How Soon After Sex Can I Test for Gonorrhea?
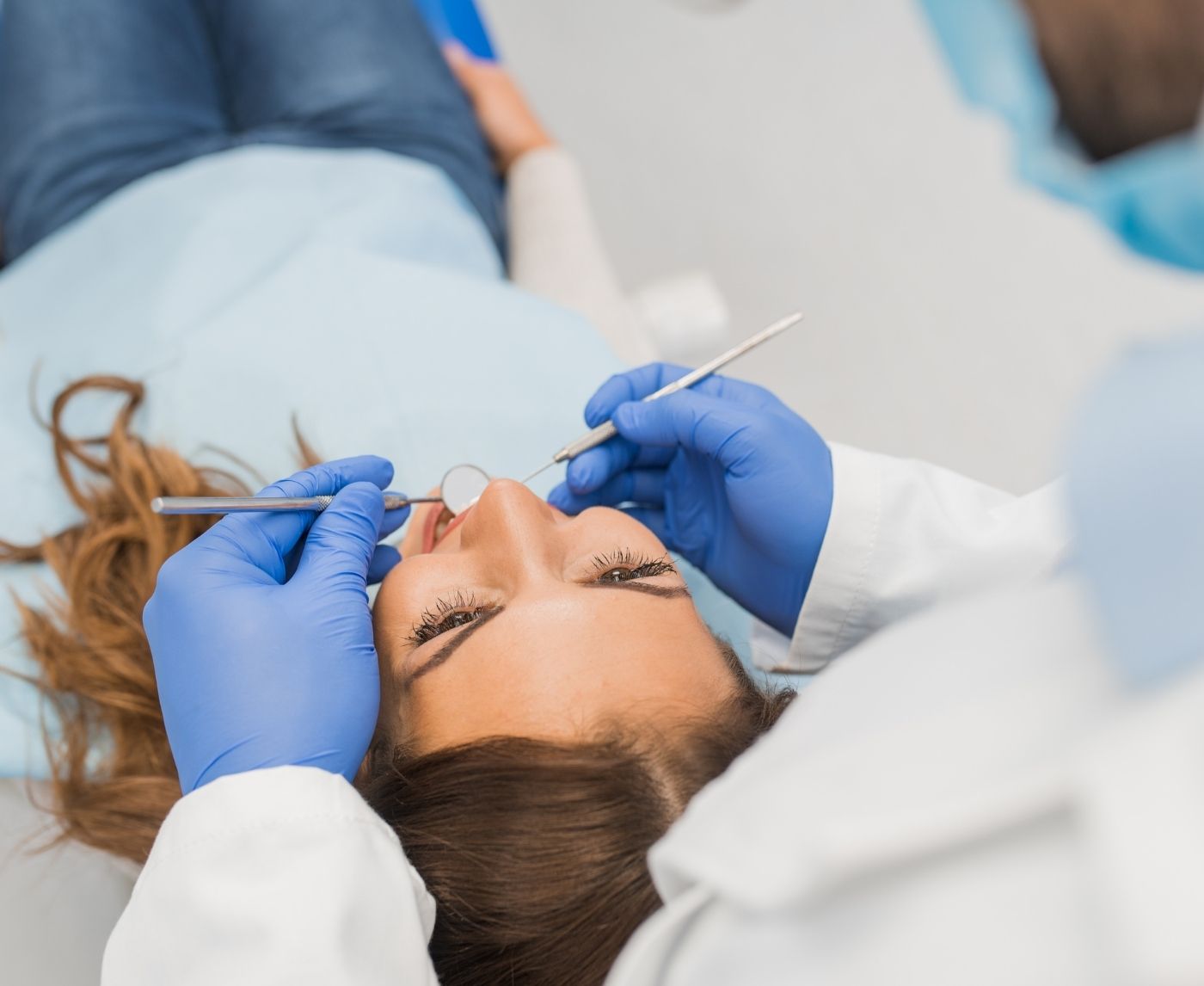
Quick Answer: STD symptoms in the mouth can appear as early as a few days after exposure, often before genital symptoms. Dentists may be the first to notice signs like ulcers, gum inflammation, or white lesions during routine exams.
When Your Mouth Sends the First Signal
For many people, oral sex seems like the “safer” option. No penetration, no risk, right? Not exactly. While it's true that the risk of HIV is lower with oral sex than with vaginal or anal sex, many other STDs transmit easily through the mouth, including gonorrhea, chlamydia, herpes, syphilis, and HPV.
