Last updated: April 2026
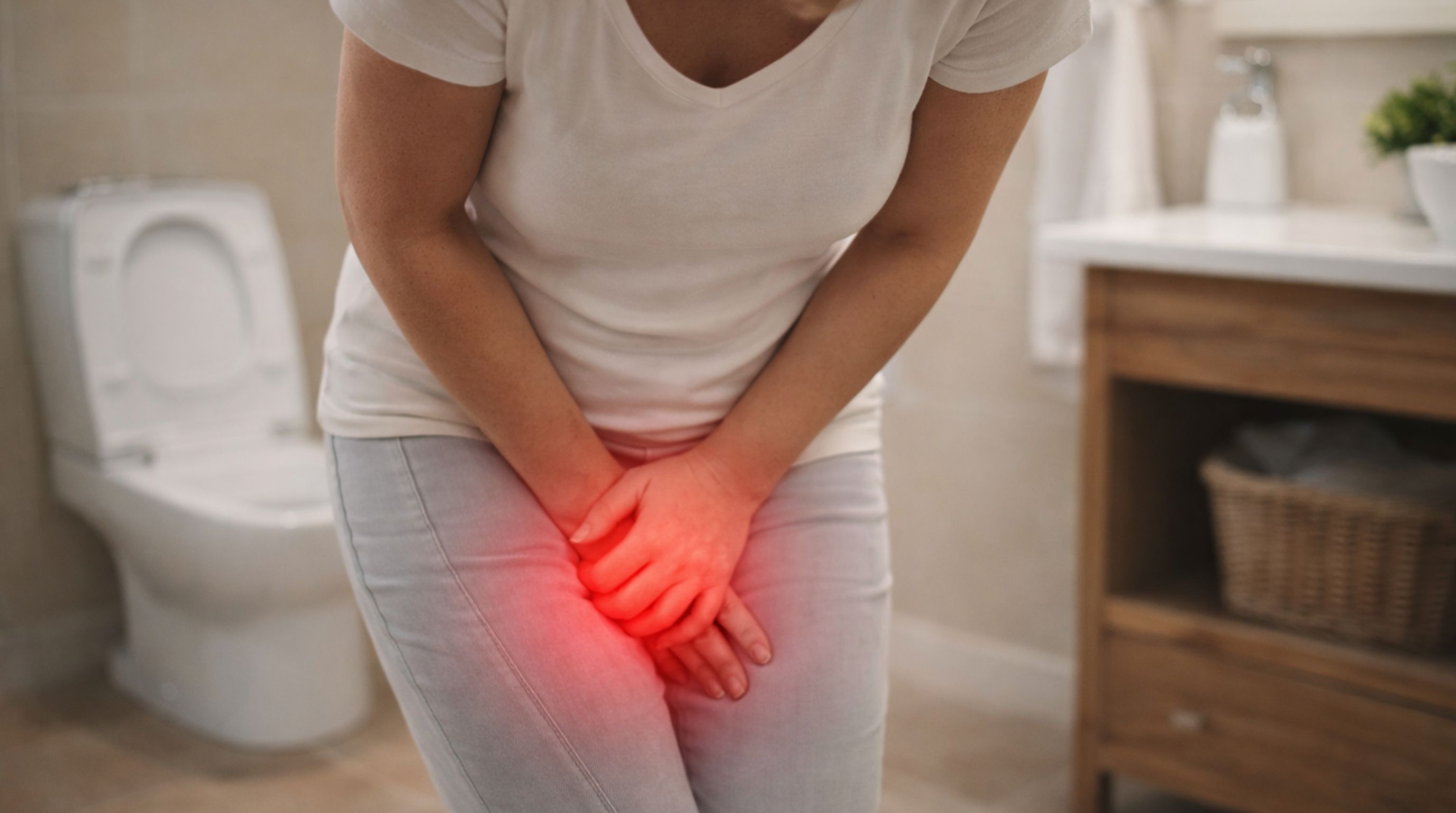
Something changes down there, a different smell, a shift in discharge, that low-grade burning when you pee, and your first instinct is to figure out what's going on. BV crosses your mind because it's common, because you've had it before, or because you Googled your symptoms and it came up first. That instinct isn't wrong. But here's the part that doesn't get talked about enough: chlamydia, gonorrhea, and trichomoniasis can feel exactly the same. Same discharge. Same odor. Same burn. And without a test, there's genuinely no way to know which one you're dealing with.
