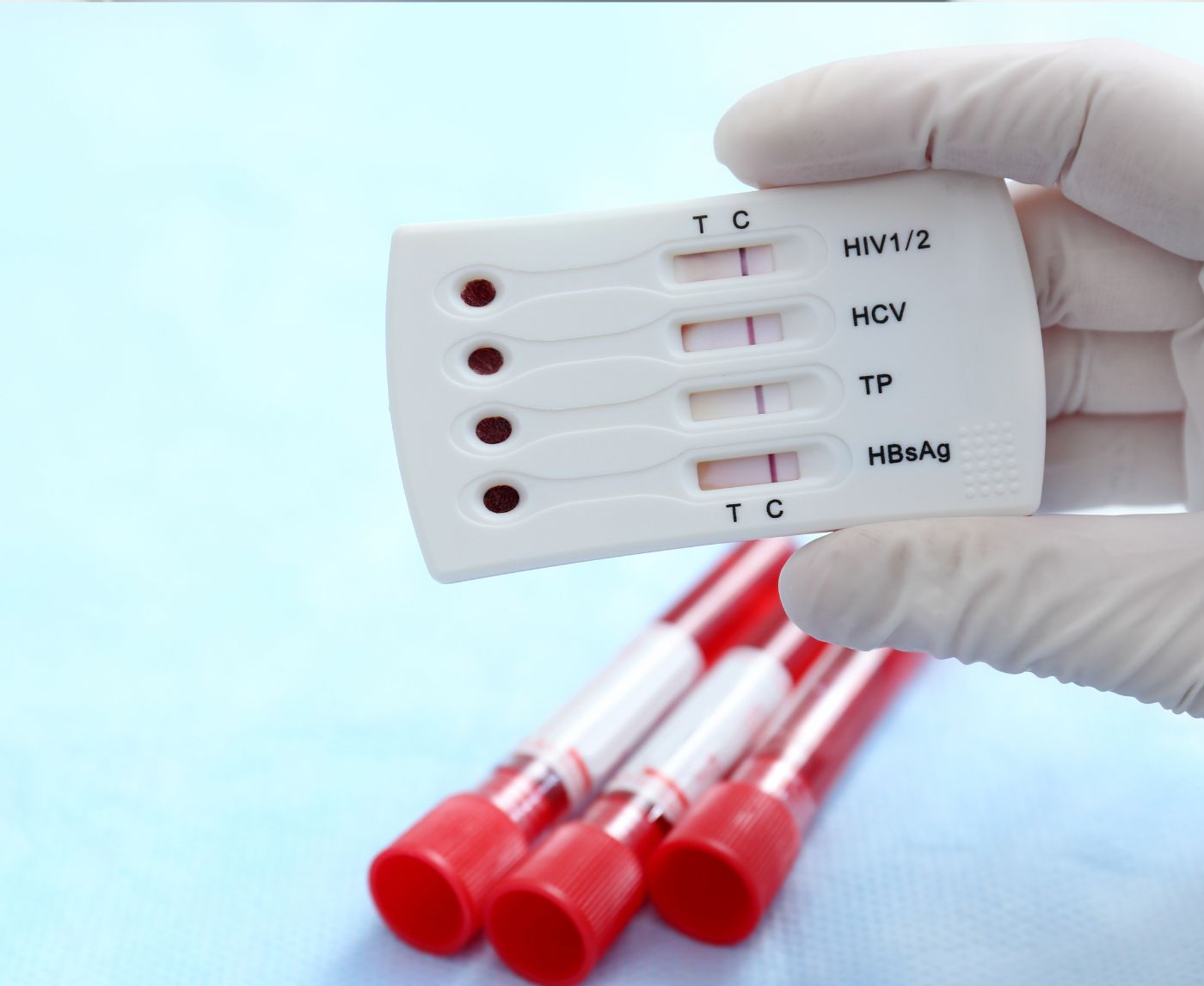
Think You Have HIV? Why Testing Too Early Can Backfire
Quick Answer: A sore throat after oral sex can be an early symptom of an STD, including HIV, but it’s also commonly caused by non-STD infections. If the pain lasts longer than a few days, comes with white patches, swollen lymph nodes, or mouth sores, it’s time to test.
Why This Guide Exists (And Who It’s For)
If you’re here, you probably searched something like “can you get HIV from oral” or “STD sore throat vs strep.” That means you're worried, and likely in a state of panic, shame, or total uncertainty. Maybe you can’t go to a doctor right now. Maybe you don’t want anyone to know you even have this question. This article is for you.
