Quick Answer: Mouth sores on their own don’t mean you have HIV. Yes, some people with HIV can develop oral symptoms, but those signs aren’t specific enough to tell you anything for sure. If you’re worried, the only real way to get a clear answer is to test at the right time based on your exposure, not just what you’re seeing in the mirror.
This Is Where Most People Spiral: “I Found a Sore… Now What?”
There’s a very specific kind of anxiety that hits when something shows up in your mouth. It’s visible. It’s sensitive. And it feels connected to everything, your immune system, your last sexual experience, your worst-case scenario.
One person described it like this:
“I had a tiny ulcer near my gum. It didn’t even hurt that much, but I couldn’t stop thinking about it. I kept checking it in the mirror, Googling ‘HIV mouth symptoms’ over and over.”
This reaction is incredibly common. Mouth lesions trigger anxiety because they feel like a signal. But here’s the truth: most mouth sores are not HIV-related, even if they show up after a sexual encounter.
What matters isn’t just what you see, it’s the bigger picture. Timing. Type of exposure. Other symptoms. And whether testing has been done within the right window.
What Mouth Lesions Can Actually Be (And Why HIV Isn’t the Default)
Before jumping to HIV, it’s important to understand how many everyday things can cause lesions, ulcers, or changes in the mouth. The mouth is one of the most reactive environments in the body. Stress, friction, minor injuries, and even spicy food can trigger visible changes.
Here’s a breakdown of the most common causes people confuse with HIV symptoms:
Notice something important here: several sexually transmitted infections, not just HIV, can affect the mouth. In fact, oral herpes and syphilis are far more likely causes of mouth sores than HIV.
And even beyond STDs, everyday triggers like biting your cheek or brushing too hard can create lesions that look alarming but heal on their own.
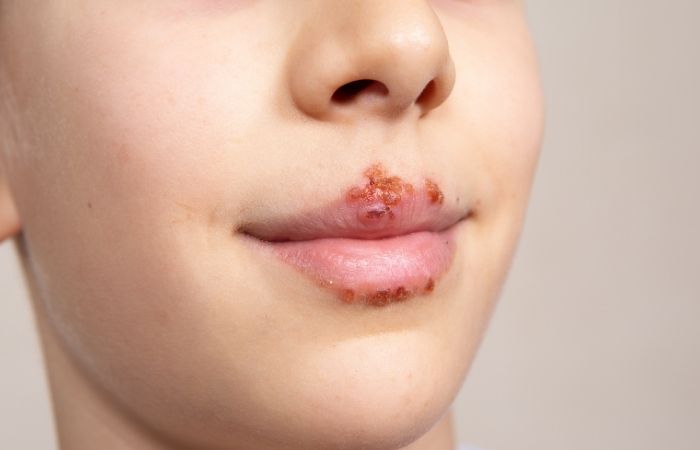
People are also reading: How Soon After Sex Can You Test for HSV-1 or HSV-2?
So… When Is HIV Actually Connected to Mouth Symptoms?
Here’s where things get more nuanced, and where most internet searches go wrong.
HIV doesn’t usually show up as a single, random mouth sore. When oral symptoms do happen, they tend to appear in specific contexts, often alongside other signs or later in the infection timeline.
There are two main situations where HIV-related mouth changes might appear:
1. During Early HIV (Acute Infection Phase)
This phase happens 2–4 weeks after exposure. Some people develop flu-like symptoms, fever, sore throat, fatigue. In a smaller number of cases, mouth ulcers or throat irritation can occur.
But here’s the key: they don’t happen in isolation. If HIV is causing mouth symptoms this early, it’s usually part of a bigger picture that feels like a full-body illness.
2. In Later or Untreated HIV
This is where oral symptoms become more clear. Conditions like oral thrush, persistent ulcers, or unusual lesions can appear when the immune system is weakened.
But this stage doesn’t happen overnight. It develops over time without treatment. For someone recently exposed, this is not what you’re seeing.
“I thought the white patch on my tongue meant I had HIV. Turns out it was thrush from antibiotics. I had already convinced myself it was something way worse.”
The takeaway: timing matters more than the symptom itself.
