Do Men and Women Need Different STD Tests? What Actually Changes (And What Doesn’t)
Quick Answer: A full panel STD test is best if you had unprotected sex, multiple partners, or don’t know your partner’s status. A single STD test makes sense when you have a specific exposure or symptom linked to one infection. Timing and risk level matter more than panic.
The Moment You Start Googling: What Are You Actually Afraid Of?
When someone asks whether they need a full panel STD test or just one, they’re rarely asking about lab science. They’re asking whether they messed up. They’re asking whether one night could change everything. They’re asking whether a small symptom means something bigger.
Rashida, 27, told me, “I didn’t even feel sick. I just kept thinking, what if I’m missing something?” That’s the psychology behind full-panel testing. It isn’t always about symptoms. It’s about peace of mind.
On the other hand, Daniel, 34, noticed burning during urination five days after sex and thought, “This has to be chlamydia or gonorrhea. Why would I test for HIV?” That instinct isn’t wrong either. Sometimes a targeted STD test is logical and efficient.
The difference comes down to risk exposure, symptom pattern, and timing. Not fear. Not guilt. Not worst-case scenarios from a forum thread at 2 a.m.
People are also reading: Why Does It Burn After Sex? Friction vs Infection Explained
What a Full STD Panel Actually Includes (And Why That Matters)
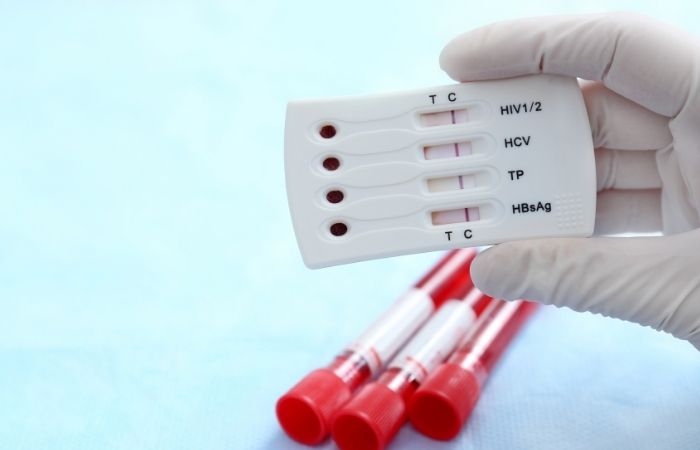
A full STD panel is not a single test. It’s a bundle. Most comprehensive panels screen for Chlamydia, Gonorrhea, Syphilis, and HIV. Some expanded panels also include Trichomoniasis, Hepatitis B, and Hepatitis C. Fewer include Herpes unless specifically requested, because herpes testing has nuance and is not routinely recommended for everyone without symptoms.
According to the CDC’s screening recommendations, routine screening for chlamydia and gonorrhea is advised for sexually active women under 25 and for others based on risk factors. HIV screening is recommended at least once for most adults, and more often for higher-risk groups. That means full-panel testing is often preventive, not reactive.
When you order a discreet at-home STD test kit, a combo kit essentially mirrors what many clinics call “routine screening.” It’s about coverage. You’re testing for common infections that frequently show no symptoms at all.
If you had unprotected vaginal or anal sex and don’t know your partner’s status, this level of coverage is usually appropriate. Not because you’re “high risk,” but because common infections are common.
When a Single STD Test Is Enough
There are situations where targeted STD testing makes perfect sense. If you had oral sex only and developed a sore throat, you might consider throat testing for gonorrhea specifically. If you have discharge and burning within a week of exposure, chlamydia and gonorrhea testing may be the priority.
Targeted testing is most appropriate when the exposure type clearly aligns with one infection and your risk profile is otherwise low. For example, if you are in a long-term monogamous relationship and both partners previously tested negative, a single test after a specific concern may be reasonable.
But here’s the nuance: symptoms are unreliable. Many infections produce mild or no symptoms. Choosing just one STD test based solely on what you feel can create false reassurance.
The key word is appropriate. Not cheaper. Not faster. Appropriate. Choosing the right STD test is about matching the biology to the behavior.
Cost, Privacy, and the Real-Life Decision
Some people choose a single STD test because of cost. That’s understandable. A full panel costs more upfront than one test. But paying twice because you discover later that you should have tested broadly can cost more emotionally and financially.
At-home combo STD test kits bundle common infections at a lower combined price than buying each separately. They also eliminate clinic copays, time off work, and the stress of sitting in a waiting room wondering who might recognize you.
If privacy is your top concern, discreet shipping and confidential results can make a full panel feel safer than staggered clinic visits. Many people prefer ordering a combo STD home test kit once rather than scheduling multiple appointments.
