Full STD Panel vs Single Test: How to Choose
Quick Answer: Disseminated gonococcal infection (DGI) occurs when untreated gonorrhea spreads into the bloodstream, causing fever, joint pain, swelling, and a distinctive rash. It is rare but requires urgent medical treatment.
Gonorrhea Isn’t Always “Just” a Genital Infection
Most people think of gonorrhea as a localized STD. It infects the cervix, urethra, rectum, or throat. It’s treated with antibiotics. End of story.
But according to the CDC, gonorrhea doesn’t always stay put. If it isn’t diagnosed and treated, the bacteria Neisseria gonorrhoeae can enter the bloodstream. That’s when things shift from uncomfortable to systemic.
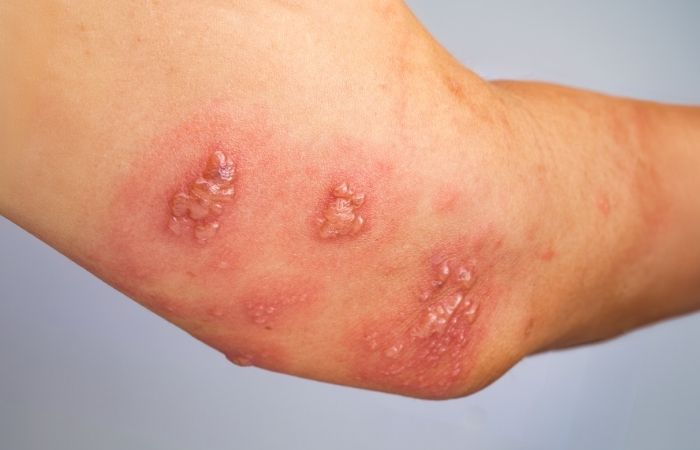
Instead of discharge or burning, DGI often shows up as inflammation in the joints, skin lesions that look like small red or pus-filled spots, and flu-like symptoms. Some people have no obvious genital symptoms at all when the bloodstream infection appears. That’s part of why it gets missed.
One patient, “Arjun,” described it this way: “I thought I had the flu. My knee felt like I’d twisted it. Then I noticed these weird spots on my palms. I didn’t connect it to sex at all.”
That disconnect is common. And it’s dangerous if it delays treatment.
People are also reading: Anal Itch, Burn, or Bleed? How to Tell If It’s an STD or Something Else
What DGI Looks Like Compared to Typical Gonorrhea
Standard gonorrhea symptoms tend to stay near the site of infection. DGI spreads. The difference matters, especially if you’re trying to figure out whether joint swelling or a rash after sex could be related.
Table 1. Comparison between localized gonorrhea infection and disseminated gonococcal infection.
Notice something important here: many people with DGI never had noticeable discharge. Searches like “gonorrhea without discharge” spike for a reason. Up to half of infections in some groups are asymptomatic, according to WHO data.
That means someone can carry the infection silently, and only realize something is wrong when their joints swell or they spike a fever.
If you’re reading this because you have joint pain after sex and can’t explain it, you’re not being dramatic. You’re being observant.
The Rash, The Fever, The Joints: The Symptoms That Set Off Alarms
DGI tends to announce itself in a very specific trio: rash, fever, and migratory joint pain. “Migratory” means the pain moves. One day it’s your wrist. The next, your ankle. Then your knee feels hot and swollen.
The rash can look like small red or purplish spots, sometimes with a tiny blister in the center. They often appear on the palms, soles, or around joints. People frequently Google “gonorrhea rash on hands” because that’s where it’s most visible.
Then there’s the fever. Not always dramatic, but enough to make you feel off. Fatigue creeps in. Your body feels inflamed.
“Elena,” 26, said: “My fingers were stiff. I couldn’t open jars. I had no discharge, no pain peeing. I almost didn’t tell the ER doctor about my new partner because I didn’t think it mattered.”
It did matter. Blood tests confirmed DGI.
In rare cases, untreated DGI can progress to septic arthritis, where infection fills a joint space, or even systemic sepsis. The Mayo Clinic emphasizes that bloodstream infections require immediate antibiotic treatment, usually intravenously.
This is not a “wait and see” situation. If fever and severe joint swelling develop, urgent care or an ER visit is appropriate.
How Does Gonorrhea End Up in the Bloodstream?
This is the part most people don’t realize: gonorrhea doesn’t usually start in the blood. It begins quietly on a mucous membrane, the cervix, urethra, rectum, or throat. From there, if untreated, the bacteria can invade deeper tissues and eventually cross into the bloodstream.
