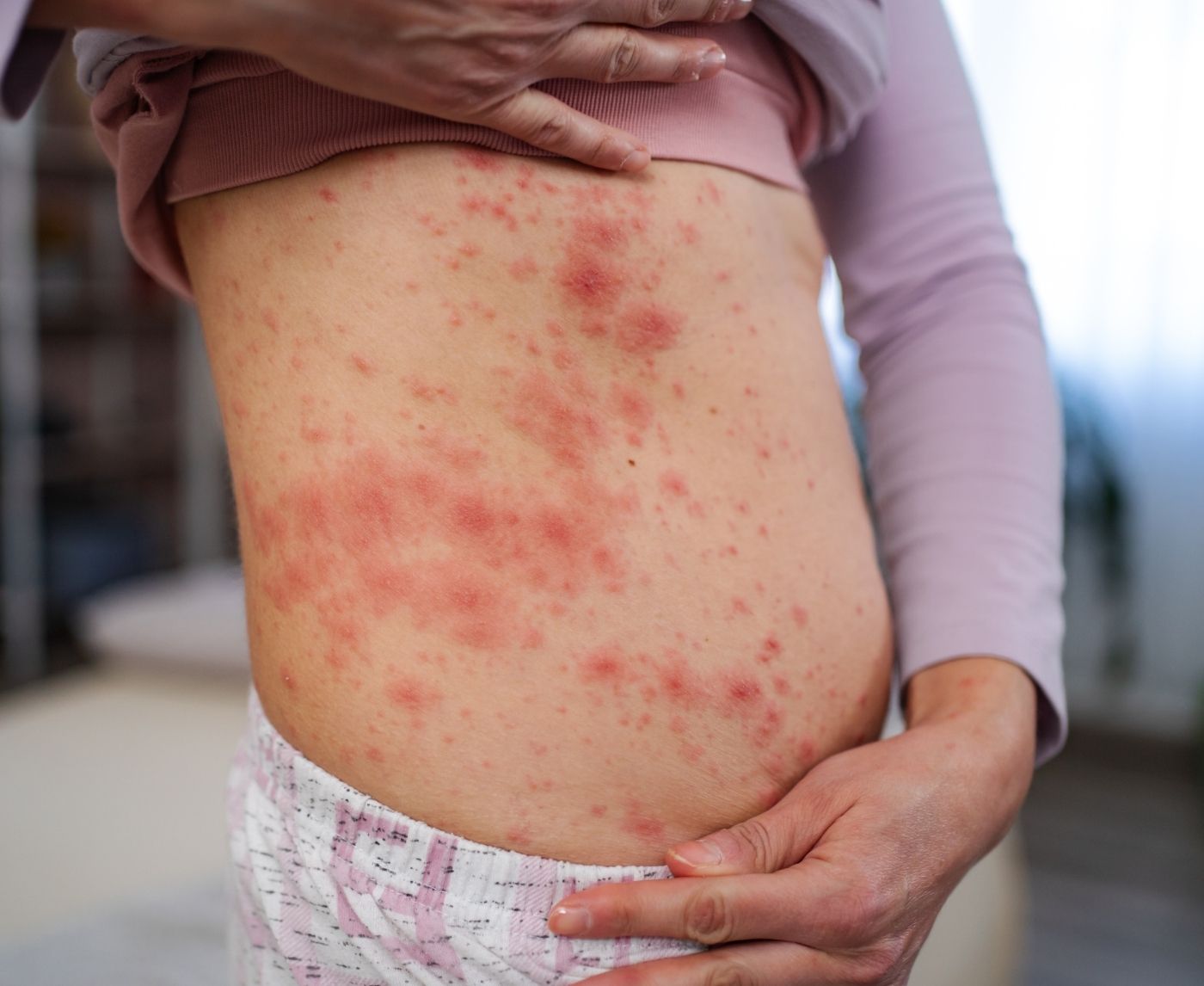
One Night Stand STD Risk: What Should You Actually Test For?
Quick Answer: A rash after sex is usually caused by friction, irritation, or an allergic reaction, not an STD. However, if the rash persists, spreads, becomes painful, or is paired with sores, discharge, or flu-like symptoms, testing is recommended.
