Last updated: April 2026
Fake health stories spread fast when they tap into real anxieties, and few anxieties are more universal than the quiet worry after an unprotected encounter. The "Houston STD" stories that keep circulating are built on that formula: take something people are already nervous about, attach an extreme or impossible-sounding claim, and publish it without accountability. The stories are fiction. The underlying biology of STD co-infection is not. This article explains exactly how multiple STDs can occur at the same time, which infections most commonly travel together, why they almost always go undetected without proper testing, and how a single at-home session can give you the complete picture.

People are also reading: Do Some STDs Go Away on Their Own? Here's What Really Happens
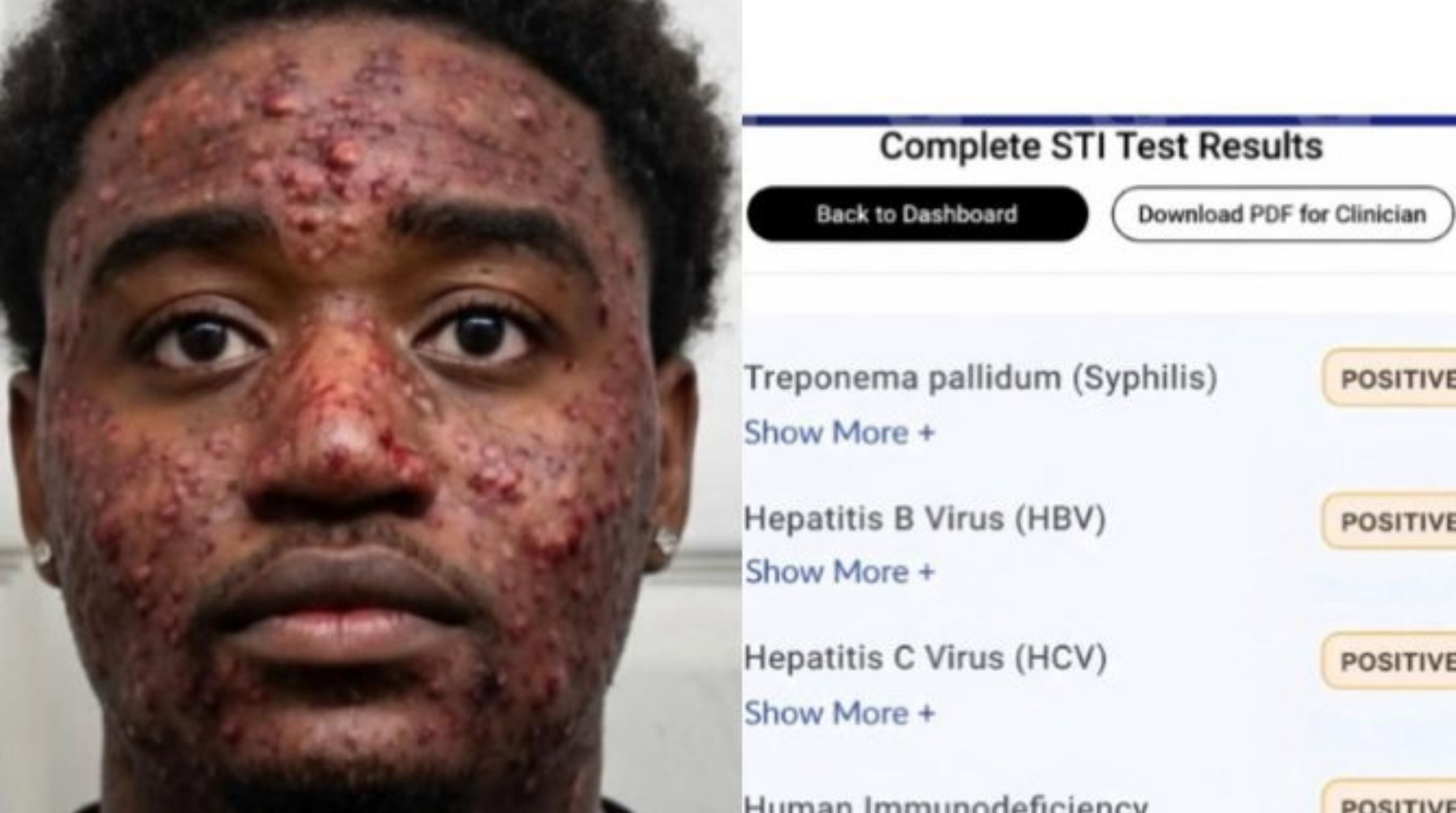
The Houston "Every STD" Story Is Fake, Here's What Actually Happened
The story claiming a man tested positive for every STD after a Houston vacation has no sourcing, no verifiable person, no hospital, and no public health authority has confirmed it. It's fabricated. Stories of this type get manufactured by low-credibility content farms because extreme health claims generate clicks, and STD anxiety is a reliable trigger.
