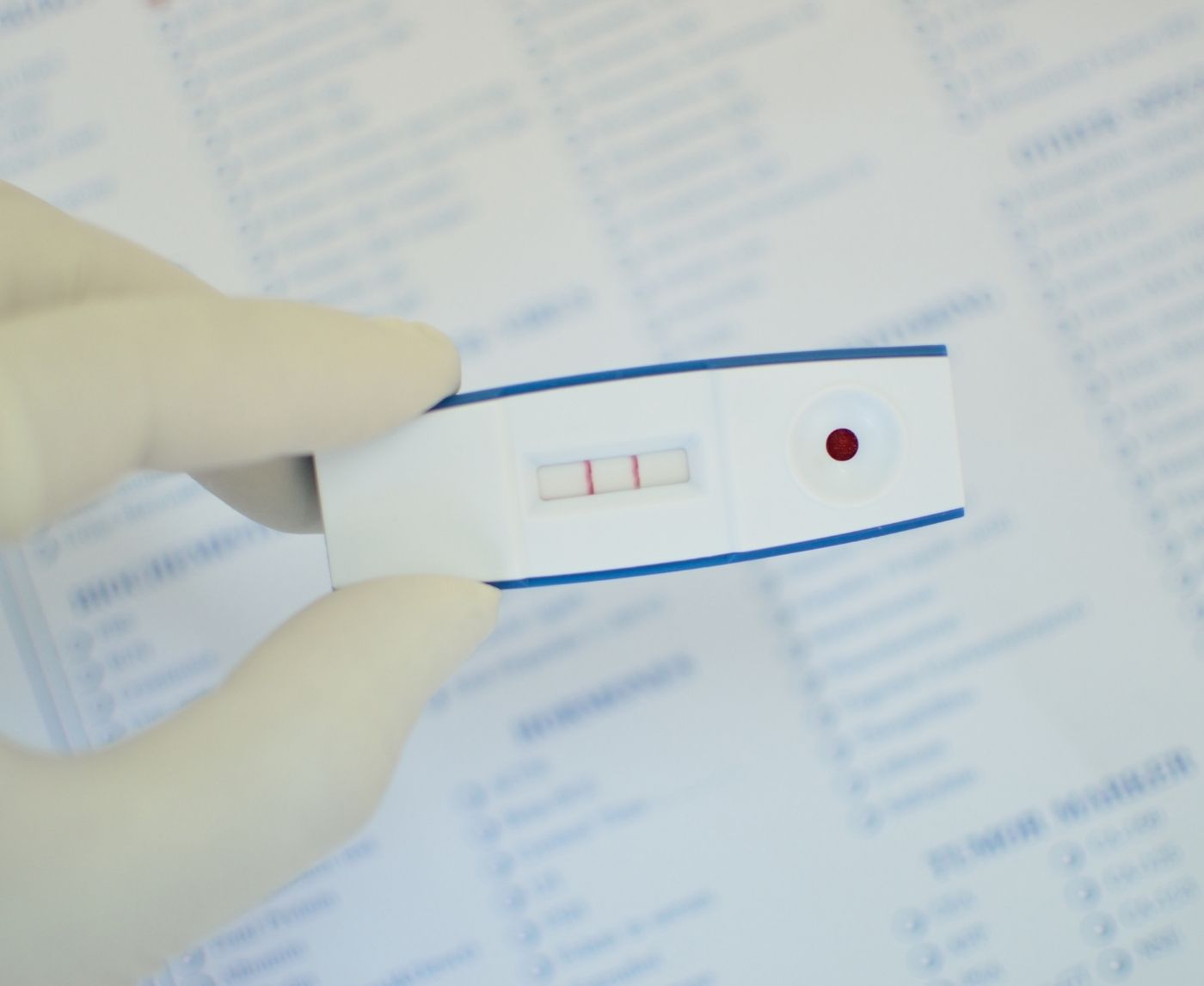
HIV Rapid Test Errors and Faint Lines: How to Know What’s Real
Last updated: April 2026
You take the test. It comes back negative. You exhale. You move on. But here's the thing: if you tested too early, that negative might not mean what you think it means. The window period is the gap between when an infection enters your body and when a test can reliably detect it. Get the timing wrong, and you're not getting answers. You're getting false reassurance.
