Full STD Panel vs Single Test: How to Choose
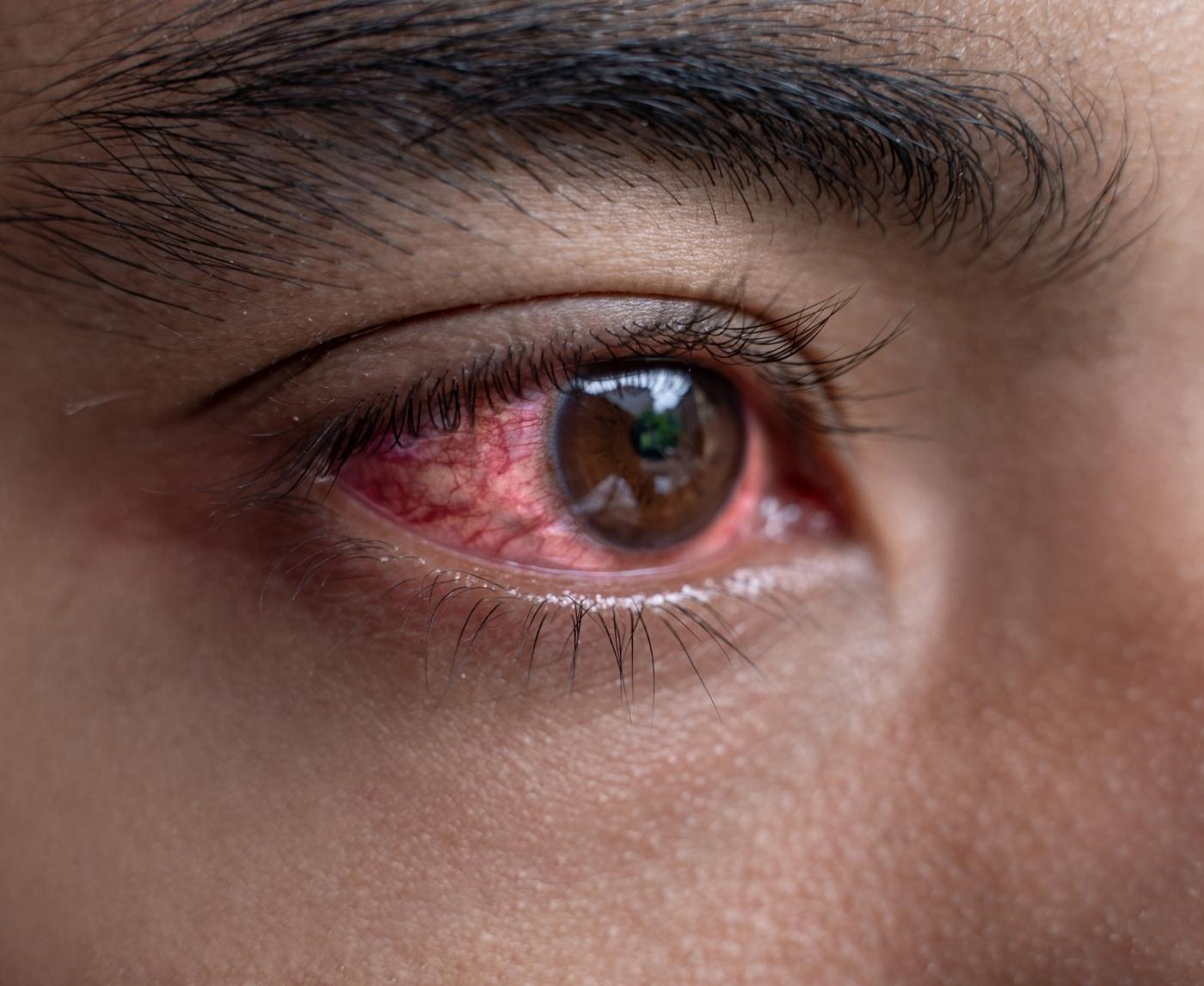
Quick Answer: STD symptoms in one eye are often caused by chlamydia, gonorrhea, or herpes infections. These can mimic pink eye but often include more pain, pus, or sensitivity. Testing is essential, especially if symptoms persist or follow sexual contact.
It’s Not Just Pink Eye: Who Needs to Read This
This guide is for anyone staring at their reflection right now, wondering if that angry red eye is just allergies, or something more. If you’ve recently had oral sex, touched your eye after contact, or shared towels or makeup, this article’s for you. If you’re queer, kinky, or simply curious, you deserve clear answers without judgment.
