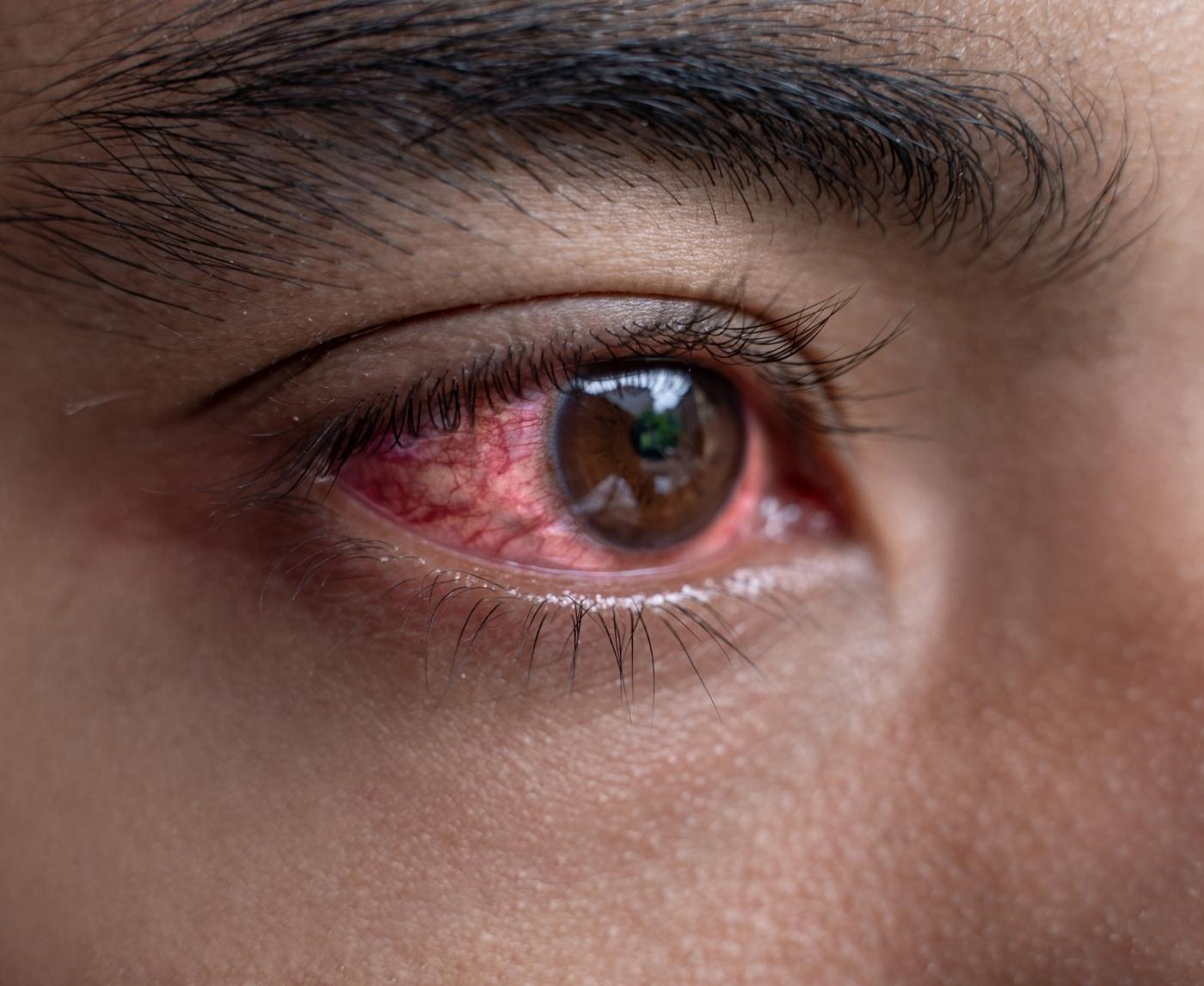
Can Chlamydia or Gonorrhea Infect Your Eye? What to Watch For
Quick Answer: A recent article has found a significant rise in antibiotic resistance in gonorrhea among doxyPEP users, emphasizing the importance of at-home STD testing for effective prevention.
The study, published in Clinical Infectious Diseases and reported by the Center for Infectious Disease Research and Policy (CIDRAP), takes a hard look at the effectiveness, and consequences, of using doxycycline as a post-sex prevention tool. DoxyPEP, already embraced by some health communities for reducing chlamydia and syphilis, seems to be hitting a wall with gonorrhea. Specifically, researchers found that people taking doxyPEP developed higher rates of tetracycline-resistant strains of Neisseria gonorrhoeae.
So where does that leave us? The short answer: prevention isn’t just pills. Testing is still your first line of defense. This article unpacks what the new study says, what it doesn’t, and how at-home STD test kits help you stay ahead of evolving threats like antibiotic-resistant gonorrhea.

