "most people are fine" doesn't mean "there's no risk worth addressing," especially when the infection can be found and treated. When you add in the fact that trich is often completely asymptomatic during pregnancy, the math changes even more. This means that many women don't know they have it.
For more information on how trichomoniasis can affect your pregnancy, check out this article: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
Why Trich Is So Easy to Miss During Pregnancy
One of the most important things to understand about trichomoniasis in general, and especially during pregnancy, is that between 70 and 85 percent of people with the infection have no symptoms at all. Nothing. No discharge, no odor, no itching, no burning. The infection can be present and active for months or even years before any symptoms appear, and in many cases, symptoms never develop. This is what makes trich particularly relevant in a pregnancy context: you can carry this infection without any signal that something is wrong.
During pregnancy, the vaginal environment shifts. Hormonal changes alter the pH of the vaginal tract, which some research suggests creates conditions more conducive to T. vaginalis establishing and persisting. At the same time, the immune system modulates itself during pregnancy, it has to, to tolerate the developing baby, and that modulation can affect how the body responds to an existing infection. The result is that trich in pregnancy may behave differently than it does outside of pregnancy, and the downstream effects on the uterine environment can occur even when a woman feels completely normal.
This is not a reason to panic. It is a reason to test. The most significant gap in trich-during-pregnancy outcomes is the gap between infection and knowledge. Women who don't know they have trich can't make informed decisions about treatment. And unlike some infections where the risk/benefit calculation for treatment during pregnancy is complicated, trichomoniasis has an available, well-studied treatment option for symptomatic pregnant women.
When Should You Test for Trichomoniasis During Pregnancy?
If you're pregnant and have any reason to think you might have been exposed to trichomoniasis, a recent partner change, a new relationship, or simply the knowledge that this infection is extremely common and frequently asymptomatic, testing is the right call. The CDC's current guidelines state that symptomatic pregnant women, regardless of how far along they are, should be tested and considered for treatment. Routine screening for asymptomatic women hasn't been formally recommended, but individual providers, and many OBs, will screen based on risk factors and patient history.
Testing for trichomoniasis during pregnancy is straightforward. The most accurate method is a nucleic acid amplification test (NAAT), which detects the parasite's genetic material from a vaginal swab. This method is significantly more sensitive than the older wet-mount microscopy approach, it detects three to five times more infections. At-home rapid test options are also available and provide a practical option for women who want to know their status before or between prenatal appointments.
The testing window for trichomoniasis is relatively short: you can test for active T. vaginalis infection from around 5 to 28 days after exposure, which is when the parasite has established in the urogenital tract and becomes detectable. Unlike STIs that require an antibody response, trich testing looks for the organism itself, so there's no extended waiting period to worry about.
Is Trichomoniasis Treatment Safe During Pregnancy?
This is where many pregnant women get nervous, and understandably so. The standard treatment for trichomoniasis is an oral antibiotic, and the idea of taking medication during pregnancy sets off alarm bells even when the medication is well-studied. Here's the clear picture.
Metronidazole is the first-line treatment for trichomoniasis and is considered safe to use during pregnancy. Decades of clinical data, multiple meta-analyses, cohort studies, and randomized trials have not found evidence that it causes birth defects, fetal harm, or increased miscarriage risk. It does cross the placenta, which is why some providers are cautious about timing, but the weight of evidence consistently supports its safety profile for pregnant women.
The nuance here is around symptomatic versus asymptomatic infection. The CDC recommends treatment for symptomatic pregnant women at any stage of pregnancy. For asymptomatic pregnant women, the guidelines are less definitive; the benefit of treating an infection that isn't causing symptoms hasn't been conclusively established, and at least one notable trial (the NICHD Maternal-Fetal Medicine Units study) raised questions about whether treating asymptomatic trich in mid-pregnancy with high-dose metronidazole might actually increase preterm birth risk. That finding was controversial, and the methodology has since been criticized, but it contributed to the current cautious stance on routine screening and treatment of asymptomatic cases.