First, Let’s Slow the Panic
When people search “rash after sex,” they’re rarely calm. They’re sitting on the edge of the bed replaying the night. Maybe the condom broke. Maybe it was rougher than usual. Maybe it was someone new. The body becomes evidence. Every red spot feels like a verdict.
Here’s the grounded truth: skin reacts. Genitals are sensitive. Friction alone can cause redness, especially if there wasn’t enough lubrication. Add sweat, latex, body wash residue, shaving stubble, or semen exposure, and the skin can flare quickly.
Dr. F. David, MD, often tells patients, “Skin irritation can show up within minutes. Most STDs do not.” That timing matters. Immediate redness is more likely mechanical or allergic than infectious.
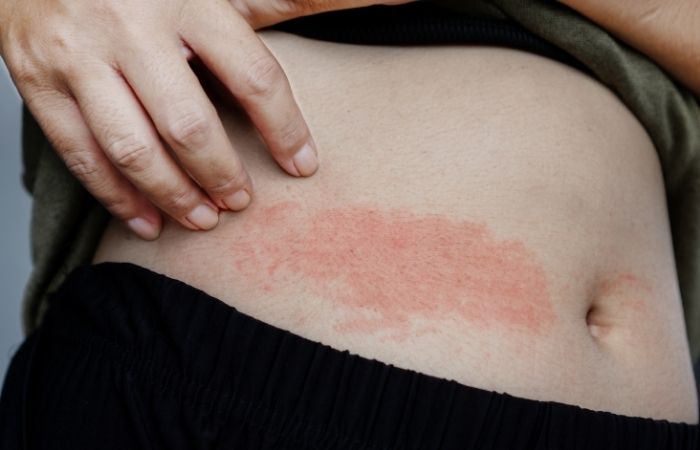
People are also reading: HPV and Throat Cancer: What a BBC Story Reveals About Early Warning Signs
What Friction Actually Looks Like
Friction burn after sex is common, especially after longer sessions or positions that create repeated rubbing. It often appears as diffuse redness, mild swelling, or a shiny irritated patch. It may sting when you urinate or shower, but it usually improves within 24 to 72 hours.
There are usually no blisters, no open sores, and no systemic symptoms. The skin looks irritated, not ulcerated. Think chafing, not infection.
People with vulvas often describe it as a “raw” feeling around the labia. People with penises may notice redness along the shaft or underside near the frenulum. It can mimic an STD rash in the moment, but the speed of onset and quick resolution are key clues.
Allergic Reactions: The Overlooked Trigger
An allergic reaction after sex can look dramatic but isn’t contagious. Latex allergy, sensitivity to spermicide, flavored lubricants, warming gels, new soaps, or even a partner’s detergent can cause redness, itching, and small bumps.
Latex allergy symptoms on genitals often include itching within minutes to hours. The rash may feel intensely itchy rather than painful. Swelling can occur, especially in people who already have sensitive skin or eczema.
Some people also react to semen proteins, a condition called seminal plasma hypersensitivity. It’s rare, but it happens. In those cases, burning and redness may appear after unprotected intercourse and resolve over a day or two.
Unlike most STDs, allergic reactions typically improve with antihistamines, cool compresses, or avoiding the trigger. They don’t evolve into blisters or ulcers over several days.
When Infection Enters the Conversation
Now we talk about the part your brain jumps to first: sexually transmitted infections. Some STDs can cause rashes, but the timeline and appearance usually differ from simple irritation.
- Herpes often begins with tingling or burning before visible sores appear. These sores become small fluid-filled blisters that break and crust. They are usually painful. The first outbreak may include swollen lymph nodes or flu-like symptoms.
- Syphilis can start with a painless sore called a chancre, often unnoticed. Weeks later, a body rash may appear, sometimes on palms and soles. That rash typically does not itch.
- HPV causes warts, not flat redness. They appear as raised, flesh-colored bumps over weeks to months, not overnight.
- Most bacterial STDs like chlamydia and gonorrhea do not cause a visible rash at all. They more commonly produce discharge, burning with urination, or no symptoms whatsoever.
A Side-by-Side Reality Check
Figure 1. Comparing common causes of rash after sex.
This comparison doesn’t replace testing, but it helps recalibrate fear. A rash that appears the same night and fades by the weekend is unlikely to be a new STD infection. Infection requires incubation time.