According to the CDC treatment guidelines, disseminated gonococcal infection develops in a small percentage of untreated cases. It’s considered uncommon, but not rare enough to ignore. Certain strains of the bacteria are more likely to spread systemically, and some bodies are more vulnerable than others.
When the bacteria enter the bloodstream, they don’t just float around harmlessly. They trigger inflammation. Your immune system reacts aggressively. That’s why symptoms feel widespread instead of localized.
“Mateo,” 31, described it bluntly: “It felt like my body was fighting something bigger than a UTI. My whole system felt inflamed.”
That systemic inflammation is what separates DGI from a standard infection.
The Timeline: How Long Before Gonorrhea Spreads?
One of the most common searches is “how long before gonorrhea spreads to the blood?” The honest answer is: it varies. There isn’t a fixed countdown clock. But we do understand the general pattern.
Localized gonorrhea symptoms usually appear between two and fourteen days after exposure. If the infection remains untreated, bloodstream spread can occur days to weeks later. Some people develop DGI even when their original symptoms were mild or barely noticeable.
Here’s a simplified progression overview.
Table 2. Simplified timeline of progression from localized gonorrhea to disseminated infection.
Important: not everyone with untreated gonorrhea develops DGI. Many infections remain localized. But because gonorrhea can be asymptomatic, particularly in women and in throat infections, someone may not know they’re carrying it.
That’s why searches like “gonorrhea life threatening” spike when people experience unexplained fever and joint swelling. The fear isn’t irrational. It just needs grounding in facts.
Who Is Most at Risk for Disseminated Gonococcal Infection?
Anyone with untreated gonorrhea could theoretically develop DGI, but certain groups show higher risk in medical literature. People assigned female at birth appear to have slightly higher rates of dissemination. Hormonal fluctuations during menstruation and pregnancy may influence bacterial spread.
Individuals with compromised immune systems may also face increased risk. If your immune response can’t contain the infection locally, bloodstream spread becomes more likely.
There’s also a behavioral layer here. Delayed testing plays a role. If someone assumes symptoms are “just irritation” or avoids care due to stigma, the bacteria have more time to persist.
One ER physician quoted in a PubMed clinical review summarized it this way: DGI often presents in patients who either had mild symptoms or never realized they were infected at all.
This is why regular screening matters, especially if you’ve had new or multiple partners, even if you feel fine.
People are also reading: Do Men and Women Need Different STD Tests? What Actually Changes (And What Doesn’t)
Can Gonorrhea Cause Sepsis?
This is one of the most anxiety-driven searches: “can gonorrhea cause sepsis?” The answer is yes, but rarely. When gonorrhea spreads systemically and isn’t treated promptly, severe inflammatory responses can escalate.
However, most DGI cases are caught and treated before reaching full sepsis. Modern antibiotics are effective when administered appropriately. The key variable is timing.
If someone has high fever, severe joint pain with redness and swelling, rapid heart rate, confusion, or feels acutely ill, emergency evaluation is warranted. Those symptoms are not “wait it out” territory.
But here’s the part people forget: DGI is preventable. Early testing and treatment of localized gonorrhea almost always stop the infection before it spreads.
Why Some People Have No Genital Symptoms at All
It feels unfair. You expect warning signs. You expect discharge or pain. Yet many people with gonorrhea, especially throat or cervical infections, experience nothing obvious.
According to global surveillance data cited by the World Health Organization, a significant proportion of infections are asymptomatic. That silent window allows the bacteria to persist undetected.
That’s why someone might search “STD causing joint swelling” instead of “gonorrhea symptoms.” The body doesn’t always read from the textbook.
This is also why at-home screening options matter. If you’re not experiencing discharge but have had a recent exposure, testing is about clarity, not accusation.
If you want discreet answers without sitting in a waiting room, you can explore testing options at STD Test Kits. Peace of mind isn’t dramatic. It’s responsible.
How Doctors Diagnose Disseminated Gonococcal Infection
When someone walks into urgent care with joint swelling and a fever, gonorrhea is not always the first thing on the provider’s mind. It might look like the flu. It might resemble rheumatoid arthritis. It might even be mistaken for a skin infection if the rash is prominent.