This is not about encouraging overspending. It’s about understanding the tradeoff between coverage and uncertainty. Sometimes paying for clarity is worth more than saving $40 and staying anxious.
The Window Period Problem No One Talks About
Testing too early can make any choice, full panel or single test, unreliable. Each infection has a window period between exposure and detectability. For example, chlamydia and gonorrhea can often be detected within 7 to 14 days. HIV antigen/antibody tests are most reliable around 18 to 45 days after exposure. Syphilis may take several weeks before antibodies are detectable.
So if you test three days after sex, a full panel does not magically override biology. It may simply give you false reassurance. Sometimes the smartest strategy is staged testing: an initial targeted test for early bacterial infections, followed by repeat screening for HIV or syphilis at the recommended window.
This is where panic makes people overshoot. They order everything immediately, test too early, and still feel uncertain. Timing matters more than volume.
If You Have No Symptoms, Here’s the Honest Answer
Most sexually transmitted infections do not announce themselves dramatically. No fireworks. No dramatic rash. No cinematic fever. In fact, Chlamydia and Gonorrhea are asymptomatic in a significant percentage of cases, especially in women. HIV can remain symptom-free for years.
That’s why “I feel fine” is not a reliable screening tool. When someone searches “STD test without symptoms,” they’re usually wrestling with invisible risk. If you had unprotected sex with a new or casual partner, a full panel STD test is generally the smarter move because you cannot symptom-check your way to certainty.
Leila, 29, told me, “I almost didn’t test because nothing felt wrong. I only did the full panel because I kept thinking about it.” Her result came back positive for chlamydia. No discharge. No pain. Just bacteria doing what bacteria do when unnoticed.
Silence isn’t safety. It’s just silence.
One New Partner: Does That Automatically Mean Full Panel?
Not automatically. But often, yes.
Here’s why: when you enter a new sexual relationship, you don’t just inherit a person. You inherit their testing history, their previous partners’ histories, and whatever gaps may exist in that chain. Even if someone says, “I was tested,” it matters what they were tested for. Many people assume a standard visit includes a full STD panel when it may have only included chlamydia and gonorrhea.
If both partners test comprehensively before becoming exclusive, that conversation becomes grounded in data instead of assumptions. A single STD test may miss infections that were never screened in the first place.
This isn’t about distrust. It’s about starting something new with clarity instead of crossed fingers.
After Oral Sex, Do You Need Everything?
This is where targeted testing can make sense. Oral sex carries lower risk for HIV transmission but can transmit Gonorrhea, Chlamydia, Syphilis, and Herpes. The site of exposure matters. Throat infections often require a throat swab rather than urine testing.
If oral sex was your only exposure and you have no genital symptoms, a full 10-panel STD test may not be necessary. But if oral sex was part of broader unprotected contact, or if you’re unsure of your partner’s status, broader screening becomes reasonable.
It comes back to context. A single act rarely exists in isolation. Most exposures are layered.

People are also reading: HPV and Throat Cancer: What a BBC Story Reveals About Early Warning Signs
The Anxiety Trap: When “Testing for Everything” Feels Safer
There’s a psychological pattern I see often. Someone has a low-risk encounter. They go online. They read worst-case stories. Suddenly, a single targeted STD test feels reckless, and only a full panel seems responsible.
But more testing doesn’t always equal better testing. If you test too early for infections with longer window periods, you may still need retesting. If you add low-probability tests without indication, you may create confusion from ambiguous results.
That said, sometimes ordering a full panel is not about probability. It’s about closure. And closure has value. If your anxiety is dominating your sleep, your work, your relationships, paying for clarity may be justified.
Testing should reduce anxiety. If your strategy increases it, it needs adjusting.
Cost Comparison: Single vs Full Panel
Let’s talk numbers without drama. Buying individual tests separately often costs more per infection than bundled combo kits. Clinics may bill per test. Insurance coverage varies. Copays, lab fees, and repeat visits add up.
At-home combo kits reduce those variables. You order once. You test once. You get comprehensive results at once. For many people, that simplicity outweighs the slightly higher upfront cost compared to one targeted test.
If your budget is tight and risk is clearly isolated, a single STD test may be rational. But if your exposure involved multiple types of contact, full screening may be more cost-effective in the long run.
Routine Screening vs Exposure Testing
Routine screening is preventive. It’s not about a mistake. It’s about maintenance. If you’re sexually active with more than one partner, or you’re dating casually, regular full-panel screening once or twice per year can be part of normal healthcare.