According to the CDC, herpes symptoms typically appear 2 to 12 days after exposure. Syphilis sores usually appear around 3 weeks after contact. That timeline matters when you’re trying to interpret your skin.
When It’s Not Friction or Allergy: Yeast, BV, and Other Lookalikes
Not every rash after sex is an STD, but not every rash is friction either. One of the most common culprits people overlook is a yeast infection. Sex doesn’t cause yeast directly, but it can disrupt vaginal pH enough to trigger an overgrowth of Candida. That irritation can look like redness, swelling, and tiny fissures that sting during urination.
Unlike friction burn, yeast usually comes with persistent itching and sometimes thick discharge. It doesn’t resolve in a day or two without treatment. The discomfort lingers, and the itching tends to intensify at night. Many people search “yeast infection rash vs STD” because visually, early yeast irritation can resemble mild herpes redness before blisters form.
Bacterial vaginosis (BV) doesn’t typically cause a rash, but it can create irritation from discharge changes. If the skin is already sensitive, that moisture can contribute to redness. In penis owners, fungal infections can also develop under the foreskin, especially if moisture gets trapped.
Heat Rash, Razor Burn, and the Timing Trap
Sometimes the rash isn’t sexual at all. Sweat, tight clothing, and shaved skin create the perfect setup for heat rash. If you had sex after working out or stayed in tight underwear afterward, tiny red bumps can appear where sweat ducts get blocked.
Razor burn can also flare post-intercourse because friction irritates already inflamed hair follicles. These bumps are usually centered around hair follicles and may feel tender but not deeply painful.
The key distinction here is distribution. Heat rash and razor burn follow friction zones and hair growth patterns. STD rashes tend to localize differently, herpes lesions cluster, syphilis sores ulcerate, HPV forms distinct growths.
How Long Does an STD Rash Last?
This question drives a lot of late-night panic searches. The answer depends on the infection, but one principle holds: infectious rashes usually evolve rather than fade quickly.
Herpes lesions typically progress from tingling to blisters to open sores over several days before crusting and healing in about two to four weeks during a first outbreak. Syphilis sores may last three to six weeks even without treatment. HPV warts persist until treated or cleared by the immune system.
Friction and allergic reactions, by contrast, improve within a few days once the irritant is removed. If redness is clearly better within 48 to 72 hours, infection becomes less likely.
When to Test After a Rash Appears
This is where anxiety meets biology. If you notice a rash immediately after sex, testing that same day won’t tell you much about a new infection. Most STDs require a window period before tests become accurate.
Herpes testing is most accurate when a fresh blister is swabbed within the first 48 hours of appearing. Blood antibody tests require more time, often several weeks, to turn positive. Syphilis blood tests usually become reliable around three to six weeks after exposure.
If your rash appeared within hours of sex, it’s unlikely to represent a brand-new infection from that encounter. However, if you had unprotected contact in the prior weeks, testing may still be appropriate based on that earlier timeline.
Peace of mind matters. If your brain won’t settle, a discreet at-home panel from STD Test Kits can help you check for common infections without a clinic visit. Testing isn’t an admission of guilt. It’s information.

People are also reading: Itchy Anus: STD or Hemorrhoids? How to Tell the Difference
A Practical Timeline Table
Figure 2. Approximate timelines for common post-sex rash concerns.
“I Thought I Gave Him Something”
Arjun, 28, noticed redness on his penis the morning after sex with a new partner. “It was bright red and kind of shiny. I spiraled. I kept thinking, I infected someone.”
He tested two days later. Negative. The redness faded by day three. His doctor later explained it was likely friction combined with a new lubricant. “I felt ridiculous,” he said. But the fear was real.
This is the emotional part people don’t talk about. A rash after sex can trigger shame faster than science can catch up. You start imagining conversations you haven’t even had yet. That spiral is common, and human.
When It’s Time to Take It Seriously
You should seek testing or medical care if the rash includes painful blisters, open sores, spreading lesions, fever, swollen lymph nodes, unusual discharge, or if it persists beyond several days without improvement.
If you had unprotected sex and symptoms appear days later rather than immediately, infection moves higher on the list. That’s when an at-home kit like the 6‑in‑1 At‑Home STD Test Kit can provide broader screening in one step.