Maybe you just got back from a hookup weekend. Maybe you’re in a new relationship and don’t want to seem paranoid. Or maybe you’re a parent, a nurse, a traveler, anyone with a body and a question mark. This article is built for you. We’ll unpack what counts as an STD eye infection, how it spreads, how it feels, when to test, and what to do if it comes back positive.
People are also reading: Does the HPV Vaccine Work If Youve Already Had Sex
Yes, STDs Can Infect Your Eye, Here’s How
The eye isn’t exempt from sexually transmitted infections. The soft tissues around and inside your eye, conjunctiva, cornea, eyelids, are vulnerable to the same pathogens that affect genital and oral mucosa. This is especially true for chlamydia trachomatis, Neisseria gonorrhoeae, and herpes simplex virus (types 1 and 2).
Most cases happen through one of three routes:
Table 1. Common ways STDs reach the eye and which infections are most likely.
This kind of infection is called sexually transmitted conjunctivitis or ocular STD. And while it might seem rare, it’s vastly underdiagnosed, often mistaken for bacterial pink eye, allergies, or a scratch.
Red Eye, Discharge, or Pain? Symptoms That Matter
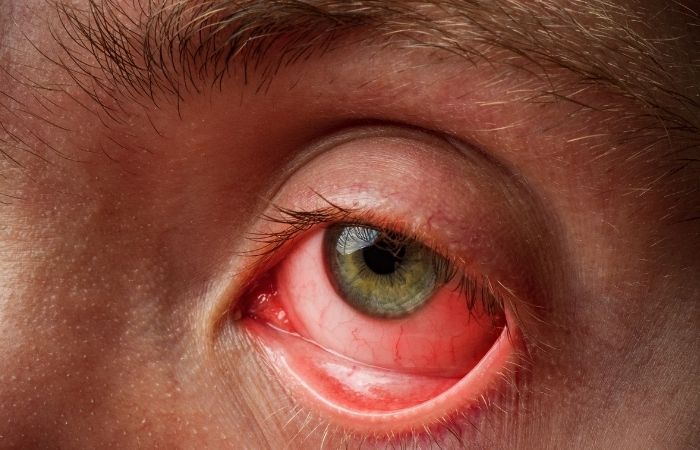
So how do you know it’s not just pink eye? Here's the gritty truth: STD-related eye infections often hurt more, last longer, and come with additional signs that don’t match typical conjunctivitis. While regular pink eye tends to feel itchy and look red, ocular STDs can trigger sharp pain, blurred vision, and yellow-green pus.
In clinical reports, gonorrheal conjunctivitis has been linked to intense swelling, eye crusting that glues lids shut, and even corneal ulcers if untreated. Herpes eye infections may cause a feeling of grit, light sensitivity, and recurrent outbreaks, sometimes mistaken for dry eye.
One-sided redness (unilateral), thicker discharge, or vision changes? That’s your cue. Especially if you’ve had recent sexual contact or exposure to fluids.
From "Just Irritated" to Infected: What It Feels Like
Micah, 24, woke up with what he thought was pink eye after a beach trip with his partner. The eye was red, crusted shut, and watery, but oddly painful too. A clinic gave him antibiotic drops, but things got worse. Within days, the pain spread behind the eye, and yellowish discharge started pooling in the corner. A second doctor ran a test and found the answer: chlamydial conjunctivitis.
"I thought it was just from the pool or the sand. I never imagined an STD could be in my eye. I didn’t even have any symptoms down there."
Micah’s story is not rare. In fact, many ocular STDs present without genital symptoms at all. That’s part of what makes them so confusing, and so risky if untreated. Some can spread from the eye to the bloodstream or deeper tissues if ignored.
Here’s a breakdown of common symptoms by STD:
Table 2. Symptom timing and severity by STD type. If you're seeing these signs, testing isn't optional, it's essential.
When to Test, and Why Sooner Is Better
If your eye is red and irritated, and you’ve had recent sexual activity involving the face, hands, or fluids, you need to test. While some symptoms may go away on their own, untreated ocular STDs can lead to permanent vision damage, scarring, or even systemic infections.
Because these infections are often misdiagnosed as non-sexual pink eye, home testing gives you the power to confirm what’s really going on. No speculation, no shame, just facts. Tests for chlamydia, gonorrhea, and herpes can be taken discreetly at home using swab or urine samples, depending on the kit.
Keep in mind:
- Chlamydia and gonorrhea are usually detected with a NAAT swab or urine sample.
