How Long Should You Wait to Retest for STDs After Antibiotics?
Quick Answer: Strawberry cervix is a visual pattern of small red spots on the cervix most commonly associated with Trichomoniasis, a treatable sexually transmitted infection. It does not automatically mean cancer, and it does not confirm an infection without proper testing.
First, Let’s Translate the Drama Out of the Name
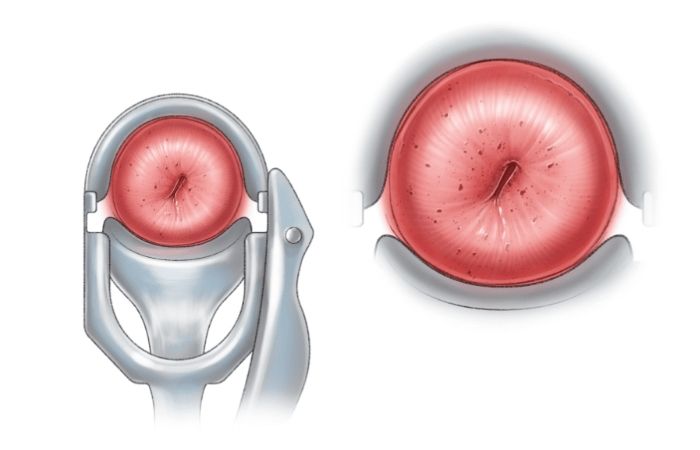
“Strawberry cervix” is not a diagnosis. It’s a visual description. During a pelvic exam, a clinician may see tiny red pinpoint spots on the surface of the cervix. The medical term for this appearance is colpitis macularis. It looks speckled, almost like the surface of a strawberry, which is how the nickname stuck.
The cervix itself is simply the lower part of the uterus that opens into the vagina. It naturally changes color and texture depending on hormones, inflammation, and infection. When it becomes irritated, tiny capillaries can dilate and create that dotted red pattern.
Here’s the important part: the appearance alone doesn’t confirm anything. It’s a clue, not a verdict.
According to the CDC’s guidance on Trichomoniasis, strawberry cervix is considered a classic but not universal finding in people with this infection. Many cases of trichomoniasis don’t show this pattern at all. And many people with this pattern may have mild inflammation from other causes.
People are also reading: STD Symptoms in Women That Don’t Involve the Vagina
So… Is Strawberry Cervix an STD?
This is the question that sends people into a spiral at 1:00 a.m. Is strawberry cervix an STD? The honest answer is layered.
Strawberry cervix is most commonly associated with Trichomoniasis, a sexually transmitted infection caused by a parasite called Trichomonas vaginalis. According to the World Health Organization, trichomoniasis is one of the most common non-viral STIs globally, affecting millions each year.
But here’s what gets lost in translation online: seeing a strawberry cervix does not automatically mean you have trichomoniasis. It also does not mean you have multiple STDs. It doesn’t even confirm infection without laboratory testing.
Think of it like a rash. A rash can be allergic, infectious, hormonal, or friction-based. The pattern alone isn’t enough. Doctors confirm trichomoniasis through lab testing, often a nucleic acid amplification test (NAAT), which detects the parasite’s genetic material. The Mayo Clinic explains that lab testing, not visual inspection, is the reliable way to diagnose it.
So if your chart mentions strawberry cervix but no positive lab result, you don’t have a confirmed STD. You have a visual note that may prompt further testing.
What Actually Causes That “Strawberry” Pattern?
Most often, it’s inflammation. And inflammation has many possible triggers.
With trichomoniasis, the parasite irritates the vaginal and cervical lining. This irritation leads to small hemorrhagic spots, tiny bleeding points under the surface, that create the speckled look. That’s the textbook explanation. But textbooks don’t always reflect real life.
Other causes of cervical inflammation can include bacterial vaginosis, recent sexual friction, hormonal shifts, or even a reaction to new products. The NHS overview of trichomoniasis notes that while discharge and irritation are common, many people have mild or no symptoms at all.
To ground this in reality, here’s how strawberry cervix compares to other cervical changes:
The takeaway is steady and boring, and that’s good news. The cervix reacts to irritation in visible ways. The pattern isn’t destiny.
The Symptoms People Notice (And The Ones They Don’t)
When strawberry cervix is linked to trichomoniasis, symptoms may include frothy green or yellow discharge, a strong vaginal odor, itching, burning during urination, or discomfort during sex. Some people search phrases like “vaginal discharge green frothy” or “trichomoniasis symptoms female” and land in a panic spiral.
But here’s the reality that doesn’t trend on social media: up to 70% of people with trichomoniasis may have mild symptoms or none at all, according to CDC data. That means someone can have the infection without dramatic discharge or pain.
