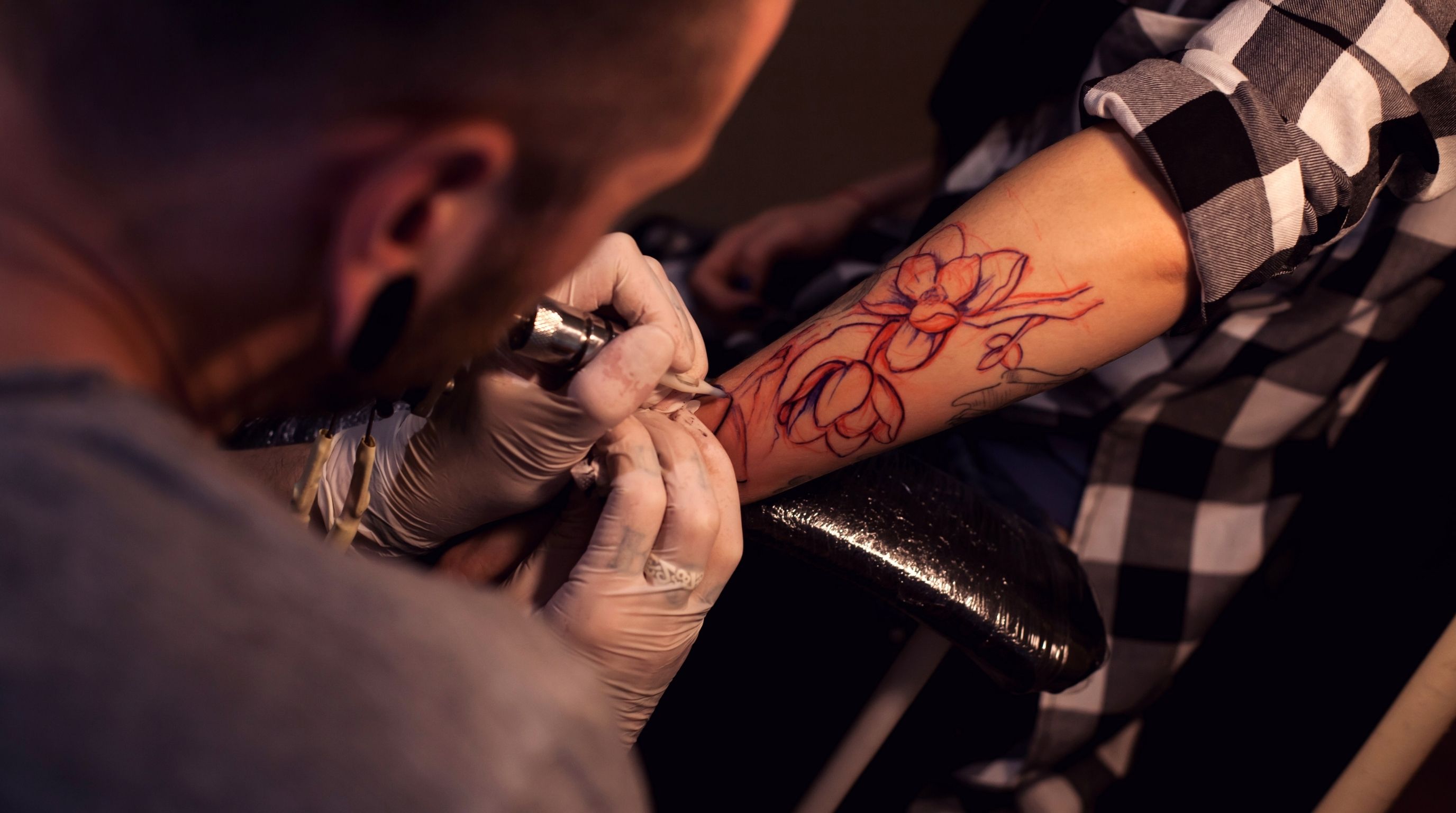Last updated: April 2026
Tattoos and piercings both involve breaking the skin, which means blood is involved, which means bloodborne infections are theoretically in play. But "theoretically possible" and "likely" are very different things, and most articles on this topic conflate them in ways that create unnecessary panic. The infections worth actually understanding here are hepatitis B, hepatitis C, HIV, and, depending on the type of piercing, herpes, HPV, chlamydia, and gonorrhea. Understanding exactly how each one transmits through body art, and under what conditions, gives you a much cleaner picture of your real risk from tattoos and piercings than any vague warning about "dirty needles" or recycled common STD myths.