This guide exists to fix that. Whether you're testing after a one-night stand, a condom failure, or just a gnawing feeling you can't shake, the single most important variable isn't which test you take; it's when you take it.

People are also reading: Why You Can Test Negative for an STD After Exposure (And What It Actually Means)
Window Period vs. Incubation Period: They're Not the Same Thing
These two terms get mixed up constantly, and the confusion leads people to test at the wrong time. The incubation period is how long it takes for symptoms to appear after exposure. The window period is how long it takes for a test to reliably detect an infection, even when it's already in your body. Those two timelines are often very different, and the one that matters for your test result is always the window period.
Here's why that distinction is critical: herpes symptoms, itching, tingling, the unmistakable feeling that something is wrong, can show up within four to seven days of exposure. But an antibody-based blood test for herpes won't reliably turn positive until around twelve weeks post-exposure. That's a ten-week gap between "I feel something" and "my test can confirm it." Someone who tests at day five, gets a negative, and stops worrying has not been cleared. They've just tested too early.
The opposite is also true. Trichomoniasis often causes no symptoms at all, and yet the infection becomes detectable by rapid test or NAAT as early as seven to fourteen days after exposure. No symptoms doesn't mean no infection. No positive doesn't mean no infection either, if you're still inside the window. The only way to navigate this correctly is to understand the window period for the specific infection you're concerned about, not to go by how you feel.
The Master Testing Window Table
The table below gives you the confirmed window periods for every major STD, the type of test used, and the earliest point at which a result becomes reliable. These figures are drawn from CDC STI Treatment Guidelines and reflect the testing windows used in clinical practice. Use the "Best Time to Test" column as your target, not the earliest possible date.
One thing worth noting: these are the windows for at-home rapid tests and standard antibody-based tests, which are the most widely used. Lab-based NAAT testing can sometimes detect bacterial infections slightly earlier, but for the purposes of planning your testing schedule, especially with at-home kits, the figures above are your reliable benchmarks.
Chlamydia: Test at 14 Days, Not Before
Chlamydia is the most reported STD in the United States, and one of the most frequently mistimed when it comes to testing. The bacteria can be present and replicating in your body within days of exposure, but most tests, including at-home rapid tests, won't reliably detect it until around fourteen days post-exposure.
The frustrating part: chlamydia often produces no symptoms at all. You might feel completely fine while the infection quietly causes damage to reproductive tissue. That's why the CDC recommends annual screening for sexually active people under 25, not waiting for a reason to test, but building it into routine health care. The bacteria that causes chlamydia is detectable through urine or a swab sample, making it one of the easier infections to test for at home once you're past the window.
A negative result at day five means very little. A negative at day fourteen, when the window has closed, is a result you can actually rely on. If you tested early and want real clarity, retest at the two-week mark. And if you're also concerned about gonorrhea, which frequently co-occurs with chlamydia, the same timing applies, though the recommended window for gonorrhea extends to three weeks for maximum accuracy.
For chlamydia specifically, the Chlamydia At-Home STD Test Kit is designed for use after the fourteen-day window has passed. If you're concerned about both chlamydia and gonorrhea together, the Chlamydia & Gonorrhea 2-in-1 kit covers both in a single test.

People are also reading: How Long After Exposure Can Chlamydia Be Detected?
Gonorrhea: Three Weeks for a Reliable Result
Gonorrhea moves fast. Symptoms, when they appear, can show up within two to five days in men. Women often experience nothing at all, or symptoms so mild they're attributed to something else entirely. But symptom timing and testing timing are two different things, and gonorrhea's recommended testing window extends to three weeks after exposure for the most reliable result. If you want a deeper look at exactly how that window behaves depending on exposure type, gonorrhea testing windows explained covers the full breakdown.
The infection is caused by a bacteria that targets mucous membranes, the urethra, cervix, throat, and rectum are all susceptible. That means if the exposure was oral, the throat can carry the infection even when genital swabs come back clear. Standard urine-based at-home tests check for urogenital gonorrhea, not throat or rectal infections, something worth knowing if the exposure involved oral or anal sex.
Gonorrhea is also an infection that's becoming harder to treat, with drug-resistant strains now documented across the US and globally. That makes early, accurate detection more important than ever. Testing at three weeks gives you a result that reflects the biological reality, not a snapshot from before the test could do its job.