Exposure testing is reactive. Something specific happened. A condom broke. A partner disclosed something. Symptoms appeared. In those cases, your testing strategy should align with what actually occurred.
Many people confuse these two categories. They test reactively but choose preventive-level coverage, or vice versa. The right choice depends on whether you’re responding to an event or maintaining sexual health long-term.
So How Do You Actually Decide?
Ask yourself four grounded questions instead of spiraling:
First: Was the encounter protected or unprotected, and what types of contact occurred? Vaginal, anal, oral, or multiple?
Second: Do I know my partner’s recent test results, and do I trust that information?
Third: Do I have symptoms that strongly point toward one infection?
Fourth: When did the exposure occur relative to window periods?
If answers feel uncertain or layered, full panel testing often brings clarity faster. If risk is clearly narrow and timing is appropriate, a single targeted STD test may be enough.
The goal is not to test the most. The goal is to test intelligently.
What If You Already Tested for One STD?
This is where things get complicated fast. Maybe you ordered a single Chlamydia test because you had mild discharge. It came back negative. Now you’re wondering if that’s enough or if you should have done a full panel STD test from the beginning.
Here’s the honest answer: a negative single test only rules out that specific infection, at that specific time, assuming the window period has passed. It does not rule out Gonorrhea, Syphilis, HIV, or anything else unless they were tested too.
Omar, 31, told me, “I tested for chlamydia and felt relieved. Then I realized I never checked for HIV.” That second wave of anxiety is common. It’s not irrational. It’s just incomplete coverage catching up with you.
If you’ve already tested for one infection but your exposure was broader, adding a panel afterward isn’t overreacting. It’s finishing the job.
The Myth of the “10-Panel Overkill”
You may have seen people online say that 10-panel STD tests are excessive. In some situations, they are. If your only risk was protected sex in a long-term monogamous relationship, broad testing may be unnecessary.
But labeling full screening as “overkill” ignores something important: most common STDs are silent. Chlamydia and Trichomoniasis frequently cause no symptoms. Early Syphilis can be painless. HIV may feel like nothing at all in early stages.
A full panel is not dramatic. It’s comprehensive. The question is whether your risk profile justifies comprehensiveness. For many sexually active adults, especially with new or multiple partners, it does.
Testing isn’t about punishment. It’s about information.
People are also reading: Herpes Flare Cycles in Women vs Men
Decision Map: Matching Exposure to Testing Strategy
Instead of guessing, let’s align common real-life scenarios with logical testing choices. Not emotionally driven. Not shame-driven. Just aligned with biology and public health guidance.
This isn’t a rigid rulebook. It’s a framework. You still need to consider timing, which we’ll get to next.
Timing Can Change Your Answer
If you’re testing three days after exposure, almost any strategy is premature. A full panel won’t override window periods. A single STD test won’t either. You may need staged testing.
For example, bacterial infections like Chlamydia and Gonorrhea are often detectable within 7 to 14 days. HIV antigen/antibody tests typically become reliable within 18 to 45 days. Syphilis may take several weeks before antibodies appear.
Testing too early is one of the biggest reasons people retest. It’s not that the first test was wrong. It’s that biology hadn’t caught up yet.
If you’re unsure about timing, sometimes ordering a combo test kit now and planning a follow-up at the correct window gives you both early insight and long-term certainty.
What Clinics Don’t Always Explain
Many people assume that when they ask for “an STD test,” they automatically receive full screening. That isn’t always true. Some clinics test only for chlamydia and gonorrhea unless you specifically request additional screening.
That misunderstanding creates confusion later. Someone thinks they had a “full panel” last year, but it didn’t include HIV or Syphilis. Then a new partner conversation reveals the gap.
Being explicit about what you want tested is not awkward. It’s responsible. Whether you’re in a clinic or ordering from STD Test Kits, clarity about what’s included prevents assumptions from doing the decision-making for you.
Emotional Honesty: Are You Testing for Risk or for Relief?
There’s no shame in wanting relief. Sometimes the exposure was low risk, but your mind won’t let it go. You replay the moment. You reread old texts. You inspect your body for phantom symptoms.
In those moments, a full panel STD test may serve a psychological purpose as much as a medical one. That doesn’t make it frivolous. Mental peace is real health.
But if you’re ordering every possible test repeatedly after low-risk encounters, that may signal anxiety that needs addressing beyond testing. Testing should resolve fear, not feed it.
When in Doubt, Broader Testing Is Usually Safer Than Narrow
If you truly can’t decide between a full panel STD test and a single test, and your exposure was unprotected or uncertain, broader testing is generally the safer path. Missing an infection because you narrowed your scope too much creates more stress than covering your bases once.