The Part Most People Miss: Mouth Lesions Don’t Diagnose HIV, Tests Do
It’s tempting to treat symptoms like clues you can decode. But HIV doesn’t work that way. There’s no reliable way to look at a mouth lesion and determine whether HIV is present.
This is where testing becomes everything. Not random testing, but testing based on the right window period.
If you’re noticing mouth symptoms but haven’t tested within the correct window, the symptom itself doesn’t give you answers. It just creates more anxiety.
Testing does the opposite. It replaces guessing with clarity.
After Oral Sex, Everything Feels Suspicious, Here’s What Actually Matters
A lot of people start worrying about HIV specifically after oral sex. It’s one of the most common triggers for this exact question: “I have a mouth sore, should I test?”
Here’s the grounded reality:
HIV transmission through oral sex is extremely low risk. Not zero, but significantly lower than vaginal or anal sex. Even then, it is still rare, but things like open wounds, ejaculating in the mouth, or having an infection can slightly raise the risk.
What’s much more likely after oral sex?
- Herpes (HSV-1 or HSV-2): especially if there was skin-to-skin contact
- Syphilis: can present as a painless sore in the mouth
- Irritation: friction, minor trauma, or sensitivity
This is why focusing only on HIV can actually distract from more likely explanations.
If something shows up in your mouth after oral sex, the smarter question isn’t just “Is this HIV?”, it’s:
“What should I test for, and when?”
When You Should Actually Get Tested (Even If You’re Not Sure)
Testing isn’t about panic, it’s about timing and context. You don’t need to wait for symptoms, and you don’t need to assume the worst. You just need a clear reason and the right window.
You should consider HIV testing if:
- You had unprotected vaginal or anal sex
- You’re within a known exposure window
- You’re experiencing flu-like symptoms after risk
- You want peace of mind after any sexual encounter
And importantly: you do not need mouth lesions to justify testing.
If anything, relying on symptoms alone delays testing, and keeps you stuck in that loop of uncertainty.
Not All Mouth Symptoms Feel the Same, Here’s How to Read the Pattern
One of the biggest mistakes people make is treating all mouth lesions like they mean the same thing. But your body doesn’t speak in single symptoms, it speaks in patterns. And once you start paying attention to those patterns, the anxiety usually starts to loosen its grip.
A random ulcer that shows up, hurts for a few days, and disappears? That behaves very differently from something that spreads, persists, or comes with other systemic symptoms.
Let’s break that down in a way that actually reflects real-life experiences, not just textbook definitions.
The key takeaway here is simple but powerful: HIV-related oral symptoms almost never show up alone. If your only symptom is a mouth sore, that dramatically lowers the likelihood that HIV is the cause.
The Internet Will Tell You Everything Is HIV, Here’s Why That’s Misleading
If you’ve been Googling phrases like “mouth lesions HIV” or “white tongue HIV or thrush,” you’ve probably noticed something frustrating: every result feels alarmist. Every symptom seems to loop back to HIV, even when it shouldn’t.
That’s not because your situation is high-risk, it’s because search engines prioritize worst-case scenarios. They’re designed to answer possibilities, not probabilities.
“Every article I read made it sound like any mouth issue could be HIV. I didn’t realize how rare that actually was without other symptoms or risk.”
Here’s what those articles often leave out:
Most people with HIV don’t diagnose it from a mouth symptom. They find out through testing, often before any visible symptoms appear at all.
And even when oral symptoms do happen, they’re usually part of a broader clinical picture, not a standalone clue you can interpret on your own.
Let’s Talk About Oral Thrush, The Symptom That Freaks People Out the Most
Few things trigger HIV anxiety faster than seeing a white coating on your tongue. It’s one of the most searched symptoms for a reason. It looks unusual, it feels unfamiliar, and it’s often linked online to immune system issues.
But oral thrush is not exclusive to HIV. Not even close.
It can show up after:
- Taking antibiotics
- Using inhaled steroids (like asthma meds)
- Dry mouth or dehydration
- High stress or disrupted sleep
Yes, it can also appear in people with untreated HIV, but context matters. In those cases, it tends to be persistent, widespread, and accompanied by other signs of immune suppression.
