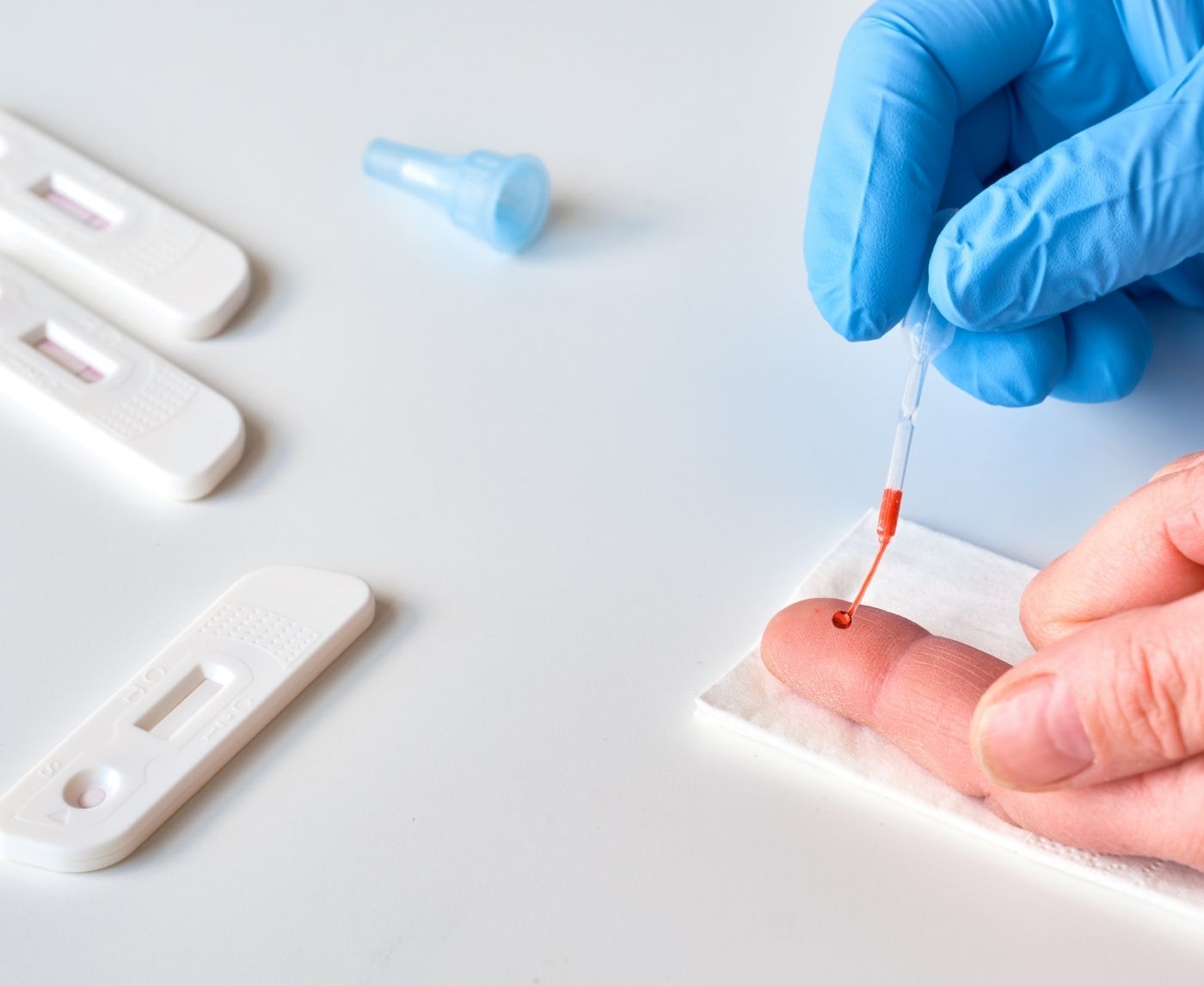
Swab vs Blood vs Urine STD Tests: What’s the Real Difference?
Quick Answer: Men and women usually test for the same STDs, but the type of sample and routine screening recommendations differ based on anatomy and risk factors. What changes is how the test is collected and when screening is recommended, not which infections matter.
The Big Misunderstanding: It’s Anatomy, Not Gender
When people ask whether STD testing for men vs women is different, they’re usually picturing two completely separate medical universes. That’s not what’s happening. The infections, Chlamydia, Gonorrhea, Syphilis, HIV, Herpes, Trichomoniasis, are the same organisms affecting different tissues.
What changes is where those organisms live. A cervix is different from a urethra. A rectum is different from a vagina. A throat exposed during oral sex doesn’t care whether you’re a man or a woman. Testing follows exposure and body parts, not identity labels.
