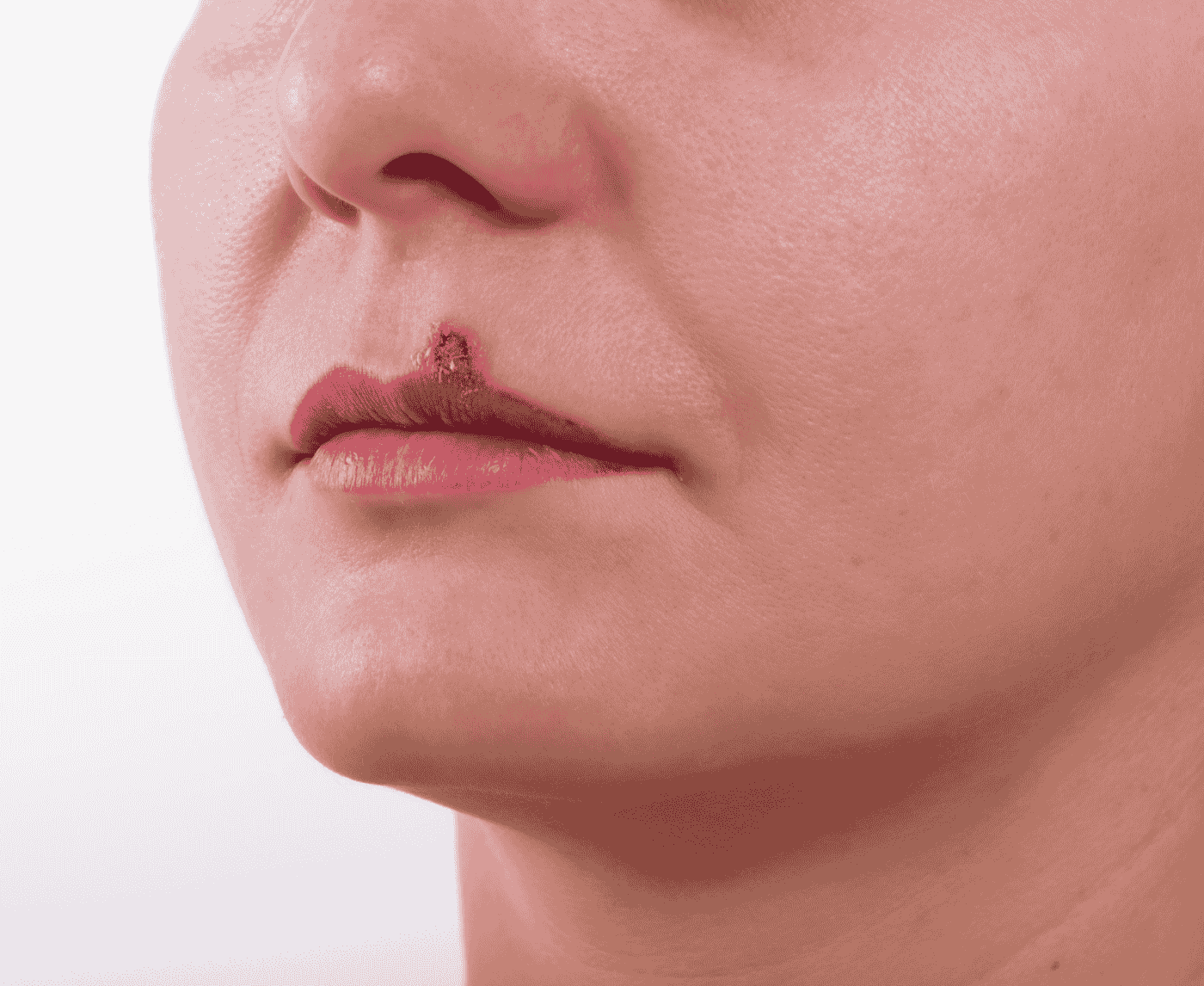Why So Many People Have Herpes and Don’t Even Know
Quick Answer: Herpes keratitis is a corneal infection caused by the herpes simplex virus that often begins with mild eye redness, light sensitivity, tearing, or a gritty sensation. Early symptoms can mimic pink eye or dry eye, but untreated ocular herpes can lead to corneal scarring and vision loss.