People are also reading: I Got an STD Without Having Sex, Here’s How It Happens
Who This Guide Is For (And Why It Matters)
If you’re relying on medications to protect yourself from STIs, or just heard about doxyPEP and are curious if it's all you need, this guide is for you. It’s also for anyone who’s seen headlines about superbugs and is wondering if gonorrhea just got harder to detect or treat. This isn’t fear porn. It’s fact-checking, empowerment, and options.
Many people assume they’d “know” if they had an STD. But gonorrhea is slippery: half of people with it don’t show obvious symptoms. Even worse, if the bacteria start dodging antibiotics like it’s been shown to do in doxyPEP users, missing an early infection could lead to bigger problems down the line, like pelvic inflammatory disease, infertility, or urethral damage.
This guide will walk you through what this new resistance data means for real-world prevention, the limits of doxycycline after sex, and why rapid testing, especially at home, is still critical. We’ll break down sample types, timelines, resistance mechanics, and what to do if your result is positive.
Doxycycline and Gonorrhea: A Relationship Built on Limits
Doxycycline has never been a go-to for treating gonorrhea. In fact, the CDC stopped recommending it back in the 1980s due to growing resistance. So why has it come back into the conversation?
The recent excitement around doxyPEP stems from its effectiveness against chlamydia and syphilis. In clinical trials, including the French ANRS 174 DOXYVAC trial, doxyPEP users saw an 83% drop in those two STIs. But for gonorrhea? Not so much. The same study found a relatively small reduction in gonorrhea cases, and a big spike in tetracycline resistance. That’s like patching a leak in one part of the boat while drilling a hole in another.
In numbers: 35.5% of gonorrhea samples from the doxyPEP group showed high-level tetracycline resistance versus 12.5% in the placebo group. That’s a big enough jump to get global health agencies to pump the brakes.
Why This Resistance Matters Now
This isn’t just about one antibiotic. The same gonorrhea samples showed reduced susceptibility to cefixime, a second-line treatment option still used worldwide. Researchers flagged a novel mutation, penA34.007, that might signal future problems with more front-line treatments like ceftriaxone.
Translation: if we overuse doxyPEP, we may be accelerating the evolution of strains that don’t respond to *any* of our existing tools. And because gonorrhea is fast-spreading, often silent, and affects disproportionately high-risk communities, this is more than a science problem. It’s a public health pressure cooker.
This is exactly where testing becomes your best ally, not an afterthought. When you test regularly, you’re not just protecting yourself. You’re interrupting transmission chains and giving labs the data they need to track resistance in real time.
How At-Home Testing Fits Into the Resistance Crisis
At-home STD tests may not sound as high-tech as post-exposure antibiotics, but they are consistent, evolving, and remarkably effective when used correctly. Whether you’re using a rapid test with visual results or a mail-in kit with PCR-grade accuracy, you’re giving yourself something doxycycline never could: confirmation.
If you’re MSM, trans femme, or in a network with high STI exposure, here’s the hard truth: resistance is already here. Prevention is now a full-body strategy. Regular testing, especially after new partners, symptoms, or exposure events, lets you catch infections early, treat them properly, and prevent the spread of resistant strains.
Our at-home combo test kits check for chlamydia, gonorrhea, syphilis, and HIV, and arrive in discreet packaging with fast results.
Resistance by the Numbers
To understand why testing now matters more than ever, here’s a breakdown of what the French DOXYVAC study uncovered, and why it set off alarm bells among STI experts worldwide:
Figure 1. Comparison of resistance outcomes in DOXYVAC trial arms. These numbers reflect bacterial samples collected from trial participants and genetically analyzed for resistance markers.
The rise in the penA34.007 mutation among DoxyPEP users is particularly worrisome because it suggests we could be nurturing a more cefixime-resistant gonorrhea strain in the population, while falsely believing we're preventing it.
What Testing Reveals That Medication Can’t
Testing tells you what’s actually going on inside your body. Medication taken preemptively, like doxyPEP, is always a gamble, especially when you don’t know what you’ve been exposed to. And as we’ve now seen, relying on antibiotics to "cover your bases" could backfire if resistance is already in play.
Consider this: if you’ve taken doxyPEP and still feel off, burning during urination, discomfort during sex, unusual discharge, an at-home test can tell you if gonorrhea has slipped through the cracks. This isn’t paranoia. This is prevention informed by evidence. You can’t treat what you don’t test for.
That’s why combining behavioral strategies (like condom use and risk awareness) with regular testing remains the most reliable way to catch and control STIs, especially ones trying to outsmart our meds.
When Gonorrhea Doesn’t Look Like Gonorrhea
Gonorrhea has mastered the art of going undetected. Nearly 50% of infections in people with penises show no symptoms at all, and in people with vaginas, it’s even more likely to go silent. And yet, untreated gonorrhea can cause serious complications like pelvic inflammatory disease, infertility, chronic pain, and even increased HIV risk.
