Can Chlamydia or Gonorrhea Infect Your Eye? What to Watch For
Quick Answer: Eye infection after sex can be caused by certain STDs including chlamydia, gonorrhea, and herpes. Transmission usually happens when infected fluids touch the eye directly or indirectly, and symptoms often resemble pink eye but may be more intense.
How STDs Actually Reach the Eye (It’s More Common Than You Think)
The eye is a mucous membrane. That means it’s soft, moist, and biologically similar to the inside of your mouth or genitals. Certain bacteria and viruses that infect genital tissue can also attach to eye tissue if they’re transferred there.
This transfer usually happens in one of three ways. Direct exposure during oral sex if semen or vaginal fluid gets into the eye. Indirect transfer if you touch infected genitals and then rub your eyes without washing your hands. Or rarely, through contaminated fingers, sex toys, or towels used immediately after sex.
It’s called autoinoculation when you spread an infection from one part of your body to another. It sounds clinical, but in real life it’s just this: you didn’t think about it. You touched something. Then you touched your face.
According to guidance from the CDC, infections like chlamydia and gonorrhea can infect mucous membranes including the eyes. It’s not the most common site, but it is documented and treatable.
People are also reading: Green or Yellow Discharge After Sex: What It Really Means
Pink Eye or an STD? Why the Symptoms Overlap
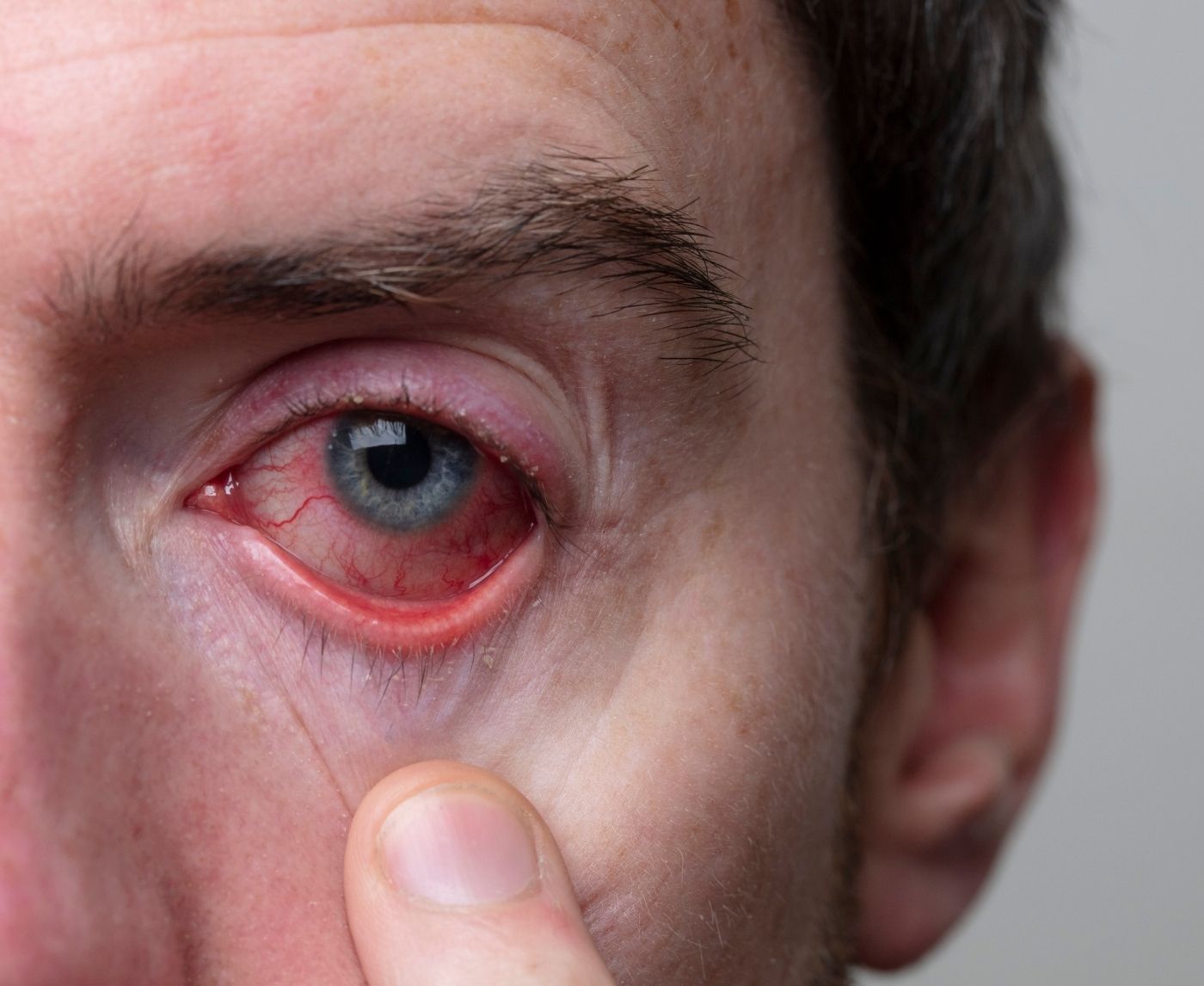
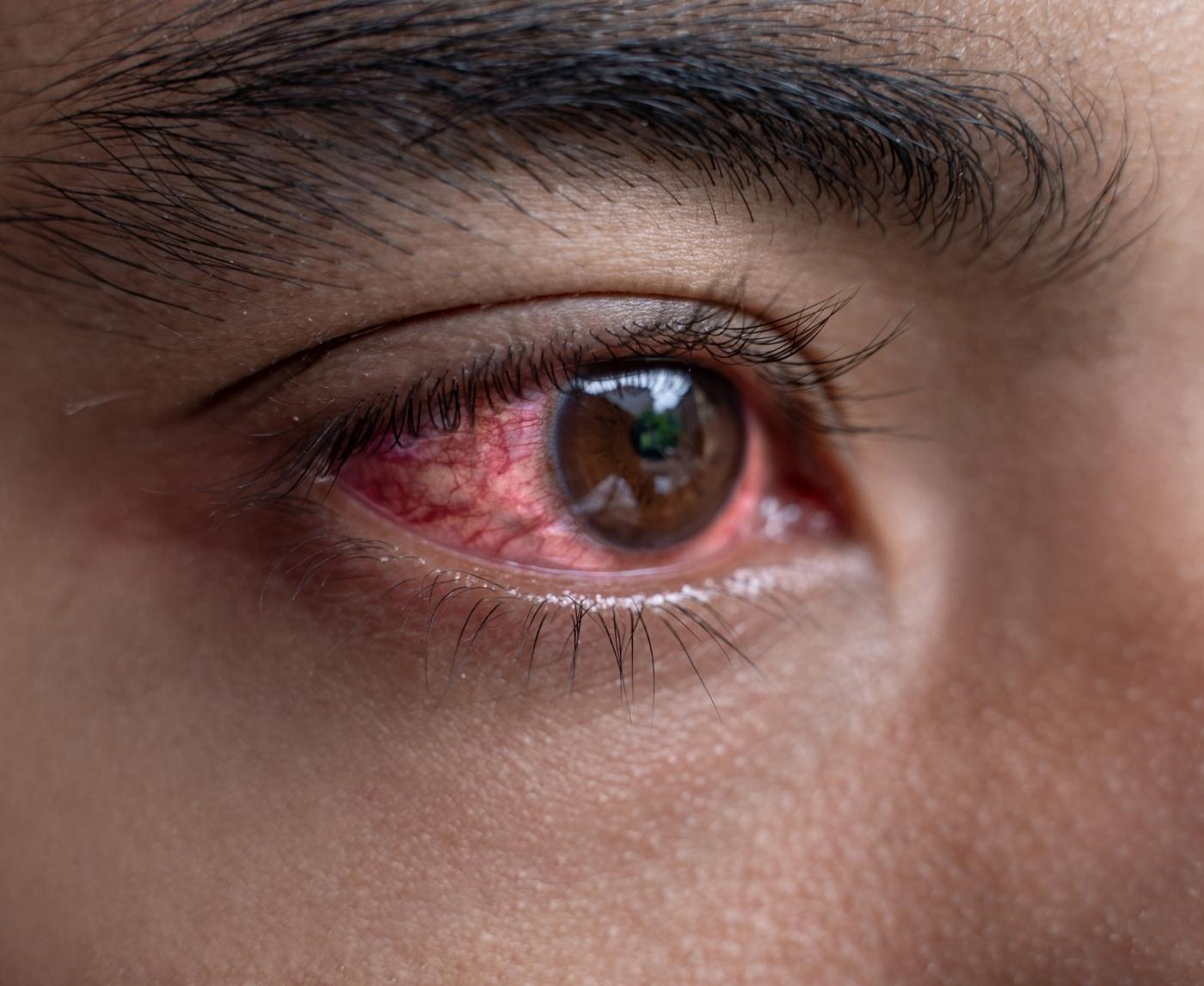
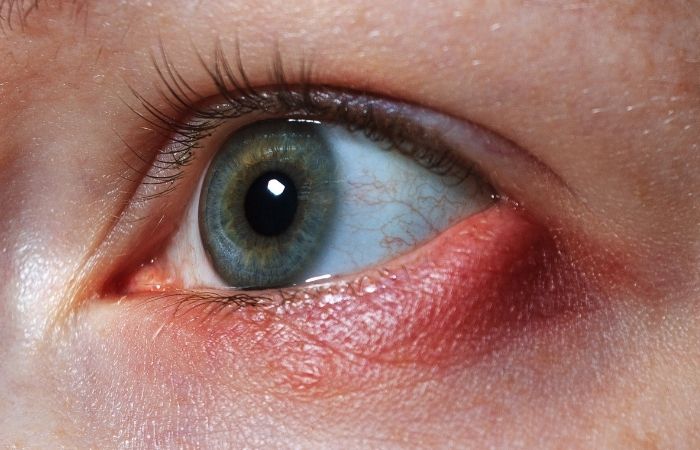
