Is It Your Period or an STD? Signs You Shouldn’t Ignore
Quick Answer: DoxyPEP may still lower STD risk, but new 2026 data links it to rising gonorrhea resistance. Talk to your provider about alternatives if you use it regularly.
Who This Is For, and Why It Matters in 2026
If you’ve ever left a hookup wondering, “Should I take something just in case?”, this article is for you. If you’ve used DoxyPEP after sex with multiple partners, especially in queer or high-risk communities, you’re also the audience. And if you're just now hearing the word “DoxyPEP” for the first time, welcome to one of the most important, and complicated, topics in modern sexual health.
In 2024, DoxyPEP started showing promise in reducing bacterial STDs like chlamydia, syphilis, and even gonorrhea among high-risk populations. But by late 2025, reports of increasing tetracycline-resistant gonorrhea began to circulate in peer-reviewed journals. In 2026, the data is stronger, and it's forcing a real conversation about trade-offs.
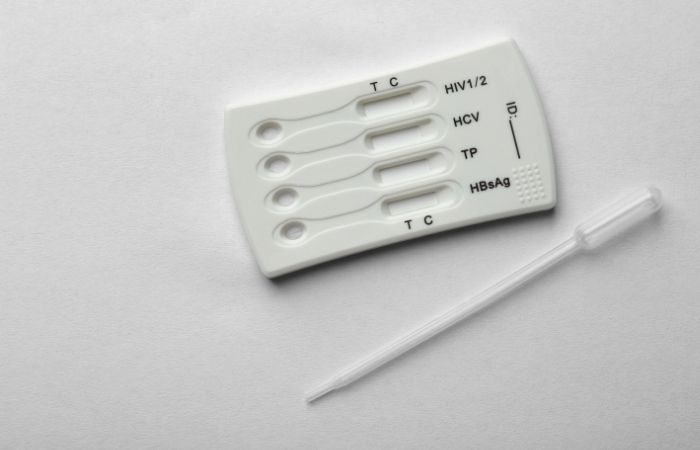
Testing, not just treatment, is at the core of staying safe. And while DoxyPEP might feel like a shortcut, it doesn’t replace regular STD testing. That’s why thousands of people are turning to discreet, at-home kits like the Combo STD Home Test Kit to stay ahead of infections while keeping resistance in check.
People are also reading: Hepatitis C Can Live in You for Years, Here’s How It Goes Undetected
What Is DoxyPEP, Exactly?
DoxyPEP stands for doxycycline post-exposure prophylaxis. It's not a new drug, but a new way of using an old one. The idea is to take a single 200mg dose of doxycycline within 72 hours after unprotected sex to reduce your chances of contracting certain bacterial STDs. Studies have shown it can cut down infections by up to 60% in specific populations, especially cisgender men who have sex with men and transgender women using PrEP for HIV prevention.
But here’s the catch: Doxycycline belongs to a class of antibiotics that bacteria can adapt to. Unlike HIV or herpes, which are viruses, gonorrhea is a fast-mutating bacterium. And it’s already notorious for evading nearly every antibiotic we’ve thrown at it. That includes penicillin, ciprofloxacin, and now, maybe, doxycycline too.
This matters not just for individual health, but for public health. If DoxyPEP drives resistance, we could lose one of the last semi-reliable treatment options for gonorrhea. And that’s a problem bigger than one pill after sex.
What the New Research Says in 2026
A landmark 2026 multicenter surveillance study published in the journal Sexually Transmitted Diseases tracked DoxyPEP users across six U.S. cities. It found that among regular users, those taking DoxyPEP more than four times per month, there was a 35% higher rate of infection with tetracycline-resistant Neisseria gonorrhoeae compared to non-users. These weren’t mild resistance patterns, either. In several cases, the bacteria were resistant at levels high enough to render doxycycline useless.