There's also a category difference between tattoo STD risk and piercing STD risk that most people miss entirely. Tattoos carry a bloodborne transmission risk that's almost entirely about needle and ink hygiene. Piercings carry that same bloodborne risk, but oral and genital piercings introduce a second, distinct risk profile involving skin contact and sexually transmitted infections that a standard bloodborne warning doesn't cover. The STD you need to worry about after a tongue piercing is not the same one you need to worry about after a back tattoo. Both deserve their own honest treatment.
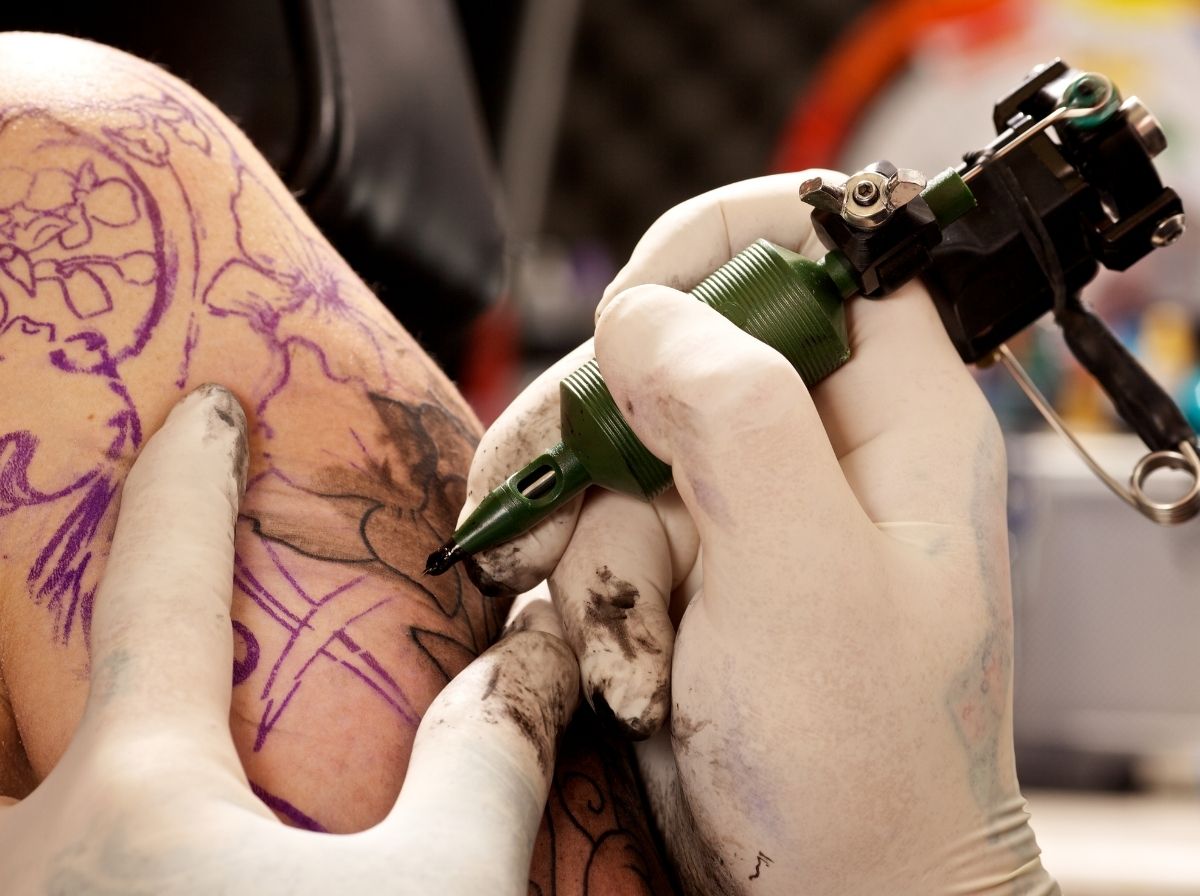
People are also reading: The Least Dangerous STDs: Which Ones Are Easily Treatable?