This Isn’t Just “Pink Eye” And That’s the Problem
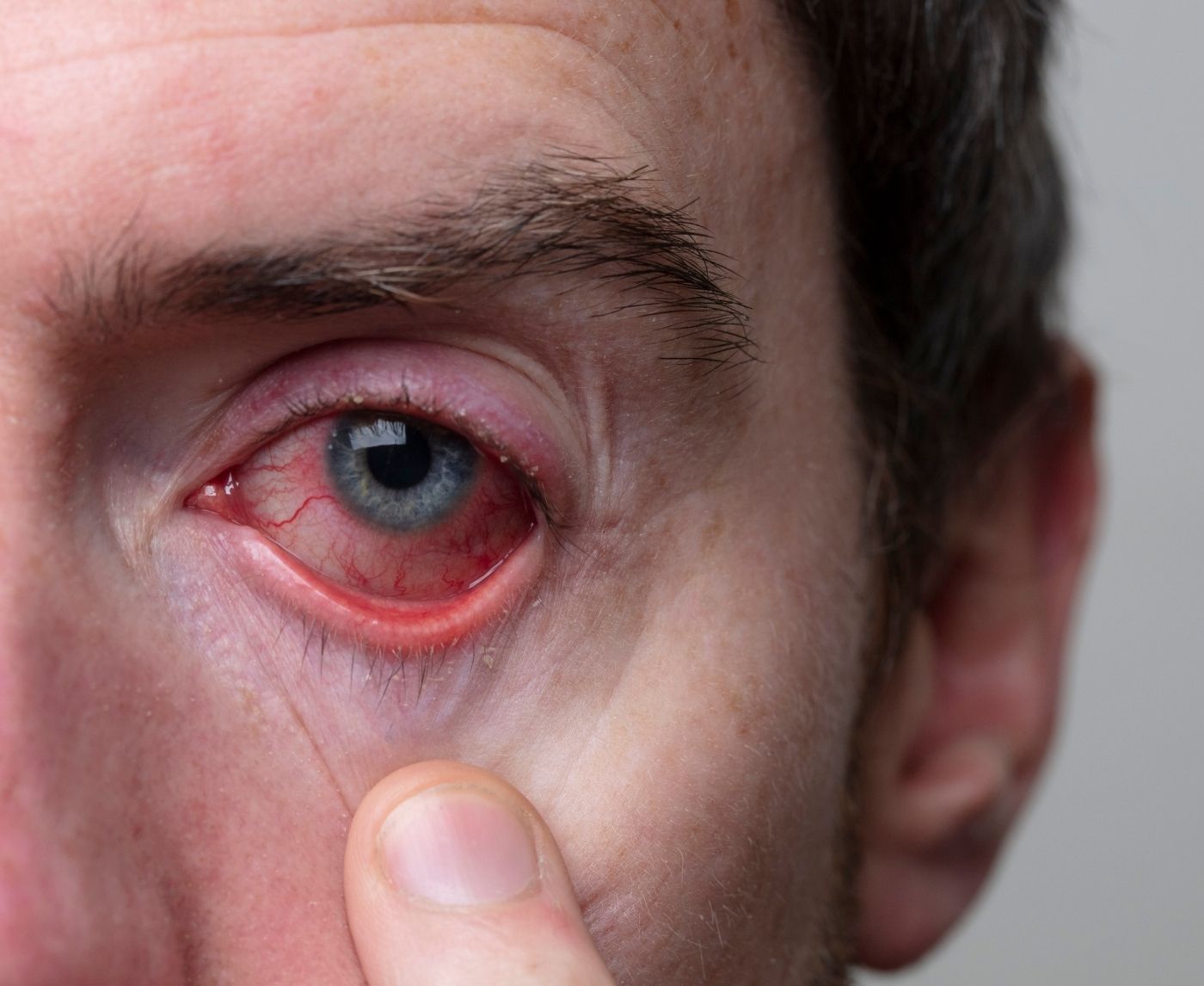
Omar, 27, thought it was pink eye. His right eye was red and watering after a stressful week at work. No thick discharge. No dramatic swelling. Just irritation and light sensitivity that made his commute uncomfortable.