We wrote this for people who are nervous, newly sexually active, exploring oral sex without condoms or barriers, or just navigating symptoms that aren’t going away. It’s also for people living in places where testing access is limited, or where stigma makes it hard to ask the right questions out loud. Whatever brought you here, we’ve got you.
In this guide, you’ll learn the truth about oral HIV symptoms (including what they don’t feel like), what other STDs can affect your throat, how timing affects testing, and when to take action. You’ll also see what real people have experienced, based on anonymized narratives and clinical data.

People are also reading: WHO Just Changed the HIV Guidelines. Here’s What That Means If You’re Testing at Home
What Does Oral HIV Actually Feel Like?
One of the biggest myths is that HIV “shows up” clearly in the mouth right after exposure. In truth, most people who acquire HIV, including through oral sex, have no noticeable symptoms for weeks. But for those who do, the earliest signs are often mistaken for a cold, mono, or even COVID.
The medical term for this early phase is acute retroviral syndrome (ARS), and it usually shows up 2 to 4 weeks after exposure. When HIV does cause mouth-related symptoms early on, they may include:
Figure 1. Oral HIV symptoms typically occur during the acute phase and may resemble common infections. Testing is the only way to know for sure.
“I Thought It Was Just From Singing Too Loud”
Jordan, 27, was fresh off a karaoke night and thought the sore throat was from belting 2000s hits. “It burned when I swallowed, but I didn’t think much of it. Then I noticed white spots on the back of my throat, like little ulcers, and my neck was tight.”
“I was googling strep, mono, even COVID. HIV never crossed my mind until a friend mentioned that oral sex can spread it. I didn’t even know HIV could live in the throat.”
Jordan took an at-home oral HIV test 17 days after exposure. It was negative, but he retested at 6 weeks, when results are more reliable. The second test came back positive. He started antiretroviral therapy immediately and hasn’t had symptoms since.
This isn’t about fear. It’s about catching what others miss, and giving yourself the chance to act early. The first 30 days matter.
Can You Really Get HIV from Oral Sex?
Let’s get real: yes, you can get HIV from oral sex, but the risk is lower than with vaginal or anal intercourse. That said, “lower” doesn’t mean zero, especially if there are open sores, bleeding gums, untreated STDs, or ejaculation in the mouth.
According to CDC data, the estimated risk of HIV transmission through oral sex is very low, but it increases under certain conditions:
- Risk is higher if the person performing oral sex has cuts, ulcers, or recent dental work
- Risk is higher if the person receiving has a high HIV viral load and ejaculates in the mouth
- Risk is higher if either partner has another untreated STD
So while the numbers may be small, they’re not irrelevant. Especially when symptoms follow close behind.
What makes oral HIV even harder to detect is that people assume it doesn’t happen. This leads to delayed testing and more transmission. If you’ve had unprotected oral sex, especially with a new or unknown partner, it’s worth testing at the right time, even if you “feel fine.”
And yes, you can take an HIV test at home using either a fingerstick or oral swab, depending on the test type. We'll cover how soon testing works below.
STDs That Can Cause a Sore Throat (Besides HIV)
Here’s something no one tells you: HIV is not the only STD that shows up in your throat. In fact, gonorrhea, chlamydia, syphilis, and even herpes can infect the mouth and throat during oral sex. And some of them mimic everyday colds or strep.
So if you’ve got a sore throat, swollen tonsils, or white spots after oral sex, don’t assume it’s nothing. Here’s how some common STDs can show up orally:
Figure 2. Oral STD symptom comparison by infection and timeline. HIV often overlaps with common viral symptoms, which makes testing even more crucial.
This Isn’t Just Strep: How to Know When It’s Something Else
A big question we hear from readers is: “How do I know if it’s an STD and not just strep throat?” Here’s the tough truth: you can’t tell based on symptoms alone. But certain patterns can help guide your next step.
Consider this comparison:
Figure 3. Strep vs STD in the throat: Overlapping symptoms but different patterns. Use this to guide, but not replace, testing decisions.
When to Test After Oral Sex (And Which Test Works Best)
If you’re feeling symptoms right now, the urge to test immediately is strong, and valid. But the timing of the test is just as important as the type. Testing too early can give you a false sense of security. Here's what to know:
If it's been less than 5 days: Most tests won't catch infection yet. Exception: if you have intense symptoms or visible ulcers, a clinician may swab the throat or test blood early for markers.
If it's been 7–14 days: You’re in the “gray zone.” Rapid tests for gonorrhea, chlamydia, or herpes may work, but a follow-up test at the optimal window (often 3+ weeks) is usually needed.