That’s why sexual history matters, even when the symptoms feel unrelated. According to the CDC treatment guidelines, clinicians diagnose disseminated gonococcal infection using a combination of clinical signs and laboratory testing. Blood cultures, joint fluid analysis, and swabs from genital, rectal, or throat sites may all be part of the workup.
Here’s the tricky part: blood cultures are often negative in DGI. The bacteria can be difficult to isolate once the immune system has reacted. That means diagnosis sometimes depends on pattern recognition, rash plus migratory arthritis plus confirmed gonorrhea at another site.
“Nadia,” 29, said: “They kept asking about my partners. I felt embarrassed at first. But when the doctor explained that my ankle swelling could be connected to a throat infection, it finally clicked.”
This isn’t about shame. It’s about connecting dots quickly enough to treat before complications develop.
Testing for Gonorrhea Before It Spreads
If you’re worried about DGI, the bigger question becomes: how do you catch gonorrhea before it reaches the bloodstream?
The gold standard for diagnosing gonorrhea is a nucleic acid amplification test (NAAT), which detects bacterial genetic material. These tests are highly sensitive and are recommended by both the Mayo Clinic and the CDC.
Samples can come from urine, cervical swabs, urethral swabs, rectal swabs, or throat swabs depending on exposure type. That last part matters. If someone had oral sex and only tests urine, a throat infection could be missed.
Testing early doesn’t just protect you. It protects your joints, your bloodstream, and your long-term health. If you’ve had a recent exposure or unexplained symptoms, a discreet option like a Gonorrhea Test Kit can provide initial answers quickly. For broader screening, a combo kit can check for multiple infections at once.
This isn’t about assuming the worst. It’s about removing uncertainty before it escalates.
What Treatment for DGI Actually Involves
Here’s the reassuring truth: even when disseminated gonococcal infection occurs, it is treatable. Modern antibiotic regimens are effective when administered promptly.
According to CDC guidelines, DGI typically requires intravenous (IV) antibiotics at first, often ceftriaxone, followed by oral antibiotics once improvement is documented. Hospitalization may be necessary, especially if septic arthritis is suspected.
If a joint is severely inflamed, doctors may drain fluid from it. This isn’t punishment. It’s infection control. Removing infected fluid helps antibiotics work more effectively and prevents joint damage.
Most patients respond quickly to treatment when it’s started early. Fever subsides. Swelling decreases. Rash resolves. The body calms down.
But delays increase risk. Untreated septic arthritis can permanently damage cartilage. Severe systemic infection can strain organs. That’s why early action matters more than embarrassment ever should.
Can You Fully Recover From DGI?
In the majority of cases, yes. When treated appropriately and promptly, people recover without long-term complications.
The biggest risk factor for lasting damage is delayed treatment. If someone waits weeks while joint inflammation worsens, cartilage can erode. If systemic infection progresses unchecked, the illness becomes more dangerous.
But caught early? Prognosis is strong.
“Arjun,” the patient who initially thought he had the flu, said afterward: “I felt stupid for not connecting it sooner. But once they started treatment, I improved within days.”
This isn’t a moral story. It’s a medical one. Bacteria move when untreated. Antibiotics stop them.
The Emotional Spiral: When Google Makes It Worse
If you’re reading this after typing “bloodstream infection STD” at 1:17 a.m., take a breath.
DGI is uncommon. Most gonorrhea infections remain localized and are treated before they ever spread. Even when dissemination happens, modern medicine handles it effectively when addressed quickly.
The danger isn’t that gonorrhea always becomes life-threatening. The danger is ignoring symptoms because they don’t look like the version you expected.
If you have fever plus joint swelling, seek care. If you’ve had a recent exposure and haven’t tested, test. If you feel fine but had risk, screen anyway. Silence is not safety.
You deserve clarity, not catastrophic thinking.
How to Prevent Gonorrhea From Reaching This Point
Disseminated gonococcal infection sounds dramatic because it is, but it is also preventable. The overwhelming majority of bloodstream cases begin as untreated, localized gonorrhea. That means early detection changes everything.
Routine screening is recommended for sexually active individuals with new or multiple partners, and especially for men who have sex with men, according to the CDC screening recommendations. Testing is not a confession. It is maintenance.
Barrier protection reduces transmission risk. Open communication with partners lowers delayed diagnosis. And prompt treatment stops bacterial spread before it ever leaves its original site.
If you’ve had a recent exposure, or if something in your body feels off, discreet screening options are available through STD Test Kits. A Combo STD Home Test Kit can screen for multiple infections at once, helping you catch issues early and avoid complications like DGI.
