Is One STD Test Enough After a One-Night Stand?
Quick Answer: Yes, HIV can cause mouth sores, especially in early or advanced stages, often showing up as ulcers, white patches (thrush), or gum inflammation. But not all mouth sores mean HIV. Testing is the only way to know for sure.
This Isn’t Just a Canker Sore, And Here’s Why
When it comes to early signs of HIV, the mouth is often the first place the virus makes itself known, quietly, subtly, and often misdiagnosed. People in acute HIV infection (the earliest stage) can experience flu-like symptoms, and in some cases, this includes painful ulcers inside the mouth, swelling of the gums, or patches of white coating on the tongue and cheeks.
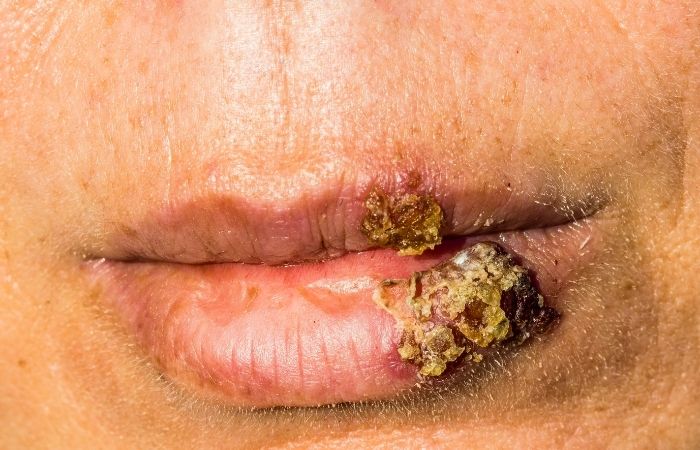
Unlike a regular canker sore or a hot pizza burn, HIV-related mouth sores tend to linger longer, appear in multiples, and may be accompanied by swollen lymph nodes, fatigue, or fever. And here’s the kicker: some people experience no fever at all, just the oral symptoms. That’s why paying attention to your mouth matters, especially after recent exposure.
According to the CDC’s symptom breakdown, mouth ulcers and thrush are documented symptoms of HIV, particularly during the acute and chronic phases. But they’re not exclusive to HIV, which is where confusion sets in.
People are also reading: When Antibiotics Fail: Why Your STD Isn’t Going Away
“I Thought It Was From Stress, It Was HIV”
Diego, 27, noticed two painful ulcers inside his cheek about ten days after a weekend where the condom slipped. He didn’t have a fever, just a nagging sore throat and swollen gums. A week later, the sores were still there, and a strange white coating appeared on his tongue. His dentist called it “probably thrush.”
“I’d just started a new job. I figured it was stress. I’d never even heard that HIV could show up in your mouth first.”
Two weeks later, Diego took a rapid HIV test at home. It was positive. Confirmed by a follow-up blood test. The mouth symptoms were his only warning sign.
Diego’s story isn’t rare. In many cases, especially for people without fevers or rashes, oral symptoms are the only red flag their body raises during early HIV infection.
Common HIV-Linked Mouth Conditions (And What They Look Like)
It’s not just one type of sore. HIV can manifest in the mouth in several different ways, depending on your immune status and the phase of infection. Here's a breakdown of the most common ones:
Table 1. Common oral symptoms linked to HIV infection. These signs aren’t unique to HIV but become more common or persistent when the immune system is compromised.
Not Every Mouth Sore Is HIV, But Some Are a Warning
It’s easy to spiral. One sore in your mouth and suddenly you're Googling pictures of late-stage HIV complications at 2 a.m. But the truth is: most mouth sores are not caused by HIV. That doesn’t mean you should ignore them, especially if you’ve had unprotected oral, vaginal, or anal sex recently.