If it's been 3–6 weeks: Now is the best time to take a full panel or an at-home combo STD test. Most STDs, including HIV, will show up by now. Rapid tests for oral HIV using blood (not just oral swab) are more accurate at this stage.
If your head keeps spinning, peace of mind is one test away. Order a discreet combo test kit here, it’s lab-backed, private, and ships fast.
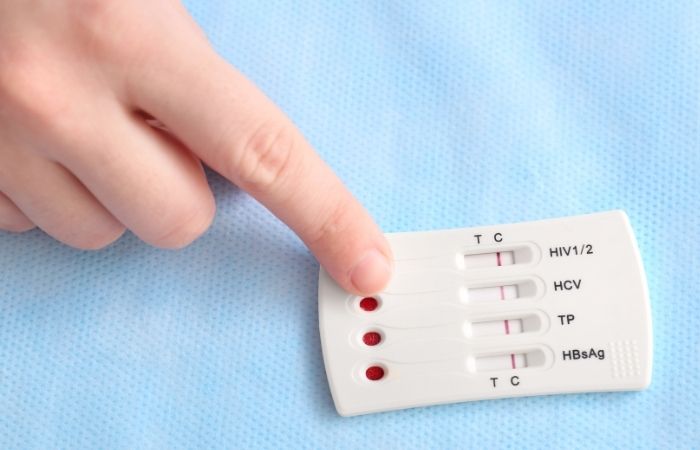
People are also reading: If You Can Talk About Your Wild Night, You Can Talk About STD Testing
Should You Retest? Here’s How to Know
One of the most common mistakes people make after a risky encounter is testing too soon, and then not retesting. But here’s the deal: some infections take time to become detectable. A negative test early on doesn’t always mean you’re in the clear.
If your first test was within 7–14 days of exposure, and it came back negative, that’s not the final word. Most clinicians and test manufacturers recommend a follow-up test at or after the 28-day mark. For HIV, some experts advise waiting up to 6 weeks for best accuracy, depending on the test type.
If you tested positive for anything, retesting is still part of the process, either to confirm the result or to ensure your treatment worked. And if you’re sexually active with new partners, regular testing (every 3–6 months) is a healthy habit, not a red flag.
Scenario: Retesting Saved Him from Misdiagnosis
Chris, 34, took a rapid STD test 9 days after unprotected oral sex. It was negative. But his sore throat kept getting worse. “I felt like a hypochondriac going back to test again,” he said. “But the second test showed chlamydia in my throat. I would’ve kept spreading it if I hadn’t followed my gut.”
“Testing twice saved me. I’d rather deal with awkward than with untreated infection.”
If that’s you, still unsure, still anxious, it’s not overreacting to double-check. It’s owning your health.
Privacy, Shipping, and Discreet Support
Let’s talk about the part that stresses people out the most, getting tested without anyone knowing. Whether you live with roommates, have a judgmental doctor, or just value your space, here’s what you need to know:
At-home test kits from reputable providers like STD Test Kits come in plain, unbranded packaging. There are no logos or labels on the outside that say what’s inside. Kits usually ship within 24 hours and can be delivered to your home, work, or PO box.
Results are yours and yours alone. No one sees them unless you choose to share. Most test types require a small blood sample (via fingerstick) or a mouth swab. Either way, it takes just a few minutes, and you’ll have results quickly.
Some users report testing in their cars, in a bathroom at work, or while visiting a partner. The point is: you choose where and when. The power’s back in your hands.
What If Your Test Comes Back Positive?
First: breathe. Testing positive for an STD, whether it’s HIV, gonorrhea, chlamydia, or anything else, isn’t the end of the world. It’s the beginning of taking care of yourself, and maybe someone else too.
Here’s what to do:
- Confirm the result with a second test, especially if it was an at-home screening
- Start treatment if the infection is treatable (most are!) or begin care planning for long-term management like HIV
- Notify partners, anonymously if needed, so they can get tested too
Maria, 22, said it best: “I cried when I saw the word 'positive.' But then I remembered: this is why I tested, to stop the spiral, not feed it.”
“It wasn’t a death sentence. It was a wake-up call. I got on meds, told my ex, and booked a therapist. All in 24 hours.”
Whatever your result, there’s a next step. And it’s not fear. It’s information, care, and control.
Want to help protect your partners too? You can send them a link to order a combo test kit of their own, quick, private, no awkward clinic visit.
