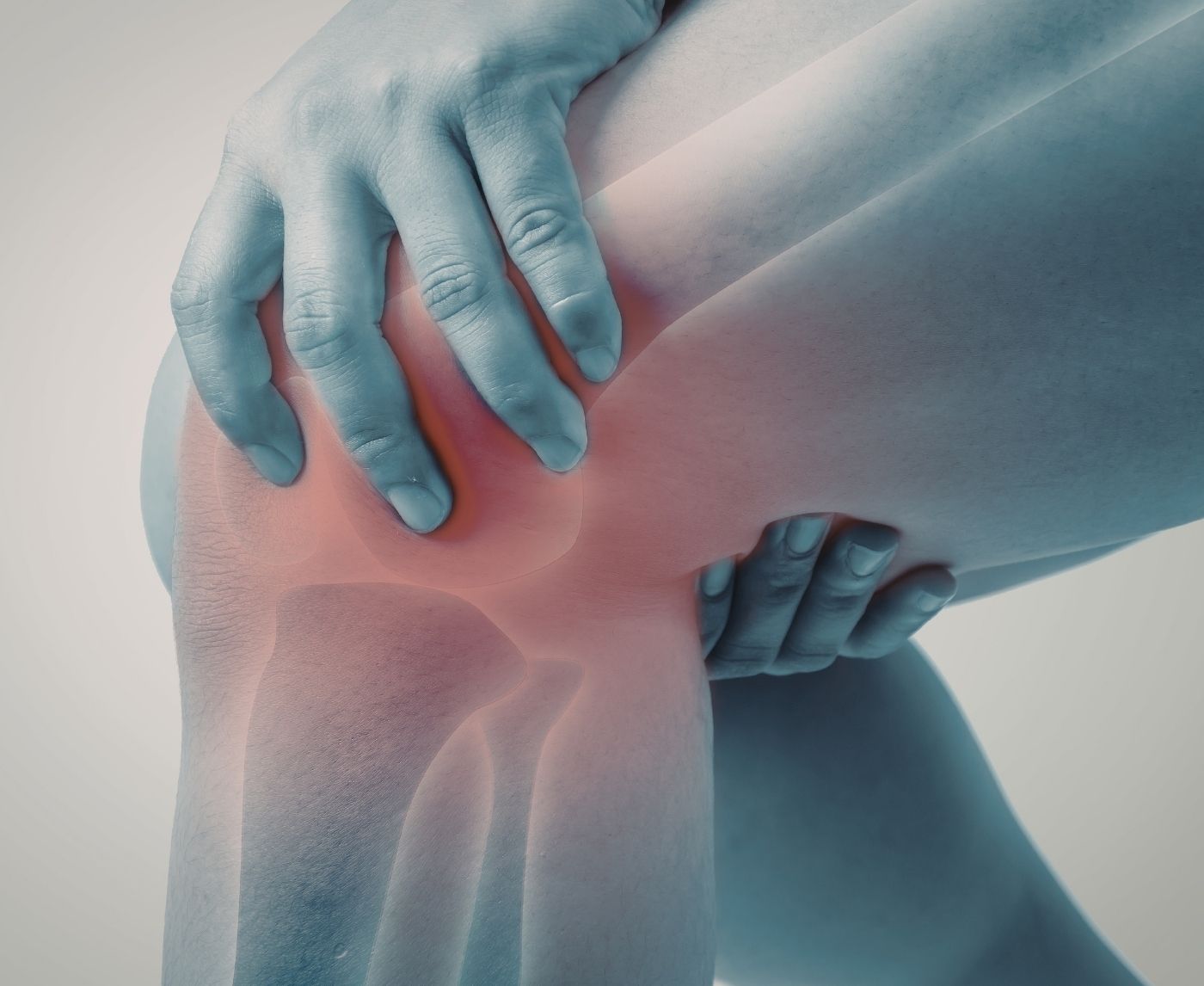
Burning But Not All the Time? Why STD Symptoms Flare and Fade
Quick Answer: Yes, an STD can cause joint pain. Untreated gonorrhea can spread to the bloodstream and infect joints, and chlamydia can trigger reactive arthritis days to weeks after exposure.
This Isn’t Just a Sprain: When Infection Shows Up in Your Knees
Most people don’t connect joint swelling to a recent hookup. Aiden, 27, told his doctor he thought he had overtrained for a half marathon. His right knee ballooned, then his ankle. He had no discharge. No genital pain. What he did have, quietly, was untreated gonorrhea he didn’t know about.