The trouble is, most people don’t associate sore throats or mouth ulcers with STDs. And because oral symptoms are usually mild or mistaken for something else, like strep throat, thrush, or a canker sore, they often go untreated. That’s where dentists come in. Dentists examine areas of the mouth, throat, and tongue that even doctors don’t always inspect. When they see certain lesions, inflammation, or discoloration, they may quietly wonder: Could this be more than just gingivitis?
Case Study: “My Dentist Saw It Before I Did”
Luis, 34, hadn’t noticed much, just a bit of gum irritation and a sore at the back of his throat that hadn’t gone away in weeks. He chalked it up to flossing too hard and a lingering cold. But during his six-month dental cleaning, his hygienist noticed something unusual: a red patch on the roof of his mouth and slight swelling near his tonsils.
“I thought maybe it was just allergies,” Luis recalls. “But the dentist asked if I’d had unprotected oral sex recently. It was kind of awkward, but also validating. He said I should see a doctor and consider getting tested.”
Two weeks later, Luis was diagnosed with oral gonorrhea. He had no genital symptoms at all.
How STDs Appear in the Mouth: A Visual Breakdown
Oral symptoms vary by infection type, but certain patterns tend to show up again and again. Dentists are trained to spot irregularities in the gums, lips, tongue, and tonsils, but most people don’t recognize these as warning signs of an STD.
Table 1. Common oral symptoms of STDs and their typical appearance timelines.
People are aslo reading: STD Testing Before the Wedding: What Couples Should Really Talk About
Why Dentists Are Picking It Up First
Most people aren’t checking their tonsils in the mirror. Dentists, however, routinely look at the soft tissues of the mouth during cleanings and oral cancer screenings. Their training makes them alert to lesions, nodules, and ulcers that deviate from the norm. While they don’t formally diagnose STDs, they can identify red flags that lead to faster medical intervention.
What makes this so important is the subtlety. A herpes blister might resemble a pimple. A syphilis chancre might look like a small nick. Even experienced doctors might miss these if they’re not actively looking. Dentists, though, see the mouth as their primary diagnostic canvas.
And when they do notice something off, many now refer patients for STD testing, especially if the patient reports recent oral sex, a new partner, or sore throat with no fever. This quiet collaboration between dental care and sexual health can be life-changing. And in some cases, life-saving.
Next, we’ll break down exactly which signs to watch for, and when to test, even if you don’t have genital symptoms.
This Isn’t Just a Canker Sore, And Here’s Why
It’s tempting to shrug off a sore in your mouth. Maybe you bit your cheek, ate something acidic, or haven’t been drinking enough water. But when that sore lingers, or if it looks unusual, it’s worth stepping back and asking a different question: Could this be from a recent hookup?
Marina, 29, had recently gotten out of a relationship and was exploring dating again. After giving oral sex to a new partner, she developed what she thought was a heat blister on her inner lip. When it didn’t go away after a week, she grew concerned. By week two, a second sore appeared near her gums. Her doctor assumed it was viral, but her dentist spotted it and quietly suggested an STD test, especially since she’d mentioned a new partner.
“It was the first time anyone had brought up the possibility of herpes,” she says. “The dentist wasn’t judgmental at all. Just factual, and calm.”
She tested positive for oral HSV-1. If she hadn’t mentioned it during her dental visit, she might’ve dismissed the symptoms completely.
STD or Something Else? Here’s How They Compare
Not every mouth sore means you have an STD. But many STDs mimic everyday conditions like strep throat, thrush, allergies, or even dehydration. When symptoms are subtle, or when you’ve never had an oral STD before, it’s easy to mislabel what you’re experiencing.
This table breaks down how oral STDs stack up against more common mouth conditions. It’s not meant to replace medical advice, but it can help you sense when it’s time to test.
Table 2. Symptom comparison between oral STDs and other common mouth conditions.
How Soon After Oral Sex Should You Test?
If you’re experiencing mouth symptoms after oral sex, or if your dentist flagged something unusual, you’re likely wondering: When should I test? The answer depends on which STD you may have been exposed to and how long it’s been since the encounter.
In most cases, oral symptoms show up within 2 to 21 days of exposure. Herpes may appear faster, while HPV may take months. Some infections cause no symptoms at all but can still be passed to partners.
Here’s what matters most: testing too early may lead to false negatives. Testing too late can miss the opportunity for early treatment. If you’re in that uncomfortable “do I or don’t I” window, here’s a general rule:
Wait at least 7–14 days after a possible exposure to test for gonorrhea, chlamydia, or herpes. For syphilis, testing around 3 weeks post-exposure is ideal. And if symptoms show up early? Don’t wait, get tested now, and be prepared to retest later if results are unclear.