How do tattoos and piercings actually create STD risk?
To understand the risk, it helps to understand the mechanics. A tattoo machine drives a needle, or cluster of needles, in and out of the skin anywhere from 50 to 3,000 times per minute, pushing ink into the dermis layer just below the surface. Every one of those punctures is a micro-injury that draws blood. If that needle carried trace amounts of blood from a previous client, or if the ink was contaminated, those pathogens now have a direct route into your bloodstream. That's the core mechanism, and it's why needle sterilization is the single most important safety factor in a tattoo environment.
Piercings work differently but create the same core risk. A piercing needle punctures through tissue, sometimes highly vascularized tissue like the tongue, genitals, or cartilage, and leaves an open wound that takes weeks to months to fully heal. The risk of bloodborne transmission occurs at the moment of piercing if the equipment isn't sterile. But piercings also create a secondary, ongoing risk during the healing window: an open wound in or near an area where sexual activity happens is a more accessible entry point for infections than intact skin.
The key variable in both cases is sterilization. At a licensed professional studio, needles are single-use and disposed of after each client, ink is poured into individual cups (never double-dipped from a shared container), and surfaces are sanitized between clients. This is the standard that eliminates most of the risk. The risk profile looks dramatically different in non-professional settings, home tattoos, prison tattoos, and informal piercings done with shared equipment, where none of those safeguards are consistently in place. That same shared-tool logic is why people also ask whether a nail salon can spread an STD or hepatitis; the real issue is not the setting, but whether blood-contaminated tools can contact broken skin.
Can you get hepatitis from a tattoo or piercing?
Here's what the research actually shows about professional studios: the same NCBI review found no definitive evidence of increased hepatitis C risk when tattoos or piercings were received at professional parlors following proper sterilization protocols. The elevated risk, with adjusted odds ratios of 2.0 to 3.6, appeared specifically in prison settings, home tattoos applied by friends, and other non-professional environments. This is a meaningful distinction. Going to a licensed studio dramatically changes your risk profile compared to getting inked by a friend with a kit they ordered online.
The contaminated ink angle is also worth knowing about in detail, because it's one that genuinely surprises people, and it's a real documented transmission route that most "tattoo STD risk" articles skip entirely. Even if a tattoo needle is sterile and single-use, if an artist dips a used needle back into a shared ink pot between passes on your skin, which should never happen but does in unregulated settings, that ink becomes contaminated with your blood. If the same pot is then used on another client, or if that ink had already been contaminated by a previous client, you now have a bloodborne transmission pathway that bypassed the needle sterilization entirely.
Imagine this: you're watching an artist work, and you notice the needle going into an ink bottle that's sitting on the counter rather than into a small individual cup poured fresh for your session. That's the moment to say something, or to leave. Reputable studios pour ink into individual single-use cups for each client and dispose of anything left over after the session. Unused ink from your cup never goes back into the main bottle. If a studio doesn't follow this protocol, the needle sterilization becomes largely irrelevant because the ink itself can carry infection between clients. This is especially true for hepatitis C, which, as noted, can survive on surfaces for up to six weeks and doesn't require visible blood to be transmissible.
Hepatitis B and hepatitis C are the infections most legitimately associated with tattoos and piercings, and for good reason. Both viruses live in the blood, both can survive on surfaces outside the body for meaningful periods of time, and both have documented transmission pathways through contaminated needles. The difference between them, and the reason hepatitis C is the more discussed concern, comes down to survivability. A critical review of hepatitis C transmission through tattooing and piercing published in NCBI found that HCV can remain infectious on surfaces for up to six weeks, which is far longer than HIV, and long enough to make contaminated equipment a genuine transmission route even when no visible blood is present.