The practical takeaway: if you have symptoms, your provider will almost certainly recommend treatment. If you're asymptomatic but have a positive test result, the conversation with your OB or midwife is worth having, because individual circumstances, trimester, and risk factors all play a role in that decision. What's not helpful is sitting on an untreated symptomatic infection and hoping it resolves on its own. It won't, trich doesn't clear without treatment, and in the meantime, the inflammatory environment it creates in the vaginal and cervical tissue continues to exert pressure on the pregnancy.

People are also reading: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
Does My Partner Need to Be Treated If I Have Trich While Pregnant?
One aspect of trichomoniasis in pregnancy that often gets overlooked: your partner needs to be treated too. Trich doesn't resolve on its own for them either, and if only one partner is treated, reinfection is almost certain. This is not a hypothetical; reinfection rates for trichomoniasis are notably high, with some studies documenting rates of around 17 percent within three months of initial treatment even when both partners were told to seek care.
During pregnancy, reinfection matters more than usual. Going through treatment once, then reacquiring the infection, means your body returns to the same pro-inflammatory state that drives the adverse pregnancy outcomes described above. It also means a second round of treatment and a second round of navigating the risk/benefit calculation. The cleanest path through this is making sure your partner tests and treats at the same time, and that both of you abstain from sex until the infection has cleared and any symptoms have resolved.
This isn't about blame or suspicion. Trich is the most common curable STI globally, affecting an estimated 156 million people each year according to WHO data. It's been called one of the most neglected STIs precisely because it so rarely announces itself. A partner who has trich almost certainly doesn't know it. Getting them tested and treated isn't a confrontation; it's just a step in protecting your pregnancy.
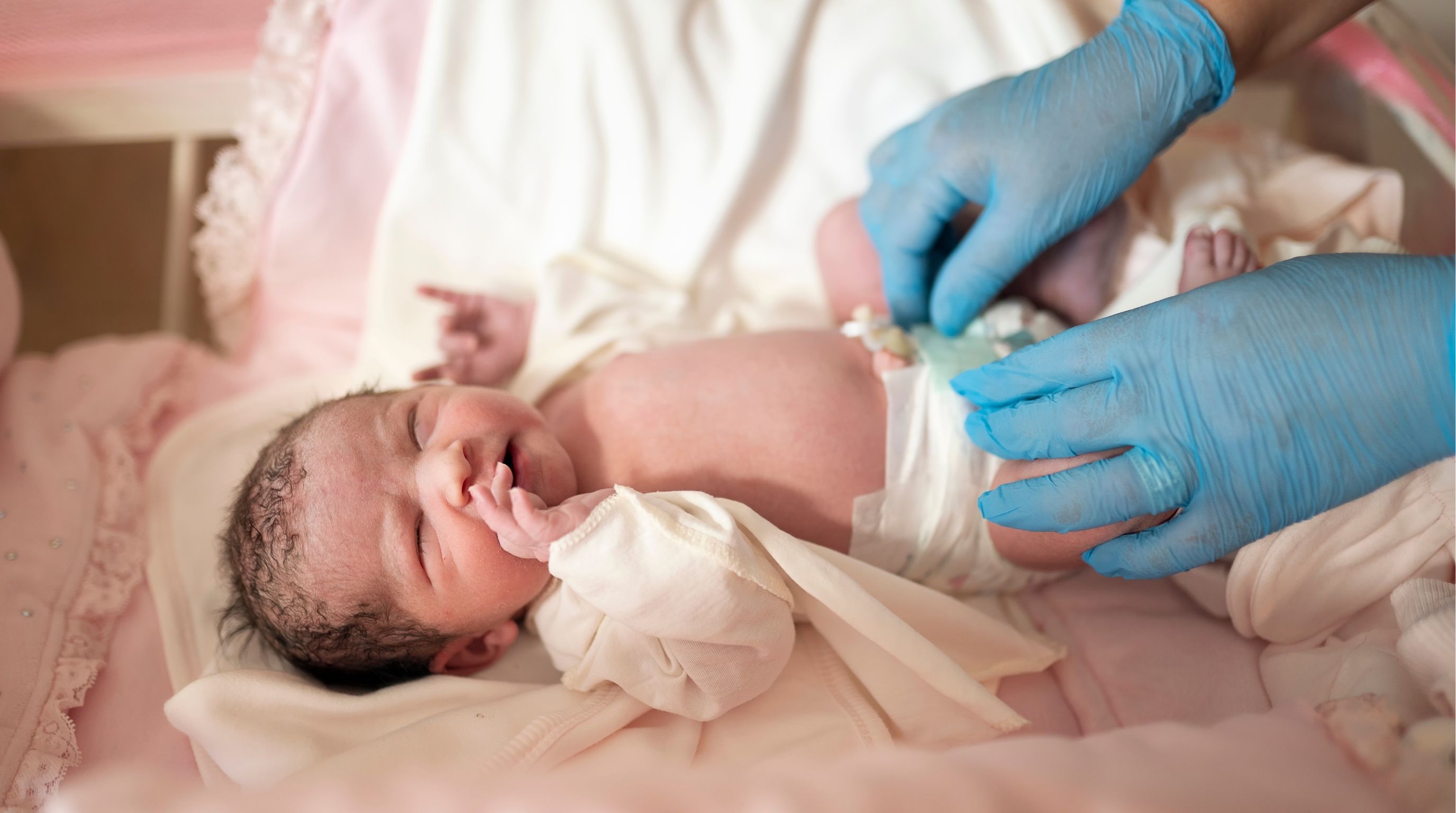
Can the Baby Get Trichomoniasis During Delivery?
The short answer is yes, but rarely. Vertical transmission, passing the infection to the baby during vaginal delivery, is documented but uncommon. When it does occur, the newborn may develop vaginal discharge or a respiratory infection. Both conditions are treatable. The risk of transmission drops to essentially zero if the infection is cleared before delivery, which is another strong argument for identifying and treating trichomoniasis well before your due date rather than letting it ride.