That’s the part that unsettles people. You can have an STD and not feel it where you expect. According to the CDC’s gonorrhea fact sheet, many infections cause minimal or no symptoms. When left untreated, the bacteria can enter the bloodstream in a condition called disseminated gonococcal infection. From there, it can settle in joints and cause what looks and feels like septic arthritis.
Joint pain linked to STDs is uncommon, but it is medically documented. And because it’s uncommon, it’s often misdiagnosed at first as a sports injury, autoimmune flare, or random inflammation.
People are also reading: Eye Infection After Sex: Can STDs Infect Your Eyes?
How Gonorrhea Can Travel: From Genitals to Bloodstream to Joint
Gonorrhea is caused by the bacterium Neisseria gonorrhoeae. In most cases, it infects the cervix, urethra, rectum, or throat. But in a small percentage of untreated cases, the bacteria enter the bloodstream. That’s when things escalate.
Disseminated gonococcal infection, sometimes abbreviated as DGI, can present with fever, rash, and joint pain. Some people develop a single severely painful joint. Others feel migrating pain that moves from wrist to knee to ankle. According to Mayo Clinic, untreated gonorrhea can lead to joint infections and other systemic complications.
The tricky part is timing. You might have had mild urinary discomfort weeks earlier and ignored it. By the time your knee swells, you don’t mentally connect the two events. The body, however, remembers.
Septic arthritis is considered a medical urgency. A hot, swollen joint accompanied by fever deserves immediate evaluation. But not every STD-related joint issue is a direct bacterial infection.
Reactive Arthritis: When Your Immune System Overreacts
Now let’s talk about the quieter, more delayed pathway. Reactive arthritis is not bacteria inside the joint. It’s your immune system misfiring after an infection, often chlamydia.
Samira, 31, had mild pelvic discomfort she brushed off. Two weeks later, her knees stiffened and her eyes burned with redness. Blood tests eventually revealed a recent chlamydia infection. The joint pain wasn’t from bacteria invading her knees. It was from her immune system reacting to the infection.
The NHS overview of reactive arthritis explains that symptoms can develop days to weeks after an infection, commonly in the urinary or gastrointestinal tract. Joints, eyes, and the urinary tract can all become inflamed.
This is why some people Google “why do my joints hurt after sex” or “body aches after sex STD” and feel dismissed. The pain is real. The timeline is real. But it’s not always obvious.
Both conditions are rare compared to uncomplicated STDs. But they matter because untreated infections increase the risk.
What It Feels Like (And Why It’s So Confusing)
Joint pain from an STD doesn’t always scream infection. It can feel like stiffness in the morning. A swollen finger you assume is from typing. A knee that locks slightly when climbing stairs. Some people describe it as flu-like aches without a cold.
And here’s where shame creeps in. If you had a recent new partner, your brain may whisper that this is punishment. It’s not. It’s biology. According to CDC data on chlamydia, many infections are asymptomatic. That means your joints may be the first noticeable signal.
The body does not moralize exposure. It responds to pathogens and immune triggers. That’s it.
When to Test If You’re Worried
If you’re connecting dots between joint swelling and a possible exposure, timing matters. Testing too early can give you a false sense of security. For chlamydia and gonorrhea, nucleic acid amplification tests are usually reliable about 7 to 14 days after exposure, with accuracy improving after two weeks.
If joint pain is present, especially with fever or rash, seek medical evaluation promptly. But if symptoms are mild and you’re in that waiting window, testing is still powerful information.
You can order discreet screening directly from STD Test Kits. For broader reassurance, a Combo STD Home Test Kit checks for multiple common infections at once. It’s not about panic. It’s about clarity.
Peace of mind is sometimes one test away. And clarity changes how you move forward.
Why It’s Missed So Often, And Why That Matters
Joint pain linked to an STD is uncommon enough that many clinicians don’t jump to it first. If you walk into urgent care saying your knee hurts, you’ll likely be asked about sports, strain, or arthritis. You may get an X-ray. You may be told to rest and ice it. If no one asks about recent sexual activity, the root cause can stay hidden.
Rafael, 34, described it this way: “I felt embarrassed even bringing up that I’d had a new partner. I didn’t think it was relevant. My knee was the problem.” It wasn’t until his second visit, when he mentioned mild burning weeks earlier, that testing was ordered. The result was positive for gonorrhea. By then, the bacteria had already triggered inflammation in his joint.
