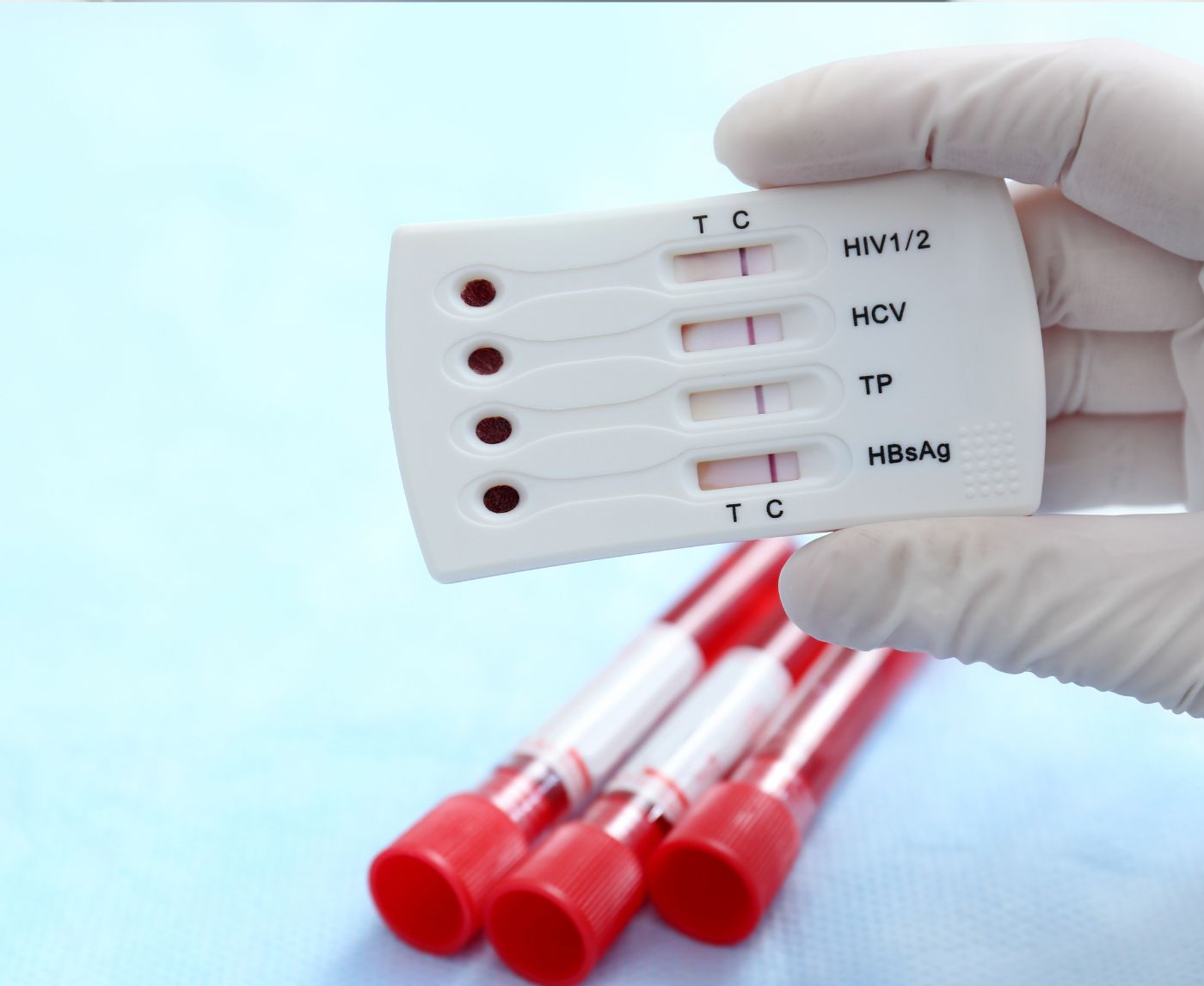
Think You Have HIV? Why Testing Too Early Can Backfire
Quick Answer: Stress, poor sleep, and immune suppression can worsen HPV by lowering your body’s ability to suppress or clear the virus. While sex doesn’t “cause” reactivation, immune changes linked to physical or emotional strain may.