Most people think of pink eye as something kids get from school. But medically, “pink eye” just means conjunctivitis, inflammation of the thin membrane that covers the white part of your eye. That inflammation can be caused by viruses, bacteria, allergies, or STDs.
The uncomfortable part is that STD-related conjunctivitis can look almost identical to routine bacterial conjunctivitis at first. Redness. Swelling. Discharge. Crusting. Tearing. The overlap is real.
Where things start to diverge is intensity and timing. Gonorrhea-related eye infections, for example, can produce thick, heavy discharge and rapid swelling. Ocular herpes can cause pain, light sensitivity, and a gritty sensation that feels deeper than surface irritation.
Figure 1. Symptom comparison between common conjunctivitis and STD-related eye infections. Diagnosis requires medical evaluation.
The tricky part? You can have chlamydia in the eye without noticeable genital symptoms. Many people with chlamydia have no symptoms at all, according to the World Health Organization. That’s where confusion creeps in.
The Main STDs That Can Infect Eyes
Not every STI spreads to the eye. But a few absolutely can. Understanding which ones matter keeps this grounded in reality instead of worst-case spirals.
- Chlamydia can cause a form of conjunctivitis when the bacteria Chlamydia trachomatis reaches the eye. It may present as redness, discharge, and swelling. Adults usually acquire it through hand-to-eye transfer after genital contact.
- Gonorrhea in the eye, known medically as gonococcal conjunctivitis, can be more aggressive. The Mayo Clinic notes that gonorrhea can infect the eyes and requires prompt antibiotic treatment to prevent complications.
