Flu or Early HIV? Symptoms That Show Up First
Last updated: April 2026
Why STD Symptoms Disappear Without the Infection Clearing
Here's the thing about your immune system: it's good at suppressing symptoms, but it's not always good at eliminating the underlying cause. When a bacterial STD like chlamydia or gonorrhea causes noticeable discomfort, burning, discharge, or pressure, that's your immune response in action. And sometimes, that immune response gets strong enough to reduce inflammation and quiet the symptoms down. The bacteria, however, are still there. They've just stopped getting your attention.
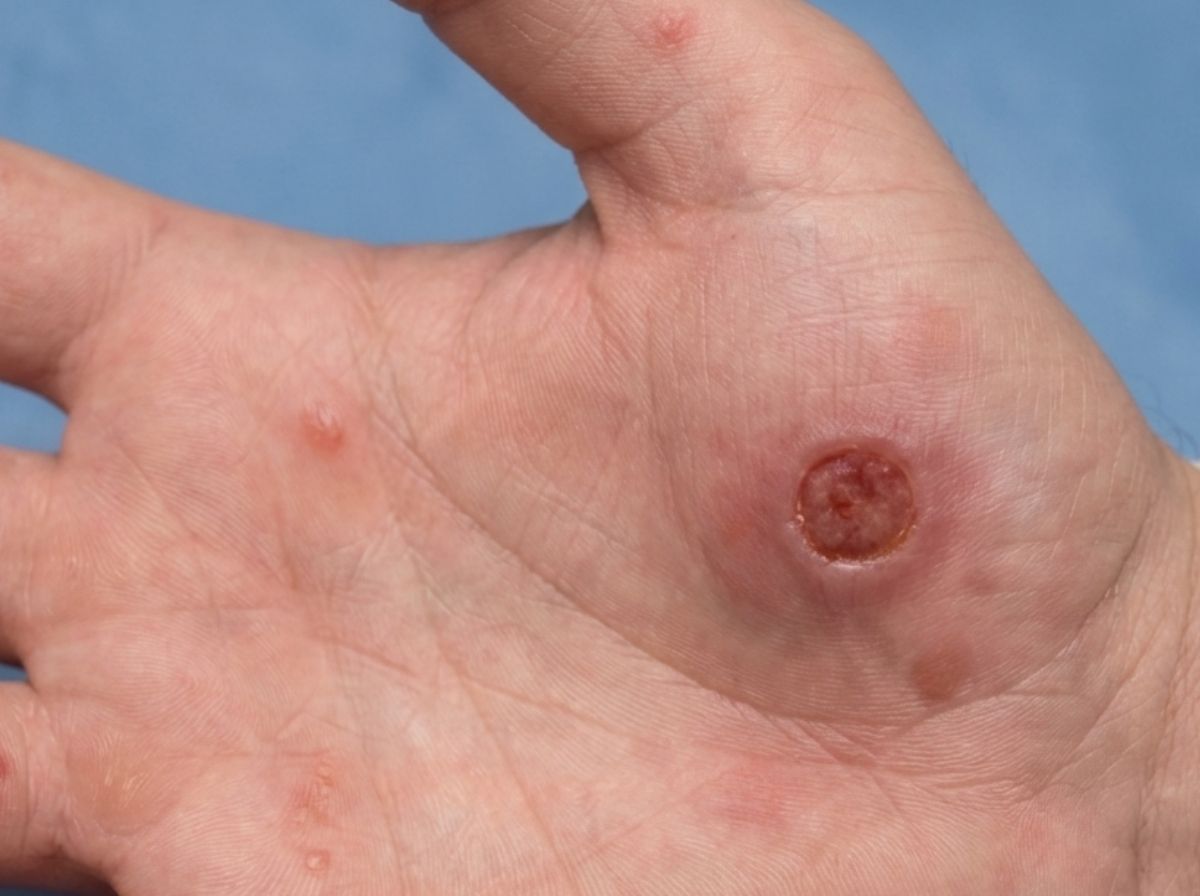
This distinction, between symptom suppression and actual clearance, is one of the most important things to understand about sexual health. Many STDs have what's called a latent phase, a period where the pathogen settles in, stops causing obvious trouble, and continues doing damage or remaining contagious without any warning signs. Syphilis is the clearest example. The first-stage sore (the chancre) heals on its own within a few weeks. Many people interpret that as recovery. It isn't. The bacteria responsible have simply moved deeper into the body and are heading toward the next stage of infection.