One patient once told me, “I kept waiting for something obvious to happen. I thought an STD would feel louder.” That’s the myth. Many STIs don’t announce themselves.
This is why testing matters more than guessing. If you were told your cervix appeared inflamed or “strawberry-like,” and especially if you have new discharge or irritation, a targeted test for trichomoniasis is the next logical step, not self-blame.
If you prefer privacy, at-home options exist. You can explore discreet testing kits at STD Test Kits, including options that screen for common infections without a clinic visit. Getting clarity shouldn’t require sitting in a waiting room replaying every hookup in your head.
What It Doesn’t Mean: Let’s Calm the Biggest Fears
This is the section your nervous system is waiting for.
Strawberry cervix does not automatically mean cervical cancer. The speckled appearance associated with trichomoniasis is inflammatory, not malignant. Cervical cancer involves abnormal cellular changes typically detected through Pap smear results and confirmed with biopsy, not a simple red dot pattern.
It also does not mean you’ve had multiple partners or “did something wrong.” Trichomoniasis can be transmitted through sexual contact, and like many STIs, it can remain asymptomatic for long periods. Someone can carry it without knowing. That includes long-term partners.
And finally, it does not mean your body is damaged beyond repair. Trichomoniasis is treatable with antibiotics. According to the CDC treatment guidelines, a standard course of metronidazole or tinidazole is highly effective.
The internet often collapses inflammation, infection, and cancer into one terrifying blob. Medicine doesn’t work that way. These are separate pathways with separate tests and separate treatments.
When Should You Actually Get Tested?
If the phrase “strawberry cervix” showed up in your chart, the next thought is usually: how soon do I need a test, and what kind?
With Trichomoniasis, the incubation period, the time between exposure and when infection can be detected, typically ranges from about 5 to 28 days. Some people develop irritation within a week. Others feel completely normal for weeks or even months.
Testing too early can give false reassurance. Testing too late can mean unknowingly passing it to a partner. The sweet spot is usually about two weeks after a potential exposure, but if symptoms appear earlier, testing right away is reasonable.
According to the CDC Treatment Guidelines, nucleic acid amplification tests (NAATs) are highly sensitive for detecting trichomoniasis. These tests look for the parasite’s genetic material rather than just visual signs.
Notice what’s not in that table: panic. Timing improves clarity. That’s it.
Can You See a Strawberry Cervix at Home?
This question pops up more than you’d think. People search things like “can you see strawberry cervix” or try to self-diagnose using mirrors and flashlights.
The short answer is no. The cervix sits at the top of the vaginal canal. Even with a mirror, it’s extremely difficult to evaluate without proper lighting and a speculum. And even if you could see it, interpretation requires clinical training.
A red cervix does not equal trichomoniasis. A smooth cervix does not rule it out. Visual self-checks often increase anxiety rather than provide answers.
If your concern is real, and it probably feels very real, testing beats guessing every time.
What Happens If the Test Is Positive?
Let’s say the lab confirms Trichomoniasis. What now?
First, understand this: trichomoniasis is treatable. A short course of prescription antibiotics, usually metronidazole or tinidazole, clears the infection in the vast majority of cases. The Mayo Clinic confirms that treatment is straightforward and effective when taken as directed.
Second, partners need treatment too. Reinfection happens when one person completes antibiotics and the other doesn’t. It’s not about blame. It’s about preventing the cycle from repeating.
A patient once told me, “I felt more embarrassed telling my partner than I did taking the pills.” That’s common. But trichomoniasis is one of the most common non-viral STIs worldwide. It’s a medical event, not a moral one.
After treatment, many clinicians recommend retesting within about three months because reinfection rates can be significant. That follow-up isn’t a sign of failure. It’s a safety net.

People are also reading: STD Symptoms in Women That Don’t Involve the Vagina
What If the Test Is Negative?
If your test comes back negative and you were told you have a strawberry cervix, then there is probably another reason for the inflammation.
Temporary irritation of the cervix can happen because of friction during sex, recent tampon use, bacterial vaginosis, yeast imbalance, or even changes in hormones. In these instances, the redness dissipates once the underlying irritation subsides.
If you still have discharge, smell, or pain after a negative trichomoniasis test, you may need to be checked for other infections. This is why it makes sense to get a full screening, especially after getting a new partner.
If you're not sure what to test for, combination panels can check for a number of common infections at once. STD Test Kits offer discreet options, such as multi-STD testing kits that let you collect samples in private and get results that are kept secret.
Strawberry Cervix vs. Cervical Cancer: A Necessary Separation
Let’s untangle the most catastrophic search query: “strawberry cervix vs cervical cancer.”
Cervical cancer is primarily linked to persistent high-risk strains of HPV, not trichomoniasis. Cancer develops from abnormal cellular changes over time. These changes are detected on Pap tests as dysplasia or abnormal cytology, not as speckled redness alone.
