STD Symptoms in Women That Don’t Involve the Vagina
Quick Answer: The STD test you need depends on your symptoms, exposure type, and timing. Burning urination often points to Chlamydia or Gonorrhea testing, sores suggest Herpes or Syphilis, and no symptoms after a risky encounter may call for a targeted panel based on window periods.
This Isn’t Random, Your Symptoms Are Clues
When people search “which STD test do I need,” what they’re really asking is: what does this mean? A sensation. A bump. A discharge that wasn’t there before. A sore throat after oral sex. Your body doesn’t send random notifications. But it also doesn’t label them clearly.
Chlamydia and Gonorrhea are notorious for causing burning with urination and unusual discharge, yet they are equally notorious for causing no symptoms at all. According to the CDC, a large percentage of infections are asymptomatic, especially in women and people with cervixes, which means waiting for “proof” from your body can delay care.
On the other hand, a cluster of painful blisters leans toward Herpes (HSV-1 or HSV-2). A single painless sore can suggest Syphilis. A sore throat after oral sex may require throat-specific swab testing for gonorrhea or chlamydia, not just a urine test. This is where people get tripped up, they test the wrong site.
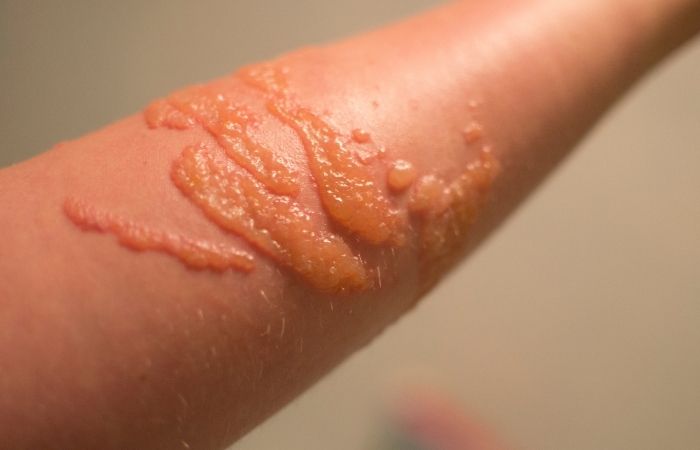
People are also reading: Latex Allergy or STD Rash? How to Tell After Sex
Symptom → Likely Infection → Best Test Type
If you’re trying to match what you’re feeling to what to test for, this table simplifies the logic without overselling a full panel. It reflects common clinical patterns supported by CDC and WHO guidance, while acknowledging that overlap happens.
Figure 1. Symptom-to-test mapping based on common presentation patterns. Overlap exists; timing and exposure history refine decisions.
Do I Need a Full STD Panel or Just One Test?
This is where anxiety and over-testing collide. A lot of people think if they feel one symptom, they should test for everything. Sometimes that makes sense. Often, it doesn’t.
If your only symptom is burning when you pee and it started five days after vaginal sex, your highest-yield test is for Chlamydia and Gonorrhea. Adding Herpes testing without sores may not provide useful information. Testing for HIV the next morning will likely fall inside the window period and give false reassurance.
But if you had unprotected sex with a new partner and you don’t know their status, even with no symptoms, a broader screen makes more sense. That might include HIV antigen/antibody testing, syphilis antibody testing, and urine-based chlamydia/gonorrhea screening.
There’s no moral hierarchy here. There’s just probability and timing. The right test is the one that answers your real risk.
Timing Changes Everything (The Window Period Problem)
One of the biggest mistakes people make is testing too early. You wake up anxious and want answers immediately. That’s human. But infections need time to reach detectable levels.
For example, most NAAT tests for Chlamydia and Gonorrhea become reliable around 7–14 days after exposure. Syphilis antibodies may not show up for 3–6 weeks. Fourth-generation HIV tests typically detect infection between 18–45 days, depending on the test type.
Figure 2. Approximate window periods based on CDC and major public health guidelines. Individual variation exists.
If you test on day three and it’s negative, that doesn’t necessarily mean you’re clear. It means your body hasn’t produced enough detectable markers yet. In those cases, retesting at the peak window gives real confidence instead of fragile reassurance.
Scenario 1: “It Burns When I Pee, Is It an STD or Just a UTI?”
Burning urination is one of the most Googled sexual health symptoms in the world. It’s also one of the most misunderstood. A urinary tract infection and sexually transmitted infections like Chlamydia or Gonorrhea can feel nearly identical in the early stages.
If the burning started within a few days of sex, especially with a new partner, you should strongly consider testing for chlamydia and gonorrhea using a urine NAAT or swab-based test. These bacteria infect the urethra and can cause inflammation that mimics a UTI. The difference is that antibiotics used for common UTIs do not reliably treat these STDs.