“It didn’t hurt that bad. I figured it was allergies. I even used leftover eye drops from last year.”
Two weeks later, his vision blurred slightly in that same eye. That’s when he went in. It wasn’t bacterial conjunctivitis. It was herpes simplex virus infecting the cornea, ocular herpes.
According to the CDC and ophthalmology guidelines, HSV-1, the same virus responsible for most cold sores, can reactivate and travel along nerve pathways to the eye. Once there, it infects the cornea, the clear dome that allows you to see sharply.
And here’s the quiet truth: most adults carry HSV-1. Many don’t know it. That means herpes in the eye isn’t rare or reckless. It’s biological.
People are also reading: Burning But Not All the Time? Why STD Symptoms Flare and Fade
The Early Signs People Brush Off
The early symptoms of herpes keratitis don’t scream emergency. They whisper. That’s why they’re missed.
People Google things like “eye redness not pink eye,” “dry eye or herpes keratitis,” or “blurry vision herpes.” They’re searching because something feels different, not catastrophic, just persistent.
Figure 1. Subtle early symptoms of herpes keratitis compared to common misattributions.
What makes ocular herpes different from typical pink eye is that it often affects just one eye and tends to recur. It also frequently includes pain that feels deeper than surface irritation, not always severe, but noticeable.
And if you’ve recently had a cold sore, touched your face, or been under stress? That timing matters. HSV reactivates during stress, illness, or immune shifts. It doesn’t require a new exposure.
When Subtle Turns Serious
Left untreated, herpes keratitis can move deeper into the cornea. The infection may create characteristic branching lesions visible under special dye during an eye exam. These dendritic ulcers are classic for HSV infection.
As inflammation increases, vision can blur more noticeably. In severe or recurrent cases, corneal scarring can occur. That’s when permanent vision changes become possible.
This is why early recognition matters. Not because you should panic, but because timing protects vision.
If redness and light sensitivity persist for more than a few days, especially in one eye, especially with a history of cold sores, it deserves evaluation.
How the Cold Sore Virus Reaches the Eye
Let’s get one thing straight. You can get herpes in the eye even if you don’t have genital herpes. And the most common cause is HSV-1, the same virus responsible for oral cold sores.
The virus is dormant in nerve cells after the initial infection. When the virus reactivates, often in response to stress, fever, sun exposure, or hormonal changes, it can travel down nerve pathways to the eye.
Yes, you can spread the disease by touching the cold sore and then the eye. But many cases of herpes simplex virus in the eye are not the result of poor personal habits. This is important because shame can cause people not to get medical help. Biology doesn’t need blame.
If you’re wondering, “Can cold sores spread to the eye?” the answer is yes, but usually through reactivation rather than dramatic transfer events.
How Doctors Tell the Difference, And Why It Matters
One of the most dangerous myths about herpes keratitis is that it looks dramatic right away. It usually doesn’t. Early ocular herpes can resemble viral conjunctivitis so closely that even primary care providers sometimes treat it as routine pink eye at first.
Lina, 34, was given antibiotic drops during her first visit. They didn’t help. Her redness improved slightly, then returned with sharper pain and stronger light sensitivity.
“It felt deeper the second time. Not just irritated. Almost like pressure behind my eye.”
That distinction, surface irritation versus deeper corneal inflammation, is often the turning point in diagnosis.