The same quiet-but-active pattern plays out with chlamydia, gonorrhea, herpes, and HIV, each in its own biological way. According to the CDC, the majority of STIs produce no symptoms at all in most people who carry them, which means symptom disappearance is often not even a phase; it's the entire experience. You never felt sick. That doesn't mean you were never infected.
People are also reading: STD Testing Window Periods: When to Test for Each
Can Chlamydia Go Away Without Treatment?
Chlamydia is the most reported bacterial STI in the United States, and it's the infection most likely to make people believe they've gotten lucky. The symptoms, if they appear at all, tend to be mild: a slight burning sensation when urinating, some unusual discharge, a vague pressure in the lower abdomen. Then they fade. And because chlamydia is asymptomatic in roughly 70% of women and about half of all men, many people never had symptoms in the first place and assume they're simply in the clear.
In a small number of cases, chlamydia does appear to clear spontaneously, research published in the journal Sexually Transmitted Diseases has observed this in roughly 20% of cases in the interval between screening and treatment, more often in people without signs of active infection. But that leaves the overwhelming majority still infected, often without knowing it. And "cleared naturally" doesn't mean it left without consequence. During the weeks or months before it resolved (if it resolved), the infection was actively silently damaging the reproductive tract and was fully transmissible to any partner.
Left untreated long enough, chlamydia causes pelvic inflammatory disease (PID) in women, which can scar the fallopian tubes and lead to chronic pelvic pain or infertility. In men, it can cause epididymitis, painful inflammation of the tube that carries sperm, and increase the risk of fertility problems. The insidious part is that none of this necessarily announces itself with noticeable symptoms. You can be building up serious internal damage while feeling completely fine. If you've had unprotected sex and there's any chance of exposure, testing from 14 days after that exposure is the only way to actually know where you stand.
Can Gonorrhea Clear Up On Its Own?
Gonorrhea has a reputation as an infection that announces itself loudly, discharge, burning, urgency. And sometimes it does. But it also frequently doesn't, particularly in the throat and rectum, where most infections produce no symptoms whatsoever. Someone can transmit gonorrhea through oral sex for months without any awareness they're carrying it. That's not a rare edge case. It's the typical pattern for pharyngeal gonorrhea.
As for spontaneous clearance: it happens rarely enough that it's not a reasonable thing to count on. Gonorrhea is caused by the bacterium Neisseria gonorrhoeae, which has evolved to evade immune responses effectively, it's one of the reasons it's also developed significant antibiotic resistance over time. Even in cases where symptoms appear to resolve, the infection is overwhelmingly likely to still be present. And untreated gonorrhea progresses. In women, it leads to PID. In men, it causes epididymitis and potential infertility. In both sexes, it can disseminate into the bloodstream and cause septic arthritis, a painful joint infection, if left completely unaddressed.
If you think you might have been exposed to gonorrhea, the testing window is 3 weeks after exposure. It's worth noting that this is one of the infections with a real risk of asymptomatic transmission through routes that people sometimes consider "lower risk", like hand and oral contact in certain situations, so the exposure question is worth thinking through carefully before assuming you weren't at risk.
Does Syphilis Go Away If You Wait It Out?
Syphilis is in a category of its own when it comes to the illusion of self-resolution. Its progression through stages is almost designed to be misread as recovery. The primary stage produces a painless sore, the chancre, that heals on its own within 3 to 6 weeks. No medication required. The sore disappears, and unless you knew what you were looking at, you'd be forgiven for thinking the problem solved itself.
It didn't. The secondary stage follows weeks later: a rash, flu-like symptoms, sores in the mouth or genitals. These also eventually clear without treatment. Then comes the latent stage, which can last for years with zero symptoms while Treponema pallidum, the bacteria responsible, continues to work through the body. Tertiary syphilis, which affects around 15–30% of people who reach the latent stage untreated, causes damage to the heart, brain, nervous system, and major blood vessels. It can be fatal.
