Last updated: April 2026
Here's something most articles don't tell you upfront: chlamydia discharge in men is rarely dramatic. It's not a flood. It's not always colorful. In most cases, it's subtle, and that's exactly why so many men overlook it or chalk it up to something else entirely.
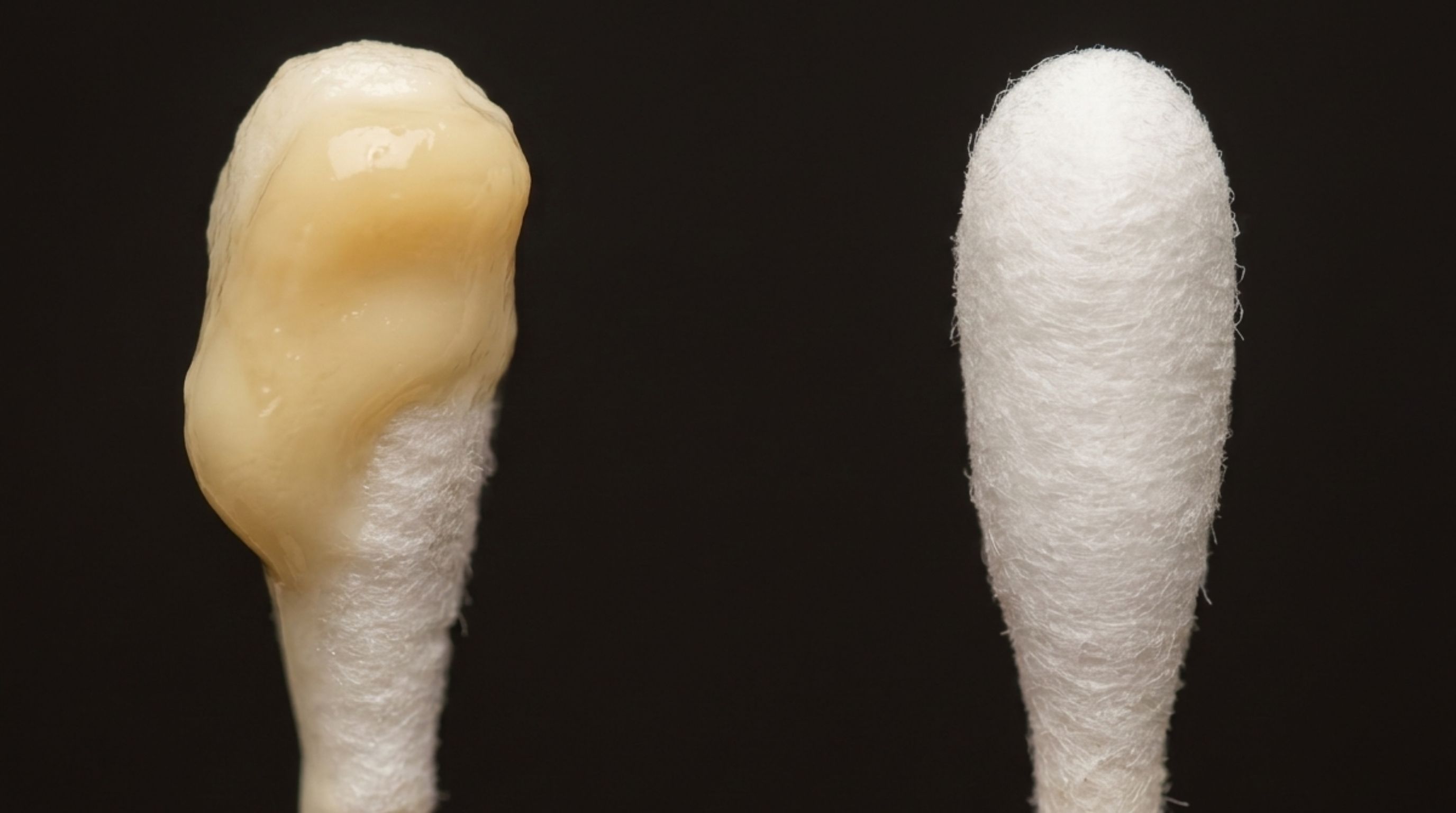
The most common presentation is a small amount of white, cloudy, or watery fluid at the tip of the penis. It may appear as little as a single drop of clear or slightly milky fluid at the urethral opening, particularly noticeable first thing in the morning before urinating. Some men describe it as a faint glossy moisture around the tip. Others notice dried secretions, a slight crustiness around the urethral opening after waking up, without obvious fluid at any other time of day.