If you also notice discharge, pelvic discomfort, bleeding between periods, or testicular pain, the likelihood leans more toward an STD than a simple bladder infection. The safest move in this scenario is targeted testing for chlamydia and gonorrhea rather than guessing.
If your exposure was recent, less than 7 days ago, you may need to wait until the 14-day mark for optimal detection. Testing too early can give you a negative result that doesn’t reflect reality.
Scenario 2: “I Have a Rash or Bump, What Am I Supposed to Test For?”
This is where anxiety spikes. A bump appears and suddenly every image search result looks catastrophic. But not every bump is Herpes, and not every rash is an STD.
Painful clusters of blisters or ulcers that crust over within a week or two are classic for herpes. In that case, the best test is a swab taken directly from the lesion while it is active. Blood antibody testing can help later, but it does not confirm whether a current sore is herpes unless timed correctly.
A single painless sore, especially one that feels firm and doesn’t hurt, raises concern for early Syphilis. That requires a blood antibody test. Syphilis is highly treatable, but timing matters. Antibodies may not appear until several weeks after exposure.
On the other hand, razor burn, ingrown hairs, allergic reactions, yeast infections, and friction injuries are far more common than most people assume. If a lesion is isolated, improving quickly, and clearly associated with shaving or irritation, monitoring for a few days may be reasonable. But if it persists, spreads, or feels systemic, testing is the responsible next step.

People are also reading: Can I Test for STDs While on PrEP? What Changes
Scenario 3: “I Have Discharge, But It Doesn’t Hurt”
Discharge without pain can still signal infection. In fact, many Chlamydia infections produce minimal discomfort while quietly affecting reproductive organs. That’s why it’s sometimes called a silent infection.
If discharge is unusual in color, odor, or consistency after a new sexual partner, testing for chlamydia and gonorrhea is a smart first step. In people with vaginas, Trichomoniasis may also be considered, especially if there is frothy or yellow-green discharge.
Testing should match anatomy and exposure. Vaginal exposure calls for vaginal swabs or urine tests. Anal exposure may require rectal swabs. Oral exposure requires throat swabs. Many people test urine only and miss infections at other sites.
If you’re unsure, a targeted multi-site panel can provide clarity without overtesting unrelated infections.
Scenario 4: “Sore Throat After Oral Sex”
A sore throat after oral sex is often dismissed as a cold. But pharyngeal Gonorrhea and Chlamydia are real, and they frequently cause mild or no symptoms. When symptoms do appear, they can resemble strep throat or irritation.
A standard urine STD test will not detect throat infections. You need a throat swab NAAT specifically designed for that site. This is one of the most common testing mismatches we see, people assume a urine test covers everything.
If the exposure involved receptive oral sex and your throat feels inflamed or persists beyond a few days, targeted throat testing is the right move.
Scenario 5: “I Have No Symptoms, Just Anxiety”
This is more common than any rash or burning. You replay the night. The condom slipped. You don’t know their status. Now you’re hyper-aware of every sensation.
No symptoms does not mean no infection. According to public health data, a large percentage of Chlamydia, Gonorrhea, and even early HIV infections are asymptomatic. Testing in this case is about exposure risk, not visible signs.
If it has been less than a week since exposure, immediate testing may be premature for bacterial STDs. If it has been 14 days or more, chlamydia and gonorrhea testing becomes reliable. HIV and syphilis may require longer windows depending on the test type.
In situations like this, a focused panel that includes HIV antigen/antibody testing, syphilis antibody testing, and urine-based bacterial screening is often appropriate. It’s not about panic. It’s about certainty.
When Symptoms Overlap, And Why Guessing Fails
Here’s the uncomfortable reality: many STDs share overlapping symptoms. Burning can mean chlamydia, gonorrhea, UTI, or even irritation. A rash can be herpes, syphilis, dermatitis, or nothing serious at all.
Self-diagnosis through symptom comparison alone is unreliable. Testing is what separates speculation from fact. The right test answers the right question, and prevents unnecessary treatment or untreated infection.
If you’re still asking “which STD test do I need based on my symptoms,” the answer is usually narrower than you think. It’s rarely everything. It’s almost always something specific, targeted, and timed correctly.
Rapid Test or Lab Test, What Actually Makes Sense for You?
Once you know which infection you’re targeting, the next question hits fast: should you use a rapid at-home test, a mail-in lab kit, or go to a clinic? This is where fear and practicality collide. You want accuracy. You want privacy. You also want answers before your imagination spirals.