That’s why someone assigned male at birth who engages in receptive anal sex may need rectal swabs. Someone with a cervix may need cervical screening. Someone who has oral sex may need throat testing. The biology of exposure is what drives the test plan.

People are also reading: Can I Test for STDs While on PrEP? What Changes
What’s Actually the Same for Everyone
Let’s strip this down. Most core STD panels screen for the same major infections across all sexes. If you walk into a clinic or order an at-home panel from STD Test Kits, the infections screened are not “male” or “female” versions. They are universal pathogens.
Table 1. Core STD tests are largely identical across sexes; the sample site may vary based on anatomy and exposure.
The organism doesn’t check your driver’s license. It attaches to mucosal tissue. That’s it. So when people ask, “Are STD tests different for males and females?” the honest answer is: not in terms of what infections we’re screening for.
The differences start showing up in screening guidelines and how samples are collected.
Why Women Are Screened More Routinely
This is where confusion starts. Many women are offered STD testing during annual exams, birth control visits, or pregnancy. That can make it look like women “need more tests.” But public health recommendations drive this pattern.
The CDC recommends routine Chlamydia and Gonorrhea screening for sexually active women under 25 because untreated infections can silently lead to pelvic inflammatory disease and infertility. These infections are frequently asymptomatic in women. That asymptomatic risk drives proactive screening.
Men, on the other hand, are less likely to experience severe long-term reproductive complications from untreated Chlamydia, so routine screening isn’t recommended at the same frequency for low-risk heterosexual men. That’s a public health decision, not a statement that men “don’t need testing.”
It’s not about fairness. It’s about statistical risk of complications.
The HPV Question: Why This Feels Unequal
“Can men get tested for HPV?” is one of the most searched questions in sexual health. And this is where things truly diverge.
Women with a cervix receive Pap smears and HPV testing because persistent high-risk HPV strains can cause cervical cancer. There is a clear screening method and defined guidelines. That’s why HPV testing is routine in gynecologic care.
There is no equivalent routine HPV screening test for men without symptoms. There’s no approved general screening swab for asymptomatic cisgender men. HPV in men is usually identified only if genital warts appear or if anal screening is performed in high-risk groups.
This difference isn’t because HPV spares men. It’s because medicine currently lacks a standardized screening tool for asymptomatic men the way it has for cervical screening. That’s a limitation of available testing methods, not biology playing favorites.
Vaccination helps close this gap, for everyone.
Urine, Swab, Blood: What Actually Changes Between Men and Women
When someone says “STD testing is different for men and women,” they’re usually picturing completely separate lab panels. That’s not what’s happening. What changes most often is how the sample is collected.
For many infections like Chlamydia and Gonorrhea, nucleic acid amplification testing (NAAT) is the gold standard. The science is identical across sexes. The difference is whether the sample comes from urine, a vaginal swab, a cervical swab, a urethral swab, or another exposed site.
A person with a penis often provides a first-catch urine sample. A person with a vagina may use a vaginal swab, sometimes self-collected. Both are highly accurate when performed at the right time after exposure. The organism doesn’t behave differently, the collection method adapts to anatomy.
Table 2. Sample type depends on anatomy and exposure site, not identity label.
If you’ve had oral sex, your throat may need testing. If you’ve had receptive anal sex, rectal screening matters. If you have a cervix, cervical health becomes part of the equation. The real question is not “Are you male or female?” It’s “Where was the exposure?”
Exposure Drives Testing More Than Gender Ever Will
Let’s say Daniel has only had insertive vaginal sex. His risk profile looks different from Alina, who has vaginal and oral exposure. Now imagine Malik, who has receptive anal sex with male partners. His testing needs may include rectal and throat swabs in addition to urine. None of this is about identity politics. It’s about contact surfaces.
This is why sexual health experts now talk about anatomy-based testing. A trans man with a cervix may still need cervical screening. A cisgender woman who engages in anal sex may need rectal testing. A bisexual man who performs oral sex may need throat screening.
When people search “Do I need a different STD test if I’m gay?” what they’re really asking is whether their behavior changes the panel. The answer is yes, behavior can expand testing sites. But the infections being screened are the same ones affecting everyone else.
Why Men Often Under-Test (And Women Over-Internalize Risk)
There’s a cultural layer here. Many men grow up without routine reproductive healthcare visits. There’s no annual Pap smear equivalent. No default screening appointment. That can create the illusion that men don’t need testing as often.
Meanwhile, many women receive regular gynecologic care and are screened more routinely. That proactive system is designed to prevent silent reproductive damage. But it can also create anxiety, the feeling that women are uniquely vulnerable.