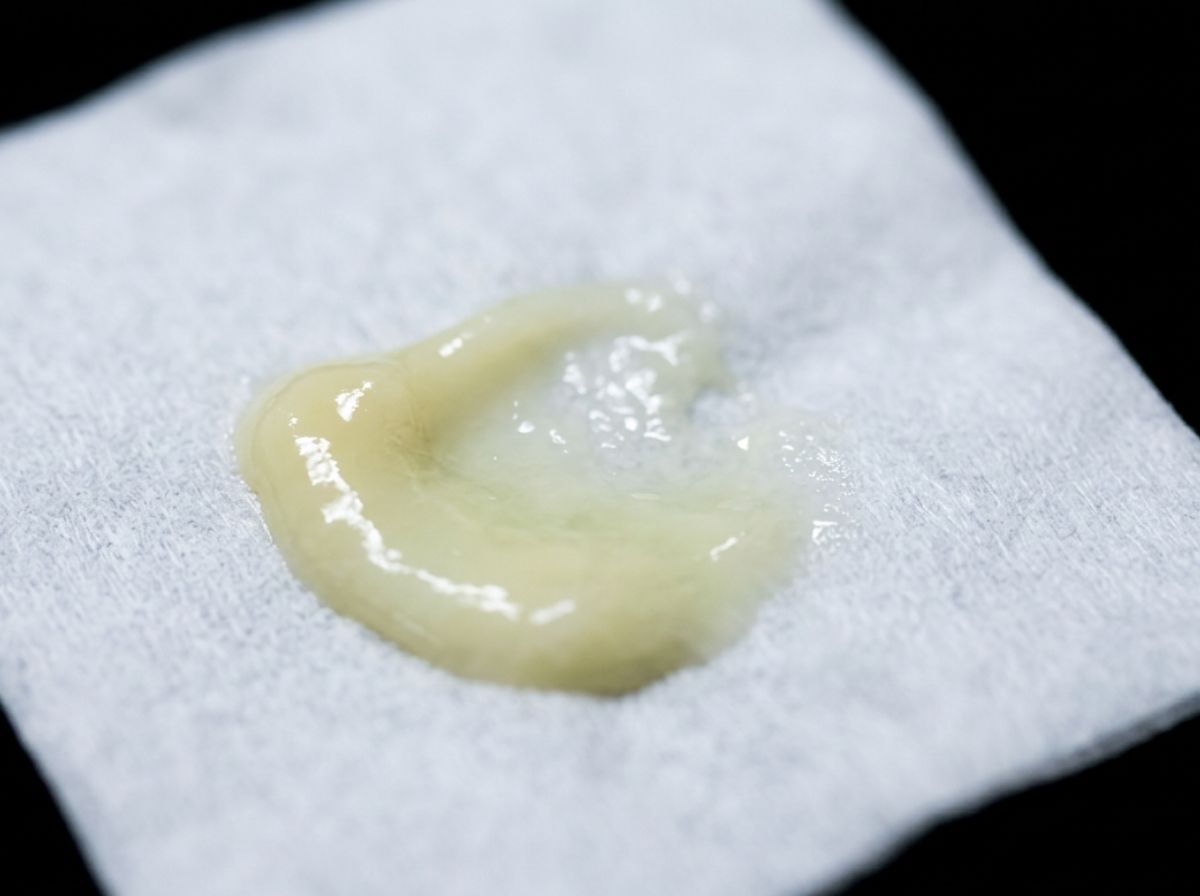
When discharge is more pronounced, it tends to be described as mucoid or mucopurulent, a thicker, cloudy consistency somewhere between clear mucus and white fluid. Occasionally, it takes on a yellow tint, and in rarer cases, a slightly brownish or off-white color. It may come with an unpleasant or slightly musky odor, though smell alone is unreliable as a diagnostic signal; hygiene, urine concentration, and other factors all affect how things smell down there. The honest answer to "what does chlamydia smell like on a guy" is: there's no single answer, and odor cannot confirm or rule out infection.