This pattern, symptoms appearing, clearing, appearing again, clearing again, is the exact mechanism that makes syphilis so dangerous and so easy to rationalize away. According to CDC surveillance data, congenital syphilis (passed from mother to child) has risen nearly 700% over the past decade, a direct consequence of infections going undetected and untreated in people who felt fine. If there's any chance of syphilis exposure, testing from 6 weeks after exposure is essential, and the disappearance of any symptom is not, under any circumstances, a sign that treatment isn't needed.
Can Viral STDs, Herpes, HIV, HPV, Go Away On Their Own?
This is where the biology changes fundamentally. Bacterial infections like chlamydia and gonorrhea can theoretically be cured because bacteria are separate organisms that can, in some cases, be fought off. Viruses operate differently; they integrate into your cells, sometimes into your DNA itself, and your immune system cannot eradicate them the way it might a bacterium. For herpes and HIV, "going away" is not a thing that happens. Ever.
Herpes (HSV-1 and HSV-2) establishes itself in nerve cells near the base of the spine and lives there permanently. Outbreaks occur when the virus travels back to the skin surface and replicates. Between outbreaks, which can be months or years apart, the virus is dormant in the nerve tissue, not gone. And critically, it can still be shed asymptomatically, meaning it can be transmitted to partners during periods with no visible sores, no itching, no warning at all. Someone who "never has outbreaks" is not necessarily non-infectious.
HIV embeds itself into the DNA of immune cells. Without treatment, the viral load may fluctuate, and early acute symptoms, such as fever, fatigue, rash, may clear within weeks. But HIV itself never clears. It continues depleting CD4 cells slowly and silently until the immune system is compromised enough for AIDS-defining conditions to develop. Testing from 6 weeks after exposure (with a retest at 12 weeks for certainty) is essential after any potential exposure, regardless of whether you felt ill and then felt better.
HPV is the nuanced exception in the viral category. Most people who contract HPV do clear it, their immune systems resolve the infection within one to two years, especially in younger adults. But "most" is not "all," and the strains that don't clear are the ones linked to cervical cancer, penile cancer, anal cancer, and oropharyngeal cancer. You cannot tell which strain you have based on symptoms. Genital warts are caused by low-risk strains; the high-risk cancer-linked strains typically cause no visible symptoms at all. Regular Pap smears and HPV testing remain necessary even if previous HPV has apparently resolved.
People are also reading: STD Risk Checker Quiz: Do You Need to Get Tested?
What About Trichomoniasis and Hepatitis B?
Trichomoniasis, caused by a parasite rather than a bacterium or virus, is worth addressing directly because it's often left out of these conversations despite being one of the most common curable STDs in the United States. The majority of trichomoniasis infections (up to 70–80%) are asymptomatic. When symptoms do occur, itching, burning, unusual discharge, they can come and go in ways that make the infection seem self-limiting. It isn't. Without treatment, trichomoniasis can persist for months or years, increasing susceptibility to other STIs, including HIV, and in pregnant people, it raises the risk of preterm delivery.
Hepatitis B is a more variable situation. Acute hepatitis B, the initial infection, does resolve on its own in most adults with healthy immune systems. Around 95% of adults who contract hep B as adults will clear it within six months. But for the 5% who don't, the infection becomes chronic, leading to progressive liver disease and an elevated risk of liver cancer over decades. Testing from 6 weeks after exposure tells you whether you've been infected; a follow-up test at 3–6 months determines whether your immune system has cleared it or whether you've moved into chronic infection. Sitting and waiting because you feel fine carries real risk in that 5% scenario.
This is also worth remembering when it comes to less obvious routes of exposure. Hepatitis B and hepatitis C, are blood-borne, which means they can be transmitted in contexts that have nothing to do with sex, including unsterilized tattoo or piercing equipment or, historically, blood transfusions. The absence of sexual exposure doesn't rule out the need for testing.
How Long After Exposure Should You Test for Each STD?
You had a symptom. It lasted a few days and then disappeared. Now you're Googling this at midnight, wondering if you needed to do something about it. Here's the honest answer: yes, you probably still need to test. Not because you're definitely infected, but because the only way to actually know is to check.