BV is the most common vaginal infection in women aged 15 to 44, according to the CDC, which means most people have experienced it, most people have a mental picture of what it feels like, and most people assume they'd recognize it if it came back. The problem is that assumptions get people into trouble all the time. STDs mimic BV so closely that the overlap isn't a minor footnote. It's the main story.
People are also reading: Trichomoniasis Symptoms During Pregnancy, Or Why You Probably Won't Have Any
What Does BV Feel Like, and Why Can't You Use That to Diagnose Yourself?
BV happens when the normal balance of bacteria in the vagina tips out of control, specifically when anaerobic bacteria overgrow and crowd out the protective lactobacilli that keep your vaginal environment stable. The result is a shift in pH, and that shift is what drives the symptoms most people associate with BV: a thin, gray, or off-white discharge, a fishy odor that gets stronger after sex or during your period, and sometimes mild burning or itching around the vaginal opening.
Here's what makes BV particularly deceptive: up to 84% of people who have it experience no symptoms at all, according to the CDC. So if you do have symptoms, you might feel relieved that at least you know something is going on. But that relief can lead to a shortcut, assuming that because the symptoms fit a BV pattern, BV must be the answer. That shortcut skips over the part where multiple infections can produce the exact same pattern.
The CDC's own treatment guidelines are direct on this point: obtaining a medical history alone is insufficient for accurately diagnosing vaginitis. Lab testing is required. That's not a formality. It reflects the genuine clinical reality that symptoms don't reliably tell you which infection is present, and treating the wrong one means the actual infection keeps going, untreated, doing damage in the background.
Which STDs Feel the Most Like BV?
Three STDs come up again and again in the context of BV misdiagnosis: chlamydia, gonorrhea, and trichomoniasis. Each one can produce symptoms that are, from a purely experiential standpoint, indistinguishable from BV. Understanding why they overlap, biologically, makes it easier to understand why testing is the only real answer.
Chlamydia is the most commonly reported bacterial STD in the US, with over 1.6 million cases documented in a single year according to CDC surveillance data. In women, it typically causes inflammation of the cervix (cervicitis), which can produce an abnormal discharge, burning during urination, and pelvic discomfort. These are also core BV symptoms. What makes chlamydia especially likely to be missed is that the majority of infections cause no symptoms at all, meaning someone can have chlamydia and BV simultaneously, treat the BV, and never know the chlamydia is still there. According to the CDC, untreated chlamydia can lead to pelvic inflammatory disease (PID) and long-term fertility complications, outcomes that don't come from BV.
Gonorrhea produces a similar picture. Like chlamydia, it infects the cervix and urethra in women, and it can cause discharge, burning when urinating, and vaginal irritation. The discharge with gonorrhea tends to be yellow-green and slightly thicker than the thin, gray discharge typical of BV, but "tends to be" is doing a lot of work in that sentence. Discharge appearance alone is not a reliable diagnostic tool, and the overlap is real enough that clinicians are explicitly warned against relying on symptoms to differentiate these infections.
Trichomoniasis is the closest mimic of all. Trich is caused by a parasite, Trichomonas vaginalis, and it's actually the most prevalent non-viral STD in the US. It causes vaginitis, meaning direct inflammation of the vaginal walls, which produces discharge, odor, burning, and itching. The discharge with trich is classically described as frothy and yellow-green, but research shows that many people with trichomoniasis have discharge that looks nothing like that. Between 70 and 85% of trich infections produce minimal or no symptoms, according to CDC treatment guidelines, which means the overlap with asymptomatic or mild BV is almost complete.
How Often Is BV Misdiagnosed as an STD, or the Other Way Around?