Syphilis: Six Weeks Minimum, Twelve Weeks for Certainty
Syphilis has earned its nickname, "the great imitator", because its symptoms mimic dozens of other conditions. The primary stage produces a painless sore (chancre) at the exposure site. Many people miss it entirely because it doesn't hurt, appears in a location they can't easily see, and disappears on its own within three to six weeks. The infection doesn't go with it. For a full breakdown of what the syphilis window looks like at each stage, see when to test for syphilis after exposure.
Syphilis testing works by detecting antibodies your immune system produces in response to the infection. The problem is that antibody production takes time. Testing too early, before your immune system has mounted a detectable response, produces a false negative even when the bacteria is actively present. The recommended window is six weeks post-exposure for an initial reliable result, with a confirmatory test at twelve weeks for anyone who wants certainty or had a very high-risk exposure.
According to recent CDC provisional data, primary and secondary syphilis cases declined 22% in 2024 compared to 2023, the second consecutive year of decreases. That's genuine progress. But the CDC notes that congenital syphilis, infections passed from a pregnant person to their baby, rose for the twelfth consecutive year, with nearly 4,000 reported cases in 2024. The infection is still spreading, and many of those cases stem from people who didn't know they were infected, often because they tested too early, or not at all.
HIV: Six Weeks, Then Twelve, Here's Why Both Matter
HIV testing has more nuance than almost any other STD when it comes to window periods, because the type of test you use determines how early it can detect infection. Modern 4th-generation combination tests detect both the p24 antigen (a protein produced by the virus itself in early infection) and HIV antibodies. This dual detection shortens the window considerably compared to older antibody-only tests.
With a 4th-generation test, which is what most at-home rapid HIV tests now use, a reliable result is typically possible at six weeks post-exposure. This is the point at which the vast majority of people who have been infected will test positive. A negative at six weeks is genuinely reassuring. But for complete certainty, especially after high-risk exposures, retesting at twelve weeks is the clinical gold standard. At twelve weeks, the window is definitively closed for nearly everyone.
One important note: if you were potentially exposed to HIV within the last 72 hours, testing isn't the first step. Post-Exposure Prophylaxis (PEP) is a 28-day course of antiretroviral medication that can prevent HIV from establishing infection, but it must be started within 72 hours of exposure. If that window applies to you, contact a clinic or emergency room before testing.
The HIV-1/2 At-Home STD Test Kit is designed for use after the six-week window. For broader post-exposure screening that includes HIV alongside other infections, the 7-in-1 Complete At-Home STD Test Kit covers seven of the most common infections in a single panel.
Herpes (HSV-1 and HSV-2): The Trickiest Window of All
Herpes has the most misunderstood testing window of any STD, and the confusion causes real harm. The virus is extraordinarily common, estimates suggest the majority of adults carry HSV-1, and a significant proportion carry HSV-2 without knowing it, but blood-based antibody testing for herpes takes longer to become reliable than almost any other infection. The specific question of how soon after sex you can test for HSV-1 or HSV-2 is one of the most searched herpes questions for good reason — the answer genuinely surprises people.
Here's the biology: after exposure, your immune system begins producing IgG antibodies against the herpes virus. But that process takes time. Most antibody-based blood tests for herpes won't reliably turn positive until six weeks post-exposure, and some people don't reach detectable antibody levels until twelve weeks or longer. Testing at day seven and getting a negative means almost nothing. Even a negative at four weeks requires a follow-up to be meaningful.
The exception to this is swab testing during an active outbreak. If a sore or blister is present, a swab taken directly from the lesion can detect the virus immediately, before antibodies have had time to develop. This is actually the most accurate way to confirm herpes, which is why doctors often recommend testing during the first outbreak rather than waiting for a blood test to catch up.
If you're testing between outbreaks, or if you've never had visible symptoms but want to know your status, the six-week mark is the earliest point worth testing. For the most reliable answer, twelve weeks is the target.
Hepatitis B: Six Weeks After Exposure
Hepatitis B is transmitted through blood and bodily fluids, including unprotected sex, and it's one of those infections people tend not to think about in a sexual health context, even though it absolutely should be on the radar. It's also vaccine-preventable, which makes it somewhat unique among the STDs covered in this guide. For a detailed look at how the hepatitis B window behaves and when testing is and isn't reliable, see too soon to test: the hepatitis B window period explained.