When untreated gonorrhea spreads to the bloodstream, the condition is called disseminated gonococcal infection. According to the CDC’s treatment guidelines, DGI can present with arthritis, tenosynovitis, and skin lesions. The genital symptoms may be mild or absent entirely. That disconnect is what makes this condition easy to miss.
Body Aches After Sex: STD, Flu, or Something Else?
Not every ache after intimacy is infection. Sex can be physically demanding. Muscles tense. Hips flex. Sleep might be short. It’s normal to wake up feeling a little sore. The problem is when soreness becomes swelling, redness, warmth, or persistent stiffness that doesn’t improve.
Flu-like symptoms are also a complicating factor. Early HIV infection can cause fever, body aches, and fatigue, often described as a viral syndrome. According to World Health Organization HIV fact sheets, acute HIV infection can resemble influenza. That doesn’t typically involve isolated joint swelling, but it can create generalized aches that feel unsettling.
Then there’s reactive arthritis. This immune response can cause joint pain, urinary discomfort, and eye irritation. Some people experience heel pain. Others notice swollen fingers that look like sausages. It’s inflammatory, not mechanical, which means rest alone won’t fully resolve it.
The overlap in symptoms is what drives late-night searches like “STD and joint pain,” “knee pain STD,” or “flu like symptoms STD.” The body does not label the source of inflammation. It just signals distress.
Who Is Most at Risk for STD-Related Joint Complications?
Although any infected person is liable to suffer from complications, there are some factors associated with an increased risk of exposure, such as the delay in testing, which is one such risk factor. Since chlamydia and gonorrhea are often not symptomatic, infected persons might be unaware of the fact that they are infected.
Another risk factor is the increased incidence of chlamydia and gonorrhea in young adults, which statistically increases the risk of exposure to the two diseases. According to the CDC, the surveillance summaries show that the number of persons below the age of 30 comprises a significant portion of new cases of chlamydia and gonorrhea.
Another risk factor for suffering from reactive arthritis is the susceptibility of the human immune system, which is associated with the genetic marker HLA-B27. Although not all infected persons have this genetic marker, it is associated with an increased risk of an exaggerated reaction to the two diseases.
However, gender does not reduce the risk of exposure to the two diseases, such as the risk for persons assigned female at birth, who might not be aware of the silent infection in the cervix, and the risk for persons assigned male at birth, who might not take the symptoms of urethral irritation seriously.

People are also reading: Why Does It Burn After Sex? Friction vs Infection Explained
When Joint Pain Becomes an Emergency
Most reactive arthritis cases are uncomfortable but not life-threatening. Septic arthritis, however, can damage joint cartilage quickly if untreated. If a joint is intensely painful, visibly swollen, warm to the touch, and accompanied by fever, urgent medical care is essential.
Septic arthritis is not exclusive to STDs. It can occur from other bacterial infections. But when someone has risk factors for untreated gonorrhea, it must be considered. According to peer-reviewed clinical summaries on septic arthritis, prompt antibiotic treatment is critical to prevent long-term joint damage.
If you’re unsure whether your symptoms cross into emergency territory, err on the side of caution. Severe joint immobility with fever deserves evaluation that day. Mild stiffness without fever allows space for testing and outpatient assessment.
Testing Strategy: Don’t Guess. Confirm
If you think there is a possibility of recent sexual exposure causing new joint pain, your goal is not self-blame but clarity. Testing can determine if there is an active infection. If there is, treatment can prevent further complications and minimize the chance of passing it onto a partner.
For chlamydia and gonorrhea, nucleic acid amplification is considered a highly accurate form of testing if done at an appropriate time. This is the same form of testing used in at-home kits. You can get discreet at-home testing with STD Test Kits without having to go into a waiting room.
If your recent exposure has been with multiple forms of risk, you should consider getting tested for more. A Combo STD Home Test Kit can provide results for several common infections. This is not a replacement for medical care if your symptoms are severe, but it is empowering yourself with knowledge.
It is not an admission of guilt, but rather a medical procedure. It is just as important as checking your blood pressure or cholesterol level.
What Happens If It’s Positive?
If these infections are confirmed, treatment is simple. Antibiotics are prescribed, as recommended. For disseminated gonococcal infections, intravenous antibiotics may be necessary, especially if the joints are infected.
For reactive arthritis, treatment is aimed at eliminating the underlying infection and reducing inflammation. Nonsteroidal anti-inflammatory drugs are usually first-line treatment. If symptoms persist, referral to a rheumatologist is warranted.