There are no documented cases of trichomoniasis spreading to a baby through the placenta or amniotic fluid; the parasite doesn't work that way. The transmission route is specifically through contact with infected vaginal secretions during passage through the birth canal. This means that even a positive test result during the third trimester, followed by prompt treatment and clearance, carries very low risk to the newborn.
The calculus here is straightforward: test early, treat promptly if indicated, and confirm clearance before delivery. That sequence essentially eliminates the newborn transmission risk and significantly reduces the preterm and low birth weight associations discussed above.
Is Trichomoniasis Tested for Routinely During Prenatal Care?
One thing that makes the conversation about trichomoniasis during pregnancy more complicated is that not all pregnant women in the US are routinely screened for it. Chlamydia and gonorrhea are common parts of prenatal STI panels, but trich is not a reportable disease and there is no formal CDC recommendation for universal prenatal screening. Researchers and public health experts, including those who have written articles for the American Journal of Obstetrics and Gynecology, have actively argued that this needs to change because trich has been shown to affect pregnancy outcomes and is more common in some groups than others.
What this means in real life is that a trichomoniasis test might not be part of your prenatal care. If you have any of the following risk factors: a new partner in the past year, a history of STIs, multiple partners, or symptoms like unusual discharge or vaginal irritation, you should ask your provider to test you. You can also take the initiative and do a test at home. This will give you information to bring to your prenatal appointments instead of waiting for a test that may not be part of the standard panel.
In general, the testing gap is a big problem for managing trich. Many infections go undetected and untreated, even during pregnancy, because they don't show any symptoms and aren't regularly screened. You can directly close that gap, at least for yourself.
To learn more about how trichomoniasis can impact your pregnancy, make sure to read our guide: Trichomoniasis During Pregnancy: Risks, Symptoms, Testing, and Treatment
FAQs
1. Is it possible for trichomoniasis to directly lead to a miscarriage?
No, trich is not connected to miscarriage. The study does not show that Trichomonas vaginalis directly causes pregnancy loss in the first trimester. It is linked to preterm birth and low birth weight, which are two completely different things. The fear of miscarriage is not supported by evidence if you were diagnosed early in your pregnancy.