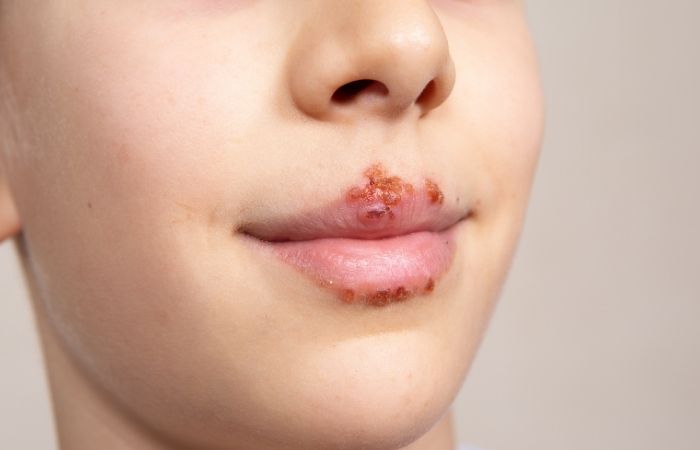
Many STDs can cause oral symptoms that look similar to HIV’s early signs. For example, herpes can cause blister-like sores in or around the mouth, while syphilis often begins with a single, painless sore that can appear on the tongue, lips, or inner cheek. Even gonorrhea and chlamydia can infect the throat, sometimes leading to irritation, redness, or soreness, without causing visible lesions at all.
So how do you tell the difference? You don’t, not with your eyes. Visual diagnosis isn’t reliable for any STD. But you can understand the patterns. HIV-related mouth sores are more likely to appear with other systemic symptoms (like fatigue or swollen lymph nodes), and they tend to last longer or recur. If you have any doubt, test, because only a test can tell you what’s really going on.
Can You Get HIV From Kissing or Oral Sex?
Short answer: kissing is not a realistic way to get HIV. Even deep, tongue-heavy kissing is considered extremely low risk by all major health organizations, including the CDC. The virus doesn’t transmit through saliva alone.
Oral sex, on the other hand, carries some risk, especially if there are open sores, bleeding gums, or untreated oral infections present. Receptive oral sex (giving oral to a penis or vagina) has a lower risk than anal or vaginal sex, but it’s not zero. The presence of mouth ulcers, gum disease, or even a small cut in the mouth can increase the chances of HIV transmission if exposed to infected semen, vaginal fluids, or blood.
And here's the uncomfortable truth: if you’ve had oral sex with someone whose status is unknown or if a condom broke, your mouth sore could mean something. Not necessarily HIV, but enough to warrant a test.
When to Test If You’ve Noticed Mouth Symptoms
If you’ve recently had a potential exposure and now you’re seeing ulcers, white patches, or gum inflammation, it’s valid to be concerned. But timing your test is just as important as taking it.
Here’s the testing window for HIV:
Table 2. HIV test types, window periods, and retesting recommendations. Earlier testing is possible, but may require confirmation later for accuracy.
Got mouth symptoms and unsure when exposure happened? Err on the side of action. A rapid at-home test can give you answers in minutes, and peace of mind in hours. If you test negative early, retest at the 3-month mark or sooner if symptoms continue.
Don’t wait and wonder. Order a discreet HIV test kit you can take from home. Whether it’s a sore or a hunch, you deserve to know.
Other Reasons Your Mouth Might Be Acting Up
Before you assume the worst, let’s get real about how many things can cause mouth sores. From spicy food to stress, your oral tissue reacts to a lot. Canker sores, allergic reactions, vitamin deficiencies, and even hormonal shifts can all lead to ulcers or irritation inside your mouth.
White patches? Not always HIV. Oral thrush can appear if you’ve recently taken antibiotics, used corticosteroid inhalers (like for asthma), or if you’re diabetic. Gum bleeding can spike during hormonal changes, after dental procedures, or due to poor oral hygiene. Your mouth is sensitive, and not every symptom is a signal of a serious infection.
The difference with HIV-related oral symptoms is persistence. They're more likely to last, come back frequently, or appear alongside other immune-related signs like fatigue, night sweats, or swollen glands. But again, these patterns are helpful, not diagnostic. Only a test can confirm what’s going on.
Immune Suppression Changes the Game
HIV affects the immune system at its core, and the mouth is one of the first places that immune breakdown can show up. If you’re already living with HIV but not on treatment, or if you don’t know your status, symptoms like recurring thrush, severe gum disease, or unusual oral lesions could signal a drop in CD4 count.
This is especially important for people with past exposures or those who stopped treatment. The worse your immune suppression, the more susceptible your mouth becomes to secondary infections. That includes viral (herpes, HPV), fungal (candida), and bacterial issues. Even simple wounds can take longer to heal.
If you’re seeing mouth symptoms over and over, especially when paired with fatigue or weight loss, talk to a provider. You can start with a home test, but follow-up care matters, too.
People are also reading: Can You Get an STD at a Sex Party If You Use Protection?