You deserve clarity. Not because you did something wrong, but because your health matters.
Red Bumps After Sex But They Don’t Hurt
This is one of the most common anxiety spirals: you notice small red bumps after sex, but they don’t itch, don’t burn, and don’t hurt. They just exist. And suddenly your brain is whispering herpes.
Here’s the reality most people aren’t told clearly enough. Many harmless skin reactions create small red bumps. Inflamed hair follicles, mild contact dermatitis, blocked sweat ducts, or simple post-friction swelling can all produce visible changes without pain.
Herpes lesions, by contrast, are usually tender. They often start with tingling or burning before visible sores form. Those sores typically become fluid-filled blisters before breaking open. If what you’re seeing is flat redness or tiny bumps that never blister, infection becomes less likely.
Still, no article replaces your lived context. If the bumps change shape, fill with fluid, crust over, or become painful within a few days, that’s when testing makes sense.
Can Semen Cause a Rash?
Yes. And almost nobody talks about it.
Some people have a mild sensitivity to semen proteins. This isn’t an STD. It’s an immune response. After unprotected intercourse, redness and burning can appear in the vulvar area and resolve within a day or two. The reaction doesn’t spread and doesn’t evolve into blisters.
This condition, seminal plasma hypersensitivity, is rare but real. More commonly, semen can temporarily alter vaginal pH, which may later trigger yeast irritation. That irritation may appear a day or two after sex, creating confusion about cause and effect.
The key distinction is progression. Allergic or pH-related irritation improves with avoidance or treatment. STD-related rashes evolve.
Why Shame Amplifies Skin Symptoms
A rash after sex isn’t just a dermatologic issue. It’s psychological. If the encounter felt uncertain, risky, new, or emotionally loaded, your nervous system is already heightened. The body becomes something to monitor.
People often say, “I can’t stop checking.” That checking fuels fear. Every tiny change feels dramatic. In clinic settings, Dr. F. David, MD, has seen patients convinced they have syphilis when the redness is simple friction.
Testing can interrupt that spiral. Not because you’re reckless. Because information replaces imagination. If your exposure risk was real, testing is responsible. If your rash is fading and timing doesn’t match incubation periods, that’s reassuring data.
How Timing Changes the Risk Equation
If redness appears the same night as sex, mechanical irritation rises to the top of the list. Infectious causes rarely manifest within hours of exposure. That biological delay is protective, it gives your immune system time to react before symptoms show.
But if symptoms begin several days later, especially with tenderness or sores, infection becomes more plausible. Herpes typically appears within 2 to 12 days. A syphilis sore averages about 3 weeks after exposure. HPV warts can take months.
This is why the question isn’t just “Is this an STD?” It’s “When did this start, and what else is happening?” Context is diagnostic power.
What Makes a Rash Concerning
There are specific red flags that shift the equation from irritation to possible infection. Painful blisters, open ulcers, spreading lesions, fever, swollen groin lymph nodes, unexplained fatigue, or a rash on palms and soles all warrant evaluation.
A rash that persists beyond several days without improvement also deserves attention. Friction and mild allergy improve once the irritant is gone. Infections progress.
If you’re unsure and the mental load feels heavy, broad screening through a 7-in-1 Complete At-Home STD Test Kit can check for multiple infections at once. That step transforms guessing into clarity.
Another Case Study: “It Wasn’t What I Feared”
Lina, 32, noticed itching and redness two days after sex. “I kept Googling STD rash vs friction rash. I convinced myself it was herpes.”
There were no blisters. Just irritation. She tested anyway. Negative. Her doctor later diagnosed a yeast infection triggered by antibiotic use earlier that month. “I lost sleep for three nights over something treatable,” she said.
The lesson isn’t that testing was unnecessary. It’s that fear often overestimates probability. But testing gave her closure. That peace mattered.
You’re Allowed to Want Certainty
There’s a stigma that says if you test, you must have done something wrong. That narrative is outdated. Testing is modern sexual health maintenance. It’s routine, responsible, and protective, for you and your partners.
If your rash is fading and matches friction or allergy patterns, observation may be enough. If it lingers, evolves, or follows a higher-risk encounter, discreet testing through STD Test Kits gives you answers privately and quickly.
