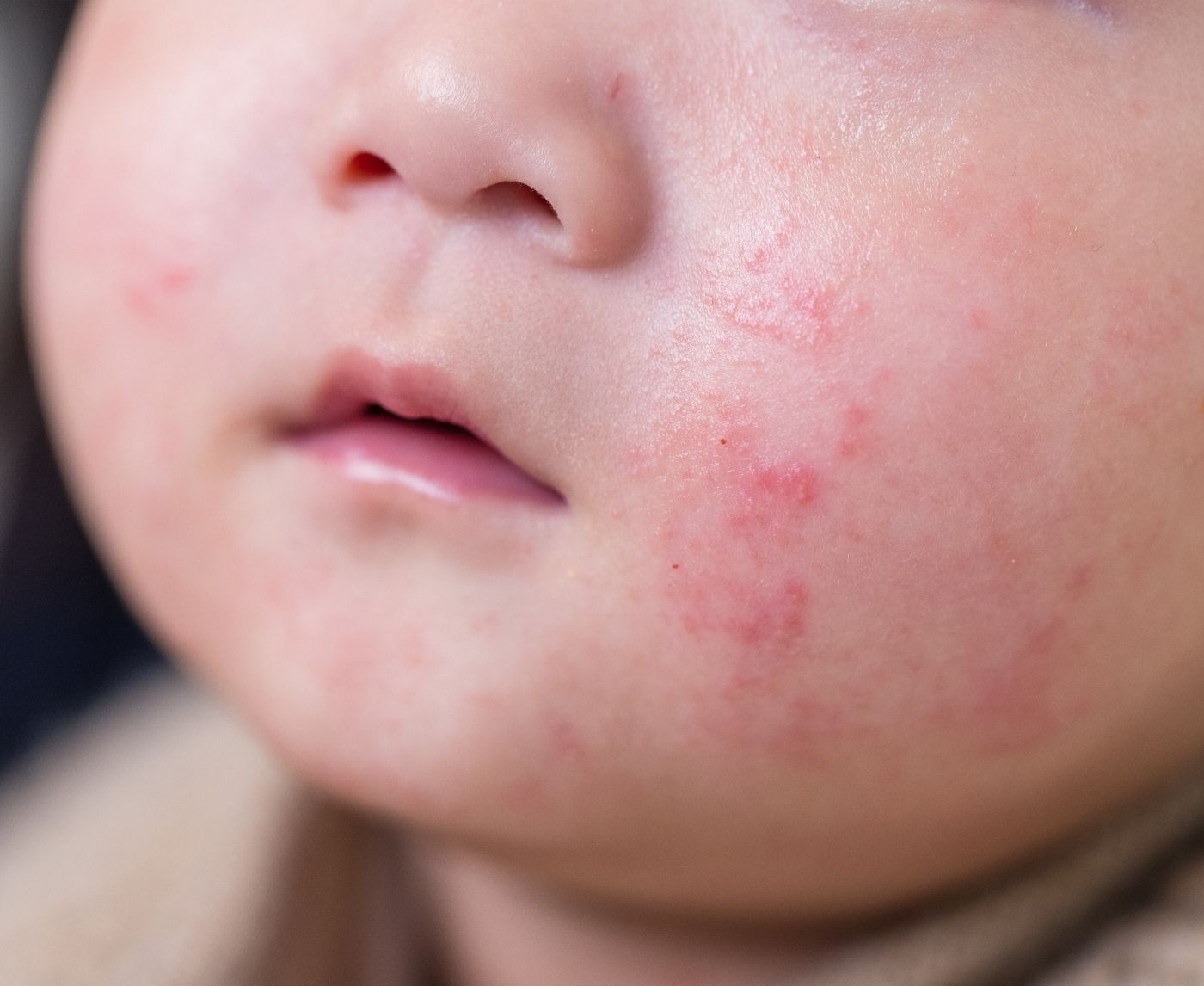
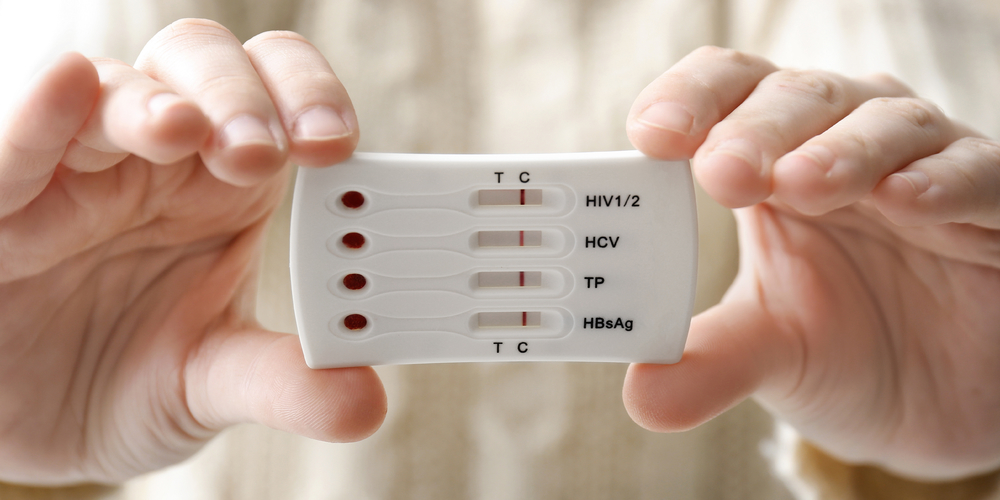
When the STD Test Says “Negative” But Your Body Says “Something’s Wrong”
Quick Answer: Yes, children can get STDs like herpes, HPV, and hepatitis B through nonsexual routes such as childbirth, casual contact, or shared items. Not all STDs in kids indicate sexual abuse.
Why This Article Matters (And Who It’s For)
This guide is for the parent who panicked after seeing “positive for herpes” on their child’s lab report. For the doctor unsure if a case requires mandatory reporting. For foster parents, social workers, and teachers trying to make sense of a deeply stigmatized issue. And for any adult asking: “Is it possible my child caught this another way?”
We live in a world where the words “STD” and “child” feel irreconcilable. But pediatric medicine, virology, and real-life data say otherwise. This article is here to unpack truth from fear, and to walk through the routes, birth, contact, and surface exposure, that make nonsexual STD transmission possible in kids. We’ll look at what infections are most likely, how transmission happens, when it signals danger, and what steps to take if your child tests positive.

People are also reading: How a Cold Sore Kiss Nearly Blinded a Toddler, and What It Means for Herpes Testing
Understanding the Basics: What “STD” Really Means
Let’s clear something up. “Sexually transmitted disease” is a label about transmission, not morality. And in pediatric cases, that label can mislead. Many STDs are caused by pathogens (viruses, bacteria, parasites) that can spread in nonsexual ways, especially in children whose immune systems and skin barriers are still developing.