- Herpes can infect the eye as well, typically as herpes keratitis. Unlike bacterial infections, ocular herpes often causes sensitivity to light and a painful, gritty sensation. It may recur because herpes viruses remain in the body long-term.
Rarely, untreated syphilis can affect the eyes during later stages, causing inflammation and vision changes. This is uncommon but medically documented.
If you’re reading this thinking, “Okay but can you go blind from an STD?”, severe untreated gonorrhea or herpes infections can damage the cornea. But early treatment dramatically reduces that risk. Blindness is not the typical outcome when people seek care promptly.
How Soon Would Eye Symptoms Show Up?
Timing matters. Symptoms from bacterial eye infections caused by chlamydia or gonorrhea may appear within two to seven days after exposure. Sometimes it takes longer. Herpes-related eye symptoms may develop days after direct contact or during a recurrence.
This is where people spiral. “It’s been 24 hours, is this it?” Most infections don’t erupt instantly. Irritation the next morning is more likely mechanical friction, allergy, or standard conjunctivitis. But persistent redness or worsening discharge over several days deserves attention.
If your eye symptoms appear alongside genital burning, discharge, or sores, the suspicion level rises. If eye symptoms are isolated, STD transmission is possible but statistically less common.
When Testing Makes Sense (And What to Test)
If you have an eye infection after sex and there was direct fluid exposure or hand-to-eye contact, testing is reasonable. That doesn’t mean your eye itself always gets swabbed first. Often clinicians test the genital site because eye infections can mirror genital infection.