Rapid tests are designed for speed and discretion. Many use antigen or antibody detection methods and can provide results in minutes. Lab-based NAAT or PCR tests, especially for Chlamydia and Gonorrhea, remain the gold standard for sensitivity. That doesn’t mean rapid tests are useless, it means timing and correct use matter.
If your exposure was recent and you are inside a window period, even the most advanced lab test can return a false negative. That’s not a flaw in the kit. It’s biology. Your body needs time to produce detectable markers.
Figure 3. Comparing speed, privacy, and use cases across testing methods.
If discretion matters, and for many people it does, ordering directly through STD Test Kits allows you to test privately without sitting in a waiting room rehearsing explanations in your head.
How Accuracy Really Works (And Why Timing Beats Panic)
Accuracy isn’t a single number. It depends on sensitivity, specificity, and when you test. Sensitivity reflects how well a test catches true infections. Specificity reflects how well it avoids false positives. Both matter.
NAAT tests for Chlamydia and Gonorrhea typically show very high sensitivity when performed after the window period. Fourth-generation HIV antigen/antibody tests are considered highly accurate after 45 days. Blood antibody testing for Herpes becomes more reliable several weeks after infection, but it cannot always pinpoint timing.
The most common cause of inaccurate results is not the kit, it’s testing too soon or collecting the sample incorrectly. Reading instructions carefully and respecting timing windows is what transforms a test from a guess into a decision-making tool.
When a Combo Panel Actually Makes Sense
A combo STD panel is not about panic-buying every possible test. It makes sense when exposure risk is broad or unclear. For example, if you had unprotected vaginal or anal sex with a new partner and do not know their status, limiting testing to just one infection may leave blind spots.
In that case, a discreet multi-infection panel that checks for HIV, Syphilis, Chlamydia, and Gonorrhea provides comprehensive screening aligned with public health recommendations. It’s especially appropriate when you have no symptoms but want certainty.
If your situation matches that description, a Combo STD Home Test Kit can cover the most common bacterial and viral infections in one private step. That’s not fear-based medicine. That’s efficient medicine.
How to Avoid False Negatives and Misreads
Testing is only as good as execution. For urine-based tests, avoid urinating for at least an hour before collection. For swabs, follow depth and timing instructions carefully. For fingerstick blood tests, ensure adequate sample volume.
Reading a rapid test too early can show incomplete results. Reading it too late can create evaporation lines that look positive but are not. If a result is unclear, repeating the test at the appropriate interval is more reliable than obsessively zooming in under bathroom lighting.
If symptoms persist despite a negative result, retesting after the peak window period is recommended. Symptoms evolving over time can change the testing strategy.
If You’re Still Unsure, Use This Decision Logic
If you have burning or discharge → test for Chlamydia and Gonorrhea.
If you have sores or blisters → consider Herpes and Syphilis testing.
If you had condom failure or unprotected sex and no symptoms → consider a targeted panel including HIV and syphilis in addition to bacterial screening.
If your only symptom is anxiety → timing matters more than symptom matching. Wait for the appropriate window, then test strategically.
The question is not “what STD do I have?” It’s “what question am I trying to answer?” Once that’s clear, the right test becomes obvious.
If the Test Is Positive, Take a Breath First
If you see two lines. If the portal says positive. If your chest drops into your stomach. Pause. Most sexually transmitted infections are treatable, and many are curable. A positive result is a medical situation, not a moral verdict.
Chlamydia, Gonorrhea, Syphilis, and Trichomoniasis are bacterial infections and are typically treated with antibiotics. Herpes and HIV are viral, meaning they are managed rather than cured, but modern treatment makes long, healthy lives absolutely possible. According to CDC treatment guidelines, early detection dramatically improves outcomes and reduces transmission risk.
The first step after a positive rapid result is confirmatory testing if required. Some rapid tests are considered preliminary screens. A follow-up lab test ensures clarity before treatment decisions are finalized.
How to Tell a Partner Without Spiraling
This is the part people fear more than the infection itself. The conversation. The text. The imagined judgment. But disclosure is about care, not confession.
You can keep it simple: “I tested positive for something that’s treatable. I’m letting you know so you can get tested too.” You do not owe a dramatic explanation. You owe honesty and timing.
Public health departments often provide anonymous notification systems, especially for infections like HIV and Syphilis. The goal is stopping spread, not assigning blame. Testing is shared responsibility.
When to Retest After Treatment or Exposure
Retesting depends on the infection. For Chlamydia and Gonorrhea, many guidelines recommend retesting about three months after treatment to rule out reinfection. Testing too soon after antibiotics can detect leftover bacterial DNA and produce confusing results.
For HIV, if initial testing was performed early, follow-up testing at the 45-day mark (for fourth-generation tests) or longer may be advised. For Herpes, antibody testing becomes more reliable weeks after the initial outbreak.