Take HSV-1, the virus that causes cold sores. In adults, it’s often sexually transmitted. In children? It’s more likely passed by a kiss from a family member, shared utensils, or sippy cups. Likewise, hepatitis B can spread through blood contact from minor cuts or even during birth. HPV, the virus behind genital warts, has been detected on fingers, towels, and diaper-changing surfaces, though transmission in such cases is rare.
Bottom line: If you’re staring down an STD diagnosis in a child, don’t assume the worst before understanding how that infection works biologically.
Common STDs That Can Affect Children Non-Sexually
Not all STDs behave the same. Some rely on direct genital contact. Others are opportunistic travelers, hitching a ride via saliva, shared surfaces, or vertical transmission from parent to child. Below is a breakdown of the most common STDs that can show up in children without sexual contact.
Figure 1. STDs that can appear in children via nonsexual exposure, and how medical teams determine if further investigation is needed.
“My Toddler Got Herpes, and I Was Accused of Something I Didn’t Do”
Daniela, 29, brought her 2-year-old son to urgent care for what she thought was teething pain. It turned out to be oral herpes. “They pulled me aside and said they had to file a report,” she recalls. “I felt like a criminal, for a cold sore I probably gave him by accident.”
“No one tells you that if you’ve had cold sores, you can pass them to your kid even without symptoms. I would never hurt him.”
Daniela’s story isn’t unique. The stress of a mandatory report, even when abuse is ruled out, can leave families traumatized. But it’s also an example of how common viruses like HSV-1 can move silently between loved ones. In fact, studies show that 30–60% of children acquire HSV-1 during childhood, often from household members.