If you woke up with a white tongue after a stressful week or a course of antibiotics, that’s a very different scenario than someone with advanced immune changes.
The visual alone doesn’t tell the story. The timing does.
What Testing Actually Does (That Symptom Checking Never Will)
There’s a quiet shift that happens when someone moves from symptom-checking to testing. It’s the difference between guessing and knowing. And for most people, that shift brings relief, even if they were scared to take it.
Symptoms are ambiguous. Testing is definitive.
If you’re in that loop of checking your mouth, checking your body, checking Google, this is where you break it.
Test based on your exposure, not your fear.
If your last possible risk was recent, you may need to wait for the appropriate window. If enough time has passed, a test can give you a clear answer today.
And if you’re not sure what you were exposed to? That’s more common than people admit.
In that case, using a broader option like a combo STD home test kit can check for multiple infections at once, including HIV, syphilis, and others that are more likely to cause mouth symptoms.
Because sometimes the question isn’t just “Is this HIV?”, it’s “What else could this be?”
People are also reading: Herpes Symptoms but Negative Test? Read This First
“But What If I Miss Something?”, The Fear That Keeps People Stuck
This is the part most people don’t say out loud.
It’s not just about the sore. It’s about the fear of missing something serious. Of ignoring a warning sign. Of finding out too late.
“I kept thinking, what if this is the one symptom I shouldn’t ignore? What if I brush it off and regret it?”
That fear makes sense. But it can also lead to overinterpreting normal body changes as signs of something severe.
The balance is this:
Pay attention, but verify.
Don’t ignore symptoms. But don’t assign them meaning without evidence either. That’s what testing is for. It grounds the situation in reality instead of possibility.
When Mouth Lesions Should Actually Push You to Act
Most mouth sores are harmless. But there are situations where they should prompt you to take the next step, not because they mean HIV, but because they’re part of a bigger picture worth checking.
You should take action if:
- The lesion lasts longer than 2–3 weeks
- You have multiple symptoms (fever, fatigue, sore throat)
- You had a recent high-risk exposure
- The sore is painless and unusual in appearance
Notice that last point. A painless sore, especially after oral contact, can be more suggestive of syphilis than HIV. And that’s something many people completely overlook while focusing only on HIV.
This is why broad testing, not narrow assumptions, leads to better outcomes.
A Practical Decision Guide (Without the Guesswork)
Let’s strip this down to something usable. Not theory, real-world decision-making you can apply today.
This isn’t about dismissing your concern. It’s about putting it in the right category. Most people fall into that first or second row, and spend days assuming they’re in the third.
The Timing Piece No One Explains Clearly Enough
Even when someone decides to test, there’s another layer of confusion: “What if I test too early?”
This is where a lot of unnecessary retesting, and anxiety, comes from.
HIV tests don’t detect infection immediately after exposure. There’s a window period where the virus isn’t yet detectable, even if it’s present. Testing during that window can give you a false sense of security, or keep you stuck in uncertainty.
Here’s the part that matters:
If your mouth sore showed up a few days after exposure, it’s too early for that symptom to be a reliable indicator of HIV. And it’s also likely too early for most tests to detect anything.
That doesn’t mean ignore it. It means plan your testing instead of reacting impulsively.
A well-timed test is more valuable than three early ones driven by panic.
What Taking Control Actually Looks Like
There’s a moment in this process where things shift. You stop trying to decode symptoms and start choosing clarity instead.
That might look like:
- Waiting until the right testing window instead of testing too early
- Choosing a comprehensive test instead of guessing which infection to check
- Getting answers privately without delaying out of fear or stigma
For a lot of people, the barrier isn’t access, it’s hesitation. Not wanting to know. Or not wanting to deal with what comes next.
But the reality is, most results bring relief, not bad news.
And even when something does come back positive, it’s manageable, treatable, and far less overwhelming than the uncertainty that came before it.
FAQs
1. I found a mouth sore and immediately thought HIV… am I overreacting?
Honestly? You’re reacting like a human with internet access. A lot of people jump straight to HIV because it’s the scariest possibility, not the most likely one. In reality, a random mouth sore is almost always something minor like a canker sore or irritation, not HIV.