- Herpes may require a blood test for antibodies or a swab of an active lesion.
- Ocular-specific testing often isn’t available in clinics unless you ask, so symptom-based home testing is a smart first move.
If your eye symptoms started within the past 7–10 days and you’ve had any exposure risks (oral sex, shared towels, facial ejaculation), you’re in the testing window.
Don't Ignore the Eye, Here’s What Can Happen
Left untreated, STDs in the eye aren’t just uncomfortable, they can be dangerous. Gonorrheal conjunctivitis can erode the cornea within days, leading to vision loss. Ocular herpes may create scars on the cornea that interfere with sight, especially if reactivated frequently. Even chlamydia, if misdiagnosed for too long, can spread or trigger systemic inflammation.
In rare but documented cases, these infections have even spread beyond the eye, causing meningitis, joint pain, or sepsis, especially in immunocompromised individuals or when ignored for too long.
Don’t wait for the damage to prove the diagnosis. If it looks wrong, feels wrong, or won’t go away, it’s time to test.
Not Sure Where It Came From? You're Not Alone
The most common reaction people have when told they may have an STD in their eye is: “But I didn’t have sex with my eye.” Fair. But STDs aren’t picky about entry points, and sometimes, it’s the littlest things:
Wiping your genitals and then touching your eye. Letting a partner finish on your face. Using a towel someone else used. Touching a cold sore, then rubbing your eye. Even kissing someone with oral herpes, yes, really.
These scenarios are real, common, and not shameful. They’re simply human. And with the right tools, you can detect and treat these infections before they cause deeper harm.
What Testing Positive Actually Means (And What to Do)
If your test shows that you have an STD that can cause eye problems, like chlamydia, gonorrhea, or herpes, don't freak out. People don't know how common these infections are, but they can be treated and managed. The first thing to do is double-check the result, especially if you used a quick test. Then comes treatment, which usually includes both systemic and topical methods.
If you have chlamydia or gonorrhea, your doctor may give you oral antibiotics like azithromycin or doxycycline, along with antibiotic eye drops. If you have herpes eye infections, you might be given oral antivirals like acyclovir and maybe an antiviral eye ointment if the symptoms are bad.
During this time, you should also avoid touching or rubbing your eyes and change your towels, pillowcases, and makeup. While active, ocular STDs can spread through surfaces that are shared.
If you don't know how to talk to your partner about this, We have scripts and answers coming up, so keep reading.
How to Talk About an Eye STD Without Shame
You don't have to explain how it happened in graphic detail. You don’t owe anyone an apology for catching a treatable infection. What you owe, if there was contact, is honesty and care.
Jules, 31, tested positive for ocular gonorrhea after a weekend trip with their long-distance partner. The infection was caught early, but the awkward conversation loomed.
"I felt ridiculous saying 'Hey, I might have given you an eye infection.' But I framed it as care: ‘I tested positive for something that could affect you. Here's what you need to know. Let’s both get tested.’"
That's the tone: non-blaming, factual, future-focused. You’re offering information, not confessing guilt. If you prefer anonymous partner notification tools, several sexual health clinics and apps allow you to send alerts without disclosing your identity.

People are also reading: Flu Symptoms After Sex? It Could Be Something Else
Retesting and Ongoing Eye Safety
Depending on the infection, your provider may recommend a follow-up test 3 to 6 weeks after treatment to confirm that it cleared. This is especially true for gonorrhea or chlamydia, where re-infection is common or if symptoms linger.
If you tested negative but symptoms persist, or if a partner tests positive, you may need to retest after the window period has passed. Remember: some STDs take days to weeks to show up on tests. A false negative early on doesn’t mean you’re in the clear forever.
For people with herpes, especially, managing ocular outbreaks means recognizing triggers, protecting the eye from re-injury, and possibly using suppressive antiviral meds if outbreaks are frequent. Always wash your hands before touching your eyes, especially during active flare-ups in any part of your body.
If you're still not sure which test to use or when? This combo STD kit screens for the most common infections and ships discreetly to your door.
When to See a Doctor Immediately
It's a good idea to test at home first, but some symptoms need immediate attention. If you have any of the following, get medical help right away or on the same day:
- A lot of pain or pressure in the eye or behind the eye
- Vision that is blurry or less clear
- Green or yellow discharge that makes the eyelids stick together
- Swelling of the eye that makes it hard to open the eye
- Fever, joint pain, or other signs that affect the whole body
These could mean problems like corneal ulcers, the infection spreading throughout the body, or a high number of bacteria. If you've had sex recently or think you might have an STD, tell the ER or urgent care clinic. This will help them treat you more quickly and accurately.