How Doctors Evaluate Risk Without Jumping to Conclusions
Not every case of a child with an STD should spark panic, or police. Pediatricians and child protection teams follow established protocols to assess whether a finding suggests possible abuse. Factors include:
- Child’s age and verbal ability: A 2-year-old with herpes is different from a 10-year-old with gonorrhea.
- Infection type: Some STDs (like chlamydia in an older child) are highly suspicious. Others (like HSV-1) are often benign.
- Presence of physical trauma: Genital injuries or signs of penetration require immediate action.
- Family medical history: If a parent has an active STD or cold sore history, transmission may be explainable.
That said, if a child tests positive for chlamydia, gonorrhea, or syphilis and is beyond the perinatal age window, medical and legal professionals are mandated to investigate further.
Myths That Make It Worse: What Pediatric STDs Are NOT
When it comes to kids and STDs, misinformation can do real harm. Many well-meaning people, even medical professionals, believe myths that fuel stigma, trauma, and even unnecessary investigations. Let’s debunk a few of the most damaging:
Myth #1: Any STD in a child = sexual abuse. This is false. While some STDs are highly suggestive of abuse, many (like HSV-1 or hepatitis B) have multiple transmission routes, especially in children under five. Abuse must be considered, but it is not always the cause.
Myth #2: Cold sores aren’t STDs. Technically, they can be. HSV-1 is a herpes virus, and while it's commonly acquired nonsexually in childhood, it can be transmitted sexually in adulthood. Medical terminology evolves; so should our understanding of transmission.
Myth #3: If a child has an STD, someone is hiding something. Sometimes yes. But often, no. Many pediatric STD diagnoses are tied to maternal infections passed during birth or casual contact. The assumption of guilt can tear families apart before facts are gathered.
Medical teams must walk a careful line: investigate when warranted, but not criminalize nonsexual illness. Parents, too, must resist the urge to panic, or to self-blame. Viruses don’t ask permission before they spread.
How STDs Can Spread in Children Without Abuse
Children are messy. They drool, share cups, trade pacifiers, and touch everything. Their skin is thinner. Their immune systems are developing. All of this makes them more susceptible to certain infections, and some of those infections happen to be classified as STDs.
Below is a breakdown of real-world, nonsexual ways pediatric STDs can spread:
Figure 2. Documented nonsexual transmission methods for STDs that may appear in pediatric patients.
Some infections, like chlamydia or gonorrhea, are far less likely to spread outside of sexual contact or perinatal exposure. But others, especially viral infections like herpes and HPV, are more opportunistic. A cold sore kissed onto a baby’s face is a form of transmission, even if the person had no idea they were shedding virus at the time.
What to Do If Your Child Tests Positive
If you’re facing a pediatric STD result, the path forward will depend on the child’s age, infection type, symptoms, and social context. Here’s what to expect:
- Do not panic, or blame yourself. These infections can be medical accidents, not moral failings. Focus on facts and next steps.
- Request a full explanation from your provider. Ask how the infection may have been acquired, and whether further testing is needed. Not all providers are trained in pediatric STD protocols, don’t be afraid to request a specialist consult.
- Follow the reporting laws in your region. Some cases, like genital warts or oral herpes in young children, don’t require mandatory reporting. Others do. Your doctor must follow child protection guidelines, but that doesn’t always mean police involvement.
- Protect siblings and others. If the infection is contagious by touch (e.g., HSV-1), practice hygiene: no shared towels, avoid kisses during outbreaks, wash hands after diaper changes.
- Get follow-up care and support. You may be referred to a child protection team, infectious disease specialist, or family therapist. Use this as an opportunity to protect, not punish, your family unit.
It’s normal to feel overwhelmed. Many caregivers break down, even when abuse is ruled out. If needed, seek support from pediatric social workers or trauma-informed counselors who can walk you through what comes next.
When Testing Makes Sense (Even Without Symptoms)
STDs in children often go unnoticed until a routine checkup or related illness brings it to light. But there are situations where proactive testing might make sense, even without symptoms:
- Newborns born to mothers with untreated STDs
- Adopted or foster children with unclear medical history
- Children living in crowded or communal care environments
- Siblings of children diagnosed with transmissible infections (like HSV-1 or hepatitis B)
If you’re unsure whether your child needs to be tested, you can start by consulting your pediatrician, or a discreet option: STD Test Kits offers at-home combo test kits for situations that call for privacy and speed.
