You Can Get an STD from Oral Sex, Here’s How It Happens
Last updated: April 2026
If you've had unprotected oral sex and something feels off, or nothing feels off at all, you're asking the right question. Oral chlamydia doesn't always announce itself. Symptoms are easy to dismiss as a cold or allergies, and a significant number of people carry the infection with zero signs. That gap between what people feel and what's actually there is precisely why throat chlamydia stays underdiagnosed and keeps spreading.
People are also reading: Which Hepatitis C Home Test Should You Trust in 2026?
Can You Really Get Chlamydia in the Mouth or Throat?
Yes, and this isn't a fringe scenario. The bacterium Chlamydia trachomatis can establish itself in the oral cavity and throat when it comes into contact with an infected partner's genitals. Performing oral sex on someone with a genital chlamydia infection is the primary route, but receiving oral sex from someone with an active throat infection can also transmit it. Many people still operate under the assumption that oral sex is risk-free when it comes to STDs, and that assumption is how oral infections go undetected for months.
According to the CDC, oral sex is a documented route of chlamydia transmission. What makes this particularly tricky is that pharyngeal chlamydia, infection at the back of the throat, is severely underreported. Most routine STD panels don't include a throat swab unless the patient specifically discloses oral exposure. The testing gap isn't because oral chlamydia is rare. It's because most people and providers aren't looking for it.
The WHO counts chlamydia among the most common bacterial STIs globally, and that's counting only genital cases that make it into surveillance data. The oral picture is almost certainly broader. The latest provisional CDC surveillance report, released in September 2025, confirmed that while overall reported chlamydia cases declined 8% from 2023 to 2024, more than 2.2 million combined STI cases were still reported in the US that year, a reminder that this infection is far from rare even as reporting trends shift.
Can You Have Oral Chlamydia With No Symptoms at All?
Yes, and this is the norm, not the exception. Research consistently shows that roughly 40% of men with oral chlamydia experience no symptoms, and that figure climbs to around 70% in women. The infection sits quietly in the throat, fully transmissible, with no fever, no visible inflammation, and nothing to prompt a test. Feeling fine after oral sex doesn't mean you're in the clear; it means the most common presentation of oral chlamydia looks exactly like how you feel right now.
The British Association for Sexual Health and HIV (BASHH) recommends pharyngeal screening for anyone with known oral sexual exposure, even without symptoms, specifically because relying on symptom presentation leads directly to missed diagnoses. A test that's negative after a symptom check isn't finding the same nothing twice; it's finding something that symptoms couldn't catch on their own.
This gap is especially relevant for anyone who engages primarily in oral rather than penetrative sex, including many queer and trans people whose sexual health conversations with providers often default to genital-only screening. If your provider hasn't asked about your specific sexual practices, raise it yourself and ask for pharyngeal testing to be included.
What Oral Chlamydia Symptoms Actually Look Like, Men vs. Women
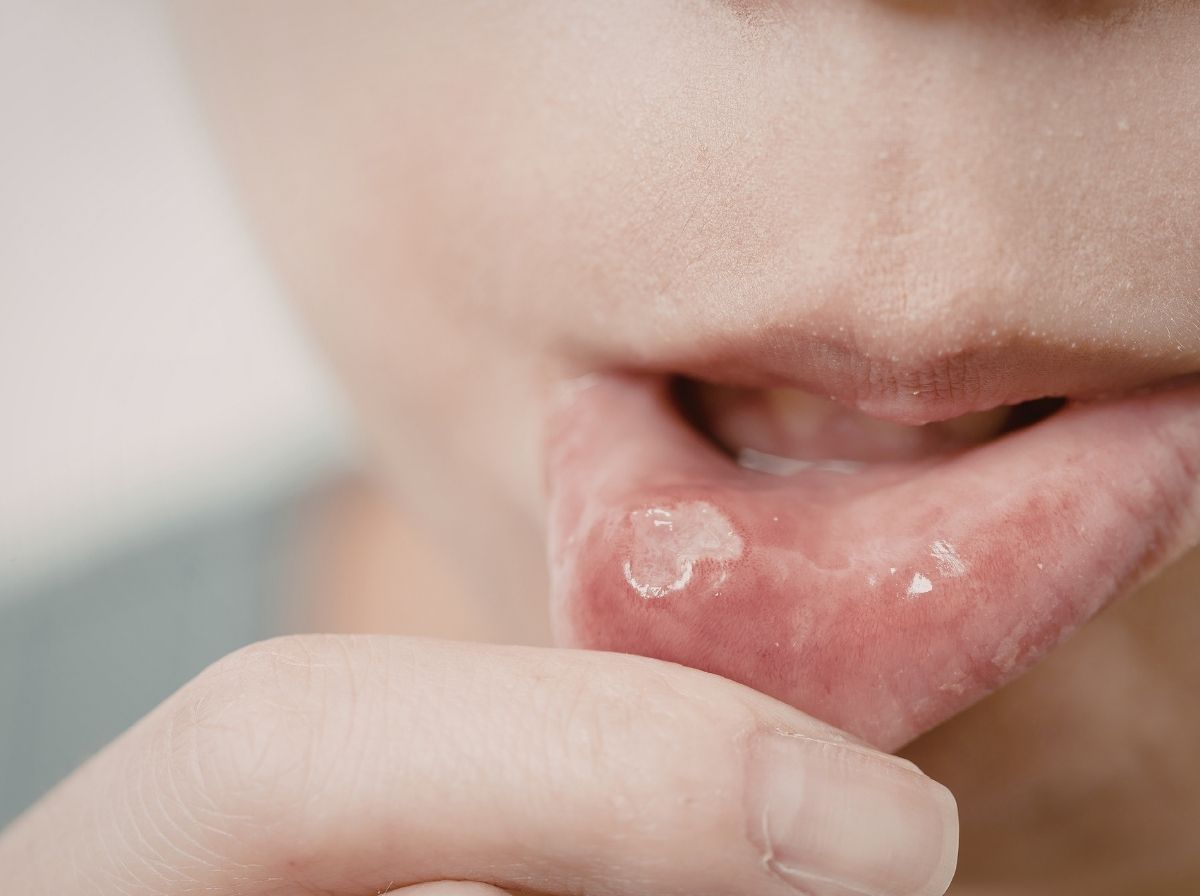
Oral chlamydia symptoms include a persistent sore throat, white patches on the tonsils, swollen lymph nodes under the jaw, and occasional mild fever. These symptoms appear in roughly 60% of men with the infection and as few as 30% of women, the rest have no symptoms at all. When they do appear, they're easy to dismiss: the scratchy throat that won't quite clear, mild tonsil swelling that doesn't feel severe enough to act on, a vague sense of being slightly off. Most people chalk it up to a cold or allergies and wait it out.