Hepatitis B survives on surfaces for up to seven days outside the body and is significantly more infectious per exposure than hepatitis C. A single needlestick from an infected person carries roughly a 5–30% transmission risk for hepatitis B, compared to 3–7% for hepatitis C and 0.2–0.4% for HIV. This is why hepatitis B vaccination is strongly recommended for anyone engaging in activities that involve potential blood contact, including body art. If you haven't been vaccinated against hepatitis B, that's the most straightforward protective step you can take before getting tattooed or pierced. This blood-route distinction also explains why modern blood transfusion STD risk is evaluated through screening systems and blood safety protocols, not through the same risk lens as informal tattooing.
Can you get HIV from a tattoo or piercing?
This is the question most people are actually asking when they Google this topic, and the answer deserves to be clear: the CDC states there are no known confirmed cases of HIV transmission through tattooing or body piercing. That doesn't mean it's biologically impossible, it means the conditions required for transmission are specific enough that it hasn't been documented to occur in practice, even though millions of people get tattooed and pierced every year.
HIV is far less stable outside the body than hepatitis B or C. Exposed to air, it becomes mostly inactive within hours. The virus also requires a very specific entry route, direct contact between infected fluid and a mucous membrane or open wound in the bloodstream. A tattoo needle that was used on an HIV-positive person and then used again without sterilization would theoretically create this pathway, but the viral load on a needle diminishes rapidly with air exposure. The risk is not zero in theory, but it is negligible in practice, and essentially zero at a professional studio using single-use needles. This is the same biology that gets lost when viral posts argue about HIV and nail salons: HIV risk depends on a viable blood-to-blood or mucous membrane route, not just the existence of tools near skin.
Where the risk becomes more real is in settings where needles are genuinely shared and reused repeatedly without any sterilization, such as certain prison environments or informal tattooing. Even there, the per-exposure HIV risk from a contaminated needle is far lower than from sharing IV drug equipment, which is a far more efficient transmission route. The takeaway: HIV from a tattoo or piercing is a theoretical risk that responsible studio practice eliminates almost entirely.
What about oral piercings, tongue, lip, and cheek?
Oral piercings deserve their own section because they introduce a risk dimension that bloodborne warnings alone don't capture. The mouth is one of the most bacteria-rich environments in the human body, which creates local infection risks, but more relevant to this article is the role oral piercings play in STD transmission during sexual activity. A tongue piercing, lip ring, or cheek piercing creates an open wound in tissue that frequently comes into contact with another person's genitals, mucous membranes, and bodily fluids during oral sex. That changes the transmission picture considerably.
Herpes (HSV-1) is the infection most directly relevant to oral piercings. HSV-1, the strain responsible for cold sores, spreads through direct contact with infected oral tissue. A fresh or healing oral piercing represents broken skin in a high-contact area, which creates a more accessible entry point for the virus during any oral contact. There is documented evidence of HSV transmission associated with oral piercings, including a case report in NCBI describing a fatal HSV infection in a previously healthy young woman following a tongue piercing. While this extreme outcome is exceedingly rare, it illustrates that oral piercings are not infection-neutral when it comes to herpes.
Beyond herpes, oral piercings also carry a general elevation in STD transmission risk during the healing period, typically defined as the first six weeks after the procedure. Brown University's sexual health guidance notes explicitly that STD risk during oral sex is increased during the six weeks following any oral or genital piercing, because the healing wound creates a more efficient entry point for pathogens. If you've recently had a tongue, lip, or cheek piercing and you're sexually active, this is the window where extra caution makes the most practical difference.
HPV is also worth mentioning in the context of oral piercings. HPV spreads through skin-to-skin contact, and oral HPV, linked to throat and oropharyngeal cancers, is transmitted through oral sex. A healing oral piercing doesn't directly cause HPV infection, but it does lower the biological barrier to transmission during oral contact. The practical implication: avoid oral sex during the healing period of any oral piercing, or use a barrier method throughout that window.
What about genital piercings?