Whether your concern is medical, emotional, or logistical, peace of mind is often just one test away.

People are also reading: Is Gonorrhea the New Teen STI? Why It’s Spreading Again
“But What Will People Think?”: Facing Stigma as a Parent
Let’s be honest: nothing prepares you for the shame spiral that comes when someone hints that your child’s infection might be “your fault.” Many parents report fear of being judged, investigated, or even separated from their kids.
It’s critical to remember that pediatric infections, yes, even labeled STDs, don’t mean you’re a bad parent. They mean your child, like every other human, is susceptible to pathogens. Period.
If you find yourself afraid of being blamed, advocate for trauma-informed care. Ask your doctor or caseworker if they are trained in pediatric STD evaluation. You have the right to medical explanations without moral judgment.
And if someone in your community judges you? Let this be your mantra: “We got answers. We took care of it. And we did what loving parents do.”
How to Protect Your Child Without Fear
Prevention doesn't have to feel like paranoia. If your child has tested positive, or if you’re worried about possible transmission, there are proactive steps you can take without disrupting daily life or relationships. The key is balancing hygiene, awareness, and emotional reassurance.
- Teach safe touch early. Explain that we don’t share toothbrushes, razors, or drinks. Encourage handwashing after using the bathroom or touching the mouth, nose, or genitals. For younger kids, make it playful, “Soap fights germs like superheroes.”
- Model safe behavior. Adults with active cold sores should avoid kissing children on the face. If you know you’ve had herpes or hepatitis B, be mindful of contact during outbreaks or cuts. Use your own towel, even when it’s tempting to share.
- Keep vaccinations up to date. The hepatitis B vaccine is one of the most effective tools we have to prevent long-term liver damage from early infection. It's recommended for all infants at birth, and catch-up doses are available for older children.
- Address concerns directly. If your child is in daycare or communal living, you have every right to ask about hygiene practices and infection control policies. Ask how shared toys are cleaned, how diaper stations are sanitized, and how caregivers handle signs of illness.
Protecting your child from STDs, just like from colds or flu, is not about blame. It’s about informed care.
Confidential Testing Options: When You Need to Know
If you need to rule out or confirm an STD in a child, your options may depend on how old they are, what symptoms they have, and how comfortable you are with going to the doctor in person. Most of the time, pediatric testing happens in a clinic, but there are some discreet options for parents or older teens who are in sensitive situations.
Here are three common ways to get there:
Figure 3. Overview of testing options for concerned caregivers and teens navigating privacy and timing concerns.
If you’re not sure where to start, begin here: STD Test Kits. Whether you need a chlamydia test, a herpes test, or a combo kit that covers multiple infections, you can test quickly, on your terms.
When to Report, and When to Ask Questions First
Let’s be clear: if a child presents with an STD that strongly suggests sexual transmission, especially after infancy, reporting is mandatory. These include:
- Chlamydia or gonorrhea in a child over one year old
- Genital herpes with no oral symptoms or family exposure history
- HPV/genital warts in pre-teens without perinatal history
In these cases, pediatricians are required to follow child protection laws and may involve CPS, forensic interviews, and trauma-informed evaluations. This is not about punishment, it’s about protection.
But for borderline or ambiguous cases, oral herpes, hepatitis B, or HPV with no signs of trauma, many states allow discretion. Doctors can consult child abuse pediatricians or multidisciplinary teams before reporting. You can request this if you feel the case warrants a careful look instead of a knee-jerk reaction.
Sometimes the most powerful thing you can say in a tense moment is:
“I’m open to anything that protects my child. But I also want to understand all medical possibilities before assuming abuse.”
Your Next Step Might Be Simpler Than You Think
Whether you’re navigating a new diagnosis or a creeping fear that won’t go away, remember: you’re not alone. The majority of pediatric STDs are treatable, and many are survivable, medically and emotionally.
Don't wait in fear. If you have questions about your child’s exposure, symptoms, or risk factors, testing is one of the clearest ways to get answers. And in the privacy of your home, you can begin without judgment or delay.
Order a discreet combo test kit to screen for common STDs in one step. It’s fast, accurate, and doesn’t require clinic access.
FAQs
1. Can kids really get herpes without anything bad happening?
Yes, it's more common than you think. Oral herpes (HSV-1) often shows up in childhood and is usually passed on from a loving kiss, not a crime. Grandma kisses the baby, baby ends up with a cold sore six months later. That’s how sneaky this virus can be. It doesn’t mean abuse, it means someone had herpes and didn’t know they were contagious.