This isn't Houston's first appearance in viral STD fiction. In 2024, posts claimed the city saw 42,000 STD cases during spring break. The Houston Health Department publicly called those numbers "grossly overstated" and launched an investigation into how the misinformation spread. Reuters and PolitiFact both traced the figures to statewide data stripped entirely of context. Our full breakdown of how that happened is here: Did Houston Really Have 42,000 STD Cases This Spring Break?
The pattern is consistent: real concept, impossible framing, no accountability. What's worth taking seriously is not the story, it's the question it accidentally raises. Because yes, co-infection with two or more STDs at the same time is a documented clinical reality, and it's far more common than most people realize.
So Can You Actually Have More Than One STD at Once?
STD co-infection means having two or more sexually transmitted infections simultaneously. It's more common than most people expect; up to 40% of women diagnosed with chlamydia are also co-infected with gonorrhea. Having one STD biologically increases your vulnerability to others, which is why comprehensive testing always outperforms testing for a single infection.
The reason co-infection is possible is straightforward: each STD is caused by a completely different organism, a different bacterium, virus, or parasite. Your body does not become immune to other pathogens just because it's already fighting one. If you're exposed to two during the same encounter, or across different encounters with the same or different partners, both can take hold independently. There is no biological protection mechanism that prevents a second infection from establishing itself alongside a first.
This is not a fringe clinical scenario. Research published through the NIH confirms that the risk factors driving one STD acquisition, unprotected sex, multiple partners, and prior STI history, are identical to the factors driving co-infection. The same exposure that gives you one infection gives you access to everything else that partner might be carrying. And according to the American College of Obstetricians and Gynecologists, co-infection is common enough between chlamydia and gonorrhea specifically that clinicians routinely test for both whenever either is suspected. Among people living with HIV, rates of concurrent bacterial STI co-infection exceed 30%.
Why One STD Makes You Biologically More Vulnerable to Others
The co-infection pattern isn't just about behavior; there are specific biological mechanisms that explain why having one STD increases your risk of acquiring another. Syphilis creates open sores at the infection site. Those sores act as direct entry points for other pathogens, including HIV, that might not have been able to establish infection through intact skin or mucous membranes. Gonorrhea triggers inflammation throughout the genitourinary tract that disrupts the natural barrier function of the mucous membranes, membranes that normally serve as a frontline defense against incoming pathogens.
The result is a compounding effect: an active infection doesn't just coexist with a second infection, it actively lowers the threshold required for that second infection to take hold. This is why clinicians treating any one bacterial STD will almost always screen simultaneously for the others. It's not clinical overcaution. It's a recognition that the presence of one infection changes the biological landscape in ways that make co-infection meaningfully more likely.
It's also worth noting that some STDs can be acquired at multiple sites on the body simultaneously. Chlamydia and gonorrhea can both establish infection in the genitals, rectum, and throat independently, meaning someone who's had oral, vaginal, and anal sex could technically be carrying the same infection in multiple locations, each requiring separate testing to confirm. That's a different scenario from co-infection with two distinct pathogens, but it adds another layer to why single-sample testing often misses the full picture.
Why Co-Infections Almost Always Go Undetected Without Testing
The most dangerous feature of STD co-infection isn't the biology, it's the silence. Most STDs, even severe ones, are frequently asymptomatic. Chlamydia shows no symptoms in roughly 70–80% of women and up to 50% of men who carry it. Gonorrhea can be entirely silent. Hepatitis B can go years without obvious signs. HIV often produces brief flu-like symptoms in early infection that disappear completely for years before the virus causes visible damage.