Testing for hepatitis B involves detecting the hepatitis B surface antigen (HBsAg), a protein the virus produces that becomes detectable in the blood approximately three to six weeks after exposure. The recommended window for at-home testing is six weeks post-exposure. If your result comes back negative at six weeks and you had a confirmed high-risk exposure, testing again at nine to twelve weeks provides an additional layer of confirmation.
Worth noting: if you've been vaccinated against hepatitis B, you have antibodies in your system already. This doesn't affect standard antigen-based testing, which looks for evidence of the virus itself rather than your immune response to the vaccine. Your vaccination status doesn't alter the testing window or interfere with results.
Hepatitis C: The Longest Wait
Hepatitis C has the widest testing window of any common STD, and that makes it uniquely frustrating for people trying to get peace of mind quickly. The infection is caused by a virus that can take eight to eleven weeks before antibodies reach detectable levels in standard testing. Some people take even longer, particularly those with certain immune conditions.
The reason the window is so wide is that hepatitis C antibodies develop more slowly than those for many other infections. RNA-based tests (which detect the virus's genetic material directly) can identify the infection sooner, sometimes within one to two weeks, but these tests are generally only available through clinical laboratories, not at-home rapid kits. For at-home testing purposes, the eight-to-eleven-week mark is the reliable window to plan around.
Hepatitis C is also worth flagging because it's one of the infections that can live in the body for years or decades without causing symptoms that would prompt testing. Most people who have it don't know. That's why the CDC now recommends that all adults ages 18 to 79 be tested for hepatitis C at least once in their lifetime, regardless of risk factors, a guideline worth knowing if routine testing has never been part of your health care routine.
People are also reading: What to Do After a Positive Hepatitis C Test, No Panic, Just Steps
Trichomoniasis: Faster Than You'd Think
Trichomoniasis doesn't get as much attention as HIV or herpes, but it's actually one of the most common curable STDs in the world. It's caused by a parasite rather than a virus or bacteria, and its testing window is one of the shorter ones, becoming detectable around five to fourteen days after exposure, with fourteen days being the recommended target for the most reliable result.
The tricky part with trichomoniasis isn't the testing window; it's the absence of symptoms. Most infected people have none, or symptoms so mild they're written off as irritation or a yeast infection. The discharge, odor, or itching that does sometimes appear can mimic other common conditions, which is why testing is the only real way to know. And because reinfection is common, particularly if a partner isn't treated simultaneously, a negative result is only meaningful if both partners test and treat at the same time.
Trichomoniasis is entirely curable, which makes early and accurate detection particularly worthwhile. The Trichomoniasis At-Home STD Test Kit is available for women after the fourteen-day window, and women's combo kits that include trichomoniasis alongside other infections provide a more complete picture after exposure.
HPV: Why There's No Simple Window Period
HPV stands apart from every other STD on this list when it comes to testing, because there's no at-home rapid test for HPV, and testing doesn't work the same way it does for bacterial or blood-borne infections. HPV is detected through Pap smears and HPV DNA tests performed on cervical cells, which means testing is clinician-guided and integrated into routine gynecological care rather than triggered by a specific exposure event.
This creates a genuinely confusing situation for people who've just had a potential exposure and want to know their status. The honest answer is: there's no test you can take that will tell you whether you acquired HPV from a specific encounter. The virus can take weeks, months, or even years to cause changes that are detectable on a Pap smear. And many HPV infections clear on their own without ever producing detectable changes at all.
For women, the practical approach is to stay current with routine cervical screening, Pap smears every three years, or Pap plus HPV co-testing every five years, and to speak with a provider if you have a specific concern about high-risk HPV strains. For men, there's currently no approved HPV screening test, though the virus can cause genital warts and certain cancers, including anal and throat cancers. HPV vaccination remains the most effective protective measure available for anyone who hasn't already been fully exposed.
How to Read This Table: Earliest vs. Reliable vs. Confirmatory
Understanding the difference between these three milestones is what separates a meaningful result from a false sense of security. The table below maps them out for the infections where the distinction matters most.
The "earliest" column is when a test might catch the infection under ideal conditions with a highly sensitive test. The "reliable" column is when the window has closed for most people. The "confirmatory" column is for anyone who wants to be certain, or who had a very high-risk exposure and got an early negative. If you're only going to test once, always aim for the reliable column. If something still feels wrong after a negative result, the confirmatory window is your answer.