If symptoms continue despite negative tests, reassessment is important. Not every genital symptom is an STD, and not every STD behaves predictably. Persistent pain, fever, or systemic symptoms warrant in-person care.
People are also reading: Can I Test for Herpes While on Antivirals?
FAQs
1. I have burning when I pee, but no discharge. Is that still an STD?
It can be. Burning alone is enough to justify testing for Chlamydia and Gonorrhea, especially if it started after sex. A lot of people expect dramatic discharge as “proof,” but many infections are subtle. If it feels different than your baseline and there was recent exposure, that’s your cue, not your shame.
2. I only had oral sex. Do I really need to test?
Oral sex counts. It’s lower risk for some infections, higher for others. A sore throat after giving oral sex can point to throat-based gonorrhea, which won’t show up on a urine test. If your exposure was oral, your test site should match your exposure site. Your body doesn’t care what you call it, it just reacts to contact.
3. What if I just feel “off” but can’t explain it?
That intuition matters. Maybe there’s no textbook symptom, just a sense that something shifted. In that case, think back to timing. If it’s been at least two weeks since exposure, a targeted screen for common bacterial STDs is reasonable. Testing isn’t dramatic. It’s clarity.
4. Should I test for herpes even if I don’t have sores?
This one’s nuanced. Blood testing for Herpes can detect antibodies, but it doesn’t always tell you when you were infected or whether a specific partner transmitted it. If you’ve never had sores and just feel anxious, talk through timing and risk first. If you’ve had a new unexplained lesion, that’s when swab testing becomes powerful.
5. If a condom was used, am I safe enough to skip testing?
Condoms dramatically reduce risk. They’re one of the best tools we have. But they don’t cover all skin, and they don’t eliminate risk entirely. If the condom broke, slipped, or you’re unsure, testing becomes less about distrust and more about confirmation.
6. What if my symptoms disappeared, does that mean I’m fine?
Not necessarily. Some STDs calm down without leaving. Chlamydia can go quiet while still present. Herpes can flare and then fade. Symptom disappearance isn’t the same as infection clearance. Testing answers that question cleanly.
7. I’m embarrassed to order a test. Is that ridiculous?
It’s human. Sexual health still carries stigma, even though infections are common. But ordering a test is an act of responsibility, not confession. You’re not the first person to click “add to cart” with a racing heart. You won’t be the last.
8. What if I test positive, is my sex life over?
No. Absolutely not. Most bacterial STDs are cured with antibiotics. Viral infections like Herpes and HIV are manageable with modern treatment. Millions of people date, love, have sex, and build families after a diagnosis. A test result is information. It’s not identity.
9. How do I know I’m not overreacting?
If you’re reading this at 1 a.m., you’re not overreacting. You’re seeking answers. Overreacting would be ignoring symptoms, avoiding testing, or gambling with uncertainty. Calm, informed action is not panic. It’s maturity.
10. Do I need to tell every past partner if I’m just testing “to be safe”?
Not if you don’t have a confirmed infection. Routine screening is preventive care. If you do test positive, then partner notification becomes part of responsible follow-through, and it can be done respectfully, even anonymously when needed.
You Deserve Answers, Not Assumptions
The entire point of this guide is clarity. Not panic. Not overtesting. Not denial. If you’re asking which STD test you need based on your symptoms, you’re already doing the responsible thing.
Whether that means a targeted urine test for Chlamydia, a throat swab for Gonorrhea, a blood test for Syphilis, or a broader panel for peace of mind, the goal is the same: accurate information that lets you move forward.
If you’re ready for discreet, private testing, you can explore options at STD Test Kits. If your situation calls for broader screening, the 7-in-1 Complete At-Home STD Test Kit checks multiple common infections in one step, without a waiting room.
How We Sourced This Article: This guide integrates CDC sexually transmitted infection treatment guidelines, WHO public health data, peer-reviewed infectious disease studies, and lived-experience reporting from sexual health education platforms. Approximately fifteen sources informed this article; below are six key references chosen for authority and reader clarity. All links open in a new tab for verification.
Sources
CDC Sexually Transmitted Infections Treatment Guidelines
World Health Organization: Sexually Transmitted Infections Fact Sheet
Accuracy of NAAT Testing for Chlamydia and Gonorrhea (Peer-Reviewed Study)
Planned Parenthood: STD Information and Testing
Mayo Clinic: Herpes Diagnosis and Treatment
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He combines clinical precision with sex-positive public health advocacy, helping patients navigate testing decisions with clarity and confidence.
Reviewed by: L. Hernandez, MSN, APRN, FNP-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.