The Shame Cycle: “I Thought I Was Done With HPV”
Malia’s story isn’t rare. Many people think they’ve “cleared” HPV, only to get a positive result months or years later. That’s because HPV doesn’t always disappear; it often becomes dormant. Your immune system holds it in check, silently. But when stress floods your body with cortisol, or when you run on five hours of sleep for too long, your defenses can falter.
For some, this means HPV shows up again on a routine cervical screening. For others, it means new symptoms, genital warts, abnormal cells, or Pap results that feel like a betrayal. But here’s the truth: this isn’t your fault. Reactivation doesn’t mean failure. It means your body needs support.
HPV reactivation is common, especially in people with fluctuating immunity, like those who are pregnant, navigating grief, under high workplace pressure, or even adjusting to new meds. And yet, most people never hear this until it happens to them.
People are also reading: Partner Positive, You Negative? The Real Reasons Behind Mismatched STD Tests
Your Immune System: The Real MVP Against HPV
So how does the body actually fight HPV? It’s not like chlamydia, where antibiotics can wipe it out. HPV relies entirely on your immune system’s ability to suppress or clear the virus over time. That process can take anywhere from six months to two years, and it’s not always permanent. Think of it like a dragon in a cave: quiet, but still there.
Most of the time, HPV remains invisible, no symptoms, no problems. But if the immune system weakens, the virus can become active again. That’s why stress, smoking, sleep deprivation, depression, chronic illness, and even extreme exercise can influence the virus’s behavior.
According to a 2020 review in Frontiers in Oncology, psychological stress is associated with lower cell-mediated immunity, which is critical in suppressing HPV infections. Simply put: your mindset, lifestyle, and body load all matter.
Stress and Cortisol: What Actually Happens
Let’s talk about the stress hormone, cortisol. When your body thinks you're under threat, it releases cortisol to help you survive. Great for short-term danger. Terrible for long-term immunity. Chronically high cortisol can suppress white blood cells, reduce inflammation control, and lower your ability to fight infections, including HPV.
Studies show that higher perceived stress is linked to HPV persistence. And this isn’t just about “being anxious.” It includes things like:
What does this mean for you? If you’re healing from HPV, or living with a “cleared” diagnosis, stress reduction isn’t just self-care. It’s strategy. Your nervous system is part of your immune system’s toolbox. And sometimes, slowing down is how you fight back.
Does Sleep Impact HPV Suppression?
Yes. Sleep isn’t optional when it comes to immune function. It’s the reset switch your body depends on to produce infection-fighting cytokines and maintain healthy T-cell activity. Without sleep, even healthy people show reduced immune responsiveness, and for someone with HPV, that could mean viral persistence.
One study in the journal Sleep found that sleep-deprived participants produced fewer antibodies after vaccination, an indirect marker of lowered immunity. And while that research focused on the flu shot, it illustrates a powerful point: your body doesn’t fight well when it’s tired.
So if you’re wondering why HPV keeps lingering… ask yourself: Are you resting? Are you recovering? Are you giving your body a chance to defend you?
Sex, Intimacy, and Reactivation Risk
Let’s get something clear: HPV doesn’t “come back” just because you had sex again. But the story is more nuanced. Physical intimacy can overlap with hormonal shifts, skin irritation, new strains, or, most importantly, changes in your immune readiness. So while sex itself isn’t the villain, it’s often blamed because it happens around the same time as reactivation.
That’s why people like Ty, 31, feel confused and ashamed.
“I used condoms. I hadn’t had any issues in a year. Then boom, warts again. It felt like my body betrayed me.”
What actually happened? Ty had just moved cities, lost his job, and wasn’t sleeping. He wasn’t reckless, he was overwhelmed.
Here’s what we know from the data:
Rather than blaming sex itself, the more accurate story is that sex intersects with many biological changes. And yes, HPV can still be passed between partners, even after symptoms disappear. But the answer isn’t to avoid intimacy forever. It’s to understand your body, protect your peace, and make informed choices.
Sexual healing includes immune healing. And you don’t have to choose between intimacy and immunity.