Why False Negatives Happen (And What to Do About Them)
A false negative is when a test says negative, but the infection is actually present. It's not a broken test, and it's not bad luck; it's almost always a timing issue. The biology hasn't caught up to the test yet. Here are the three most common reasons it happens:
Testing inside the window period. This is the big one. If you test before the infection has produced enough viral load, antigens, or antibodies for the test to detect, the result will be negative regardless of the actual reality. The infection doesn't care about your timeline; it operates on its own. The only solution is retesting after the window has closed.
Test sensitivity. At-home rapid tests use lateral flow technology, which is accurate and convenient but requires a certain threshold of viral load or antibody concentration to produce a positive line. Lab-based NAAT testing is more sensitive and can detect lower concentrations, which is one reason a clinic result might differ from an at-home result taken on the same day.
Sample collection errors. Urine tests for chlamydia and gonorrhea require a first-void sample, the first urine of the day, or at least urine that hasn't been passed for an hour or two. Swab tests require proper technique. An improperly collected sample can return a false negative even when the window is fully closed. Always read the instructions before testing, not during.
If you test negative but symptoms persist, or if you tested early and want a definitive answer, retesting at the appropriate window is the right move. A negative result you can trust is one that comes after the window has fully closed, not before it.

People are also reading: STD Window Periods: Why Testing Too Soon Can Give You a False Negative
What to Do Right After a High-Risk Exposure
Testing isn't always the first step. Depending on what happened and when, there may be more urgent actions to take before a test would even be meaningful.
If you had a potential HIV exposure within the last 72 hours, contact a clinic, urgent care, or emergency room about PEP (Post-Exposure Prophylaxis) immediately. This is a 28-day course of antiretroviral medication that can prevent HIV from establishing infection, but only if started within three days of exposure. No at-home test will be useful at this stage, and the window for PEP closes fast.
If you've been vaccinated against hepatitis B, your risk from a single exposure is significantly reduced. If you haven't been vaccinated, and the exposure was within the last 24 hours, hepatitis B immune globulin (HBIG) combined with vaccination can provide post-exposure protection. Again, this is a conversation for a provider, not a home test kit.
Once the immediate post-exposure window has passed, the testing timeline in this guide applies. Mark the dates. Set a reminder for the appropriate window. Testing at the right time is not a passive act, it's an active decision that gives you a result you can actually use.
At-Home Testing vs. Clinic Testing: What Changes When It Comes to Timing
At-home rapid tests and clinic-based tests don't always have the same window periods, and that's worth understanding before you choose a testing method based on speed alone.
Clinic-based NAAT tests (nucleic acid amplification tests) detect the actual genetic material of bacteria or viruses. They're highly sensitive and can sometimes detect infections slightly earlier in the window than antibody-based rapid tests. This matters most for HIV, where a clinic-based RNA test can pick up the virus around ten to fourteen days post-exposure, while most at-home rapid tests require six weeks for a reliable result.
For bacterial STDs like chlamydia and gonorrhea, the gap is smaller. Both at-home and clinic-based NAAT tests are reliable after fourteen days. The practical difference is that clinic tests can also cover throat and rectal exposure sites that urine-based at-home tests don't reach.
For most people managing routine sexual health, testing after a new partner, after a condom failure, or as part of regular screening, at-home testing at the right window is completely appropriate. The accuracy is there when the timing is right. If you had a very high-risk exposure, symptoms that won't resolve, or a negative result that doesn't match what your body is telling you, a clinic visit gives you access to a broader range of tests and a provider who can help interpret the full picture.
FAQs
1. How soon after unprotected sex can I test for STDs?
It depends entirely on which infection you're concerned about. Chlamydia and gonorrhea become reliably detectable around fourteen days to three weeks after exposure. HIV and syphilis need six weeks minimum. Herpes antibody tests aren't reliable until six to twelve weeks. If you're testing right after a hookup, you're almost certainly still inside the window for most infections, which means you'll need to retest at the right time to get a result that actually means something.
2. What does it mean if I test negative but still feel like something's wrong?
It usually means one of two things: you tested too early, or you're dealing with something the test doesn't cover. Both are common. If you're inside the window period for the infection you're concerned about, that negative is not a clearance, it's just an early data point. Retest after the window closes. If something physical is still bothering you after a full-window negative, that's a conversation for a doctor, because it could be a non-STD issue that needs a different kind of test.