Nucleic acid amplification tests (NAATs) are highly accurate for detecting chlamydia and gonorrhea. These are the same lab-grade technologies discussed by the CDC laboratory recommendations. If you suspect exposure from oral sex, genital and throat testing may also be recommended.
If you’re not ready for a clinic visit, you can start with a discreet option at STD Test Kits. At-home screening for common bacterial STDs can give you clarity quickly and privately. If results are positive, treatment through telehealth or a provider becomes the next step.
Peace of mind matters. If your head is racing, taking action often feels better than refreshing search results at 2AM.
What It Actually Feels Like: Real Scenarios, Not Just Symptoms
Leila, 27, noticed her right eye felt scratchy two days after a new partner performed oral sex. “I thought it was just allergies,” she said. “Then it started producing this thick discharge that wasn’t normal. I kept thinking, this can’t be connected… right?”
When she finally went to urgent care, a swab confirmed gonorrhea. She had no genital symptoms at all. The bacteria had likely transferred through fluid contact and a moment of rubbing her eye afterward. Treatment worked quickly, but the emotional spiral lasted longer than the infection.
Another case looked different. Rafael, 34, experienced intense light sensitivity and a sharp, stabbing pain in one eye after kissing and oral sex with a partner who later disclosed cold sores. He assumed it was pink eye until an ophthalmologist diagnosed ocular herpes. Antiviral treatment controlled the outbreak, but it required immediate attention.
These stories aren’t meant to scare you. They’re meant to ground this in reality. Eye infections after sex are uncommon compared to genital infections, but when they happen, they follow predictable biological rules.
Transmission Isn’t Magic, It’s Contact
Let’s dismantle one myth right now: STDs do not “travel” through your bloodstream randomly to your eyes after sex. They reach the eye through contact. That contact can be direct fluid exposure or indirect hand transfer.
If semen, vaginal fluid, or discharge enters the eye during oral sex, transmission risk increases. If you touch infected genital tissue and then rub your eyes without washing your hands, that also creates opportunity. Towels and fabrics used immediately after sex can theoretically transfer bacteria if they’re damp with fresh fluid, though this is less common.
This is why washing hands after sex matters. Not because sex is dirty. Because bacteria and viruses respond to opportunity.
According to clinical guidance summarized by the National Center for Biotechnology Information, gonococcal conjunctivitis in adults is typically linked to direct inoculation from genital secretions. It’s preventable and treatable when caught early.
How Doctors Distinguish STD Eye Infections From Routine Pink Eye
This is one of the most common fear-driven queries: “Can semen cause eye infection?” Semen, in itself, is not infectious. What can be infectious is what it carries.
Semen can be said to be infectious if it carries any kind of bacteria or virus. If the person does not have any kind of STD, then it may cause irritation, not infection. If they have chlamydia or gonorrhea, then they can transmit infection. Irritation caused by friction, lube, or even tears can cause redness in the eyes the following day.
Not all redness in the eyes after oral sex is necessarily infection. Sometimes it can be mechanical, which can be cured in 24-48 hours.
Figure 2. Clinical decision factors in suspected STD-related conjunctivitis. Final diagnosis requires medical evaluation.
Can Semen or Vaginal Fluid Alone Cause an Eye Infection?
This is one of the most common fear-driven queries: “Can semen cause eye infection?” Semen, in itself, is not infectious. What can be infectious is what it carries. Semen can be said to be infectious if it carries any kind of bacteria or virus. If the person does not have any kind of STD, then it may cause irritation, not infection. If they have chlamydia or gonorrhea, then they can transmit infection. Irritation caused by friction, lube, or even tears can cause redness in the eyes the following day. Not all redness in the eyes after oral sex is necessarily infection. Sometimes it can be mechanical, which can be cured in 24-48 hours.

People are also reading: Should Both Partners Get Tested Before Going Condom-Free?
When It’s Urgent, And When It’s Not
There are moments when you should not wait. If your eye becomes extremely swollen, produces thick pus-like discharge, causes intense pain, or your vision blurs, seek urgent medical care. Gonococcal infections in particular can progress quickly.
If symptoms are mild and stable, you may have time to monitor for 24 hours while arranging testing. But do not ignore worsening pain or visual changes. Your eyes are not a place for guesswork.
The good news is that with proper antibiotics or antivirals, most STD-related eye infections resolve without long-term damage. Early treatment dramatically reduces complications.