One of the most important things to understand about chlamydia discharge in men is that it can be intermittent. The discharge may appear for a day or two, then seem to stop, then return. This pattern leads a lot of men to assume things have cleared up on their own; they haven't. The infection is still there, still transmissible, and still progressing silently even when there's nothing visible to see.
People are also reading: The Michigan Syphilis Outbreak That Left 5 Women Nearly Blind
Why Chlamydia Discharge Is So Easy to Miss
Chlamydia has a well-earned reputation as the silent infection, and nowhere is that more true than in men. According to the NCBI's clinical review of urethritis, roughly half of all men with chlamydia experience no symptoms at all. That means if you're in a room of ten infected men, five of them would have no idea anything was wrong. None of them would have any discharge to notice.
For the other half, symptoms don't always announce themselves clearly. The discharge that does appear is frequently mistaken for pre-ejaculate, a normal amount of moisture, or post-urination drip. It's not thick or green or alarming in the way people imagine STI discharge to look. It can be so minimal that a man only notices it because he's specifically looking, after a risky exposure, after a partner mentions their own symptoms, or after he's just started paying closer attention to his body.
There's also a timing issue. Chlamydia symptoms, when they appear, typically develop somewhere between one and three weeks after exposure. But they can take longer. And once they show up, they don't necessarily follow a steady progression. The discharge can come and go over days or weeks, creating a false impression that the body has fought the infection off. It hasn't. Chlamydia trachomatis, the bacteria responsible, doesn't resolve without treatment, and while it lingers, it can be passed to sexual partners who are equally unlikely to notice anything wrong.
This is partly why the CDC's 2024 provisional STI surveillance data still counts chlamydia among the most widely reported bacterial infections in the United States, despite the overall STI case burden declining for the third consecutive year. More than 2.2 million combined chlamydia, gonorrhea, and syphilis cases were reported in 2024, and the actual number of chlamydia infections is believed to be significantly higher, since so many go undetected and unreported. Visibility of symptoms does not equal absence of infection.
Other Symptoms That Show Up Alongside the Discharge
Discharge rarely travels alone. When chlamydia does produce noticeable symptoms in men, it typically arrives as a package, and recognizing what's in that package makes it easier to connect the dots between what you're experiencing and what you might be dealing with.
The most common companion to discharge is a burning or stinging sensation when urinating. This happens because Chlamydia trachomatis typically infects the urethra, the tube running through the penis that carries both urine and semen. Once the urethra becomes inflamed, urine passing through it irritates the already-sensitive tissue. The discomfort can range from a mild warm sensation to something closer to fire. For some men, this burning is the first thing they notice, not discharge at all.
Urethral itch or irritation is another common companion. Some men describe it as a sandpapery, tingling sensation inside the urethra, or an uncomfortable awareness of the urethral opening, sometimes described in searches as "weird feeling in urethra male." This isn't pain exactly, but it's not normal either, and it tends to worsen without treatment. In some cases, the tip of the penis itself becomes mildly red or sore.