You might assume that a doctor or nurse looking at your symptoms would catch the difference. In some cases, yes. But the clinical reality is more complicated. A study of 220 symptomatic patients found that 61% of bacterial vaginosis diagnoses were incorrect. That's not a rare edge case; it's a majority. And it reflects the core problem: when symptoms overlap this completely, symptom-based diagnosis fails.
The CDC's treatment guidelines address this directly. For vaginal symptoms, they recommend pH testing, microscopy, and ideally nucleic acid amplification testing (NAAT), not a clinical assessment based on what the discharge looks like or what the patient describes. The reason is simple: the infections most commonly associated with vaginal symptoms (BV, trichomoniasis, and candidiasis) present similarly, and differentiating them by eye or by history alone leads to incorrect treatment.
This matters because treating BV when you actually have chlamydia doesn't just fail to fix chlamydia; it can create a false sense of resolution. Symptoms may quiet down temporarily. The antibiotic used for BV may partially suppress some of what's going on. And then weeks later, the underlying STD resurfaces, or it keeps causing damage silently, or it gets passed to a partner who had no idea anything was wrong. The cycle of recurring "BV" that many women experience is, in a meaningful number of cases, something else entirely.
Can You Have BV and an STD at the Same Time?
Yes, and this is where the story gets more complicated. BV doesn't just mimic STDs. It actively increases your risk of getting one. Women with BV are at significantly elevated risk of acquiring chlamydia, gonorrhea, trichomoniasis, and HIV, according to CDC research. The disrupted vaginal microbiome that defines BV compromises the protective barrier that healthy lactobacilli provide, making it easier for pathogens to take hold.
Research published in peer-reviewed journals has found co-infection rates between BV and trichomoniasis as high as 60 to 80%, meaning that if you have trich, there's a strong chance you also have BV at the same time. The same pattern holds with chlamydia. You can have both, treat one, and be left with the other still active. Without testing for both, you won't know.
This co-infection dynamic is also why the "it's just BV again" assumption is particularly risky after a new partner or unprotected sex. The symptoms you're seeing may genuinely be BV, or they may be an STD that developed against the backdrop of BV, or both simultaneously. Your symptoms won't help you sort that out. A test will.
How to Actually Tell Them Apart, At Home, Right Now
There is no symptom checklist that reliably separates BV from an STD. That's not a limitation of the checklist; it's a biological reality. The same inflammatory pathways, the same disruption to vaginal pH, the same tissue irritation. The only way to know which infection is present is to test for the specific pathogens causing it.
At-home rapid test kits make this straightforward, but the right test depends on your specific situation. For chlamydia, the testing window opens 14 days after exposure. For gonorrhea, test 3 weeks after exposure. For trichomoniasis, testing can be done from 5 to 28 days after exposure, though waiting until symptoms appear is also a reasonable trigger. These aren't arbitrary numbers; they reflect the time needed for the infection to reach detectable levels. Testing too early produces false negatives, which can be just as misleading as no test at all. A full breakdown of STD testing window periods and when to test for each infection is worth reading before you order anything, so you're not testing too early and getting a result you can't rely on.
If you're not sure which test applies to your situation, this guide breaks down which STD test you need by situation, new partner, recurring symptoms, post-treatment follow-up, and more. Getting the right test matters as much as getting tested at all.
Testing is not an overreaction. It's the move that stops the guessing cycle, and it's the only one that actually works.

People are also reading: Can Trichomoniasis Cause a Miscarriage or Preterm Birth?
What the Discharge Is (and Isn't) Telling You
Discharge gets a lot of attention in the BV vs STD conversation because it's the most visible symptom and the one people feel most confident reading. The reality is that discharge appearance is useful but not definitive, and placing too much weight on it leads to exactly the kind of misdiagnosis the data keeps documenting.
Here's what discharge can tell you: BV tends to produce a thin, watery, gray, or off-white discharge. Trichomoniasis classically produces a frothy, yellow-green discharge, but "classically" means in textbooks. In real presentations, trich discharge can be white, gray, or barely different from a person's usual baseline. Chlamydia and gonorrhea can cause discharge that looks indistinguishable from BV discharge in terms of color and consistency. The fishy odor associated with BV can also occur with trich, because both infections alter vaginal pH in ways that produce similar odor compounds.