Genital piercings are the category most people don't think to ask about, which is ironic, because they carry the most directly STD-relevant risk profile of any piercing type. An NCBI review of body piercing infections notes specifically that individuals with genital piercings are at increased risk for gonorrhea and chlamydia, not because the piercing needle transmits them, but because a healing genital piercing compromises the integrity of the tissue barrier during sexual activity, creating easier transmission routes for these bacterial infections.
A healing genital piercing is essentially an open wound in exactly the place where STD-transmitting fluids and skin contact occur during sex. The wound disrupts the protective function of intact skin and mucous membranes that would otherwise slow transmission. During the healing period, which can range from a few weeks for surface piercings to several months for deeper genital piercings, unprotected sexual activity carries an elevated transmission risk for chlamydia, gonorrhea, herpes, and syphilis compared to sex without a healing wound present.
Additionally, genital piercings can compromise the integrity of condoms during sex, and jewelry can catch on or puncture latex, creating gaps in barrier protection. This is a practical concern that goes beyond STD transmission from the piercing itself but is directly relevant to STD risk for people with genital piercings who are sexually active during the healing period. The standard guidance from piercing professionals is to abstain from sexual activity entirely until healing is complete, and to use condoms once you resume.
Should you get tested after a tattoo or piercing?
If you got your tattoo or piercing at a licensed professional studio using single-use needles and standard sterilization protocols, routine STD testing, specifically because of the procedure is not medically necessary. The risk profile at a reputable studio is low enough that a test three days after getting inked isn't going to tell you anything useful, except possibly that your anxiety is running the show.
The situations where testing after body art is genuinely warranted: you got a tattoo or piercing in a non-professional setting, a friend's house, a prison, or an informal setting where sterilization was uncertain or absent. You got an oral or genital piercing and subsequently had unprotected sexual activity during the healing window. You noticed signs of local infection at the piercing or tattoo site that aren't resolving normally. You simply haven't tested recently and you're sexually active, in which case any moment of reflection is a reasonable prompt to get a baseline panel.
The most relevant infections to test for after potential body art exposure are hepatitis B, hepatitis C, and HIV, the classic bloodborne trio. For oral or genital piercings with sexual activity during healing, add herpes, chlamydia, gonorrhea, and syphilis to the list. The 8-in-1 Complete At-Home STD Test Kit covers HSV-1, HSV-2, chlamydia, gonorrhea, syphilis, HIV, hepatitis B, and hepatitis C, the full relevant picture for either scenario, handled privately at home without a clinic visit. If you're worried one exposure could involve more than one infection, this guide to whether you can test positive for multiple STDs at the same time explains why a full panel is sometimes more practical than guessing one infection at a time.

People are also reading: How Often Should You Get Tested for STDs?
When should you test after a tattoo or piercing, exact timing by infection
Timing matters enormously with STD testing, and testing too early is one of the most common mistakes people make. Every infection has a window period, the gap between exposure and when a test can reliably detect it. A negative result before the window closes tells you almost nothing. Here are the exact timelines for each infection relevant to body art exposure.
For hepatitis B, test from 6 weeks after exposure, this is when antibodies have typically developed to detectable levels. For hepatitis C, wait 8–11 weeks after exposure for reliable detection. For HIV, test at 6 weeks for a first indicator, then retest at 12 weeks for certainty. For herpes (HSV-1 and HSV-2), testing from 6 weeks after exposure, the antibody test needs this window to produce reliable results. For syphilis, test from 6 weeks after potential exposure. For chlamydia, test from 14 days after exposure. For gonorrhea, test 3 weeks after exposure.
If you're primarily concerned about the bloodborne infections, hepatitis B, hepatitis C, and HIV, after a tattoo or non-genital piercing, the 8–11 week mark covers all three windows cleanly in a single test. The Hepatitis B & C At-Home STD Test Kit is a targeted option if that's your specific concern, while the full 8-in-1 kit covers everything in one go for broader peace of mind.
How do you know if a tattoo or piercing studio is actually safe?
You're about to let someone break your skin hundreds or thousands of times with a needle. That earns five minutes of research before you book. The good news is that the signals of a safe studio versus a risky one are not subtle; you just need to know what you're looking for before you walk in, rather than noticing problems after the fact.