3. Can antibiotics interfere with STD test results?
Yes, in specific ways. Antibiotics prescribed for something else, a sinus infection, a skin issue, a urinary tract infection, can partially suppress bacterial STDs like chlamydia or gonorrhea, potentially causing a false negative. If you've taken antibiotics in the weeks before testing, mention it to a provider and consider retesting fourteen to twenty-one days after finishing the course.
4. If my partner tested negative, do I still need to test?
Yes. Their result covers their biology and their timeline, not yours. They might have tested during their own window period. They might have a different exposure risk. STD testing is always individual. Your timeline is yours, and it runs independently of theirs.
5. I tested negative for HIV at two weeks. Am I in the clear?
Not definitively. Two weeks is inside the window period for most at-home rapid HIV tests, which use 4th-generation technology and become reliably accurate at six weeks. A negative at two weeks is better than nothing, but it's not the answer. Retest at six weeks, and again at twelve weeks if the exposure was high-risk or if you want certainty.
6. What's the difference between a window period and an incubation period?
The incubation period is when symptoms appear. The window period is when a test can detect the infection. These don't match up, herpes symptoms can appear within a week, but a blood test won't be reliable for six to twelve weeks. Gonorrhea can take five days to cause symptoms in men, but the test window extends to three weeks for accuracy. Always use the testing window, not the symptom timeline, to plan when you test.
7. Why do some infections have longer window periods than others?
It comes down to what the test is detecting. Tests that look for the bacteria or virus directly (NAAT tests) can work faster because they detect the pathogen itself. Tests that look for antibodies, your immune system's response to the infection, take longer because your body needs time to mount that response. HIV, herpes, and syphilis all rely on antibody detection for most standard tests, which is why their windows are longer than those of chlamydia or gonorrhea.
8. I had an STD treated with antibiotics. When should I retest?
Wait at least fourteen to twenty-one days after completing treatment before retesting for most bacterial infections. Testing too soon after antibiotics can return a false negative because bacterial DNA can persist in your system for a short time even after the infection has been cleared. A clean test at three weeks post-treatment gives you real confirmation.
9. Can I test for multiple STDs at once, and do they all have the same window?
You can absolutely test for multiple infections at once, combo kits are built for exactly this. But each infection in the panel has its own window period. A 7-in-1 kit taken at two weeks will give you reliable results for chlamydia and gonorrhea, but not for HIV, syphilis, or herpes. If you're doing a full panel after exposure, consider timing it at the six-week mark so the widest range of infections are within their reliable windows simultaneously.
10. Is testing at home as accurate as testing at a clinic?
For bacterial STDs like chlamydia and gonorrhea, at-home NAAT-based kits have accuracy comparable to clinic testing when used at the right window and with proper sample collection. For viral infections, especially HIV and herpes, clinic-based tests can sometimes detect infections slightly earlier, and clinics can offer a broader range of test types. At-home testing is genuinely reliable when the timing is right. If you've tested at the right window, followed the instructions correctly, and gotten a negative, you can trust that result.
Get Tested at the Right Time, Not Just Any Time
Most people who test after a risky exposure are doing the responsible thing. The gap between "responsible" and "accurate" is almost always timing. A test taken too early doesn't fail you, it just can't give you the answer you're looking for yet. The window period isn't a technicality. It's the difference between a result that matters and one that leaves you exactly where you started.
If you're ready to test and the window has closed, the 7-in-1 Complete At-Home STD Test Kit covers HIV, chlamydia, gonorrhea, syphilis, hepatitis B, hepatitis C, and genital herpes in a single panel, shipped discreetly, with results in minutes. For those who want the broadest possible panel at the six-week mark, the 8-in-1 Complete At-Home STD Test Kit adds oral herpes (HSV-1) to the mix. And if you're looking to test for a specific infection based on your exposure, single-infection kits are available for every major STD.
You've done the hard part by deciding to test. Let the timing do the rest of the work.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC – 2021 STI Treatment Guidelines
2. CDC – 2024 National STI Surveillance Data Release
3. WHO – Sexually Transmitted Infections Fact Sheet
4. CDC – Getting Tested for STIs
5. NCBI – Clinical Updates in Sexually Transmitted Infections, 2024
6. Brighton Sexual Health – STI Window Periods: When Should I Test?
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.