A strawberry-like appearance is inflammatory. Cancer involves structural and cellular changes confirmed by pathology. They are not interchangeable.
If your Pap smear was normal aside from inflammation, that’s reassuring. If your Pap showed abnormal cells, that is a separate conversation with separate follow-up steps, often including repeat testing or colposcopy.
Conflating inflammation with malignancy is one of the internet’s favorite fear tricks. Medicine separates them carefully for a reason.
Does Trichomoniasis Go Away on Its Own?
Another common search: “does trich go away on its own?”
Sometimes symptoms fluctuate. Discharge may lessen. Irritation may fade. That does not mean the infection is gone. Untreated trichomoniasis can persist for months or even years and may increase susceptibility to other STIs.
Treatment is simple. Ignoring it complicates things. If testing confirms infection, antibiotics are the cleanest path forward.
Peace of mind is rarely found in waiting and hoping.
The Partner Conversation No One Prepares You For
If testing confirms Trichomoniasis, the medical part is straightforward. The emotional part can feel heavier. Even people who understand that STIs are common still hesitate when it’s time to text a partner.
One patient, Alina, told me, “I kept rewriting the message. I didn’t want it to sound like an accusation.” That fear is common. But trichomoniasis can be asymptomatic for long stretches. Someone can carry it unknowingly. The presence of infection doesn’t automatically reveal when it started or who had it first.
The cleanest approach is simple and factual: you tested positive, it’s treatable, and they should get tested too. No courtroom energy. No detective work. Just shared health responsibility.
According to the CDC partner management guidance, treating all sexual partners is essential to prevent reinfection. That’s not about blame. It’s about breaking the transmission cycle.
Reinfection: The Quiet Loop People Don’t Expect
Here’s something rarely explained clearly: trichomoniasis has a notable reinfection rate. You can take your antibiotics exactly as prescribed, feel completely better, and still test positive weeks later if a partner wasn’t treated.
That’s why many clinicians recommend retesting within three months after treatment. Not because they assume you did something wrong. Because statistically, reinfection happens.
Picture this scenario: you finish treatment, symptoms disappear, and life moves on. A month later, irritation returns. It’s not necessarily a new partner or a new mistake. It might simply be untreated reinfection.
This is where a calm follow-up plan matters more than guilt.
What If You’re in a Long-Term Relationship?
When someone in a long-term relationship hears “strawberry cervix” linked to Trichomoniasis, the first fear isn’t medical. It’s relational.
Trichomoniasis can persist without symptoms. Research shows it may remain undetected for extended periods. That means a positive test does not automatically equal recent infidelity. It does not provide a timeline stamp.
These infections don’t come with date labels. They come with treatment plans.
If the relationship feels stable and trusting, approach this as a shared health update, not a cross-examination. If trust is already fragile, testing can still be framed as proactive care rather than accusation.
When Strawberry Cervix Isn’t Trichomoniasis
Let’s circle back to something critical: strawberry cervix is most commonly associated with trichomoniasis, but it is not exclusive to it.
Cervical inflammation can arise from bacterial vaginosis, yeast imbalance, recent sexual friction, hormonal changes, or even mild allergic reactions. Visual findings must be interpreted in context.
The National Center for Biotechnology Information overview of cervicitis explains that cervicitis can be infectious or noninfectious. That distinction matters. Infection requires treatment. Irritation often resolves with time and removal of the trigger.
If your trichomoniasis test is negative but inflammation persists, your clinician may evaluate for other infections such as Chlamydia or Gonorrhea, especially if you have new sexual exposure.
Testing Options: Clinic vs. At-Home
You have options. And having choices makes you less anxious.
Testing at a clinic gives you an immediate professional evaluation and, in some cases, a prescription the same day. It's best if you have a fever, severe pain, or tenderness in your pelvic area. Clinicians can also look at the cervix and take samples directly during in-person exams.
On the other hand, testing at home is private and quick, and you don't have to wait in a waiting room. For a lot of people, the problem isn't getting to the barrier, it's being uncomfortable. You can collect samples privately and get private results without having to talk to anyone at the front desk if you order discreet kits from STD Test Kits.
Both paths are correct. The best choice depends on how bad the symptoms are, how urgent the situation is, and how comfortable you are.
The goal isn’t perfection. It’s clarity.
The Emotional Side No One Mentions
Seeing a term like strawberry cervix can feel embarrassing, even though it’s simply medical shorthand. Many people internalize it as proof of recklessness.
Sex is part of being human. Infections are part of biology. Testing is part of responsibility. Those three statements can coexist without shame.
One person told me, “I felt like my body betrayed me.” Bodies don’t betray. They respond. Inflammation is your immune system doing its job.