Ophthalmologists use a fluorescein dye test, placing a special stain in the eye that highlights corneal damage under blue light. Herpes keratitis often creates branching, tree-like patterns called dendritic lesions. These patterns are highly suggestive of infection with the herpes simplex virus.
Unlike simple pink eye, which typically produces thick discharge and affects both eyes over time, herpes in the eye often remains unilateral and may cause reduced corneal sensation. That detail alone can change the diagnosis.
Pink Eye vs. Ocular Herpes: The Overlap That Confuses People
When people search “eye herpes vs pink eye,” they’re usually trying to avoid overreacting. They want reassurance. But what they actually need is clarity.
Figure 2. Clinical differences between pink eye and herpes keratitis.
Notice what’s subtle: nothing in the early column screams emergency. That’s why people wait.
The risk is not in the first red day. The risk is in ignoring persistence.
Is Herpes Keratitis Serious?
This is one of the most searched questions: “Is herpes keratitis serious?” And the answer, although somewhat unpleasant, is: “Yes, it is serious, but not in the way people fear.”
It is serious because it affects the cornea, and recurrent attacks can lead to cumulative scarring. In severe cases, it can lead to stromal keratitis, in which deeper layers of the cornea are affected, and there is a risk of loss of vision.
But, of course, there is a level of reality: “If treated appropriately and in a timely fashion, antiviral medications can clear up the infection.”
Fear is a healthy emotion, and fear can lead to care, so fear of herpes keratitis can lead to care for your eyes.
People are also reading: Can I Test for STDs While on PrEP? What Changes
Why It Comes Back, The Recurrence Factor
Herpes simplex virus doesn’t leave the body. After the initial infection, often childhood exposure, it retreats into nerve cells. It can reactivate years later.
Triggers for recurrence often include:
Stress. Fever. Sun exposure. Hormonal shifts. Immune suppression.
Darius, 41, had his first ocular herpes episode during a high-stress divorce.
“I hadn’t had a cold sore in years. I didn’t even connect the two.”
That connection matters. Many people with herpes in the eye never had noticeable oral outbreaks. They carry HSV-1 silently.
Recurrence rates vary, but ophthalmology data suggests that roughly one in three patients will experience another episode within several years. That’s not a moral failing. It’s viral biology.
What Treatment Actually Looks Like
The treatment for herpes keratitis consists of antiviral medications, which can be obtained only by prescription. This can be antiviral eye drops, such as trifluridine, or antiviral tablets, such as acyclovir.
These medications work by stopping the virus from replicating. They do not cure the virus, which remains inside the body, but the medication helps alleviate the symptoms.
In some cases, the virus can penetrate the cornea, and the patient might require steroid eye drops, which can be obtained only with the guidance and supervision of an ophthalmologist. This is because steroids can actually stimulate the virus.
Most cases of herpes keratitis that occur on the epithelial layer can be cleared up in two to three weeks with proper treatment. The only factor that determines the outcome is the timing.
What This Means for People Living With HSV
If you have a history of cold sores or have tested positive for herpes simplex virus, this article isn’t meant to scare you. It’s meant to inform you.
Most people with HSV will never develop herpes keratitis. But awareness changes outcomes. If you experience unexplained eye redness with light sensitivity, especially in one eye, it deserves evaluation sooner rather than later.
And if you’re navigating questions about HSV status more broadly, clarity matters there too. You can explore discreet at-home options through STD Test Kits, including reliable testing for common STDs that often overlap in online search anxiety.
Testing doesn’t equal stigma. It equals information. And information protects you
How to Protect Your Vision If You Carry HSV
Most people who carry herpes simplex virus will never develop herpes keratitis. That’s important to say out loud. HSV-1 is extremely common worldwide, and ocular involvement is far less common than oral outbreaks.
But if you’ve ever had a cold sore, or suspect you carry HSV, awareness becomes your protective tool. Not paranoia. Not fear. Awareness.