The one discharge finding that does point away from BV specifically is the presence of visible sores, blisters, or ulcers around the vagina or vulva. BV does not cause sores. If those are present, herpes or syphilis belong on the list of possibilities and should be tested for separately. But in the absence of visible sores, when it's just discharge, odor, and burning, discharge appearance alone isn't going to give you the answer you need.
The STD Risk That BV Creates, Even If You Don't Have One Yet
One part of this conversation that doesn't come up often enough is what BV does to your vulnerability to STDs, not just whether you currently have one, but how much easier it becomes to acquire one while BV is active. The disrupted vaginal microbiome associated with BV reduces the lactic acid and hydrogen peroxide that healthy lactobacilli produce, both of which play a direct role in preventing pathogens from establishing themselves.
According to the CDC, having BV increases the risk of acquiring HIV, gonorrhea, chlamydia, and trichomoniasis. This isn't a minor statistical bump; the biological mechanism is well established. A compromised vaginal environment is a more hospitable one for sexually transmitted pathogens. So even if your current symptoms are definitely BV with no STD co-infection, that window of active BV is a period of elevated risk. Getting tested after a new partner or unprotected sex, even if you're already treating BV, is the kind of proactive step that matters.
The CDC's 2024 provisional surveillance data underlines why this matters at a population level: over 2.2 million cases of chlamydia, gonorrhea, and syphilis were reported in the US in a single year. Young women under 25 accounted for a disproportionate share of chlamydia cases. Many of those infections went undetected for extended periods, not because people weren't paying attention to their bodies, but because the symptoms they noticed pointed them toward a different diagnosis first.
When Should You Stop Assuming It's BV and Test for an STD?
There are specific situations where defaulting to a BV assumption is particularly worth questioning. If you've had a new sexual partner in the last few weeks and symptoms appear, that timeline matters. BV can be triggered by a new partner, but so can chlamydia, gonorrhea, and trichomoniasis. The same event that disrupted your vaginal pH may also have introduced a pathogen. Both things can happen at once.
If you've treated BV with antibiotics and symptoms resolved, then came back within a few weeks, that recurrence pattern deserves attention. Recurring BV is real and common; BV recurrence rates within a year can reach 58% according to published research. But recurring symptoms can also mean that the original diagnosis was incomplete, that an STD was present alongside the BV and wasn't treated, or that a new exposure occurred during or after treatment. A recurrence is a reason to test, not just re-treat.
If burning or discharge persists beyond a completed course of BV treatment, that's a direct signal that something else may be involved. BV antibiotics don't treat chlamydia, gonorrhea, or trichomoniasis. Persistent symptoms after appropriate BV treatment are a strong reason to test for STDs, not a reason to try a different BV antibiotic. If you're unsure where to start, this STD risk checker can help you figure out whether testing makes sense for your specific situation. It takes two minutes and cuts through the uncertainty.

People are also reading: STD or BV? When the Only Symptom Is Smell
FAQs
1. Can BV actually feel identical to an STD?
Yes, and that's not an exaggeration. Chlamydia, gonorrhea, and trichomoniasis can all produce the same discharge, odor, and burning that BV does. From a purely symptom-based standpoint, they are often indistinguishable, which is why testing is the only reliable way to know what you're dealing with.
2. What's the main difference between BV discharge and STD discharge?
BV discharge is typically thin, gray, or off-white, and watery, often paired with a fishy odor that gets stronger after sex. Trichomoniasis is classically described as frothy and yellow-green, while chlamydia and gonorrhea can produce white, cloudy, or yellow-green discharge. In practice, these distinctions aren't reliable enough to diagnose by; discharge appearance overlaps significantly across all four conditions, and many infections produce little or no discharge at all. Testing is the only way to know.