At-home rapid test kits make this genuinely easy. No clinic, no appointment, no awkward conversation. You test at home, get a result in minutes, and know. The 6-in-1 STD home test kit covers six of the most common infections in a single test: HSV-2, chlamydia, syphilis, HIV, hepatitis B, and hepatitis C, and if you want gonorrhea and herpes 1 included as well, the 7-in-1 complete kit is the one to reach for. Use the exact window periods below; these are the clinically established timings that ensure you're testing when the result will actually be reliable.
If your exposure was recent enough that you're still inside the window period for a given infection, wait until the window has passed before testing, testing too early can produce a false negative, which is exactly the kind of false reassurance you're trying to avoid. Peace of mind is one test away, but timing matters.
Can You Still Infect Someone After Symptoms Disappear?
This is perhaps the most consequential misunderstanding in sexual health: the belief that you're only contagious when you have visible symptoms. It's understandable, it feels logical. But it's wrong for almost every STD on this list.
Herpes is the most studied example of asymptomatic transmission. Viral shedding, the release of infectious virus particles, occurs even during periods of no outbreak, no itching, no visible sores. Research has shown that asymptomatic shedding accounts for a substantial share of all herpes transmissions. Partners who don't know they have herpes often don't know because they've never had a recognizable outbreak, and yet they've been transmitting all along. The same silent-but-infectious dynamic applies to chlamydia and gonorrhea (particularly in the throat or rectum), syphilis in its latent phase, and HIV at all stages without treatment.
This is also worth thinking about in contexts beyond traditional sexual exposure. Someone who contracted hepatitis B or C through a contaminated nail salon tool or at a spa or massage facility with poor hygiene standards may have no symptoms and no obvious sexual exposure history, but they can still transmit the virus to sexual partners. The only thing that interrupts that chain reliably is knowing your status.
The Real Reason People Don't Test (And What It Costs Them)
People don't skip testing because they don't care. They skip it because testing feels like an admission, of something shameful, something risky, something they'd rather not have confirmed. There's a quiet hope that if you don't look, the problem might not exist. But STDs don't operate on the honor system. The 2024 CDC provisional surveillance data reported over 2.2 million cases of chlamydia, gonorrhea, and syphilis in the United States, a figure that is still 13% higher than a decade ago, even as numbers have started to edge downward. The gap between people who are infected and people who know they're infected is substantial, and it's filled almost entirely by people who assumed their bodies handled it.
The cost of that assumption is not abstract. Untreated chlamydia and gonorrhea cause PID in women at a rate that results in thousands of infertility diagnoses every year. Untreated syphilis progresses to neurological and cardiovascular damage. HIV caught late, because someone waited years before testing, requires more intensive treatment and carries a higher risk of complications than HIV caught early. The earlier the diagnosis, the simpler the path forward. That's true for almost every infection on this list, bacterial or viral.
If you've been holding off because testing feels like a big deal, the at-home option removes most of the friction. The 8-in-1 complete STD test kit covers HSV-1, HSV-2, chlamydia, gonorrhea, syphilis, HIV, hepatitis B, and hepatitis C, the full picture, shipped discreetly and read in minutes at home. Testing is not a confession. It's information. And information is what lets you make smart decisions.
FAQs
1. Can chlamydia go away without treatment?
In a small number of cases, roughly 20% over the course of a year, the immune system does appear to clear chlamydia. But that still leaves 80% of people still infected, often without symptoms. And even if you're in that 20%, there's no way to know without testing. The infection can damage the reproductive tract silently in the weeks or months before it potentially clears, and it's fully contagious the entire time.
2. What does it mean when a syphilis sore heals on its own?
It means the first stage of syphilis is progressing as the disease normally does, not that the infection is gone. The primary chancre heals without treatment in 3 to 6 weeks as a standard feature of syphilis biology. The bacteria are still present and moving deeper into the body. Secondary symptoms will follow weeks later, and from there the infection enters a silent latent phase that can last for years while causing internal damage.