When Mouth Symptoms Mean It’s Time to Act Fast
Most oral symptoms are annoying, not dangerous. But some combinations should trigger faster testing or urgent medical attention. These include:
- Painful ulcers that last more than 2 weeks
- White patches that can’t be scraped off
- Persistent sore throat with swollen lymph nodes
- Severe gum bleeding or rapid gum recession
- Fuzzy white lesions on the tongue (possible hairy leukoplakia)
If you’re experiencing any of the above, especially after potential exposure, it’s smart to test now, and again in a few weeks if needed. That’s not paranoia. That’s prevention.
Your status doesn’t define you, but knowing it gives you power. If your symptoms are mild but you’re still worried, you can return to STD Test Kits to explore discreet, doctor-trusted testing options. There’s no pressure, no clinic line, and no shame.
FAQs
1. Can HIV really show up in your mouth?
It can, and often does. Mouth sores, ulcers, white patches (like thrush), and gum inflammation are all possible signs of HIV, especially in the first few weeks after infection or later if the immune system is struggling. But here’s the twist: they’re never proof by themselves. You need a test to know for sure.
2. What do HIV-related mouth sores actually look like?
They’re not that different from other types, usually small, round or oval, reddish ulcers that hurt like hell when you eat. Sometimes they show up in clusters. Other times, you’ll notice white patches that don’t brush off easily. If it’s lingering, painful, or keeps coming back, it’s worth paying attention to.
3. How soon after exposure can HIV affect the mouth?
Mouth symptoms can pop up during the acute phase, typically 2 to 4 weeks after exposure. You might feel flu-ish, or you might feel totally fine except for that weird sore that won’t heal. Your mouth could be the only part of your body throwing up a red flag.
4. Could it just be stress or something I ate?
Totally possible. Canker sores, burns from hot food, even citrus overload can trigger mouth irritation. But if you’ve had recent unprotected sex, or you’re noticing other stuff like fatigue, swollen glands, or night sweats, it’s smart to take that sore seriously. Rule out the scary stuff first.
5. I kissed someone with a cold sore. Should I panic?
Breathe. Kissing, even with a cold sore present, is an extremely low-risk activity for HIV. The virus doesn’t spread through saliva, and you'd need significant blood exposure for any real concern. That said, herpes? Much more likely from that scenario. Testing never hurts.
6. What’s the deal with thrush and HIV?
Oral thrush is a yeast overgrowth that can show up in people with weakened immunity, which includes folks with HIV. But it’s also super common if you’ve taken antibiotics, use steroid inhalers, or have diabetes. If it keeps coming back, or shows up alongside other symptoms, it’s a clue worth following.
7. Is gum bleeding a red flag for HIV?
It can be, especially if your gums are sore, swollen, or bleeding easily. But flossing too hard or not getting your teeth cleaned regularly can also make your gums bleed. The main difference with HIV is how long and how bad it gets. Think of it like "my toothbrush looks like a weapon of murder."
8. What kind of HIV test works for mouth symptoms?
Any reliable HIV test will give you answers, oral fluid tests, finger-prick rapid tests, lab-based 4th gen tests, or even RNA options. The symptom doesn't change the type of test, it’s all about timing. Most folks start with a rapid test at home and confirm with a lab test if needed.
9. Should I retest if my first result was negative?
If you tested early, within the first 2 to 3 weeks after exposure, yes, retesting is smart. HIV can take a little time to show up on a test, depending on your body and the type of test used. Three months post-exposure is the gold standard for confirmation.
10. Can I test at home, or do I need to go to a clinic?
You can absolutely test at home. In fact, if the thought of a clinic makes you sweat, grab a discreet HIV test kit online. It’s private, fast, and gives you results in minutes, no awkward waiting room, no explaining yourself to anyone.
You Deserve Answers, Not Assumptions
Your mouth is trying to tell you something, but it’s not always clear what. A sore, a white patch, or bleeding gums don’t automatically mean HIV. But they do mean something’s off. And if you’ve had recent sexual exposure, those signals deserve your attention, not your silence.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted six of the most relevant and reader-friendly sources. Every external link in this article was checked to ensure it leads to a reputable destination and opens in a new tab, so you can verify claims without losing your place.
Sources
2. Mayo Clinic: HIV/AIDS Overview
3. How HIV Spreads | CDC (oral ulcers and transmission risk)
4. HIV/AIDS – Symptoms and Causes | Mayo Clinic
5. HIV and AIDS – StatPearls | NCBI Bookshelf
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: T. Nguyen, NP, AAHIVS | Last medically reviewed: December 2025
This article is for informational purposes and does not replace medical advice.