FAQs
1. Can HIV cause a sore throat right away?
Not right away, but it can be one of the first signs a couple of weeks in. If your throat hurts 24 hours after oral sex, it’s probably not HIV. But if it starts feeling raw, weirdly persistent, or comes with swollen glands and fatigue around weeks 2 to 4, that’s when it can signal acute HIV. The trick is: it doesn’t always show up, and when it does, it looks a lot like strep or a cold. That’s why testing matters more than guessing.
2. What does an HIV sore throat feel like?
It’s not one-size-fits-all, but many people describe it as a scratchy, burning pain that doesn’t go away after a few days, and doesn’t improve with rest or fluids. Think: “I’ve had worse sore throats… but this one’s weird.” Some also notice white spots, swollen lymph nodes under the jaw, or canker-like ulcers in the mouth. It’s not always dramatic, which makes it easy to miss.
3. Can you really get an STD from oral sex?
Yes, unfortunately, that’s a hard yes. Giving or receiving oral can pass on chlamydia, gonorrhea, syphilis, herpes, and even HIV in some cases. The risk is lower than vaginal or anal, but it’s definitely not zero. Especially if there’s no barrier, ejaculation happens in the mouth, or someone has a cut or sore. And a lot of oral STDs don’t cause symptoms, so people keep passing them without knowing.
4. How soon should I get tested after oral sex?
It depends on what you're worried about. Throat swabs can show some STDs, like gonorrhea or chlamydia, as soon as a week after being exposed. But the type of HIV test matters: a fingerstick rapid test is more accurate after three weeks, while lab-based tests can find it a little earlier. If you test early and get a negative result, test again at the 4- to 6-week mark to be sure.
5. Can a sore throat be the only symptom of an STD?
Yep. It happens more than you’d think. Sometimes that’s all you get, a nagging throat ache that lingers, maybe a little swelling, no fever, no drama. Then you test and bam: it’s gonorrhea or even early HIV. That’s why “just a sore throat” shouldn’t be dismissed if it shows up after oral sex.
6. How do I know if it’s strep or something else?
Strep usually hits like a truck, fast onset, high fever, and pus on your tonsils. An STD sore throat is more sneaky: it may come on slower, hurt differently, and doesn’t always respond to antibiotics the way strep does. If your doctor gives you meds and nothing changes in a few days? Time to look into STD testing.
7. Can I test for oral HIV at home?
Yes, and it's way easier than you think. You can use an oral swab test or a blood-based fingerstick kit. Blood tests tend to be more accurate, especially in the early window period. Just make sure you're using an FDA-approved kit from a trusted source like STD Test Kits. And remember: testing once isn’t always enough, timing is key.
8. What happens if I test positive for something?
First, breathe. Then get a confirmatory test, especially for HIV. If it's something like gonorrhea or chlamydia, you'll likely get antibiotics and be done. If it’s HIV, starting treatment early means staying healthy and undetectable. It’s a lot emotionally, but you’re not broken or dirty. You’re a person who tested, which already makes you braver than most.
9. Are oral STDs actually common?
Weirdly, yes, but most people don’t realize it. Tons of folks have oral gonorrhea or chlamydia and don’t know, because they never have symptoms and never think to swab the throat. Public health data shows that many infections live quietly in the mouth and still spread during oral sex.
10. If I might have an oral STD, can I still kiss?
Tricky question. Some STDs like herpes and even syphilis can spread through kissing, especially during an outbreak or if there’s an open sore. If your mouth feels off, or you’re worried, maybe hold off on kissing until you’ve tested. Better awkward than infected, right?
You Deserve Answers, Not Assumptions
If your throat hurts and your mind won’t shut up, you’re not alone. Whether it’s a new partner, an old mistake, or just confusion around symptoms, there’s power in knowing. You don’t need to wait for a clinic, justify your fears, or pretend nothing happened. You just need a clear next step.
Don’t guess. Don’t spiral. Order a discreet at-home combo test kit today and get the clarity you deserve, in your space, on your terms.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted some of the most relevant and reader-friendly sources.
Sources
1. NHS: HIV Symptoms and Diagnosis
2. About STI Risk and Oral Sex – CDC
3. Sexually Transmitted Infections Treatment Guidelines (throat infections and oral exposure) – CDC
4. About Gonorrhea (includes pharyngeal infection from oral sex) – CDC
5. About Chlamydia (pharyngeal infection risk) – CDC
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He combines clinical accuracy with a straightforward, sex-positive approach and is dedicated to making his work available to more people in both cities and rural areas.
Reviewed by: Renee LeClair, FNP-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.