When two or more infections are present simultaneously, the situation becomes harder to read, not easier. The symptoms of one infection can mask or mimic the symptoms of another. A burning sensation during urination might seem like a straightforward UTI, when in reality, gonorrhea and chlamydia are both present and causing overlapping discomfort through different mechanisms. A skin change in the genital area might be attributed to one infection when another is also active. And because the symptom profiles of many STDs overlap significantly, testing for only one after noticing something off is a common and consequential mistake; the person finds what they were looking for and stops looking.
A positive on one test tells you that the infection is present. It tells you nothing about whether others are also there. If you treat the confirmed infection and walk away, any untreated co-infections continue silently, spreading, causing damage, and remaining entirely unknown until the next test or the next partner who develops symptoms.
How and When to Test for Multiple STDs at Once
The most important thing to understand about multi-STD testing is that timing determines accuracy. Each infection has a window period, the time between exposure and when the test can reliably detect it. Testing inside that window produces false negatives not because the test is wrong, but because the pathogen hasn't yet developed to detectable levels. Testing too early is one of the most common sources of false reassurance.
Once you're past the relevant windows, a comprehensive multi-panel test gives you the complete picture in a single session. The 8-in-1 Complete At-Home STD Test Kit screens for HSV-1, HSV-2, HIV, Hepatitis B, Hepatitis C, Chlamydia, Gonorrhea, and Syphilis, the eight infections most clinically relevant after an unprotected encounter, with over 98% accuracy and results in 15 minutes. Women wanting the most complete picture available can use the Women's 10-in-1 At-Home STD Test Kit, which adds Trichomoniasis and HPV to the panel. Testing comprehensively once is always smarter than testing for one infection at a time over several weeks. Your results, your privacy, your power.
What to Do If One Test Comes Back Positive
A positive result for one infection is information, and it's also a reason to look further, not a reason to stop. A confirmed chlamydia result doesn't rule out gonorrhea or syphilis. A positive gonorrhea test doesn't tell you whether hepatitis B is also present. The biology of co-infection means that finding one is grounds for checking the others, not declaring the full picture complete.
The scenario that plays out when this step gets skipped is quiet and slow-moving: one infection gets treated, cleared, and forgotten. The second infection, still undetected, still asymptomatic, continues. It may affect fertility over time. It may spread to a partner who has no idea. It may lower immune defenses in ways that make future infections easier to acquire. Untreated co-infections don't announce themselves. They just continue.
If any result comes back positive using an at-home test, the next step is confirming with a healthcare provider and beginning treatment. Bacterial infections, chlamydia, gonorrhea, and syphilis are curable. Viral infections like HIV and herpes are manageable with ongoing care, and earlier identification consistently leads to better outcomes. The only thing that makes co-infection worse is the time between exposure and knowing. Take control of your sexual health today. Testing is the fastest way to stop the guessing game.
People are also reading: Blood Transfusions and STDs: Is It Still a Risk Today?
Why the "Every STD at Once" Story Is Still Biologically Implausible
While co-infection with two or three STDs is clinically documented and real, the "tested positive for every single STD" framing of viral posts fails basic biology on several fronts. Different STDs have fundamentally different transmission efficiencies and different transmission routes. Some spread primarily through genital contact; others require blood exposure. Some are transmitted far more easily in one direction than another, and some require repeated or prolonged exposure to establish infection even from an actively infected partner.
The viral version of this story also ignores window periods entirely. Several of the infections that appear in "every STD" posts, herpes and hepatitis, require weeks before detectable antibodies develop. A test taken immediately or within days of an encounter would not accurately reflect their presence, regardless of exposure. The "instant full-panel positive" framing is not how STD testing or STD biology works. What is real: two or three co-infections occurring simultaneously is a genuine clinical phenomenon worth understanding. "Every STD simultaneously, confirmed immediately" is not.
There's also a subtler myth worth addressing here, the idea that once you have one STD, you can't get it again. That's false for all of them. Reinfection is possible with every STD, which is another reason regular testing matters even after a previous positive and confirmed treatment.
FAQs
1. Is it possible to have a positive result for all STDs at the same time, viral post?
No, and it’s not biologically possible. Different STDs have different ways of transmission, different window periods, and different transmission efficiencies. The Houston story is a fraud . What is real is co-infection with two or three STDs at the same time, and this is well-documented and worth understanding.
2. How often do people get more than one STD at the same time?
More common than most people think. As many as 40% of women diagnosed with chlamydia also have gonorrhea. Rates of concurrent bacterial STI co-infection can be >30% in people with HIV. Co-infection is a regular clinical consideration, not an outlier, because if you are biologically infected with one STD, you are more susceptible to infection with others.