Amira, aged 29, said:
“I was scared it was going to be autoimmune, and I was going to be stuck with it. But when they said it was related to chlamydia and could be treated, I felt grounded again.”
Knowing what is going on can help prevent spiraling thoughts. Treatment can help alleviate inflammation. Both are important.
The Emotional Whiplash No One Talks About
There’s a specific kind of panic that comes with symptoms that don’t “match.” If you had discharge, you might connect it to an STD faster. If you had a rash, maybe you’d Google it sooner. But aching knees? Swollen fingers? That feels unfair. It feels unrelated. And that disconnect can delay care.
Jordan, 26, described sitting on the edge of his bed staring at his knee. “I kept thinking, this can’t be connected. I used protection. I don’t even have any genital symptoms.” What he didn’t know was that protection significantly reduces risk, but it doesn’t eliminate it entirely. And some infections can be silent for weeks.
This is where stigma does real damage. When we associate STDs only with visible or dramatic symptoms, we miss the subtle ones. We also miss the chance to intervene early. Joint pain linked to infection is not a moral failing. It’s a medical signal.
Why Asymptomatic Infections Complicate the Story
One of the most frustrating realities about chlamydia and gonorrhea is how often they produce no obvious symptoms. According to national public health data, a large percentage of chlamydia infections in people with cervixes cause no noticeable warning signs. That means someone can feel completely fine genitally while inflammation is brewing internally.
When infection goes untreated, the immune system continues reacting. In some people, that reaction spills into joints. In others, bacteria may circulate systemically before being detected. The absence of discharge or burning does not guarantee absence of infection.
Search queries like “STD symptoms no discharge” or “can chlamydia cause arthritis” reflect this confusion. People are trying to reconcile two truths: they feel joint pain, and they don’t feel what they were told an STD should feel like. The answer, medically, is that infections don’t read pamphlets. They behave based on biology, not expectation.
How Long After Exposure Could Joint Symptoms Appear?
Timing varies depending on the mechanism. With disseminated gonococcal infection, joint pain can develop during active untreated infection. That might be days to weeks after exposure. Fever and rash sometimes accompany it, but not always.
Reactive arthritis typically appears one to four weeks after the triggering infection. By the time joints swell, the initial genital symptoms may have faded or never appeared. This delay is what makes the connection feel implausible.
If you’re in that window and symptoms are emerging, testing now is reasonable. If it has been fewer than seven days since exposure, you may need to retest after the two-week mark for reliable detection. Accuracy improves with proper timing.
Can Other STDs Cause Joint Pain?
While gonorrhea and chlamydia are the most commonly linked to joint complications, they are not the only infections that can create systemic symptoms. Early HIV infection can produce diffuse body aches as part of an acute viral syndrome. Hepatitis B can also cause joint pain in some cases during its early phase.
That said, isolated swollen joints without other systemic symptoms are most classically associated with gonococcal spread or reactive arthritis. The key is not to self-diagnose based on one symptom alone. Testing clarifies which infections are present and which are not.
If your exposure history includes oral, vaginal, or anal contact without recent screening, a comprehensive approach makes sense. You don’t have to guess which infection is responsible. You can screen broadly and then narrow the plan based on results.
Reducing Risk Going Forward Without Panic
Learning that an STD can affect joints can feel alarming. It’s important to zoom out. These complications are uncommon compared to straightforward infections that are easily treated. Regular screening dramatically reduces the chance of progression to bloodstream spread or inflammatory complications.
Barrier protection, open communication with partners, and routine testing remain foundational strategies. Vaccination for preventable infections like Hepatitis B adds another layer of protection. None of these steps are about shame. They’re about resilience.
If anxiety is running high, grounding yourself in action helps. You can order discreet screening from STD Test Kits and get clear answers from home. A Combo STD Home Test Kit covers multiple common infections at once, which is often reassuring when symptoms don’t fit a single textbook pattern.
You deserve information that empowers you, not spirals you.
When It’s Not an STD at All
It’s also essential to say this plainly: many cases of joint pain have nothing to do with sexually transmitted infections. Autoimmune conditions, viral illnesses, overuse injuries, and metabolic disorders are far more common causes of knee and wrist pain.
If testing is negative and symptoms persist, follow up with a healthcare provider. Rheumatologic evaluation, imaging, or blood work may be needed. Being thorough is not overreacting. It’s responsible care.
The goal of this article is not to convince you that every ache is an STD. It’s to widen the diagnostic lens so rare but meaningful links aren’t ignored.
People are also reading: Is That a Pimple, Herpes, or a Genital Wart?