You do not have to wait for symptoms to justify testing. In fact, waiting is often how complications begin.
FAQs
1. Wait, can gonorrhea actually get into your bloodstream, or is that just Google being dramatic?
It’s real, but rare. Most gonorrhea infections stay localized and are treated before anything spreads. Disseminated gonococcal infection (DGI) happens when the bacteria move beyond the original site and trigger inflammation in joints and skin. It’s not common, but it’s medically documented and very treatable when caught early.
2. If I don’t have discharge, does that mean I’m safe from complications?
Not necessarily. A lot of people, especially with throat or cervical infections, have zero obvious symptoms. That’s the tricky part. DGI sometimes shows up in people who never noticed classic genital warning signs. No discharge doesn’t equal no infection.
3. What does the DGI rash actually look like?
It’s usually small red or purplish spots, sometimes with tiny blisters or a slightly raised center. People often notice them on their palms, soles, or around inflamed joints. It doesn’t usually itch like an allergic reaction. It looks… medical. Subtle but strange.
4. My knee is swollen and I had sex last month. Am I overthinking this?
Joint pain alone doesn’t automatically mean bloodstream infection. Bodies get sore for a hundred reasons. But if that swelling is paired with fever, fatigue, or a new rash, that’s when it’s worth connecting the dots and getting evaluated. Overthinking is spiraling without data. Testing is getting data.
5. How fast would something like this happen?
There’s no stopwatch. Gonorrhea symptoms can appear within two weeks of exposure, and bloodstream spread can follow days to weeks later if untreated. Some people feel fine until the joint inflammation hits. That unpredictability is exactly why routine screening matters.
6. Can gonorrhea turn into sepsis?
In rare cases, yes. But this is the important part: modern antibiotics are extremely effective. Severe outcomes usually involve delayed care. When treated promptly, DGI resolves in the vast majority of cases without long-term damage.
7. If I test positive for gonorrhea, does that mean it’s already spreading?
No. Most positive tests reflect localized infection only. Treating it quickly almost always prevents any systemic complications. A positive result is information, and information is power.
8. What’s worse, ignoring mild symptoms or panicking over every ache?
Ignoring persistent symptoms is riskier. Panicking, while uncomfortable, usually leads to action. The goal isn’t fear. It’s clarity. If something feels off and you’ve had exposure, testing replaces anxiety with answers.
9. Do I need to tell my partner if this happens?
Yes. Not because you did something wrong, but because infections don’t resolve on loyalty. Partner testing prevents reinfection and protects everyone’s health. Most people appreciate honesty more than silence.
10. Is this something people recover from fully?
Yes, especially when treated early. Fever resolves. Joints calm down. The rash fades. The body heals. The scariest part of DGI is usually the unknown. Once there’s a diagnosis and a plan, things move forward quickly.
If You’re Scared Right Now, Read This Slowly
Most people who search “can gonorrhea spread to blood” are not actually in septic shock. They are anxious. They are replaying a recent hookup in their head. They are touching a sore wrist and wondering if they missed something.
DGI is rare. When it happens, it is treatable. When caught early, recovery is strong. The goal of this article is not to alarm you, it is to inform you so you can act appropriately instead of spiraling.
If you have mild joint discomfort without fever, that alone does not confirm a bloodstream infection. If you have high fever, severe swelling, or feel acutely ill, seek urgent medical care. And if you simply haven’t tested after a risk, that’s your next logical step.
Knowledge turns panic into a plan.
How We Sourced This Article: This guide integrates CDC treatment guidelines, WHO global surveillance data, Mayo Clinic clinical explanations, and peer-reviewed infectious disease literature on disseminated gonococcal infection. We reviewed approximately fifteen medical and public health references to ensure accuracy. The six sources listed below were selected for clarity, authority, and accessibility for readers who want to verify the information independently.
Sources
1. CDC Sexually Transmitted Infections Treatment Guidelines
2. NHS: Reactive Arthritis Overview
3. Mayo Clinic: Reactive Arthritis Symptoms and Causes
4. CDC: Health Alert Template for Disseminated Gonococcal Infection (DGI)
5. Mayo Clinic: Reactive arthritis — Symptoms and causes
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He combines clinical precision with a sex-positive, stigma-free approach to help readers make informed decisions about their health.
Reviewed by: L. Ramirez, PA-C | Last medically reviewed: March 2026
This article is for informational purposes and does not replace medical advice.