The key difference between a cold and oral chlamydia is persistence without progression. A viral sore throat usually worsens for a few days, then resolves within a week. Throat discomfort from chlamydia tends to stay flat, low-grade, unchanging, never quite bad enough to push someone to a clinic. That's part of what allows it to go undetected long enough to be passed on.
In men specifically, the presentation is more likely to be noticeable: visible tonsil inflammation, occasionally with white spots, and swollen lymph nodes under the jaw that can be felt. It's still easy to misread as strep, but there's usually something there to notice. Chlamydia in men follows this same pattern at the genital level, more visible than in women, but still frequently missed without testing.
In women, the oral presentation is typically quieter: mild throat irritation, occasional redness, sometimes a strange taste. Or nothing at all. The same pattern holds with genital chlamydia in women, silent infections are the norm rather than the exception, which is exactly why women are more likely to go undiagnosed and unknowingly carry the infection longer.
People are also reading: Is Oral Sex Safe? Why You Can Still Catch STDs Without Penetration
How Long After Oral Sex Do Symptoms Appear, and When Should You Test?
Picture leaving an encounter feeling completely fine, three days pass, then a week. There's a faint scratchy feeling at the back of the throat, barely worth mentioning. By the time it might be worth mentioning, the symptoms may have already faded, or may never have appeared. This is the typical oral chlamydia trajectory, and it's why timing matters as much as symptoms when deciding whether to test.
For those who develop symptoms at all, the incubation period runs between 7 and 14 days. Throat tissue tends to produce a milder, slower immune response than genital tissue, which is part of why pharyngeal symptoms are often subtle or absent. Someone can be 10 days post-exposure, feeling nothing, and still have a fully active infection.
The right time to test is 14 days after exposure, not sooner. Testing before that window gives the bacterial load insufficient time to reach detectable levels, which produces false negatives that feel like reassurance but aren't. Chlamydia isn't always detectable right away, and a negative result before 14 days isn't a clean bill of health. If you tested early and still have symptoms, retesting at the 14-day mark is the right move.
One practical note on at-home kits: most standard chlamydia tests are designed for genital samples, urine or a urethral/vaginal swab. To test for oral chlamydia, you need a kit that explicitly includes or supports a throat swab. Don't assume a standard chlamydia kit covers the pharynx. Check the product description before ordering, or contact the provider directly. This at-home chlamydia test kit is discreet, fast, and gives you a result you can act on.
What a Positive Result Means, and How to Make Sure It's Actually Resolved
Testing positive for oral chlamydia is information, not a crisis. Treatment works and it's straightforward. What matters most is that every site of infection gets addressed, not just the one that happened to get tested.
If you had both oral and genital exposure with the same partner, both sites need to be tested independently. A provider who only treats genital chlamydia while the throat goes untested leaves half the picture unaddressed. The throat infection remains active, remains transmissible, and can cycle back through oral-genital contact, which is how most reinfections happen. Knowing when it's actually safe to resume sexual activity means confirming clearance with a follow-up test, not guessing from how you feel.
A 2023 study published in the journal Sexually Transmitted Diseases found that reinfection rates are meaningfully higher among people with untested or untreated oral exposure, reinforcing that full-site testing at diagnosis isn't just ideal, it's what actually breaks the transmission chain. Complete the full antibiotic course, avoid sexual contact during treatment, and retest at 3 to 4 weeks. If the follow-up comes back negative, the infection is cleared. If it comes back positive, the conversation with your provider needs to include all exposure sites, genital and pharyngeal.