FAQs
1. Can an STD really cause joint pain, or is that just internet paranoia?
It’s not paranoia. It’s uncommon, but medically real. Untreated gonorrhea can spread to the bloodstream and infect a joint directly, and chlamydia can trigger something called reactive arthritis weeks later. Most joint pain has nothing to do with sex. But if the timing lines up, it’s worth checking.
2. I don’t have discharge or burning. Could it still be an STD?
Yes. That’s the part that surprises people. Many chlamydia infections, especially in people with cervixes, cause no obvious symptoms. You can feel completely “normal” genitally and still have an infection your immune system is reacting to. Silence isn’t proof of safety.
3. What does STD-related joint pain actually feel like?
It’s not subtle muscle soreness from a workout. It’s usually swelling, stiffness, or warmth in a joint. Some people wake up and their knee just feels wrong, tight, puffy, harder to bend. Others notice heel pain or swollen fingers. If there’s fever and severe pain, that’s urgent. If it’s milder but persistent, it’s worth evaluating.
4. How long after sex would joint symptoms show up?
It depends. If gonorrhea spreads to the bloodstream, joint symptoms can happen while the infection is still active. Reactive arthritis from chlamydia usually appears one to four weeks later. That delay is why people don’t connect the dots. The body doesn’t always send its messages in chronological order.
5. If I test positive, does that mean my joints are permanently damaged?
In most cases, no. Septic arthritis needs quick treatment to prevent joint damage, which is why severe symptoms require immediate care. Reactive arthritis often improves over weeks to months with treatment and anti-inflammatory support. Early action changes outcomes dramatically.
6. Should I panic if my knee hurts after a hookup?
No. Panic is loud but not helpful. Most knee pain is mechanical, overuse, strain, random inflammation. What matters is context. If you also had a recent exposure and haven’t tested, that’s information. Testing replaces guesswork with facts. Facts are calmer than fear.
7. What if my test is negative but my joints still hurt?
Then we pivot. That’s not failure, that’s progress. A negative test narrows the possibilities. Your provider might explore autoimmune causes, viral infections, or orthopedic issues. Ruling out STDs is a step toward clarity, not the end of the road.
8. Can condoms prevent this kind of complication?
Condoms significantly reduce risk for gonorrhea and chlamydia. They are powerful tools. But no method outside abstinence is 100 percent protective. Regular screening, especially with new partners, catches infections early before they have time to spread or trigger inflammation.
9. Is this something I should tell a partner about?
If you test positive, yes. That conversation isn’t about blame, it’s about care. Many infections are asymptomatic, which means your partner may not know either. Sharing information gives both of you the chance to get treated and protect future health.
10. How worried should I be?
Concerned enough to get tested if the timing makes sense. Not so worried that you spiral into catastrophe. Joint pain from STDs is rare, but untreated infections can cause real complications. Testing is simple. Treatment is straightforward. Knowledge lowers the volume on fear.
You Deserve Clarity, Not Catastrophe
If you’ve been staring at your knee wondering how it connects to your sex life, take a breath. Joint pain after an STD is rare, but it is real. The key difference between anxiety and action is information. Testing replaces spiraling with facts.
If you’re within the testing window, or past it and still unsure, you can screen discreetly through this at-home combo test kit. It checks for common infections linked to reactive arthritis and bloodstream complications. Your results are private. Your next steps are yours to control.
And if the test is negative? That’s valuable too. It means you can pivot toward other explanations without carrying hidden fear. Either way, clarity is power.
How We Sourced This Article: This guide was built using current clinical guidance from the CDC, WHO, NHS, Mayo Clinic, and peer-reviewed infectious disease literature on disseminated gonococcal infection and reactive arthritis. We reviewed approximately fifteen medical and public health sources to ensure accuracy, then selected six of the clearest and most authoritative references below. All links were verified to lead to reputable medical organizations and open in a new tab for transparency.
Sources
1. CDC – Gonorrhea Treatment Guidelines
2. NHS – Reactive Arthritis Overview
3. Mayo Clinic – Gonorrhea Symptoms and Complications
4. World Health Organization – HIV Fact Sheet
5. Gonococcal Infections Among Adolescents and Adults - STI Treatment Guidelines | CDC
6. Health Alert Template for Disseminated Gonococcal Infection (DGI) | CDC
7. Reactive arthritis | MedlinePlus Medical Encyclopedia
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers who want discreet, reliable answers.
Reviewed by: Lauren Mitchell, PA-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.