Start with licensing. Most US states regulate tattoo and piercing studios, though the specifics vary dramatically. Nevada has no regulation of tattoo or piercing shops at all, while states like New Jersey impose explicit sterilization and sanitation requirements. There is no federal standard that applies everywhere. Checking your state's requirements and confirming the studio holds current licensing costs five minutes online and is worth doing. The Association of Professional Piercers (APP) and the Alliance for Professional Tattooists (APT) are both CDC-approved organizations with searchable directories of vetted studios. If a studio isn't willing to tell you its licensing status, that tells you something.
When you actually walk into the studio, look for an autoclave, the heat-and-pressure sterilization device that kills bloodborne pathogens on reusable equipment. It looks like a small industrial oven and should be visible in or near the workspace, not hidden in a back room. Ask if you can see it. Ask when it was last tested. Reputable studios will not be offended by this question; they get it regularly from informed clients and they're proud of their protocols. A studio that bristles at the question is a studio that hasn't thought carefully about the question.
Watch the setup process carefully. Before the needle touches your skin, you should see the artist open a new sterile needle package in front of you, pour fresh ink from a main bottle into a small individual cup just for your session, put on new gloves, and wipe down the work surface. These are not optional extras at a premium studio; they are the baseline that a responsible studio follows for every single client, every single time. If you see the artist dip a used needle into an ink bottle, reach for a needle that was already sitting open on the counter, or skip the individual ink cup and work directly from a shared bottle, those are red flags significant enough to stop the session.
For piercings specifically, the piercing gun question is one of the most important practical distinctions to understand before you book. Piercing guns, the spring-loaded devices used at mall kiosks and some low-cost studios, cannot be fully sterilized between clients because their plastic components cannot withstand autoclave temperatures. This makes them a meaningfully higher infection risk than the single-use hollow needles that professional piercers use. The Association of Professional Piercers explicitly recommends against piercing guns for this reason. If a studio offers piercing by gun rather than needle for anything beyond a basic earlobe, that's worth knowing before you sit down, not after.
One more thing that separates professional studios from informal settings: aftercare instructions. A studio that takes infection risk seriously gives detailed written aftercare guidance because they understand that the healing period carries its own set of risks. If you walk out of a studio with a new tattoo or piercing and the artist's only guidance was "keep it clean," that's a signal about the overall standard of care at that studio.

People are also reading: I Think I Saw a Chancre, What Should I Do?
What symptoms should you watch for after a tattoo or piercing?
Some redness, swelling, and tenderness around a new tattoo or piercing in the first 48–72 hours is completely normal, it's your body doing exactly what it's supposed to do in response to an intentional wound. The signs that something has actually gone wrong are different in character and trajectory: redness that increases rather than decreases after the first few days, warmth that spreads noticeably beyond the immediate site, pus or unusual discharge with an odor, a fever, or a rash radiating outward from the area. These point to a localized bacterial infection that needs medical attention; they are distinct from and should not be confused with the systemic signs of bloodborne infection.
The challenge with bloodborne infections, hepatitis B, hepatitis C, and HIV, is that they rarely announce themselves with symptoms you'd immediately connect to a recent tattoo or piercing. You can be infected for weeks, months, or in the case of hepatitis C, years before noticing anything wrong. This is precisely what makes them dangerous, and precisely why testing at the correct window period matters far more than waiting to feel sick. If an acute hepatitis infection does produce early symptoms, they typically include fatigue that feels disproportionate to what's going on in your life, nausea, loss of appetite, and sometimes jaundice, a yellowing of the skin or whites of the eyes that is hard to miss once you know to look for it. For hepatitis C, these acute symptoms typically appear 2–12 weeks after exposure if they appear at all. For hepatitis B, slightly earlier. For most people, they don't appear at all, which is the whole problem.
Picture this: it's six weeks after you got a tattoo at a studio you weren't entirely sure about, you feel vaguely tired and off, and you can't connect it to anything specific. That's not a definitive sign of hepatitis; fatigue has a thousand causes. But it is a reason to test rather than wait. You're in the window where hepatitis B and HIV are reliably detectable, and another two to five weeks gets you into reliable hepatitis C detection territory. A test gives you a real answer. Feeling tired and refreshing your WebMD tab every hour does not.