2. What do HIV-related mouth symptoms actually feel like?
They usually don’t show up quietly. When HIV causes symptoms early on, people tend to feel genuinely sick, fever, body aches, sore throat, like a rough flu. A single spot in your mouth without anything else going on doesn’t fit that pattern.
3. I have a white tongue… should I be worried about HIV?
Not by default. White tongue (thrush) can show up after antibiotics, stress, dehydration, or even just a rough week of not sleeping well. It becomes more concerning when it’s persistent and paired with other symptoms, but on its own, it’s rarely pointing straight to HIV.
4. How long after a risky situation would mouth symptoms from HIV show up?
If they show up at all, it’s usually around 2–4 weeks after exposure, and even then, they don’t come alone. Think “I feel sick everywhere,” not “I have one weird sore.” Timing plus full-body symptoms matters way more than one spot in your mouth.
5. Be real, can you get HIV from oral sex?
The risk is very low. Not zero, but low enough that most doctors don’t consider it a common transmission route. What is common after oral sex? Herpes, irritation, or even just a sore from friction, things that look scary but aren’t HIV.
6. If it’s not HIV, what’s the usual culprit behind mouth sores after sex?
Herpes and syphilis are the two big ones doctors actually think about. Herpes tends to hurt and come in clusters. Syphilis can be sneaky and painless. Both are testable and treatable, and way more likely than HIV in this scenario.
7. My sore is already going away… does that mean I’m in the clear?
It’s a good sign, yeah. Most harmless sores heal within a week or two and don’t come back. But if there was a real exposure risk, testing is still the move, not because something’s wrong, but because guessing only gets you so far.
8. I keep checking my mouth in the mirror… how do I stop spiraling?
You replace guessing with a plan. Figure out your exposure risk, mark the right testing window, and commit to testing once you’re in it. That’s how you get out of the loop, because right now, you’re trying to solve something symptoms can’t answer.
9. Should I test even if the risk feels low?
If it’s going to keep you up at night, yes. Testing isn’t just medical, it’s mental clarity. A low-risk situation plus a negative test is often what finally lets your brain exhale.
10.What’s the smartest move if I’m still unsure?
Don’t try to diagnose yourself from symptoms alone. Pick a test that covers your bases, take it at the right time, and let the result speak for itself. That’s how you go from “what if” to “now I know.”
You Deserve Clarity, Not Guesswork
Mouth sores can feel loaded. Not just physically, but mentally. They turn into questions, then into worst-case scenarios, then into late-night searches that never really answer anything. The goal isn’t to panic over every change in your body. The goal is to separate what matters from what doesn’t.
If there was real risk, test. If the timing isn’t right yet, plan your test instead of guessing. If symptoms are lingering, expand the scope and check for what’s actually more likely, not just what’s most feared. Each step replaces uncertainty with something solid.
Don’t sit in “what if.” If you want a clear answer, start with a private, reliable option like the Combo STD Home Test Kit. It covers HIV and other common infections, so you’re not left wondering what you missed. Clarity doesn’t just inform you, it settles you.
How We Sourced This Article: This guide combines clinical guidelines on HIV and oral health with peer-reviewed research on how infectious diseases manifest in the oral cavity and actual patient concerns. We verified the information we obtained from public health agencies, infectious disease research, and sexual health education websites to ensure its accuracy. The emotional framing reflects common patient experiences, especially regarding anxiety related to symptoms and options for testing.
Sources
1. World Health Organization – HIV/AIDS Fact Sheet
2. Mayo Clinic – HIV/AIDS Overview
4. PubMed – Oral Manifestations of HIV Research
5. Planned Parenthood – HIV Information
6. Centers for Disease Control and Prevention – Syphilis Fact Sheet
7. Centers for Disease Control and Prevention – Genital Herpes Fact Sheet
About the Author
Dr. F. David, MD is a board-certified infectious disease doctor who specializes in preventing, diagnosing, and treating STIs. He has a direct, sex-positive approach that puts clarity, privacy, and patient empowerment first, along with clinical accuracy.
Reviewed by: Michael R. Levin, MD, Infectious Disease Specialist | Last medically reviewed: March 2026
This article is just for information and shouldn't be used in place of medical advice.