3. Can you get more than one STD from a single sexual encounter?
Yeah. If a partner is infected with more than one infection, you may be exposed to several pathogens in a single encounter. Co-infections with different partners can also accumulate over time. Either way, you are at risk for whatever your partner has and your risk of exposure is the same.
4. What happens if I get two STDs at the same time?
Not necessarily, and this is exactly what makes co-infections so dangerous. Many STDs have no symptoms, and for two STDs, symptoms of one STD may mask or mimic symptoms of another. Testing – not waiting to feel something’s wrong – is the only way to know for sure what’s there.
5. Do I have to test for all STDs at the same time, or can I test for one at a time?
It is always better to do the testing thoroughly in one go. A multi-panel test run at the right window period gives you the full picture in one sitting." Just because you test one and it's positive doesn't mean there's nothing else there; it means you found one. The rest is a mystery.
6.What are the most common co-occuring STD’s?
The most common pair would be chlamydia and gonorrhea. They are transmitted in similar ways and often come from the same partner. Men who have sex with men are more likely to have syphilis and gonorrhea at the same time. Bacterial STDs generally co-exist with HIV because the same behaviors and biological vulnerabilities that drive one drive all of them.
7. If I test positive for one STD, should I be tested for others?
Yes. If you find a positive for one infection, that is a reason to dig deeper, not to stop digging. A positive chlamydia result does not rule out gonorrhea or syphilis. Most clinicians recommend testing for the full bacterial panel once any one bacterial STD is confirmed, and a comprehensive at-home multi-panel kit makes that step easy.
8. How long after exposure do I have to wait to be tested for multiple STDs?
Chlamydia 14 days, Gonorrhea 3 weeks, Syphilis 6 weeks HIV 6 weeks, retest at 12 weeks for certainty Herpes HSV-1 HSV-2 6 weeks. Hepatitis B 6 weeks. Hepatitis C 8-11 weeks. Each infection has a window . Testing outside these windows can lead to false negatives even when infection is present.
9. Did you use any real public health data in the Houston STD story?
No. The tale of a man who tested positive for every STD after a Houston vacation is unsubstantiated and has not been confirmed by any public health authority. This is the same pattern as the 2024 “42,000 spring break cases” claim, which both Reuters and PolitiFact debunked as out-of-context, statewide data misrepresented as a one-time spike.
10. Can I test for multiple STDs at home, without going to a clinic?
Yes. At-home multi-panel STD test kits test for multiple infections at the same time, take about 15 minutes per test to get results, and don’t require a visit to the clinic. So if you want the full picture after a possible exposure, the most direct and private way to know exactly where you stand is a comprehensive at-home panel.
Test for All of Them, Not Just One
The Houston story is fiction. The question underneath it is worth taking seriously. STD co-infection is real, it's common enough to be a standard clinical expectation, and it's almost entirely invisible without comprehensive testing. One positive doesn't mean there's only one infection. The only way to know the complete picture is to test for all of them at the right time.
The 8-in-1 Complete At-Home STD Test Kit screens for eight infections at once, HSV-1, HSV-2, Chlamydia, Gonorrhea, Syphilis, HIV, Hepatitis B, and Hepatitis C, with over 98% accuracy and results in 15 minutes. For the most comprehensive panel available, the Women's 10-in-1 At-Home STD Test Kit adds Trichomoniasis and HPV. If you want to start with the bacterial infections most likely to co-occur, the Chlamydia, Gonorrhea & Syphilis At-Home STD Test Kit covers the most common trio. Browse the full range at the STD Test Kits homepage.
Clarity is one test away. Testing is not a confession; it's a responsible health decision, and it's the only thing that actually tells you what's going on.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. American College of Obstetricians and Gynecologists, Chlamydia, Gonorrhea, and Syphilis
2. StatPearls / NIH, Sexually Transmitted Infections
3. PMC, Coinfection and Repeat Bacterial STIs in Male STI Clinic Attendees
4. CDC, Sexually Transmitted Infections Surveillance, 2024 (Provisional)
5. World Health Organization, Sexually Transmitted Infections Fact Sheet
6. Reuters Fact Check, Online Posts Reporting 40,000 Positive STD Tests in Houston Are Misleading
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.