2. Are cold sores actually considered STDs?
Technically? Sometimes, yes. The herpes virus that causes cold sores can also cause genital herpes. But in kids, cold sores usually come from innocent contact, family kisses, shared cups, or daycare drool fests. So while the virus falls under the “STD” umbrella, how a child gets it usually has nothing to do with sex.
3. Could my child get an STD just from being born?
Absolutely. That’s called vertical transmission. If a parent has certain STDs during pregnancy or birth, like chlamydia, gonorrhea, or hepatitis B, the baby can be exposed during delivery. It’s one of the big reasons we test pregnant people for STIs before birth. If your child tests positive and you had a known or unknown infection during delivery, that could explain it.
4. Do I have to call CPS if my child has a positive test?
Short answer: Not necessarily. Some STDs do require mandatory reporting, especially in older children. But if your toddler gets diagnosed with oral herpes or hepatitis B, your doctor may decide it doesn’t need to be reported. It all depends on the infection, the child’s age, and the full medical picture. Ask questions. You have a right to understand the process.
5. Is HPV something my kid could catch from a towel or toy?
In theory, yes. HPV is mostly spread through skin-to-skin contact, but there have been a few cases where it was spread through things like bath toys or diaper tables that were dirty. It's not common, but it can happen. That's why things that are shared in group care settings should be cleaned often. It's not about being scared; it's about good hygiene.
6. Is there a way to test my kid at home without making it a big deal?
For young children, most STD testing happens at the doctor’s office. But if you’re a caregiver who just wants to check yourself (or an older teen in your home), at-home STD kits are discreet and quick. Sometimes the best first step is testing yourself, so you can rule out household transmission before diving into worst-case scenarios.
7. What if my kid has an STD and no one knows how they got it?
You’re not alone. This happens. Start by asking your doctor for every possible explanation, birth, contact, exposure. If the answers still feel unclear, you can request a child abuse pediatrician or a multidisciplinary team to review everything with care. You’re allowed to ask for a second opinion, especially when the stakes are emotional and high.
8. Can my kid still go to school or daycare with an STD?
Most of the time, yes. Unless they’re showing active symptoms like weeping sores or contagious warts, many STDs don’t require exclusion. But every infection is different. Kids with herpes, for example, might need to stay home during an outbreak, just like with pink eye. Ask your provider. And don’t let stigma keep your child from a normal routine.
9. Is sharing bath toys or towels really a risk?
For most viruses, the risk is low, but not zero. Think about it like this: if a kid has a wart-causing HPV strain and bathes with shared toys, there's a tiny chance another kid could be exposed, especially if they have a cut. It’s not something to panic over, but it is a good reason to keep bath items personal when you can.
10. My child tested positive for chlamydia. Does that always mean abuse?
This one’s tough. In children past infancy, chlamydia and gonorrhea are red flags and must be taken seriously. These aren’t infections that spread by kissing or towels. If your child tests positive for one of these and wasn’t exposed during birth, your medical team is required to investigate. That can feel terrifying, but the goal is always protection, not punishment.
What Comes Next Is Knowledge, Not Panic
You don’t need to have all the answers today. What matters is that you’re asking the right questions. If you’re scared, overwhelmed, or confused about a child’s STD diagnosis, remember: facts, not fear, should guide your next step.
Testing is information. Treatment is healing. And stigma has no place in medical care.
Take back your peace of mind, confidentially. This at-home combo test kit screens for the most common STDs quickly and privately. Because protecting your family includes protecting yourself from shame-based silence.
How We Sourced This Article: We combined current guidance from leading medical organizations with peer-reviewed research and lived-experience reporting to make this guide practical, compassionate, and accurate. In total, around fifteen references informed the writing; below, we’ve highlighted some of the most relevant and reader-friendly sources.
Sources
1. NHS – Genital Warts Overview
2. Herpes Simplex Virus (HSV) – CDC
5. What Causes HSV (Herpes Simplex Virus) Keratitis (Eye Infection) – CDC
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He blends clinical precision with a no-nonsense, sex-positive approach and is committed to expanding access for readers in both urban and off-grid settings.
Reviewed by: Sarah J. Lin, NP-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.