3. Can I have BV and an STD at the same time?
Absolutely, and it's more common than most people expect. Co-infection rates between BV and trichomoniasis have been documented as high as 60 to 80% in some studies. Having BV also increases your biological risk of acquiring chlamydia, gonorrhea, and HIV, because the disrupted vaginal microbiome compromises the natural defenses that healthy lactobacilli provide. Treating BV alone won't touch the STD; both need to be identified and addressed separately.
4. If I treat BV and the symptoms go away, does that mean I didn't have an STD?
Not necessarily. BV antibiotics can reduce general vaginal inflammation, which may temporarily suppress some symptoms of a co-existing STD. If the STD was chlamydia or gonorrhea, it's still there, untreated, and the symptoms may return. Symptom resolution after BV treatment isn't confirmation that no STD was present.
5. How soon after exposure can I test for chlamydia or gonorrhea?
For chlamydia, test from 14 days after exposure. For gonorrhea, test 3 weeks after exposure. Testing earlier than these windows can produce a false negative, even if the infection is present, because the pathogen hasn't reached detectable levels yet.
6. Does BV make you more likely to get an STD?
Yes, this is well established. The disrupted vaginal microbiome associated with BV reduces the natural defenses that healthy lactobacilli provide. According to the CDC, having active BV increases the risk of acquiring HIV, chlamydia, gonorrhea, and trichomoniasis. Getting tested after any new exposure while BV is active is a reasonable and informed decision.
7. Can trichomoniasis be mistaken for BV?
Very easily, trichomoniasis is probably the closest mimic of BV that exists. Both produce discharge with a fishy odor. Both can cause burning and itching. Between 70 and 85% of trich infections produce minimal or no symptoms at all, which mirrors the asymptomatic presentation common in BV. On top of that, trich is not always included in standard STD panels, so it can go undetected for months unless you specifically request or use a test that screens for it.
8. What if my BV keeps coming back?
Recurring BV is common, but recurring symptoms can also mean an STD was present and untreated alongside the original BV diagnosis. If BV seems to keep returning, especially after a new partner or unprotected sex, testing for chlamydia, gonorrhea, and trichomoniasis is the right next step, not just another course of BV antibiotics.
9. Is there a test that covers both BV-related infections and STDs?
At-home STD test kits cover chlamydia, gonorrhea, and trichomoniasis, the three STDs most likely to be confused with BV. A 7-in-1 kit adds HIV, syphilis, hepatitis B, and hepatitis C. These kits don't test for BV itself (that requires a pH or microscopy test), but they cover the STD side of the diagnostic question efficiently.
10. What's the one thing most people get wrong about BV vs STDs?
Trusting their symptoms to tell the difference. The instinct to read discharge color, odor, and texture as a diagnostic tool is understandable, but the clinical data is clear that symptoms alone are not reliable enough to distinguish BV from chlamydia, gonorrhea, or trichomoniasis. The one way to know is testing. Everything else is an educated guess.
Stop Guessing, Here's How to Know for Sure
If something feels off and you're not certain whether it's BV or something more, that uncertainty is exactly what at-home STD testing is built for. The two infections most commonly confused with BV, chlamydia and gonorrhea, are covered by the Chlamydia & Gonorrhea At-Home STD Test Kit from STD Test Kits, with accuracy over 98% and results you can take seriously.
If trichomoniasis is also on your mind, especially after a new partner, recurring symptoms, or BV treatment that didn't fully resolve things, the 7-in-1 Complete At-Home STD Test Kit covers chlamydia, gonorrhea, trichomoniasis, HSV-2, syphilis, hepatitis B, and hepatitis C in a single test. It's the most thorough option when the picture isn't clear, and you want a complete answer, not a partial one.
Testing is the fastest way to stop the guessing game and start dealing with what's actually there. Visit STD Test Kits to find the right test for your situation.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. Centers for Disease Control and Prevention, About Bacterial Vaginosis (BV)
2. CDC STI Treatment Guidelines, Vaginal Discharge
3. CDC STI Treatment Guidelines, Bacterial Vaginosis
5. Evvy, How to Tell the Difference Between BV and Trichomoniasis
6. CDC, Sexually Transmitted Infections Surveillance, 2024 (Provisional)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.