The virus lives in nerve tissue. It reactivates when your immune system is under strain. That means prevention is less about perfection and more about resilience.
Sleep. Stress management. Protecting your eyes from excessive UV exposure. Avoiding contact lens use during active outbreaks. Seeking care quickly if symptoms begin. These aren’t dramatic interventions. They’re practical ones.
Contact Lenses, Micro-Trauma, and Risk Amplifiers
Contact lens wearers need to pay particular attention. The cornea is delicate. Micro-abrasions from overwear or poor hygiene can create vulnerability that makes viral reactivation more disruptive.
This does not mean contact lenses cause herpes in the eye. It means the cornea under stress becomes more susceptible to complications.
If you develop eye redness and light sensitivity while wearing lenses, remove them immediately and do not resume use until evaluated. Continuing lens wear during active inflammation increases the risk of deeper corneal involvement.
Think of the cornea like a windshield. Small cracks may not look severe at first. But repeated impact turns them into fractures.
When You Should Seek Urgent Care, Not Just Routine Care
Not every red eye is an emergency. But certain symptoms require immediate evaluation by an eye specialist.
If you experience sudden worsening pain, noticeable vision loss, extreme light sensitivity, or a white spot on the cornea, that is not a wait-and-see situation. That is same-day care.
Similarly, if you have recurrent “pink eye” that keeps returning to the same eye over months or years, that pattern alone warrants deeper investigation.
Many patients search “can herpes cause blindness” during these moments. The answer is that severe, untreated cases can impair vision. But prompt antiviral treatment dramatically reduces that risk.
Can You Test for Herpes Before It Reaches the Eye?
Here’s the question you’ve all asked at one time or another: If the HSV is hiding away in the body, can you get tested for it before problems arise?
Yes. It is possible to get tested for the presence of HSV-1 and HSV-2 antibodies. These tests do not indicate the location of the HSV in the body. They indicate whether or not you have been exposed.
If you have not been diagnosed with HSV but have reason to believe you have been exposed, especially if you are experiencing unusual symptoms, knowing your HSV status can clarify things.
If you are looking for an alternative and discreet way of getting tested for HSV, the Herpes HSV-1 & HSV-2 Test Kit is an option. It cannot detect ocular herpes, but it can determine if you have the virus that can cause it.
Knowledge is not the cause of disease. It is the cause of preparation.
Recurrence Prevention: What Actually Helps
For people who experience recurrent herpes keratitis, ophthalmologists may prescribe long-term low-dose oral antivirals to reduce recurrence frequency. This is called suppressive therapy.
Studies show that daily oral acyclovir can reduce the risk of recurrent ocular HSV episodes, particularly in patients with prior stromal involvement. That’s not speculation. It’s data-backed prevention.
Triggers differ between individuals, but common recurrence amplifiers include intense stress, systemic illness, ultraviolet exposure, and immune compromise.
If you’ve had one episode, your follow-up plan matters. Many eye specialists schedule routine monitoring even after symptoms resolve.

People are also reading: Burning But Not All the Time? Why STD Symptoms Flare and Fade
Why Early Recognition Is Everything
The difference between mild epithelial herpes keratitis and deeper stromal disease is often timing. Days matter. Sometimes hours matter.
Most early cases are highly treatable. The tragedy is not the virus. The tragedy is dismissal.
When someone searches “eye redness not pink eye” at midnight, they are usually looking for reassurance. What they actually need is informed evaluation if symptoms persist.
Your eyes deserve that respect.
FAQs
1. My eye is red but it doesn’t hurt that much. Could it still be herpes keratitis?
Yes. That’s exactly why people miss it. Early herpes keratitis can feel mild, a little gritty, slightly sensitive to light, maybe just “off.” It doesn’t have to be dramatic to matter. If redness sticks around for several days, especially in one eye, it’s worth getting checked.