3. Can herpes go away permanently?
No. Once HSV-1 or HSV-2 establishes itself in the nerve cells near the spine, it's there for life. The virus enters a dormant state between outbreaks but never leaves the body. Some people have infrequent outbreaks; some people have almost none. That doesn't make them uninfected; it makes them unknowingly infectious, since asymptomatic shedding can occur even during outbreak-free periods.
4. If I feel totally fine, do I really need to test?
Especially then, honestly. Most STDs are asymptomatic in most people most of the time. Chlamydia has no symptoms in around 70% of women and 50% of men. HIV may produce no symptoms after the initial acute phase for years. Feeling fine is not the same as being negative. Testing is the only thing that tells you what's actually happening.
5. Can gonorrhea in the throat clear up on its own?
Pharyngeal gonorrhea is one of the most commonly missed infections precisely because it rarely causes symptoms, a mild sore throat at most, and often nothing at all. Whether it could theoretically self-resolve is less important than the fact that it can be transmitted through oral sex for months without detection. If you've had oral sex with a partner whose status is unknown, the throat is a site worth including in your testing panel.
6. Can you have an STD for years without knowing?
Absolutely, and it's more common than most people realize. HIV can be present for a decade or more without obvious symptoms in people who aren't on treatment. Latent syphilis can sit quiet for years. Chronic hepatitis B and C can take decades to produce signs of liver damage. This is why routine testing matters even when you're feeling well and have no specific concern.
7. If my partner tested negative, does that mean I'm also negative?
Not automatically, for two reasons. First, if your partner tested before the window period had passed, their result may be a false negative. Second, some infections, like HSV-1, are extremely common and not always included in standard panels. Both partners testing, using accurate kits, within the correct window periods, is the only reliable picture of shared sexual health status.
8. Can HPV go away on its own and then come back?
This is a genuinely important question. HPV that has been cleared by the immune system doesn't typically reactivate, but you can be reinfected with a different strain through new exposure. The HPV strains that cause genital warts are different from the high-risk strains that cause cancer, and you can carry multiple strains simultaneously. Clearing one strain doesn't mean you're clear of all strains.
9. How long after unprotected sex should I wait before testing?
It depends on the infection. Chlamydia: 14 days. Gonorrhea: 3 weeks. Syphilis, herpes, and hepatitis B: 6 weeks. HIV: 6 weeks for a first indicator, 12 weeks for certainty. Hepatitis C: 8 to 11 weeks. Testing before these windows have passed risks a false negative, which can give false reassurance. If you're within the window, mark the date and test when you're through it.
10. Is it possible to get the same STD twice?
Yes, with the exception of some viral infections where immune memory plays a stronger role. Chlamydia and gonorrhea confer no lasting immunity, so reinfection from a new or untreated partner is common. Research has found that reinfection rates for chlamydia can be as high as 26% within the first few months of treatment, typically from partners who weren't treated at the same time. This is why both partners treating simultaneously matters.
Take Control, Know Your Status
Symptoms clearing doesn't mean the infection cleared. Feeling fine doesn't mean you're negative. The only real answer to "do I have an STD?" is a test result, not how you feel, not how long it's been, not whether your last partner seemed healthy. The good news is that testing doesn't require a clinic visit or an uncomfortable appointment. You can do it from home, in private, with results in minutes.
If you want broad coverage in a single test, the 6-in-1 STD home test kit covers HSV-2, chlamydia, syphilis, HIV, hepatitis B, and hepatitis C. For complete coverage including gonorrhea, the 7-in-1 complete STD test kit adds gonorrhea to the panel. And if you want the most comprehensive single-session picture available, including both HSV-1 and HSV-2, the 8-in-1 complete STD test kit has you covered. All kits ship discreetly and give you results without leaving home.
Your results are yours. Testing doesn't define you, it informs you. And being informed is what protects both you and the people you're close to. Visit STD Test Kits to browse the full range and find the test that fits your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. About Sexually Transmitted Infections (STIs), CDC
2. Sexually Transmitted Infections Surveillance, 2024 (Provisional), CDC
3. About Genital HPV Infection, CDC
4. Will STDs Go Away On Their Own?, Planned Parenthood Advocates of Arizona
5. CDC Releases 2024 National STI Data, HIV.gov
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: Rapid STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.