One of the study’s lead researchers, Dr. Renita Cho of the CDC, was quoted saying: “We’re seeing resistance levels that weren’t present even two years ago. While DoxyPEP may reduce short-term infections, the long-term cost could be catastrophic if gonorrhea becomes untreatable.”
Additional studies in France and Australia have mirrored these concerns, with similar spikes in resistance among populations using DoxyPEP routinely. While causation hasn’t been fully proven, the correlation is strong enough that many health agencies are revisiting their guidelines.
CDC guidance on DoxyPEP was updated in late 2025 to recommend “individualized risk-benefit assessments,” especially in communities where resistance is already high. In other words, proceed with caution.
“DoxyPEP Saved Me, Then Gave Me a Superbug”
Marco, 32, a queer man living in Los Angeles, was prescribed DoxyPEP through a telehealth platform in 2024.
“It felt like freedom,” he said. “I didn’t worry as much about getting chlamydia or syphilis again.”
But by early 2026, Marco tested positive for gonorrhea, again. This time, treatment wasn’t easy. “They gave me a shot and oral meds, but it didn’t go away. The cultures showed high-level resistance. They said the only reason they knew what to give me next was because the lab flagged it early.”
Marco hasn’t stopped having sex, and he doesn’t blame DoxyPEP. But he’s now cautious. “I still believe in harm reduction. But I test more often, and I don’t take DoxyPEP unless I know there was a real risk. It’s not my go-to anymore.”
Are There Safer Alternatives to DoxyPEP?
For people at high risk of exposure to bacterial STDs, DoxyPEP was never meant to replace routine testing, condom use, or partner communication. It was a backup plan, a tool in the harm reduction toolbox. But now, with resistance trends becoming a serious concern, it's worth asking: what else is out there?
Some sexual health experts now suggest a more "test-forward" way of doing things. This means that people in high-risk groups should get tested every three to six weeks and only use targeted antibiotics when they are needed. Some people say to stop using doxycycline and try other ways to prevent the disease, such as:
Figure 1. Alternatives and add-ons to DoxyPEP for reducing STD risk. These strategies support prevention without contributing heavily to bacterial resistance.
It’s important to note that none of these are perfect on their own. DoxyPEP was popular in part because it felt simple and empowering. Replacing it means leaning into slightly more complex plans, but ones that are likely safer long-term.
This Isn’t Just About You, Why Resistance Spreads Quietly
You might be thinking, “Okay, I’ve used DoxyPEP a few times. What’s the big deal?” The issue isn’t one person, it’s population-level pressure. Every time Neisseria gonorrhoeae encounters antibiotics, it learns. And the more it learns, the harder it is to treat.
Gonorrhea is a uniquely aggressive pathogen. Unlike some STDs, it can mutate rapidly and share resistance genes with other bacteria. This means what starts in one community can travel fast, geographically and sexually. And because gonorrhea often shows no symptoms, people spread it unknowingly.
In the 2026 surveillance data, resistance didn’t stay confined to one demographic. While queer male DoxyPEP users showed the fastest spike, the resistant strains are now appearing in heterosexual networks, rural areas, and even among people who’ve never taken DoxyPEP at all. This is the ripple effect, and it’s why the conversation matters beyond any one group.
In a world where multi-drug resistant gonorrhea is already on the CDC’s list of “urgent threats,” adding pressure with post-sex antibiotics may accelerate a tipping point we can’t undo.
Tracking the Rise of Resistance: 2022 to 2026
The story of antibiotic resistance isn’t new, but what’s happening with tetracycline-class resistance is alarming in pace and scale. Below is a simplified table comparing resistance levels by year in key regions where DoxyPEP trials and usage have been concentrated.
Figure 2. Rising tetracycline resistance in Neisseria gonorrhoeae alongside increased DoxyPEP use. Data synthesized from CDC, NIH, and regional health department reports.
The takeaway? While DoxyPEP may reduce individual infections today, its broad use may be helping build the next superbug tomorrow.