In a smaller subset of cases, when chlamydia is left untreated and the infection travels further, it can reach the epididymis, the coiled tube behind each testicle that carries sperm. This complication, called epididymitis, causes pain, tenderness, and swelling in one or both testicles. It may feel like a dull ache or a sharper pain, and the scrotum can become warm to the touch. Epididymitis from untreated chlamydia is one of the more serious complications the infection can cause in men, and if you're experiencing testicular pain alongside any discharge or urinary symptoms, that combination warrants testing without delay.
Chlamydia Discharge vs. Other Causes, How to Tell the Difference
If you're looking at some unusual moisture at the tip of your penis and wondering whether it's chlamydia, you're already halfway to the right question. The other half of the question is: what else could it be? Because several things can produce discharge-like fluid in men, and they don't all mean the same thing or require the same response.
The most important comparison to make is chlamydia versus gonorrhea, because both are extremely common, both cause urethral discharge, and both can be present at the same time. The key difference is volume and appearance. Gonorrhea discharge tends to be thicker, more copious, and more noticeably colored, often yellow, green, or white and pus-like. Chlamydia discharge, by contrast, tends to be lighter, clearer, and more mucoid. The gonorrhea discharge that appears in search results, thick, dripping, obviously infected-looking, is more typical of that infection. But here's the important caveat: you cannot reliably tell them apart based on appearance alone. Co-infections are common, symptoms overlap, and a mild gonorrhea infection can look exactly like a typical chlamydia presentation. Only a test distinguishes them accurately.
Non-specific urethritis (NSU) is another possibility. NSU is urethral inflammation caused by bacteria other than chlamydia or gonorrhea, sometimes common bacteria that found their way into the urethra during sex. The discharge and burning it produces can look and feel nearly identical to chlamydia. Prostatitis, an inflammation of the prostate gland, can also cause a transparent, sticky discharge and pelvic discomfort, though this tends to come with other symptoms like lower back pain or pain during ejaculation. Balanitis, an inflammation of the head of the penis (more common in uncircumcised men), can cause localized redness and a whitish or yellowish discharge from the skin surface rather than the urethral opening itself.
The bottom line is that symptoms and visual inspection will not tell you which infection you have. If you've noticed any kind of unusual penile discharge, regardless of how small, how clear, or how mild it seems, testing is the only way to get a real answer. An at-home test means you don't have to wait for a clinic appointment, navigate an awkward conversation at a walk-in center, or put the question on hold for days while the uncertainty mounts. The Chlamydia At-Home STD Test Kit from STD Test Kits delivers results from a simple urine sample with over 99% accuracy, no clinic, no waiting room, no guesswork. For those who've had any kind of higher-risk exposure, the Chlamydia & Gonorrhea At-Home STD Test Kit screens for both infections at once, which makes sense given how frequently they appear together.
When Discharge Appears and Why Timing Matters
Timing is one of the most misunderstood parts of chlamydia, both in terms of when symptoms show up and when testing becomes reliable. Getting both of these right matters, because acting too early in either direction can give you false reassurance.
When symptoms do appear, they typically develop somewhere between one and three weeks after exposure. This incubation window, the time between picking up the bacteria and the body beginning to show signs, is why discharge doesn't appear the morning after a risky night. If something shows up within 24 to 48 hours, it's unlikely to be chlamydia and more likely to be irritation, a pre-existing condition, or anxiety making you hyper-aware of your body. That doesn't mean it's nothing, but it means you need to wait for the testing window before you'll get a meaningful result.
The testing window for chlamydia is 14 days after exposure. Testing before that point risks a false negative, not because the test is unreliable, but because the bacterial load may not yet be detectable. This is genuinely one of the harder things to sit with: you've had an exposure you're worried about, something feels off, and the most responsible thing to do is wait two weeks before testing. But testing too early and getting a negative result you trust, while the infection is actually incubating, is worse than waiting and getting an accurate one.