You don’t have to sit in uncertainty. You don’t have to catastrophize. You can choose data.
FAQs
1. Can I get an STD if I have a rash that shows up on the same day as having sex?
Not very likely. Most STDs have what's called a window period, which means there's a time delay between when you're infected and when symptoms show up. If a rash shows up on the same day as having sex, it's most likely from friction or allergies. However, if you've had previous exposures in the days leading up to this incident, then it would be best to test after that window period.
2. What does an STD rash actually look like?
Well, it depends on what kind of STD it is. If it's herpes, there are usually painful blisters that eventually break out. If it's syphilis, there's usually a painless sore and then a body rash that might show up on your palms or soles. If it's HPV, there are usually bumps or warts. But if it's chlamydia or gonorrhea, there usually isn't any rash at all.
3. How long should I wait if I'm concerned?
Well, it depends on what kind of STD it is. If it's herpes, it would be best to test right away, as swab tests are most accurate if there's a recent lesion. If it's either herpes or syphilis, it would be best to wait a few weeks after having sex. If you're unsure which test to get, it would be best to get a general test.
4. Can friction really cause that kind of rash?
Yes, it can. Your genital area is very sensitive, and if you're having a lot of sex without lubrication, it can cause inflammation. If your rash shows signs of improvement after two or three days, then it was probably from friction.
5. What if I have a rash and it doesn't itch or hurt?
The majority of harmless skin reactions are not painful. Infected rashes, including herpes, may be accompanied by discomfort or pain. Flat, non-progressing redness without discomfort or pain is not as worrisome, although it should be monitored.
6. Could condoms be the cause of my rash?
Allergic reactions to latex or chemicals used as lubricants or spermicides may cause itching or redness. In many cases, changing to non-latex condoms or using non-fragrances may resolve the problem. If the rash disappears after changing condoms, it is probably caused by an allergy.
7. Is it possible to get an STD rash without other symptoms?
Yes, although it is not as common. That’s why we look at changes over time, not just at one particular moment. Testing answers all questions.
8. Can a yeast infection look like an STD?
The initial irritation of a yeast infection may look similar to herpes before blisters develop. However, a yeast infection typically has itching, whereas herpes does not. In addition, a yeast infection does not develop fluid-filled blisters.
9. What if I got negative test results, but I’m still worried?
Anxiety does not go away by rationalizing or using logic. Even if you’ve used a good window of time to get tested and your test results were negative, you are not at risk. In some cases, retesting after the full window period may give you peace of mind.
10. Should I get my partner tested?
If you’ve had sex without a condom and you’re not sure of either of your partners’ HIV or STD status, getting tested together can go a long way toward building trust. Testing together changes the dialogue from guilt to shared responsibility.
Before You Spiral, Do This Instead
A rash after sex does not automatically mean infection. Most of the time, it’s friction, sensitivity, yeast, or simple skin irritation. The body reacts quickly to touch and chemicals. Infections take time to declare themselves.
If your rash improves within a few days and never evolves into sores, that’s reassuring. If it persists, spreads, or aligns with a known exposure window, testing is a smart next step. Not because you should feel ashamed. Because you deserve certainty.
Don’t sit in fear and refresh search results at 2 a.m. If clarity would help you breathe easier, consider a discreet, physician-backed option like the 8‑in‑1 Complete At-Home STD Test Kit. It screens for common infections privately and quickly, so you can move from speculation to facts.
How We Sourced This Article: We reviewed current guidance from the CDC, Mayo Clinic, and the World Health Organization on STD symptom presentation and incubation periods. Peer-reviewed dermatology and infectious disease literature informed the discussion of rash progression and timing. Lifestyle reporting and patient narratives were analyzed to reflect real-world search behavior and emotional context. Approximately fifteen sources were consulted during research; six of the most authoritative and reader-accessible are listed below.
Sources
1. World Health Organization – Sexually Transmitted Infections Overview
2. Mayo Clinic – Genital Herpes Symptoms and Causes
3. StatPearls – Vulvovaginal Candidiasis
5. Latex allergy - Symptoms and causes | Mayo Clinic
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works on preventing, diagnosing, and treating STIs. He combines a clinical approach with a sex-positive, stigma-free approach to teaching people about sexual health.
Reviewed by: Jordan K. Ramirez, PA-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.