A discreet combo STD home test kit allows you to check the most common infections at once, in private, without multiple appointments. For many people, that simplicity is worth it.
The goal isn’t to test aggressively. It’s to test strategically and then move forward.
FAQs
1. Do I really need a full panel STD test after just one hookup?
It depends on what happened during that hookup. If it involved unprotected vaginal or anal sex and you don’t know your partner’s testing status, a full panel is usually the cleanest way to close the mental tab. Even one encounter can transmit common infections like Chlamydia or Gonorrhea, and those often come without symptoms. If protection was used correctly and there were no risk factors, you might not need the full sweep, but clarity beats guessing.
2. What if I feel completely fine, no symptoms at all?
That’s exactly why screening exists. Many STDs are asymptomatic, especially early on. Feeling normal doesn’t mean nothing happened; it just means your body isn’t waving a flag yet. If your exposure involved real risk, testing is about confirmation, not symptom management.
3. Can I just test for chlamydia and call it a day?
You can, and sometimes that’s reasonable, especially if symptoms point strongly in that direction. But here’s the catch: infections travel in groups more often than people realize. Chlamydia and gonorrhea frequently overlap. So if your exposure wasn’t narrow, testing for just one might leave you with half the answer.
4. Is a 10-panel STD test overkill?
For someone in a long-term, mutually tested monogamous relationship? Probably. For someone dating casually, unsure about partner history, or starting something new without prior testing? Not necessarily. “Overkill” depends on context. Broad testing isn’t dramatic, it’s just comprehensive.
5. I already tested for one STD and it was negative. Am I in the clear?
You’re in the clear for that one infection at that specific moment, assuming you tested after the correct window period. Think of it like checking one room in a house. It doesn’t automatically mean the entire house is empty. If other infections weren’t included, they simply weren’t assessed.
6. How soon after sex can I test?
This is where patience matters. Bacterial infections like chlamydia and gonorrhea are often detectable after about 7 to 14 days. HIV tests may require several weeks for reliable detection. Testing too early isn’t “wrong,” but it may mean you’ll need to retest for full certainty. Timing is everything.
7. What if I can’t afford a full panel right now?
Then prioritize strategically. If you have symptoms like discharge or burning, focus first on common bacterial infections. Plan follow-up testing when you can. Imperfect action is still better than no action, and thoughtful sequencing is smarter than avoidance.
8. Should couples get full panels before becoming exclusive?
Many do, and not because they distrust each other. It’s about starting fresh with shared data instead of assumptions. A mutual full panel creates a clean baseline and removes the awkward “I thought you tested for that” conversation later.
9. Are at-home combo STD tests actually reliable?
When used correctly and taken at the right time after exposure, yes. They’re designed to detect the same common infections clinics screen for. The key is following instructions carefully and understanding window periods. If a result is positive, confirmatory care is the next step, not panic.
10. How do I decide if I’m testing for risk or just anxiety?
Be honest with yourself. If the exposure involved real biological risk, testing is practical. If the encounter was low risk but you can’t sleep, broader testing may still serve your peace of mind. The goal isn’t to win a risk contest. It’s to quiet the noise in your head with actual information.
Before You Spiral, Let’s Ground This
You do not need to punish yourself with the biggest test panel available just because you feel embarrassed. You also don’t need to minimize your risk because you want to believe everything is fine. The smartest choice lives between those two extremes.
If your exposure was unprotected, involved multiple types of sex, or your partner’s testing history is unclear, a full panel STD test is usually the most efficient way to close the loop. If your risk was clearly isolated and symptoms point strongly toward one infection, a single targeted STD test may be completely appropriate.
Testing is not about morality. It’s maintenance. It’s information. It’s how adults take care of themselves and the people they sleep with.
How We Sourced This Article: This guide was built using current CDC screening recommendations, peer-reviewed research on STD prevalence and asymptomatic infection rates, and clinical best practices around window periods and testing strategies. We reviewed approximately fifteen authoritative and peer-reviewed sources to ensure accuracy. For clarity and reader focus, we have listed six of the most relevant and accessible references below. All links were verified and open in a new tab so you can confirm information independently.
Sources
1. CDC Sexually Transmitted Infection Screening Recommendations
2. NHS: Sexually Transmitted Infections Overview
3. Which STI tests should I get? | CDC
4. Getting Tested for STIs | CDC
5. STI Screening Recommendations | CDC
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He combines clinical precision with a candid, stigma-free approach to sexual health education.
Reviewed by: Jordan Alvarez, PA-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.