After 14 days, testing is reliable. If you have discharge or other symptoms alongside that, testing at that point is both appropriate and urgent. If you have no symptoms but had a genuine exposure, testing at 14 days still makes sense, because, as covered earlier, roughly half of infected men have no symptoms at all. The absence of discharge is not a negative test result. Only a test is a negative test result.

People are also reading: Can You Have Sex After a Gonorrhea Diagnosis? What's Safe and When
What Happens If Chlamydia Discharge Goes Untreated in Men
Discharge isn't just inconvenient. It's your body signaling that an infection is active, spreading, and doing biological work it shouldn't be doing. Left untreated, chlamydia in men doesn't usually stay confined to the urethra forever, it can travel, and when it does, the consequences get more serious.
The most significant complication for men is epididymitis, inflammation of the epididymis, the small coiled tube that sits behind each testicle and plays a key role in sperm transport and maturation. When chlamydia bacteria reach this structure, it becomes inflamed, causing testicular pain and swelling that can range from a mild ache to severe, incapacitating discomfort. In rare cases, untreated epididymitis can affect fertility, though this outcome is far more common in women with untreated chlamydia than in men. Still, testicular pain that shows up weeks after a sexual exposure, especially alongside any discharge history, is a clinical flag worth acting on.
Long-term untreated urethral infection can also cause scarring of the urethra in rare cases, narrowing the tube and making urination difficult. This is an uncommon complication, but it illustrates why chlamydia is worth treating promptly rather than waiting to see whether symptoms resolve. They can seem to improve, and the infection remains. Symptoms fluctuate. The bacteria don't leave on their own.
There's also the transmission dimension. Every day an infection goes undetected or untreated is a day it can be passed to someone else, who may be equally asymptomatic, equally unlikely to notice discharge, and equally at risk of long-term complications. This is particularly relevant for female partners, for whom untreated chlamydia carries a well-documented risk of pelvic inflammatory disease and subsequent fertility complications. Testing yourself isn't just about your own health. It protects the people you sleep with.
Partner Communication and What to Do After a Positive Result
Getting a positive chlamydia result, whether from an at-home kit or a clinic, is genuinely not a crisis. Chlamydia is one of the most treatable bacterial infections that exists, and effective treatment is available. The important thing is what you do with the information.
The first step is contacting anyone you've had sexual contact with during the period you may have been infected. This is typically defined as the 60 days prior to your positive result, though the exact timeframe depends on when your last negative test was. This conversation is uncomfortable for most people, there's no way around that, but it's the single most important thing you can do to prevent further spread. Many sexual health clinics offer anonymous partner notification services if you want support with that process. Your name doesn't have to be attached to the message.
You should avoid sexual contact until both you and your partner(s) have completed treatment and been cleared. Retesting is recommended around three months after treatment, as reinfection from an untreated partner is the most common reason chlamydia comes back. That's not a treatment failure, it's a biological reality. The infection doesn't create immunity. You can get chlamydia again even after successful treatment, which is one of the arguments for regular, routine testing if you have multiple partners or new partners over time.
FAQs
1. What does chlamydia discharge look like in men, is it always visible?
No, it isn't always visible. Around half of men with chlamydia have no symptoms at all, including no discharge. When discharge is present, it's often subtle, a small amount of white, cloudy, or watery fluid at the urethral opening, most noticeable first thing in the morning.
2. Can chlamydia discharge in men be clear?
Yes. Chlamydia discharge in men is frequently clear or watery, especially in the early stages of infection. The fact that it doesn't look obviously infected, no yellow, no green, no obvious pus, doesn't mean the infection isn't there. Clear discharge from the urethra that appears outside of sexual arousal warrants testing.
3. How quickly does chlamydia discharge appear after exposure?
When discharge does appear, it typically shows up between one and three weeks after exposure. It can take longer in some cases. Discharge appearing within 24 to 48 hours of a sexual encounter is unlikely to be chlamydia, that's too fast for the incubation period.