Should You Stop Taking DoxyPEP Completely?
This is where things get hard. Some people still think DoxyPEP is worth the risk, especially if they've had more than one STD in the last year, have trouble getting regular tests, or are part of a network with a lot of transmission. But that doesn't mean it's the best tool for everyone or for all time.
Medical providers are beginning to shift toward a more nuanced model: selective use. Rather than a blanket yes or no, DoxyPEP is increasingly framed as something to use strategically, not habitually. If your provider hasn’t updated your DoxyPEP plan since 2025, now’s the time to check in.
Here’s the core message: this isn’t about shaming prevention, it’s about making sure that prevention doesn’t backfire. And if you’re testing regularly, using barriers, and staying informed, you’re already doing most of what DoxyPEP was meant to support.

People are also reading: Tested Positive for Trich? Here’s How to Treat It Safely at Home
What Experts and the CDC Are Saying in 2026
The public health community isn’t united on DoxyPEP, and that’s telling. Some clinicians continue prescribing it under tight conditions. Others have paused entirely. But what most agree on is this: we need more personalized decision-making and better public education on the trade-offs.
The CDC’s latest update from late 2025 stops short of recommending DoxyPEP broadly. Instead, it encourages providers to weigh the pros and cons on a case-by-case basis, especially in communities already facing high levels of antibiotic resistance. It also underscores that DoxyPEP is not a replacement for regular screening or barrier protection.
Dr. Sienna Reyes, an infectious disease expert with Johns Hopkins, said in a recent webinar: “We can’t afford to treat prevention like a pill-only strategy. DoxyPEP was a breakthrough, but it was never meant to be a forever solution. We need to think long-term, and that means shifting focus back to education, testing, and community-specific prevention plans.”
Several LGBTQ+ health clinics, especially those in San Francisco, New York, and Atlanta, have begun offering structured DoxyPEP counseling. Patients get resistance education alongside prescriptions, and they’re encouraged to use rapid tests in between doses to limit blind spots.
Should You Still Take DoxyPEP? Let’s Talk Real-Life Decision Making
No one lives in a vacuum. You might have partners who don’t test often. You might live in a rural area without easy access to clinics. You might have health anxiety and feel more in control with a plan. These are all valid. What matters is making a choice that fits your life, without compromising your future options.
Here’s a simple self-check to help guide your decision:
Figure 3. Personalizing your DoxyPEP decision in 2026. The key isn’t elimination, it’s smarter integration.
If you’re feeling overwhelmed, you’re not alone. Plenty of people are rethinking their approach this year. But that’s a sign of empowerment, not failure. You’re allowed to change your mind. You’re allowed to pause. And you’re allowed to ask questions before saying yes to another round of antibiotics.
Whether you continue DoxyPEP or not, the best next move is knowing your status. This at-home combo test kit checks for the most common STDs discreetly and quickly, giving you answers without the clinic wait or the fear spiral.
FAQs
1. Is DoxyPEP still recommended in 2026?
Not across the board. The CDC has backed off from broad recommendations, which is their way of saying: this isn’t a one-size-fits-all tool anymore. If you're in a higher-risk group or have a history of bacterial STDs, it might still make sense, but only if you're also testing regularly. This is the year where nuance matters more than ever.
2. Can DoxyPEP make gonorrhea untreatable?
Not on its own, but it’s definitely nudging us closer to that cliff. The more we expose gonorrhea to doxycycline, the faster it learns how to dodge it. And once those resistant strains spread (and they do), even people who never touched DoxyPEP can end up with a bug that laughs at antibiotics. It’s not about blame, it’s about biology.
3. Are there safer ways to prevent STDs without DoxyPEP?
Totally. Think of DoxyPEP like the “Plan B” of bacterial STDs, not the everyday plan. Condoms still work. Regular rapid testing catches things early. Some folks set testing agreements with partners or test together before play. And yes, DoxyPEP can be used selectively, like after a high-risk encounter, not every weekend.