Telling a Partner, Without Making It Harder Than It Needs to Be
Telling someone you may have exposed them to an oral STD isn't comfortable, but it's one of the most genuinely considerate things you can do. Most oral chlamydia is passed without anyone realizing it, not because of recklessness, but because no one is routinely testing their throat. You didn't know. They probably don't know either. The notification isn't to blame. It's a heads-up that might save them a longer, more complicated situation later.
A simple, shame-free approach:
"Hey, I just got tested and found out I have chlamydia, oral. I didn't have symptoms, so I had no idea. Just wanted to let you know so you can get checked too, especially a throat swab."
No accusation. No drama. Just information the other person needs to make their own decision. If direct notification feels difficult, some sexual health clinics and online services offer anonymous partner notification tools, where a message goes out without your name attached. That's a legitimate option and worth knowing about.
FAQs
1. Can you really get chlamydia from giving oral sex?
Yes. If your mouth comes into contact with an infected penis, vagina, or anus, the bacteria can take hold in your throat. You don't need cuts or abrasions; mucosal contact is enough. This happens across all genders and orientations, and oral sex being "lower risk" than penetrative sex doesn't mean no risk.
2. What does oral chlamydia feel like?
Often it feels like nothing at all. When symptoms do appear, they look like a persistent scratchy sore throat, mild tonsil swelling, or a swollen gland under the jaw, all easy to write off as a cold or allergies. Men tend to have more noticeable symptoms; women are more likely to be entirely asymptomatic.
3. Can you have chlamydia in both your throat and genitals at the same time?
Absolutely. If you had both oral and genital exposure with an infected partner, both sites can be infected independently. Treatment for genital chlamydia alone doesn't clear the throat infection, which is why full-site testing matters every time.
4. Will a regular STD test check my throat?
Not automatically. Standard chlamydia tests use urine or genital swabs and don't include the throat unless you specifically ask for pharyngeal testing. This applies to both clinic testing and most at-home kits. If you've had oral sex, confirm the kit covers throat swabs before ordering.
5. Can I have oral chlamydia if I feel completely fine?
Yes, and that's the norm. Up to 70% of women and around 40% of men with oral chlamydia have no symptoms at all. Feeling fine is not the same as testing negative. Routine testing after new partners is the only reliable way to catch it.
6. Does oral chlamydia clear up on its own?
Unlikely. It might feel like it does if symptoms fade, but the infection can persist and transmit while you feel nothing. Antibiotics clear it reliably, but only if you know it's there. Waiting to see if it "goes away" isn't a strategy; it's just untreated transmission.
7. How soon after oral sex should I test?
Wait 14 days after exposure. Testing earlier can produce a false negative because the bacterial load hasn't reached detectable levels yet. If you tested before the 14-day mark and got a negative, retest before treating that result as final.
8. Is kissing a transmission risk for chlamydia?
No. Chlamydia needs oral-genital or oral-anal contact to transmit; saliva-to-saliva contact during kissing doesn't carry that risk. If your only exposure was kissing, chlamydia isn't the concern here.
9. What should I say to a partner if I test positive?
Keep it direct: "I got tested and found out I have oral chlamydia. I didn't have symptoms, so I had no idea, just wanted you to know so you can get a throat swab done too." You're not confessing anything. You're giving someone health information they need.
10. Can I test for oral chlamydia from home?
Yes, but confirm the kit includes a throat swab option; many standard at-home chlamydia kits only cover genital samples. Look for explicit language about pharyngeal testing before ordering, or contact the provider if it's unclear.
Testing for Oral Chlamydia at Home: What You Actually Need
Oral chlamydia sits in a blind spot of routine sexual health screening, not because it's rare, but because most people and most providers aren't actively looking for it. Symptoms can mimic a cold, stay subtle enough to ignore, or never appear at all. None of that means you're in the clear. Testing is the only way to know.
If you had a single oral exposure and want targeted confirmation, the at-home chlamydia test is the straightforward starting point, fast, discreet, and actionable. If you had both oral and genital exposure, the Chlamydia & Gonorrhea 2-in-1 covers both infections at once, since gonorrhea can also establish itself in the throat after oral sex. For comprehensive screening across the most common infections, the 7-in-1 complete kit covers chlamydia, gonorrhea, syphilis, HIV, hepatitis B, hepatitis C, and herpes HSV-2 from a single home collection. The full range is at STD Test Kits.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. About STI Risk and Oral Sex | CDC
3. Sexually Transmitted Infections Surveillance, 2024 (Provisional) | CDC
4. Sexually Transmitted Diseases Journal – Persistent Chlamydia Study (2023)
5. Chlamydia: Symptoms and Causes | Mayo Clinic
6. Chlamydia: Causes, Symptoms, Treatment & Prevention | Cleveland Clinic
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: A. Liu, FNP-C | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.