If there’s one thing to remember before we move into the final section, it’s this: strawberry cervix is a description, not a character judgment. It’s information that guides testing. Nothing more.

People are also reading: What Is Disseminated Gonococcal Infection (DGI)? Rash, Fever & Joint Pain Explained
What To Do Next, Without Spiraling
If you saw “strawberry cervix” in your chart, here’s your grounded plan. Confirm whether lab testing for Trichomoniasis was done. If not, schedule testing or use a discreet at-home option. If yes, follow the result, not the visual note.
If the test is positive, take the prescribed antibiotics exactly as directed and ensure partners are treated. If negative, monitor symptoms and follow up if irritation continues. Medicine works best when it’s stepwise, not catastrophic.
You deserve clarity, not worst-case scenarios.
If you want privacy and control, you can explore discreet testing options through STD Test Kits. Whether it’s a targeted test for trichomoniasis or a broader screening panel, testing puts facts in your hands instead of rumors in your head.
FAQs
1. Okay, but seriously, is strawberry cervix an STD?
Not by itself. It’s a description of how the cervix looks during an exam. Think of it like a doctor saying “your throat looks red.” That redness might be strep, or it might be irritation. Strawberry cervix is most commonly linked to Trichomoniasis, but the appearance alone isn’t a diagnosis. Testing decides that part.
2. If I have trichomoniasis, would I definitely know?
Not necessarily. That’s the tricky part. Some people get noticeable discharge or burning. Others feel completely fine and only find out during routine screening. I’ve had patients say, “I thought an STD would feel louder.” Sometimes it doesn’t. Silence doesn’t equal safety.
3. My Pap mentioned inflammation. Is that the same thing?
Not exactly. Inflammation just means irritation. It’s your immune system showing up and doing its job. That irritation could be from sex, a new product, a mild imbalance, or an infection. Strawberry cervix is one possible pattern of inflammation, but it’s not the only one.
4. Could this mean cervical cancer?
This is the fear that keeps people up at night. No, strawberry cervix itself is not a cancer diagnosis. Cancer involves abnormal cellular changes, which are detected through Pap results and sometimes biopsy. A speckled red appearance is inflammatory, not malignant. Different pathway. Different testing. Different outcome.
5. How awkward is it to tell a partner?
More awkward in your head than in real life, usually. A simple message works: “Hey, I tested positive for trichomoniasis. It’s treatable, but you should get checked too.” No accusations. No courtroom energy. Just health information. Most partners respond better to calm facts than to panic.
6. Can trichomoniasis just clear up if I wait?
Symptoms might fade, but the infection can linger. It doesn’t reliably “burn out.” And untreated infection can increase susceptibility to other STIs. The antibiotics are straightforward. Waiting tends to stretch anxiety longer than necessary.
7. If I tested negative, why did my cervix look like that?
Bodies react. Friction, hormonal shifts, bacterial vaginosis, even recent tampon use can cause temporary cervical redness. If your lab test is negative and symptoms are mild, the irritation often resolves once the trigger settles. Not every red spot is a crisis.
8. Can men carry trichomoniasis without knowing?
Yes. Men often have fewer or milder symptoms, which is one reason reinfection happens. Someone can genuinely not know they have it. That’s biology, not deception.
9. Do I need a full STD panel now?
It depends on your exposure and comfort level. If you had a new partner or haven’t tested in a while, broader screening can offer peace of mind. If the only concern is a visual finding and trichomoniasis testing was negative, your clinician may not recommend more. When in doubt, clarity beats guessing.
10. Why does this word sound so dramatic?
Because medicine sometimes names things based on appearance, not emotional impact. “Strawberry cervix” sounds scandalous. In reality, it’s just a pattern doctors recognize. Your body isn’t trying to embarrass you. It’s just responding to something.
How We Sourced This Article: This guide combines current CDC and WHO treatment guidelines, peer-reviewed research on cervicitis and colpitis macularis, and clinical diagnostic standards from major medical institutions. Approximately fifteen references informed the writing to ensure accuracy, but we selected the six most accessible and authoritative sources below for reader clarity. Every external link has been verified and opens in a new tab for transparency.
Sources
1. CDC – STI Treatment Guidelines: Trichomoniasis
2. World Health Organization – Trichomoniasis Overview
3. CDC: Trichomoniasis (STI Treatment Guidelines)
4. Mayo Clinic: Trichomoniasis — Symptoms and causes
5. Cleveland Clinic: Trichomoniasis — Causes, Symptoms, Testing & Treatment
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who specializes in preventing, diagnosing, and treating STIs. He has a no-nonsense, sex-positive approach and is dedicated to making it easier for people to get private testing and evidence-based care.
Reviewed by: L. Ramirez, NP-C | Last medically reviewed: March 2026
This article is for informational purposes and does not replace medical advice.