2. How does having trichomoniasis make you more likely to have a preterm birth?
It causes an inflammatory immune response in the cervical tissue, which can start labor early. The infection increases the levels of certain immune molecules, especially interleukin-8, that are linked to cervical ripening. The body's response to the parasite, rather than the parasite itself, seems to be what causes the risk of preterm birth.
3. Is it safe to treat trichomoniasis in the first trimester?
Yes, the standard treatment has been thoroughly researched during pregnancy and has not been demonstrated to induce congenital anomalies or fetal injury. In the first trimester, many providers are cautious about when to start treatment. However, if you have symptoms, treatment is usually recommended at any stage. Talk to your OB or midwife about your own situation.
4. Is it possible to have trichomoniasis while pregnant and not have any symptoms?
Yes, and it's very common. Between 70 and 85 percent of people with trich don't show any signs of it at all. This is more important during pregnancy because the infection can still make things worse even when you feel fine. It's better to test than to wait for something to feel wrong.
5. What happens if you don't treat trich while you're pregnant?
If trich is not treated, it can lead to preterm birth, membranes breaking too soon, and low birth weight. The infection also doesn't go away on its own; without treatment, it can last for months or even years. The only sure way to get rid of the risk is to test and treat right away.
6. Will my baby definitely be harmed if I have trich during pregnancy?
No, most pregnant women with trichomoniasis do not have the worst complications. The data shows that there is a higher statistical risk for all groups, but it doesn't mean that any one person will definitely get sick. Treatment gets rid of that higher risk, which is why it's so important to find out early.
7. Is it possible for trichomoniasis to cause membranes to break too soon?
Yes, this is one of the strongest links in the research. According to data from eight studies, women with trich have almost twice the risk of having their membranes break too early compared to women who are not infected. PROM can cause preterm labor or put the pregnancy at risk of infection, which is why treating an active infection is important.
8. If I'm pregnant with trich, does my partner need to get treatment?
Yes, without a doubt. If only one partner is treated, they are almost sure to get sick again. If they get sick again during pregnancy, the risk timeline starts over again. Both partners get treated at the same time, and neither of them has sex until the infection is completely gone.
9. How soon after being exposed can I get a trichomoniasis test while pregnant?
After being exposed, you can get a reliable result in 5 to 28 days. Trich tests find the organism directly instead of waiting for an antibody response, so there isn't a long waiting period like there is with HIV or syphilis. A few weeks after a possible exposure is enough time to do a meaningful test.
10. Do prenatal care providers regularly check for trich?
Not everywhere, and that's a big problem. Trichomoniasis is not part of the standard prenatal STI panel for all patients in the US, unlike chlamydia and gonorrhea. If you have risk factors or symptoms, ask your provider to test you, or use an at-home test to find out right away.
Know Your Status Before Your Due Date
Trichomoniasis is curable, manageable, and, when caught during pregnancy, something you have real options for addressing. The risk is real but not inevitable, and the clearest path through it is knowing your status early enough to act on it. Testing during pregnancy isn't overreacting. It's exactly the kind of proactive decision that makes a difference in outcomes.
The Trichomoniasis At-Home STD Test Kit from STD Test Kits gives you fast, private results you can act on. If you want broader coverage, especially relevant if you're planning a pregnancy or recently entered a new relationship, the 7-in-1 Complete At-Home STD Test Kit screens for trichomoniasis alongside chlamydia, gonorrhea, syphilis, HSV-2, hepatitis B, and hepatitis C in one comprehensive panel. Or explore the full combo test kit range to find what fits your situation.
Visit STD Test Kits for discreet, accurate testing you can do on your terms, because knowing what's happening in your body is always better than guessing.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
2. CDC, Trichomoniasis STI Treatment Guidelines
3. WHO, Trichomoniasis Fact Sheet (2025)
4. Sabet et al., Persistent Trichomoniasis in Pregnancy: A Case Report, Cureus (2025)
5. Klebanoff et al., Failure of Metronidazole to Prevent Preterm Delivery, NEJM
6. Cochrane Review, Interventions for Trichomoniasis in Pregnancy
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.