To make things worse, when gonorrhea does show up, it often mimics other infections: UTIs, yeast infections, bacterial vaginosis, even hemorrhoids. Burning during urination could be anything. So could itchiness or discharge. That’s why symptoms alone can’t guide you, especially when resistant strains don’t behave predictably.
In a world where more STIs are learning how to dodge antibiotics, the only thing you can trust is a test. At-home kits offer a clear yes or no without waiting for symptoms that may never show.
Gonorrhea Isn't Just a One-Time Thing
Getting treated once doesn’t mean you’re in the clear forever. In fact, many people who test positive for gonorrhea once are reinfected within months, especially if their partners aren’t tested or treated at the same time. Add resistant strains into the mix, and the stakes only get higher.
This isn’t about blame. It’s biology. Gonorrhea spreads fast, hides well, and doesn’t care if you just finished antibiotics last month. That’s why retesting is essential after any new partner, any untreated exposure, or 30–45 days post-treatment, even if you feel fine.
Testing regularly means you’re not just reacting. You’re preventing. You’re protecting your partners. You’re staying one step ahead of an infection that’s trying to evolve faster than we can treat it.

People are also reading: Tested Negative, Still Infected? Why Super-Gonorrhea Is Hard to Catch
STIs That Masquerade as Something Else
Figure 2. STIs are often mistaken for other conditions, leading to delayed testing, treatment, and rising resistance. Testing removes the guesswork.
FAQs
1. Can I still use doxyPEP?
You can, but don’t treat it like a forcefield. It works well for chlamydia and syphilis in high-risk groups, but gonorrhea is the wildcard. Think of doxyPEP like an umbrella: good protection in light rain, but not great in a hurricane of antibiotic resistance.
2. Is resistant gonorrhea a real thing, or just media hype?
Very real, and very annoying. We’ve already seen strains that laugh at the meds we used to count on. The CIDRAP-backed study just confirms what clinics have been whispering for a while: gonorrhea is evolving fast, and testing is our best way to stay in the game.
3. How would I even know if I have gonorrhea?
That’s the thing, you might not. Half the time, it doesn’t throw a parade of symptoms. When it does? It could look like a UTI, sore throat, weird discharge, or nothing at all. So unless your spidey sense is medically certified, go with a test.
4. I took antibiotics after sex. Isn’t that enough?
It might help for some STIs, sure. But here’s the kicker: if gonorrhea is already resistant to that antibiotic, you’re just giving it gym time to bulk up. You still need to test to see what’s actually happening.
5. What if my test is positive?
Take a breath, no shame here. Most STIs, including gonorrhea, are treatable. You’ll likely need a different antibiotic, maybe even a shot. But first, make sure the result is accurate and let a provider walk you through next steps. Pro tip: bring your partners into the convo early. You’re protecting them too.
6. Do I need to test even if I don’t have symptoms?
Yes, especially if you’re in a high-exposure network or have had new partners recently. Testing isn’t about symptoms, it’s about strategy. Catching something early is the difference between a quick treatment and a months-long mess.
7. How accurate are at-home tests for gonorrhea?
Very, when used properly and at the right time post-exposure. Rapid tests are great for fast checks; lab-based kits offer even higher accuracy. Always follow the timing guide, and when in doubt? Retest.
8. Can I get reinfected after treatment?
100%. It’s not like chickenpox, you don’t build lifelong immunity. If your partner wasn’t treated, or you pick up a new exposure, it can come back around. That’s why follow-up testing matters just as much as treatment.
9. What’s up with this penA34.007 mutation?
Basically, it’s a genetic tweak that makes gonorrhea more chill about cefixime, an antibiotic that used to work pretty well. The fact that it’s popping up more in doxyPEP users? Not great. It means we’re seeing evolution in real time, and it’s not trending in our favor.
10. Where can I get tested discreetly?
Right here: STD Test Kits ships test kits straight to your door in plain packaging. No awkward pharmacy pickup, no judgmental receptionist. Just you, your results, and real peace of mind.
You Deserve Better Than “Wait and See”
This isn’t about doomscrolling science headlines, it’s about making informed choices. The data is clear: gonorrhea is getting smarter, and doxyPEP isn’t the fix-all many hoped it would be. But the power to act is still yours. Testing is your clarity. It’s your control. And it doesn’t have to be complicated or public.
Don’t wait and wonder, get the clarity you deserve. The 7-in-1 Complete At-Home STD Test Kit checks for the most common STDs discreetly and quickly.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted some of the most relevant and reader-friendly sources.
Sources
1. CIDRAP – Post-trial data highlight doxyPEP resistance concerns
2. CDC – Gonorrhea: Detailed STD Facts
4. Planned Parenthood – Gonorrhea Testing & Treatment
5. Doxy PEP for Bacterial STI Prevention | CDC
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: R. Singh, PhD, Microbial Resistance | Last medically reviewed: November 2025
This article is for informational purposes and does not replace medical advice.