Boosting Your Body’s Defense: What Helps, What Doesn’t
Here’s the part people are always Googling at 2AM: Can I do anything to help my body clear HPV? The answer? Yes, but it’s not one magic supplement. It’s a full-body approach, grounded in science and compassion. You’re not “boosting” your immune system like an energy drink, you’re giving it the space and tools it needs to do its job.
Here’s what actually supports immune suppression of HPV:
- Sleep: Aim for 7–9 hours a night. Sleep debt = immune suppression.
- Stress Reduction: Mindfulness, therapy, and community all lower cortisol.
- Nutrition: Antioxidants like vitamins C and E, folate, and zinc support immune pathways.
- Quit Smoking: Smoking has been directly linked to HPV persistence and cervical dysplasia progression.
- Moderate Alcohol: Excess drinking can reduce immunity and increase risk of reactivation.
Supplements? Some early research suggests compounds like AHCC (Active Hexose Correlated Compound), mushroom extracts, and green tea catechins may support immune responses. But they’re adjuncts, not replacements for sleep, stress care, and follow-up testing.
If your head is spinning and you just want a next step, pause here:
Peace of mind is one test away. If you’re wondering whether HPV is back, or want to confirm suppression, you can test at home, privately and quickly.
Order a discreet HPV rapid test kit to check your status from home, with clear instructions and fast results.
When to Retest, And When Not to Panic
If you’ve had an abnormal result, wart recurrence, or just that “gut feeling” something’s off, it’s valid to want clarity. But retesting too soon can muddy the waters. HPV testing, especially after treatment or exposure, depends on timing.
Here’s a general rule of thumb:
- After wart treatment: Wait 6–12 weeks to retest, as inflammation can trigger false positives.
- After abnormal Pap: Follow your provider’s guidance, often 6–12 months unless high-risk strains are involved.
- After “clearing” HPV: Annual follow-up is typical; retest if symptoms recur or you have new exposures.
But emotionally? It’s not always about guidelines. It’s about feeling safe in your own skin. If waiting is making your anxiety worse, or if you’re about to start a new relationship, an at-home test can be a powerful tool to ground your decisions.
STD Test Kits offers discreet, easy-to-use options that put control back in your hands. No judgment, no waiting rooms.

People are also reading: Partner Positive, You Negative? The Real Reasons Behind Mismatched STD Tests
Privacy, Shipping, and Discreet Support
If you’re even slightly embarrassed about testing, or retesting, at home, we see you. You are not alone. HPV isn’t just a virus. It’s a trigger for shame, confusion, and isolation. That’s why privacy isn’t a luxury. It’s a medical necessity for healing minds, not just bodies.
Ordering an at-home test doesn’t mean you’re hiding. It means you’re reclaiming agency. And here’s the truth: STD Test Kits ships in discreet packaging, no logos, no sexual health branding, no one at the mailbox will know. You get results privately, quickly, and without having to explain anything to a receptionist or pharmacist.
Plus, if you’re traveling, living off-grid, or just exhausted by waiting rooms, this approach gives you flexibility. Most kits arrive in 2–3 business days (depending on your location), and results can be ready within minutes depending on the test type. That means you don’t have to put your life, or your intimacy, on hold.
What If You Test Positive?
Breathe. Seriously, take one deep breath. A positive result for HPV isn’t the end of your story. It’s a signal. A checkpoint. And it’s something that 4 out of 5 sexually active adults will face at some point, whether they know it or not.
Testing positive doesn’t mean you’re dirty, reckless, or broken. It means your immune system and the virus are in a new phase of negotiation. And guess what? You can still date. You can still have sex. You can still thrive.
Here’s what you can do:
- Confirm the type: High-risk HPV strains are linked to cancer risk; low-risk strains cause warts. Know what you’re dealing with.
- Talk to a provider: Especially if you haven’t had a cervical screening recently or if you have visible symptoms.
- Let partners know: HPV is common. Disclosure can be simple, direct, and stigma-free.
- Get vaccinated (yes, even now): The HPV vaccine protects against additional strains and may reduce reactivation risk.
And if you're spiraling? You're allowed to feel that. Just don’t stay stuck there. HPV is manageable. Many strains resolve. Treatment exists. And you’re not navigating this alone.
If you want to check on a partner or retest post-treatment, you can order a Combo STD Home Test Kit here. No extra trip. No awkward questions. Just facts, fast.