For herpes following an oral or genital piercing with sexual activity during healing, watch for tingling, itching, or small fluid-filled blisters appearing at or near the piercing site, or on the mouth or genitals, within 2–20 days of relevant contact. A new outbreak in this location and timeframe warrants evaluation, both to confirm what it is and to make sure you're not unknowingly passing it to a partner before you have answers.
FAQs
1. Is it possible to get hepatitis C from a tattoo needle?
Yes, but the risk depends heavily on where you got the tattoo. Hepatitis C can survive on surfaces for up to six weeks, which is long enough for contaminated equipment to transmit it even without visible blood present. The NCBI critical review on this topic found elevated odds ratios of 2.0–3.6 for HCV infection, but that risk was concentrated in prison tattoos, home tattoos, and informal settings, not licensed professional studios using single-use needles and individual ink cups. At a reputable studio following standard sterilization protocols, the evidence does not support an elevated hepatitis C risk compared to the general population.
2. Is it possible to contract HIV from a tattoo or piercing?
According to the CDC, there are no known confirmed cases of HIV transmission through tattooing or body piercing. HIV is considerably less stable outside the body than hepatitis — it becomes largely inactive within hours of air exposure, which dramatically limits its ability to persist on equipment between clients. The theoretical pathway exists if needles are shared and reused without sterilization, but in professional studios using single-use needles, the risk is negligible. Even in informal settings, HIV transmission through body art is far less efficient than through shared IV drug equipment, and has not been documented to occur in practice.
3. Is there a chance of getting an STD from a tongue piercing?
Yes, through two distinct mechanisms that are worth understanding separately. The first is equipment-based: contaminated piercing tools can transmit hepatitis B, hepatitis C, or herpes at the moment of the procedure, the same bloodborne risk that applies to any piercing. The second is more specific to oral piercings and more relevant to most people's actual risk: a healing tongue piercing is an open wound in tissue that comes into direct contact with genitals during oral sex. That compromised barrier raises the transmission risk for herpes HSV-1, HPV, gonorrhea, and other infections during the healing window — typically around six weeks. The standard guidance from professional piercers is to avoid oral sex entirely during that period, or to use barrier methods throughout.
4. Is it possible to get chlamydia or gonorrhea from a genital piercing?
Not from the needle itself — chlamydia and gonorrhea are bacterial infections that don't survive on piercing equipment the way bloodborne viruses do. The risk comes from what happens during the healing period. A healing genital piercing is an open wound in exactly the area where STD-transmitting fluids and skin contact occur during sex, and that compromised tissue barrier makes it significantly easier for chlamydia, gonorrhea, herpes, and syphilis to establish infection compared to intact skin. The NCBI review of body piercing infections specifically identifies elevated gonorrhea and chlamydia risk in people with genital piercings. That elevated risk persists throughout the healing window, which can be several weeks to months depending on the piercing type.
5. How long should I wait to get tested for hepatitis after getting a tattoo?
For hepatitis B, test from 6 weeks after the procedure — that's when antibodies have typically developed to a reliably detectable level. For hepatitis C, wait 8 to 11 weeks, because HCV antibody development takes longer and testing before 8 weeks carries a real risk of a false negative. A negative result two weeks after getting a tattoo is essentially meaningless — it tells you the infection hadn't reached detectable levels yet, not that it isn't present. If you're going to test, test at the right window so the result actually means something.
6. Is a piercing gun safe, or does it spread germs?
Piercing guns are a meaningfully higher infection risk than the single-use hollow needles that professional piercers use, and the reason is straightforward: piercing guns contain plastic components that cannot withstand autoclave temperatures, which means they cannot be fully sterilized between clients. The Association of Professional Piercers explicitly recommends against piercing guns for this reason. Reputable professional piercers use single-use, sterile, hollow needles — a new one opened from sealed packaging in front of you for each procedure. If a studio offers a gun instead of a needle for anything beyond a basic earlobe, that's a reason to find a different studio.