Testing After Oral Sex: What Actually Makes Sense
If your concern stems from oral sex exposure, testing strategy depends on what contact occurred. If fluids entered your eye, evaluation for conjunctivitis is appropriate. If there was oral-genital contact, throat and genital testing may also be relevant.
NAAT testing for chlamydia and gonorrhea typically becomes reliable within one to two weeks after exposure. Testing too early can miss infection, which is why timing matters. The NHS outlines similar window considerations for bacterial STIs.
If you're within that window and anxious, starting with a discreet at-home option can give you clarity without sitting in a waiting room replaying worst-case scenarios. The 6‑in‑1 At‑Home STD Test Kit screens for common bacterial infections and offers private results you control.
You deserve information, not spirals. Testing is not an admission of guilt. It’s a health decision.
Window Periods, Eye Symptoms, and Why Timing Can Calm You Down
One of the most destabilizing parts of an eye infection after sex is not knowing when something “should” show up. You replay timelines. You calculate hours. You wonder if symptoms appearing the next morning mean certainty.
Here’s the grounded version: most bacterial STDs that infect the eye do not cause symptoms within a few hours. They usually develop over several days. Viral irritation or friction-related redness, on the other hand, often appears quickly and improves quickly.
Understanding window periods doesn’t just help with testing. It helps your nervous system settle down.
Figure 3. Approximate timing for STD-related eye symptoms and testing reliability. Individual cases vary.
If your eye is red 12 hours after sex and improving the next day, infection becomes less likely. If it’s worsening at day three with thick discharge or increasing pain, evaluation makes more sense.
The Emotional Spiral Is Real, Let’s Talk About It
When something affects your eyes, it feels intimate and frightening. Vision is vulnerable. You don’t just worry about infection, you worry about damage, permanence, blindness. The mind jumps ahead of the evidence.
But here’s what data consistently shows. Severe complications from STD-related eye infections are uncommon when treated promptly. The Cleveland Clinic explains that herpes keratitis can threaten vision if untreated, but antiviral therapy is highly effective when started early.
Most adults who develop gonococcal conjunctivitis and receive antibiotics recover fully. Most ocular chlamydia cases resolve with appropriate treatment. The horror stories online almost always involve delayed care.
You are not reckless for having sex. You are not irresponsible for worrying. Anxiety after sexual exposure is common because STIs carry cultural stigma layered over medical reality. Our job here is to separate biology from shame.
If You Think You Transferred Something to Your Eye
If you immediately recognize the entry of the infectious material, rinse your eye with clean water or sterile solution. Avoid the use of harsh chemicals, and do not scrub the eye excessively, as this will cause further inflammation.
Wash your hands before touching your face again. Avoid the use of contact lenses during the duration of the illness. If the infection causes redness and discharge, it is imperative to seek medical attention immediately.
Testing the potential source of infection, which is the genitals, is included in the process of evaluation. If you suspect infection and are in the appropriate period, using STD Test Kits will give you an early idea of your situation, and your results are kept confidential.
Can You Have an STD in the Eye Without Genital Symptoms?
Yes. This is what makes the whole situation confusing. Chlamydia in particular is notorious for being asymptomatic in the genitals. You may have no burning, no discharge, no pain, and still carry bacteria capable of infecting another mucous membrane.
That doesn’t mean it’s common. It means it’s possible. And possibility is often enough to fuel anxiety.
If your only symptom is eye redness and there was no obvious high-risk contact, statistically you are more likely dealing with routine conjunctivitis. But if you had direct exposure to infected fluid, testing becomes logical rather than paranoid.
What Happens If You Ignore It?
Most mild conjunctivitis resolves on its own. STD-related eye infections, however, usually require targeted treatment. Untreated gonococcal infection can damage the cornea. Untreated herpes can cause recurrent inflammation.
The key word here is untreated. Early intervention dramatically lowers risk. The moment you seek care, the trajectory changes.
Delaying because of embarrassment is far more dangerous than the infection itself. Healthcare providers treat these cases without judgment. They see them more often than you think.
Protecting Your Eyes During and After Sex
This isn’t about fear. It’s about practical awareness. If you’re engaging in oral sex and want to reduce risk, avoid direct ejaculation into the eyes. Wash hands before touching your face. Avoid sharing towels immediately after sex.
If you or your partner have active genital discharge, sores, or known infection, pausing sexual activity until treatment is completed protects both of you. That’s not moralizing. That’s microbiology.