FAQs
1. Can stress bring HPV back?
Yes, chronic stress can suppress your immune system, making it more difficult for the body to suppress the quiet HPV. In this case, high cortisol puts the brakes on immune cells, especially T-cells and natural killer cells, which are important in fighting viruses. Stress may not cause active HPV, but it increases the chance of activation if one has had it.
2. Does sufficient sleep really work against HPV?
Sleep is important for immune function, which includes cytokine production and virus-fighting white blood cells. Poor sleep weakens your body's capability to suppress HPV; thus, one might suffer from persistent infection or reactivation. Get 7–9 hours of good quality sleep every night.
3. Can sex reactivate HPV?
Sex alone does not reactivate HPV; however, it can sometimes coincide with immune changes, exposure to different subtypes, or physical trauma. If you are fatigued, sleep-deprived, or under stress, it may seem that sex has brought on the outbreak, but it is more often only one part of a broader biological scenario.
4. Why did my HPV test go from negative to positive again?
It is possible this could be HPV reactivation, rather than an acquiring a new infection. HPV can remain dormant and undetectable for months or years. When your immune system becomes weakened, the virus can then become active again and appear in testing. This happens frequently and is not something to be deemed irresponsible.
5. Can I still have sex if I test positive for HPV?
Yes, with responsible choices. HPV is a very common virus that usually goes unrecognized. It can be prevented by using condoms and having open communication with partners. Many people have active sex lives while having HPV. You don't have to be celibate to be responsible.
6. What can I take to help clear HPV?
There is no sure cure, but it is a matter of boosting your immunity. Lifestyle modifications-sleep, proper nutrition, stress reduction-along with a few promising supplements, such as AHCC, green tea extract, or even folate-may be of great help to your body in suppressing the virus. Always consult a healthcare provider before taking up any supplementation.
7. Is the HPV vaccine still useful if I already have HPV?
Sometimes, yes. The vaccine covers several strains, and even if you had one, you can still be protected against the others. It may also help in reducing recurrence risks. It is a good topic for discussion with your provider.
8. How long does it take for HPV to go away?
Most HPV infections clear within 6-24 months. The high-risk strains may take longer or require ongoing monitoring. How you clear depends on your immune system; things like sleep, smoking, and stress impact how well you can fight it off.
9. Can I give HPV to someone if I do not have any symptoms?
Yes. HPV infection does not always have symptoms, which is why screening and open talk are important. Sometimes the virus is silent, but that doesn't mean you need to be.
10. If I have cleared the HPV virus already, do I need to be tested again?
You don't always need to bother with retesting unless new symptoms emerge or you get a different sexual partner altogether. However, this testing may be helpful for peace of mind, or if you're about to start intimacy again. At-home tests offer discretion.
You’re Not Broken, You’re Human
Living with HPV doesn’t make you reckless, dirty, or damaged. It makes you a human being with a body doing its best. Whether you’re fighting off the virus for the first time or wondering why it came back, your story isn’t over. It’s evolving.
You don’t need perfect immunity. You need knowledge, care, and control over your next move. That’s where at-home testing comes in. When the medical system feels like too much, or too far, you still deserve answers.
Don’t wait and wonder, get the clarity you deserve. This at-home combo test kit checks for the most common STDs discreetly and quickly.
How We Sourced This Article: In our guide, we have harnessed clinical research, peer-reviewed literature, and emotional first-person narratives to investigate how stress, sex, and sleep influence HPV. We have used credible sources, including the National Institutes of Health, published literature through PubMed on the reactivation of HPV, and emotional stories from online health groups on Reddit, as well as women’s health blogs, to create a medically valid and emotionally valid experience for our readers.
Sources
1. Basic Information about HPV and Cancer (CDC)
2. Human Papillomavirus (HPV) Infection - STI Treatment Guidelines (CDC)
3. Human papillomavirus (HPV) and cancer (WHO Fact Sheet)
4. HPV and Cancer (National Cancer Institute)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He combines clinical accuracy with a straightforward, sex-positive approach and is dedicated to making his work available to more people in both cities and rural areas.
Reviewed by: J. Rivera, MPH | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.