7. What is the difference between the risk of getting an STD from a tattoo and the risk of getting one from a piercing?
Tattoo risk is almost entirely bloodborne — hepatitis B, hepatitis C, and HIV through contaminated needles or ink. Piercing carries that same bloodborne risk at the moment of the procedure, but oral and genital piercings introduce a second, distinct risk profile that tattoos don't share. A healing oral or genital piercing is an open wound in a location where sexual activity happens, which compromises the tissue barrier that would otherwise slow transmission of skin-contact and fluid-transmitted infections like herpes, HPV, chlamydia, gonorrhea, and syphilis. The infection you need to think about after a tongue piercing is not the same one you need to think about after a back tattoo — both deserve their own honest assessment.
8. If I have herpes, can I get a tattoo or a piercing?
You can, but timing matters. Getting a tattoo or piercing during an active herpes outbreak is a bad idea for two reasons: the physical stress of the procedure and the resulting open wound can trigger a worsening of the active outbreak, and the procedure introduces a new wound that is more vulnerable to secondary infection while your immune system is already occupied. Professional piercers and tattoo artists typically advise waiting until an active outbreak has fully resolved — and ideally a few weeks beyond that — before booking. For oral piercings specifically, any active cold sore in or around the mouth is a reason to postpone, because the procedure creates conditions that make transmission to the artist or to the fresh wound more likely.
9. Do professional tattoo studios actually prevent STD transmission?
Yes, when standard protocols are followed correctly. The combination of single-use needles opened in front of the client, fresh ink poured into individual cups for each session, autoclave sterilization of any reusable equipment, glove changes between clients, and surface sanitation between appointments works together to eliminate the bloodborne transmission pathways for hepatitis B, hepatitis C, and HIV. The research backs this up directly: the elevated hepatitis C risk documented in studies is concentrated in informal and prison settings, not in licensed professional studios. A reputable studio operating to professional standards is not a meaningful STD risk — the risk profile that drives those statistics comes from settings where none of those safeguards exist.
10. Should I get tested for STDs after getting a tattoo at a licensed studio?
If the studio was licensed, used single-use needles, and followed standard sterilization protocols, there is no specific medical reason to test because of the tattoo itself — the risk at a reputable professional studio is low enough that targeted post-procedure testing isn't clinically indicated. That said, if you have any doubt about the studio's practices — you didn't see the needle opened from a sealed package, the ink came from a shared bottle rather than an individual cup, or anything else felt off — testing for hepatitis B, hepatitis C, and HIV at the correct windows makes sense. And if you're sexually active and haven't tested recently, any moment of reflection about your health is a reasonable prompt to run a general STI panel. The tattoo doesn't have to be the reason — it can just be the occasion.
Get Tested After a Tattoo or Piercing, Privately, at Home
If your tattoo or piercing happened in a non-professional setting, if you had sexual activity during a healing oral or genital piercing, or if you simply want confirmation that you're clear, at-home testing gives you accurate results without a clinic visit. The 8-in-1 Complete At-Home STD Test Kit covers HSV-1, HSV-2, chlamydia, gonorrhea, syphilis, HIV, hepatitis B, and hepatitis C, the complete picture for both bloodborne and sexual transmission risks in a single discreet kit.
If your concern is specifically the bloodborne trio after a tattoo or non-genital piercing, the Hepatitis B & C At-Home STD Test Kit is a focused option, accurate and ready to use at the 8–11 week mark when hepatitis C detection is reliable. For anyone who had a healing oral or genital piercing during sexual activity, the full 8-in-1 kit covers every relevant infection in one go.
Testing is how you get a clear answer instead of a running anxiety loop. Visit STD Test Kits to find the right test for your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. NCBI, Transmission of Hepatitis C Virus Through Tattooing and Piercing: A Critical Review
3. NCBI, Body Piercing Infections (StatPearls)
4. Hepatitis B Foundation, Know the Risk: Transmission Through Tattoos and Piercings
5. NCBI, Fatal Fulminant Herpes Simplex Hepatitis Secondary to Tongue Piercing
6. NCBI, Oral and Perioral Piercing Complications
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.