Whether you’re dealing with swollen tonsils, a sore that won’t quit, or just an anxious gut feeling, remember this:
Peace of mind is one test away. At-home STD testing lets you get answers privately, without waiting for a clinic slot or explaining everything to a receptionist. If you’re not ready to talk about it, you can still act on it.
Why Oral STDs Are Often Missed
Let’s be honest, oral sex isn’t always discussed during doctor visits. Many people don’t mention it. Many providers don’t ask. And unless you’re specifically tested for throat or mouth infections, they might never be detected.
Oral gonorrhea and chlamydia are often asymptomatic in the throat. HPV can live in the mouth for years before any visible sign appears. Syphilis chancres are painless and might be mistaken for a cheek bite or cold sore. Herpes can feel like a bad pimple or nothing at all.
This silence is how transmission continues. You can be contagious even if you feel fine. And you can carry an infection in your mouth without ever seeing a rash below the belt.
That’s why dentists, those who know your molars better than anyone, are sometimes the only ones catching early warning signs. They’re not diagnosing you. But their alertness might just be the nudge you need to take testing seriously.
What Dentists Actually Say, And Why It Matters
There’s a moment during a dental exam when everything goes quiet. You’re reclined, your mouth is open, and your dentist pauses. Not long. Just enough for your brain to start racing. Then they say something that makes your stomach flip.
“Have you noticed this spot before?”
Most dentists won’t come out and say, “You might have an STD.” That’s not their role. But they may suggest you follow up with a doctor, especially if they see:
- A persistent ulcer that hasn’t healed in two weeks
- Unusual white patches on the tongue or palate
- Redness around the tonsils with no sign of infection
- Small wart-like growths near the gums
- Swelling or bleeding in areas unrelated to brushing habits
Riley, 42, had all of his teeth in great shape, but his dentist still called in the supervising doctor during a routine checkup. “They were both gentle, but honest,” he said. “They told me it might be worth ruling out a sexually transmitted infection. I never expected to hear that while sitting in a dental chair.”
That experience led Riley to get tested. His positive result for oral HPV eventually prompted him to get vaccinated and inform his past partner. That dental visit may have saved more than just a molar.
What Dentists Are Trained to Look For (Even If You’re Not)
Dentists spend thousands of hours learning how to read the inside of the mouth. They’re trained to spot early signs of oral cancer, chronic inflammation, trauma, and increasingly, symptoms that align with oral STDs. They can’t diagnose or prescribe STD treatments, but they’re often the first medical professional to raise the alarm.
Here’s what typically catches their attention:
- A single, clean-edged ulcer that’s painless (a syphilis chancre)
- Clustered blisters or fluid-filled lesions (herpes simplex)
- White, flat lesions that don’t scrape off easily (HPV or HIV-related)
- Throat redness or pustules on the tonsils with no fever (gonorrhea)
- Wart-like bumps on the lips or tongue (HPV subtypes)
They also ask about oral hygiene habits. Not to shame, but to narrow down causes. If your hygiene is solid, your immune system is normal, and a sore isn’t healing, infection becomes a suspect.
That’s when they may gently say: “This doesn’t look typical. I think it’s worth getting a second opinion.” You don’t need a diagnosis in that moment. But you now have a starting point.
People are aslo reading: How mRNA Tech Could Bring Us the First Chlamydia Vaccine by 2028
Should You Test at Home or See a Doctor?
That depends on what you’re feeling, and how urgently you want answers. Home testing is discreet, fast, and accurate for many oral STDs. If you’re feeling sore, see spots, or recently gave or received oral sex without protection, home kits can help you take control before symptoms worsen.
But if your dentist notices something serious, or you’re experiencing multiple symptoms at once, it’s worth seeing a doctor. Especially if you have:
- Fever or fatigue along with oral sores
- Swelling in the neck or jaw
- Open sores that bleed or ooze
- Difficulty swallowing or speaking
These aren’t just red flags, they’re reasons to act now. The good news? Testing doesn’t have to be public, painful, or prolonged.
You can test from home with a kit that checks for multiple infections at once. No waiting rooms. No awkward conversations. Just clarity, within minutes.
If you're ready to stop guessing and start knowing, STD Rapid Test Kits has options designed for real life, real privacy, and real peace of mind.
What If the Result Is Positive?
Take a breath. Then take the next step. Testing positive for an oral STD doesn’t make you dirty, reckless, or irresponsible. It makes you human. Most STDs are treatable. All are manageable. And none define your worth.
The first thing to do is confirm your result if needed, especially with something like HPV, which isn’t always included in routine tests. You may need a throat swab or additional lab testing, particularly for syphilis or herpes.