4. Can chlamydia discharge come and go in men?
Yes. This is one of the most common patterns and one of the reasons the infection goes untreated for so long. Discharge that appears, disappears, and reappears does not indicate the infection is resolving, it reflects normal fluctuation in the body's inflammatory response. The infection remains active throughout.
5. How is chlamydia discharge different from gonorrhea discharge in men?
Gonorrhea discharge tends to be thicker, more copious, and more obviously colored, yellow, green, or white and pus-like. Chlamydia discharge is usually lighter, clearer, and more mucoid. However, the overlap between the two is significant, and co-infection is common. Only a test can tell them apart with certainty.
6. Does chlamydia discharge in men have a smell?
It can. Some men report a mild to unpleasant or musky odor associated with chlamydia discharge, but smell alone is not a reliable indicator of infection. Odor is influenced by hygiene, urine concentration, diet, and the presence of other organisms. A foul smell does not confirm chlamydia, and no smell does not rule it out.
7. When should I test after noticing penile discharge?
If you have discharge alongside a known or possible chlamydia exposure, test at the 14-day mark after that exposure. Testing earlier than 14 days risks a false negative result because the bacterial load may not yet be detectable. If you're seeing discharge but don't know when a possible exposure occurred, test now.
8. Can I have chlamydia discharge without burning when I urinate?
Yes. Discharge and burning urination often appear together, but they don't have to. Some men experience discharge with no urinary discomfort at all. Others get urethral itching or irritation without visible discharge. Symptoms of chlamydia in men vary widely, which is another reason testing matters more than symptom-matching.
9. Is morning discharge always a sign of chlamydia?
Not necessarily. Some men notice small amounts of pre-ejaculate or residual fluid in the morning, this is normal. What's not normal is a cloudy, milky, or foul-smelling discharge that appears at the urethral tip consistently in the morning, especially alongside any burning or itch. If it's new, unusual, or accompanied by other symptoms, get tested.
10. Can I test for chlamydia at home if I have discharge?
Yes, and an at-home test is an entirely appropriate first step. A urine-based NAAT test, the type used by reputable at-home kits, is the current gold standard for detecting chlamydia in men. You don't need a clinic visit, a swab, or a conversation with anyone to get an accurate result. Test from 14 days after exposure for the most reliable outcome.

People are also reading: STD Testing Best Practices for Polyamorous People
Get Tested, Because the Discharge Rarely Tells the Full Story
Whatever you've noticed, a drop of clear fluid in the morning, a cloudier discharge that showed up and then stopped, a vague urethral itch you've been trying to ignore, the one thing that turns uncertainty into clarity is a test. Symptoms are useful signals, but they are not a diagnosis. Chlamydia can look like nothing at all. It can look like something that went away. It can look like something that was probably fine. It very often isn't.
The Chlamydia At-Home STD Test Kit gives you a result from a simple urine sample with 99%+ accuracy, no clinic appointment, no waiting room, no awkward conversation. If you've had any kind of higher-risk exposure or your recent encounters have been with new or untested partners, the Chlamydia & Gonorrhea At-Home STD Test Kit screens for both infections at once, which makes sense, given that the two often travel together. For those who want a more complete picture of their sexual health, the 7-in-1 Complete At-Home STD Test Kit covers chlamydia, gonorrhea, syphilis, HIV, hepatitis B, hepatitis C, and HSV-2 in a single test package.
Testing is the fastest way to stop the guessing game. Visit STD Test Kits to find the right test for your situation, and take control of your sexual health today.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, 2024 National STI Surveillance Data Release
2. NCBI StatPearls, Urethritis: Clinical Review
3. CDC STI Treatment Guidelines, Urethritis and Cervicitis
4. MSD Manual, Chlamydia: Symptoms and Diagnosis
5. MedlinePlus, Chlamydial Infections in Males
6. World Health Organization, Chlamydia Fact Sheet
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.