The truth sits in the middle. Men absolutely can carry asymptomatic Chlamydia or Gonorrhea. Women absolutely deserve screening that protects long-term health. Neither group is immune. Neither group is biologically reckless. Public health policies simply prioritize complication prevention where risk data shows the highest downstream harm.
What About Blood Tests? Are Those Different?
Blood-based STD tests, like those for Syphilis, HIV, and sometimes Herpes antibodies, are essentially identical across sexes. A fingerstick rapid test or lab blood draw doesn’t change because of gender.
The timing matters more than the body. Testing too early in the window period can yield false reassurance. That rule applies universally. Whether you’re male, female, nonbinary, or somewhere in between, antibody development follows the same biological timeline.
If you’re choosing an at-home option, a discreet multi-panel like the 6‑in‑1 At‑Home STD Test Kit checks for the most common infections regardless of sex. The difference isn’t the panel, it’s making sure you choose the right sample type for your anatomy and exposure.
People are also reading: Which STD Test Do I Need Based on My Symptoms?
When Testing Is Truly Different
There are a few moments when the path does diverge clearly.
Pregnancy changes screening recommendations. Cervical cancer prevention requires Pap and HPV testing for people with a cervix. Prostate health does not involve STD screening but sometimes gets confused in online searches. These differences are anatomy-driven and evidence-based.
Outside of those specific scenarios, the majority of STD testing overlaps. If someone tells you men and women need completely different STD panels, they’re oversimplifying the science.
The Tests Men Commonly Miss
Here’s something that doesn’t get said enough: a lot of men think a urine test covers everything. It doesn’t. If you’ve only ever peed in a cup, there’s a chance parts of your body were never actually screened.
Rectal and throat infections are frequently missed when testing only includes urine. Gonorrhea and Chlamydia can live quietly in the throat or rectum without obvious symptoms. A man can test negative in urine and still carry infection at another exposed site.
Javier, 28, once told his clinician, “But I tested negative last month.” After a few questions, it became clear he had only done urine testing. No one had asked about oral or receptive anal sex. His rectal swab later came back positive. He wasn’t reckless. He just wasn’t asked the right follow-up questions.
This is where behavior-based testing matters more than gender categories. If exposure included oral or anal contact, site-specific swabs matter. It’s not extra. It’s accurate.
The Tests Women Sometimes Assume They’re Getting
On the flip side, many women assume a routine gynecologic visit automatically includes full STD screening. That’s not always true. A Pap smear screens for cervical cell changes and sometimes HPV, not necessarily for Chlamydia, Gonorrhea, HIV, or Syphilis.
Alyona, 24, thought she was “fully tested” because she had a Pap at her annual visit. Months later, she learned no bloodwork had been ordered. Her provider had performed cervical cancer screening, not a full STD panel. The misunderstanding is common and understandable.
Asking specifically for STD testing clarifies expectations. Pap tests and STD panels overlap in appointments, but they are not interchangeable.
Timing Doesn’t Care About Gender
Another place confusion creeps in is timing. People often wonder whether window periods differ between men and women. They don’t. The bacteria and viruses follow biological timelines that are consistent across bodies.
Chlamydia and Gonorrhea are typically detectable about 7–14 days after exposure. HIV antigen/antibody tests often become reliable within 2–6 weeks. Syphilis antibodies may take several weeks to appear. These windows are driven by microbial replication and immune response, not by gender identity.
The difference is not when to test. It’s what sample to test and from where.
Building a Personal Testing Plan Without Shame
Instead of asking whether men and women need different STD tests, try reframing the question: “Based on my anatomy and exposure, what do I need screened?” That question is more accurate, and more empowering.
Start with exposure type. Vaginal sex? Urine or vaginal swab testing for Chlamydia and Gonorrhea. Oral sex? Consider throat testing. Receptive anal sex? Add rectal screening. Multiple partners or new partner? Add blood testing for HIV and Syphilis.
Then factor in timing. If exposure was recent, waiting until the optimal detection window improves accuracy. Testing too early can create false reassurance. Testing too late prolongs anxiety. There’s a balance, and it’s the same balance for everyone.
At-Home Testing: Where Equality Is Clear
At-home testing has helped flatten some of these gender-based misunderstandings. When you browse options on STD Test Kits, you’ll notice the panels are built around infections, not gender labels.
The difference lies in choosing the right collection method. A person with a vagina may select a swab-based kit. A person with a penis may select urine-based testing. A multi-panel option like the 7-in-1 Complete At-Home STD Test Kit allows screening for multiple infections at once, regardless of sex.
The science underneath is the same. The autonomy feels different, because you’re guiding the process based on your real exposure history.
So What Actually Changes, and What Doesn’t?