Next, talk to recent partners. It’s not always easy, but it’s a powerful form of care. You can use anonymous text tools, telehealth services, or even simple scripts like: “Hey, I found out I tested positive for an oral STD. I just wanted to let you know in case you want to get checked too.”
Most importantly, get treated. Antibiotics or antivirals can clear or suppress many oral infections. And the sooner you start, the sooner you stop being contagious.
This isn’t about blame. It’s about health. Yours, and everyone you connect with.
FAQs
1. Can my dentist really tell if I have an STD?
Not with 100% certainty, but they’re often the first ones to raise a red flag. If you’ve got a sore that’s not healing, white patches on your gums, or swollen tonsils with no fever, your dentist might gently suggest following up with a doctor. They can’t diagnose STDs, but they see things others might miss.
2. What do oral STD symptoms actually look like?
Sometimes like nothing. But when they do show up, it might be a sore that doesn’t go away, a cluster of tiny blisters, redness in your throat, or something that just feels... off. Think of it like your mouth sending up a quiet flare. If it’s new and it lingers, get it checked.
3. Can I really get an STD just from oral sex?
Yup. That’s one of the biggest myths out there. Oral sex can transmit herpes, gonorrhea, syphilis, HPV, even chlamydia. Just because it’s not “real sex” in someone’s book doesn’t mean the risk isn’t real. Protection helps, but it’s not a force field.
4. I’ve got a sore throat but no fever, could that be an STD?
If you recently had unprotected oral sex, it’s totally possible. Gonorrhea and chlamydia can hang out in the throat without causing much drama, no fever, no cough, just that annoying raw feeling. Easy to mistake for allergies or a cold. That’s what makes them sneaky.
5. What’s the difference between a canker sore and a herpes sore?
Canker sores tend to stay inside the mouth, are usually round with a white or yellow center, and aren’t contagious. Herpes can show up outside or inside, might tingle or burn before they appear, and often come in clusters. If you're not sure and it's recurring, it’s worth testing. Especially if you kissed or went down on someone recently.
6. Is it too late to test if my symptoms are gone?
Not necessarily. Some STDs clear from the throat on their own, but others hang around. Even if your symptoms fade, it doesn’t always mean the infection’s gone. A test is the only way to know, and if you’re negative, you get peace of mind. If not, you get treated. Win either way.
7. Will at-home STD tests detect infections in my throat?
Many will, especially the combo kits that include throat swabs or detect antibodies through blood. Just make sure you read the instructions carefully. If the kit is meant for genital infections only, it may miss oral ones. Look for one that’s clear about oral STD screening, or use one like this combo kit that covers multiple bases.
8. Should I tell my partner if I tested positive for something oral?
Yes. It doesn’t have to be a heavy, scary conversation. Try: “Hey, I just found out I had something I didn’t know about, and I wanted to give you a heads-up so you can look out for yourself too.” That’s not shame, that’s care. Real talk saves relationships.
9. What’s the best time to test after giving or receiving oral?
It depends on the infection, but a good rule of thumb is 7–14 days. Herpes can show up sooner, syphilis a bit later. And if you’re feeling symptoms, like a sore throat, ulcers, or patches, go ahead and test now, and again later if needed.
10. I’m embarrassed to ask for an oral STD test in person. What can I do?
You don’t have to explain anything if you don’t want to. That’s the beauty of at-home testing, it’s just you, your body, and the truth. No questions, no judgment. And if you’re not sure where to start, we’ve got your back.
You Deserve Answers, Not Assumptions
STDs don’t always show up where you expect them. Your mouth might be the first place something’s wrong. A sore throat with no fever, a white spot on your tongue, or a blister that won’t heal, these are not just “little things.” They’re clues your body is offering before things escalate.
If you’re worried, act. You don’t need to explain yourself. You don’t need permission. You just need a starting point. And that can be as simple as testing at home and getting clarity without the fear.
Your mouth is talking. Are you ready to listen?
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate.
Sources
1. CDC – Oral Sex and STDs: What You Should Know
2. Mayo Clinic – Oral Thrush Overview
3. About STI Risk and Oral Sex – CDC
4. Oral Manifestations of Sexually Transmitted Infections – PubMed
5. Oral sex and oral health: An enigma in itself – PMC
6. Oral manifestations of sexually transmitted diseases – PubMed
7. Oropharyngeal Human Papillomavirus (HPV) Infection – Cleveland Clinic
8. Sexually Transmitted Diseases and Your Mouth – MouthHealthy (ADA)
9. Oral STDs: Symptoms, Treatment, and More – Healthline
10. Oral Transmission of Sexually Transmissible Infections – PubMed
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: Dr. M. Sutherland, MPH | Last medically reviewed: December 2025
This article is for informational purposes and does not replace medical advice.