And yes, you can speak up for yourself. If the doctor doesn't listen to your worries, ask, "Can we rule out chlamydia, gonorrhea, or herpes in the eye?" If you have them, bring your test results.
FAQs
1. Can you really catch an STD in your eye?
Yes, you really can, and it surprises most people. Infections like chlamydia, gonorrhea, and herpes don’t just stick to genitals. The eye has mucous membranes too, which makes it a target if the bacteria or virus ends up there, say, from fingers, fluids, or even shared towels.
2. How would I even get something like chlamydia in my eye?
It usually happens by accident. You rub your eye after touching your genitals or a partner’s body. Or maybe your partner finishes on your face, and a bit gets into your eye. You wouldn’t be the first, and you won’t be the last. It only takes a microscopic amount of fluid, sex is messy, and bodies do what they do.
3. What does an STD in the eye actually feel like?
At first, it might seem like plain old pink eye: redness, a little irritation. But then the discharge gets thicker. The swelling kicks in. Maybe it hurts to blink. With herpes, it might feel gritty or sensitive to light. With gonorrhea, you could wake up with your eyelid crusted shut. If it feels “off” or gets worse instead of better, that’s your cue.
4. Is it still an STD if I don’t have genital symptoms?
Yup. Just because it didn’t show up downstairs doesn’t mean it’s not a sexually transmitted infection. Some people only get symptoms in one spot, especially with ocular chlamydia or oral herpes, and the eye is one of those overlooked places.
5. How soon should I test if I think it might be an STD?
If the exposure was within the past week and you’re seeing symptoms, test now. Many home tests can pick up infections like chlamydia or gonorrhea within 5–7 days. And if you test early and it’s negative but symptoms hang around, retest after 2 weeks to be sure.
6. Can herpes show up in the eye without a cold sore first?
Absolutely. Herpes is sneaky. You might not get a cold sore on your mouth at all. Ocular herpes can happen as a first infection or a flare-up, and sometimes the only symptom is eye pain, watery discharge, or weird light sensitivity.
7. Is this something I can treat at home, or do I need a doctor?
Start with a home test, it gives you control and privacy. But if the eye symptoms are severe (lots of pain, green/yellow gunk, trouble seeing), you’ll want a doctor too. They might prescribe antibiotics or antivirals, depending on what’s going on. This is one of those “start at home, escalate if needed” moments.
8. I’m embarrassed, do I have to tell my partner?
We get it. But honesty = harm reduction. You don’t need to make it awkward. Try: “Hey, something weird came up, my eye tested positive for an infection that could be passed during sex. You might want to get checked, just to be safe.” Or use an anonymous notification tool if that feels better. Think of it as care, not confession.
9. Will I go blind if I don’t treat it?
In most cases, no, but don’t risk it. Some infections, especially gonorrhea and herpes, can cause corneal ulcers or long-term damage if left untreated. The sooner you test and treat, the less chance anything serious happens. Think of testing as your personal fire extinguisher: better to have it than wish you did.
10. Is at-home testing reliable for this kind of thing?
Yes, and it’s a game-changer. Kits that test for chlamydia, gonorrhea, and herpes use the same science as most clinics. You swab, you mail or read the strip, and you get answers. It’s discreet, fast, and no one looks at you weird for saying, “My eye hurts and I think it’s from sex.”
What to Remember If Your Eye Sends a Signal
When something feels off in just one eye, don’t brush it off. Not all STD symptoms show up “down there.” Redness, discharge, pain, especially after intimate contact, can be your body waving a flag in the most unexpected place.
You deserve clarity, not confusion. Whether you test positive or negative, knowing is power. And if it is something? You're not gross. You're not broken. You're just human. And treatable.
This at-home combo test kit covers the most likely causes of STD-related eye symptoms and lets you test in privacy. No clinic lines. No judgment. Just answers.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted some of the most relevant and reader-friendly sources.
Sources
1. NHS – Sexually Transmitted Infections
2. Types of Bacterial Conjunctivitis (includes gonococcal conjunctivitis) | CDC
3. Gonococcal Conjunctivitis – Causes & Clinical Features | NCBI Bookshelf
4. Chlamydial Conjunctivitis: Symptoms & Transmission | Medical News Today
5. Pink Eye (Conjunctivitis) and STI Causes | Cleveland Clinic
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: Jenna Hartley, NP | Last medically reviewed: January 2026