What changes: routine screening guidelines for people with a cervix, HPV testing availability, and sample collection methods. What doesn’t change: the organisms, the window periods, the need for blood-based screening in certain scenarios, and the importance of testing after risk.
When people ask why women are tested more for STDs, the answer isn’t that women are more infectious. It’s that untreated reproductive complications can carry higher long-term risk. When people ask why men aren’t routinely screened the same way, the answer lies in complication rates and healthcare structure, not biological immunity.
Most of the anxiety dissolves when we center anatomy and exposure instead of stereotypes.
FAQs
1. So… do men and women actually need different STD tests?
Not in the dramatic way the internet makes it sound. The infections are the same, Chlamydia, Gonorrhea, HIV, Syphilis, Herpes. What changes is the collection method and sometimes how often screening is recommended. Think “different doorways,” not different diseases.
2. If I’m a guy and I feel totally fine, do I really need testing?
Possibly, yes. Many men carry infections without symptoms, especially Chlamydia and Gonorrhea. I’ve had patients say, “But nothing burns.” That’s not a guarantee. Silence is not proof of safety; it’s just absence of obvious irritation.
3. I had my annual exam and a Pap smear. Doesn’t that mean I was tested for everything?
Not necessarily. A Pap checks cervical cells for abnormal changes and may include HPV testing. It does not automatically test for HIV, Syphilis, or other common STDs unless those labs were specifically ordered. Always ask what was included, assumptions are how infections slip through.
4. Why does it feel like women get tested more often?
Because screening guidelines prioritize protecting the cervix and preventing infertility. Untreated Chlamydia in women can quietly damage reproductive organs. Public health focuses where long-term harm is statistically higher. That’s policy, not morality.
5. Can men get tested for HPV like women can?
This is the frustrating one. There isn’t a routine screening test for asymptomatic men the way there is for people with a cervix. That doesn’t mean HPV spares men. It means medicine hasn’t built a standardized screening pathway yet. Vaccination remains one of the strongest protective tools for everyone.
6. If I only gave oral sex, do I need a different test?
You may need a throat swab. Oral exposure can transmit Gonorrhea and sometimes Chlamydia. A urine test alone won’t catch that. This is where testing by body part, not gender, becomes critical.
7. I’m in a same-sex relationship. Does that change my testing plan?
It changes the exposure pattern, not the pathogens. Two women can transmit infections. Two men can transmit infections. Testing should follow anatomy and contact points. Identity labels don’t dictate microbes, behavior does.
8. Are at-home STD tests just as reliable for men and women?
When used correctly and at the right time after exposure, yes. The key variables are timing and proper sample collection. The bacteria and viruses behave the same regardless of who’s holding the test cassette.
9. Do window periods differ between men and women?
No. The immune system does not check gender markers in a person and produce antibodies accordingly. The period of detection varies depending on the organism and test type, and not gender.
10. What’s the biggest mistake people make with STD testing?
Assuming one test covers every exposure. Someone tests urine-only and forgets about the throat. Someone assumes a Pap covered HIV. Someone tests five days after exposure and trusts a negative result too quickly. Testing isn’t complicated, but it does require asking, “Where was I exposed, and when?”
You Deserve Clarity, Not Confusion
The question “Do men and women need different STD tests?” sounds simple, but it hides layers of misunderstanding. Most infections don’t discriminate. What changes is anatomy, exposure site, and public health screening priorities. What doesn’t change is the importance of testing when risk exists.
If you’ve had a new partner, symptoms that won’t settle, or simply want peace of mind, you don’t need to overthink the label. You need the right test for your body and your exposure. This at-home combo test kit screens for the most common STDs discreetly and quickly, so you can stop spiraling and start knowing.
Your results. Your privacy. Your control.
How We Sourced This Article: We reviewed current screening guidance from the CDC, USPSTF, and WHO, along with peer-reviewed studies on NAAT testing accuracy and HPV screening limitations. Lifestyle and lived-experience reporting were also consulted to ensure this guide reflects how real people search for and experience testing decisions. While more than a dozen references informed this article, we’ve listed six key authoritative sources below for clarity and verification.
Sources
1. CDC – STD Screening Recommendations
2. USPSTF – Chlamydia and Gonorrhea Screening
3. STI Screening Recommendations | CDC
4. Men Who Have Sex with Men (MSM) - STI Treatment Guidelines | CDC
5. Recommendation: Chlamydia and Gonorrhea: Screening | U.S. Preventive Services Task Force
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He combines a no-nonsense, sex-positive approach with clinical accuracy and is dedicated to making testing more widely available in a private, evidence-based way.
Reviewed by: Lauren Mitchell, MPH | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.