2. I had a cold sore last week and now my eye feels irritated. Did I spread it?
Perhaps, but not in the way you think. HSV can reactivate internally via the nerve pathways, and therefore it can still get to your eye even without a hygiene error. Again, it is not about blame. It is about biology. Wash your hands, avoid touching active lesions, and focus on your symptoms, not guilt.
3. Is this going to make me go blind?
That’s the fear everyone Googles at 2 a.m. Severe, untreated cases can cause vision problems, yes. But most people who get prompt antiviral treatment recover without permanent damage. Early care is protective. Panic is not required.
4. How is this different from regular pink eye?
Pink eye often itches or produces discharge and it can spread to both eyes. Herpes keratitis tends to stay in one eye and can cause deeper pain or strong light sensitivity. If it keeps coming back in the same eye, that pattern matters. It’s a clue worth taking seriously.
5. Can stress really trigger herpes in the eye?
Absolutely. Stress, fever, intense sun exposure, hormonal shifts, all can reactivate dormant HSV. Think of it less as something you “caused” and more as a virus responding to immune shifts. Bodies are dynamic. Viruses notice.
6. Will I keep getting this forever?
Not necessarily. Some people have one episode and never again. Others experience recurrences, especially during high-stress stretches. In certain cases, daily antiviral medication can reduce the odds of future flare-ups. There are real, practical options here.
7. What does herpes in the eye actually feel like?
People describe it as a sandy, scratchy sensation, like there’s an eyelash stuck in there that blinking won’t fix. Light may suddenly feel harsher, especially sunlight or phone screens. Vision can look slightly hazy in one eye, like someone smudged the lens. It’s subtle, until it isn’t.
8. Can I wear contact lenses during a flare?
No. Take them out and keep them out until you’ve been evaluated and cleared. The cornea needs a calm, oxygen-rich environment to heal. Contacts during active inflammation can add friction and raise the risk of complications.
9. If I carry HSV-1, should I be worried all the time?
No. Most people with HSV-1 never develop ocular herpes. Awareness is helpful, hypervigilance isn’t. Know the signs, act early if they show up, and then let yourself live like a normal human again.
10. Is this something I should feel embarrassed about?
No. HSV-1 is extremely common, and plenty of people pick it up in childhood. Herpes keratitis is a medical condition, not a character report card. Getting care quickly is responsible, not shameful.
If Something Feels Off, Don’t Minimize It
You can't get new eyes. These are signs: redness that doesn't go away, light sensitivity that gets worse, and blurred vision in one eye. Not charges. Not punishments. Signs.
You can treat herpes keratitis. Early detection protects eyesight. Putting off care because you're embarrassed or don't think you need it is a bad idea.
If you're trying to figure out more general questions about HSV status, clarity is also important. Find out about private testing options through STD Test Kits. The Herpes HSV-1 & HSV-2 Test Kit lets you test for HSV exposure at home without anyone else knowing about it.
You have a right to know. You should be safe. And you should get care without being ashamed.
How We Sourced This Article: This guide was informed by current clinical guidance from ophthalmology associations, CDC herpes resources, WHO HSV prevalence data, and peer-reviewed research on recurrence and corneal complications. Approximately fifteen medical and lifestyle sources were reviewed to ensure balanced, stigma-free, and medically accurate information. Below are six core references selected for clarity and authority.
Sources
1. American Academy of Ophthalmology – Herpes Keratitis Overview
2. World Health Organization – Herpes Simplex Virus Fact Sheet
3. Mayo Clinic – Eye Herpes (Ocular Herpes)
4. StatPearls – Herpes Simplex Keratitis
5. Cleveland Clinic: Ocular Herpes (Eye Herpes): Symptoms & Treatment
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works on preventing, diagnosing, and treating STIs. He combines clinical accuracy with a direct, sex-positive approach and is dedicated to making reliable health information more widely available.
Reviewed by: [Reviewer Name, Credentials] | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.