Condoms and barrier methods reduce risk of transmission of bacterial STDs. They don’t eliminate risk entirely, but they lower the bacterial load and opportunity for spread.

People are also reading: 7-in-1 Complete At-Home STD Test Kit
FAQs
1. Okay, seriously, can an STD really infect your eye?
Yes. It’s not common, but it’s real. If infected fluids come into direct contact with your eye, or you touch genitals and then rub your eyes without thinking, bacteria like chlamydia or gonorrhea can transfer. It’s biology, not karma.
2. How do I tell if this is just pink eye or something sexual?
Context matters. If you woke up red-eyed after a long flight or allergy season, that’s one thing. If it showed up a few days after unprotected oral sex and it’s producing thick discharge or worsening pain, that’s another. The symptoms overlap, which is why testing, not guessing, brings clarity.
3. My eye is red the morning after sex. Is that too fast to be an STD?
Usually, yes. Most bacterial STD-related eye infections take a couple of days to develop. Redness within hours is often irritation, friction, or plain old conjunctivitis. If it fades quickly, infection becomes less likely. If it intensifies, that’s your cue to check in with a provider.
4. Can semen alone cause an eye infection?
Semen itself isn’t the villain. If your partner doesn’t carry an infection, exposure may cause temporary stinging but not an STD. Infection only happens if bacteria or viruses are present in that fluid. Irritation and infection are not the same thing.
5. What does gonorrhea in the eye actually look like?
Think heavy discharge. Swelling that feels dramatic. Sometimes rapid progression. It can look more aggressive than routine pink eye. It’s treatable, but it’s not something to ignore or “wait out.”
6. What about herpes in the eye, should I panic?
Panic won’t help, but prompt care will. Ocular herpes often feels painful and light-sensitive, almost like something is stuck in your eye. Antiviral medication works very well when started early. The key is not brushing it off as “just irritation” if pain and vision changes show up.
7. Can you go blind from this?
That’s the fear that sends people spiraling at 1AM. Severe, untreated infections can damage the cornea. But blindness is rare when treatment starts early. Most people recover fully. The horror stories almost always involve delayed care.
8. I don’t have any genital symptoms. Does that mean it can’t be an STD?
Not necessarily. Chlamydia especially can be silent in the genitals. You can carry it without knowing. That’s why eye symptoms after sexual exposure sometimes feel confusing, there’s no obvious “proof” elsewhere.
9. Should I test even if I feel a little silly?
If you had direct fluid exposure and your symptoms aren’t resolving, testing is smart, not dramatic. A discreet at-home option can help you move from anxiety to answers without sitting in a clinic lobby replaying your weekend.
10. What’s the smartest next step right now?
If symptoms are severe, pain, vision changes, heavy discharge, seek urgent care. If they’re mild but persistent and there was sexual exposure, arrange testing. Wash your hands. Don’t rub your eyes. And remember: sexual health includes your eyes, too.
You Deserve Clarity, Not Catastrophe
An eye infection after sex can be very scary because it affects both your vision and your intimacy, which are very private areas. But most cases can be treated, and many of them have nothing to do with STDs. The main thing that separates panic from power is information.
If you had fluid exposure, worsening symptoms, or simply cannot stop wondering, take action. Testing protects you and your partners. You can start privately through STD Test Kits, get answers discreetly, and move forward with facts instead of fear.
Sex does not make you irresponsible. Ignoring symptoms does. If your body is signaling something, listen, calmly, confidently, and without shame.
How We Sourced This Article: We reviewed guidance from major public health authorities including the CDC, WHO, NHS, and Mayo Clinic, alongside peer-reviewed research on gonococcal conjunctivitis, ocular herpes, and chlamydial eye infections. Approximately fifteen medical and lived-experience sources informed this piece. Below are six reader-friendly, authoritative references used to support key claims. All links were checked to ensure accuracy and credibility.
Sources
1. Centers for Disease Control and Prevention – Sexually Transmitted Infections
2. Mayo Clinic – Gonorrhea Symptoms and Causes
3. Chlamydial Infections - STI Treatment Guidelines | CDC
5. Conjunctivitis (Pink Eye) | American Academy of Ophthalmology
6. Pink eye (conjunctivitis) - Symptoms and causes | Mayo Clinic
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He combines clinical accuracy with a straightforward, sex-positive approach and is dedicated to making accurate sexual health information more widely available.
Reviewed by: L. Chen, MD, Ophthalmology | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.