4. What should I do if I’ve been using DoxyPEP regularly?
Don’t panic, but don’t stay on autopilot either. First, test. Then talk to a provider, ideally one who understands sexual health beyond scare tactics. Bring up resistance. Ask if your area’s seeing spikes. You might be totally fine. Or it might be time to shift strategies before your body starts ignoring doxycycline altogether.
5. Is DoxyPEP still effective for chlamydia and syphilis?
Yes, it’s holding strong, for now. The biggest resistance concern is gonorrhea. But here’s the deal: resistance isn’t polite. If doxycycline keeps getting overused, it could eventually stop working for other STDs too. So the name of the game in 2026? Use it less, use it smart, and always pair it with testing.
6. How do I know if my gonorrhea is resistant?
You probably won’t, unless treatment fails. Most urgent care clinics don’t automatically test for resistance. So if you’ve had gonorrhea, got treated, and symptoms linger or come back (burning, discharge, pelvic pain), get a culture. In some places, you can request resistance testing specifically. It's your body, you’re allowed to ask.
7. Can I take DoxyPEP if I’m already on PrEP?
Yes, and many do. But stacking meds has consequences, even if they’re both prevention tools. Talk to your provider about how often you’re taking DoxyPEP, and if you’re also on PrEP, make sure your kidneys and gut are getting some love too. Harm reduction means harm awareness, not harm stacking.
8. Is it safe to take doxycycline multiple times a month?
Technically? Maybe. Strategically? Probably not. The more often you take it, the higher the chance your body, and the bacteria in it, start adapting. Some people report yeast infections, gut issues, even weird skin sensitivities. Plus, frequent use makes resistance way more likely. DoxyPEP isn’t a vitamin. It’s a serious med with consequences.
9. Can DoxyPEP affect vaginal health or the microbiome?
Absolutely. Most DoxyPEP studies focus on people with penises, but anyone with a vagina knows that antibiotics = yeast city, BV territory, and microbiome chaos. If you’re using DoxyPEP and experiencing discharge changes, irritation, or more frequent infections, it’s worth reevaluating. Your body talks, listen closely.
10. How often should I test if I use DoxyPEP?
Every 4 to 6 weeks is a solid rhythm if you’re taking DoxyPEP regularly. More frequent sex with new or multiple partners? Every 3–4 weeks might be better. And hey, testing doesn’t have to mean a waiting room. At-home kits are fast, private, and let you skip the awkward small talk at urgent care.
You Deserve Protection, Not Regret
No one chooses to be part of an antibiotic resistance story. DoxyPEP gave many of us a way to feel safer, freer, and more in control. And in many cases, it worked. But the 2026 data is clear: if we don’t use it wisely, we could lose it altogether, and with it, one more defense against a fast-mutating, globally spreading infection.
This isn’t about fear. It’s about foresight. If you’ve relied on DoxyPEP, that doesn’t make you reckless. But it might be time to update your game plan. Know your options, test often, and talk to a provider who respects your autonomy without minimizing your risk.
Don’t wait and wonder, get the clarity you deserve. This at-home combo test kit checks for the most common STDs discreetly and quickly.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted some of the most relevant and reader-friendly sources.
Sources
1. CDC: Doxy PEP for Bacterial STI Prevention
3. Postexposure Doxycycline to Prevent Bacterial Sexually Transmitted Infections — NEJM (2023)
4. PubMed: CDC Clinical Guidelines on Doxy-PEP (2024)
5. EATG: Concerns About Antibiotic Resistance From Doxy-PEP (2025)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He combines clinical accuracy with a straightforward, sex-positive approach and is dedicated to making it easier for readers to find what they need, whether they live in a city or off the grid.
Reviewed by: Dr. S. Ray, MPH | Last medically reviewed: November 2025
This article is for informational purposes and does not replace medical advice.






