Swollen Lymph Nodes in Groin: STD or Something Else?
Quick Answer: Most mouth ulcers are canker sores, irritation, or minor injuries. STDs like herpes or syphilis can cause oral sores, but they usually have distinct patterns, timing, or accompanying symptoms that set them apart.
First, Breathe: Most Mouth Sores Are Not STDs
I’ve sat across from patients who whisper, “I think I ruined my life,” while pointing to a tiny ulcer on their inner cheek. Nine times out of ten, it’s a canker sore triggered by stress, biting the cheek during sleep, spicy food, or even hormonal shifts. The mouth is delicate tissue. It reacts to friction and inflammation fast.
Common non-STD causes of mouth ulcers include aphthous ulcers (canker sores), accidental trauma, dental irritation, vitamin deficiencies, immune stress, and even emotional burnout. Your immune system lives in your mouth. When it’s under pressure, it shows up there.
But here’s where nuance matters: some STDs absolutely can appear in the mouth. Herpes simplex virus (HSV-1 or HSV-2) and syphilis are the two primary infections that cause oral sores. Less commonly, gonorrhea or chlamydia can infect the throat, though those usually don’t cause visible ulcers.
This is not about assuming the worst. It’s about understanding patterns.
People are also reading: Eye Infection After Sex: Can STDs Infect Your Eyes?
What a “Normal” Canker Sore Usually Looks and Feels Like
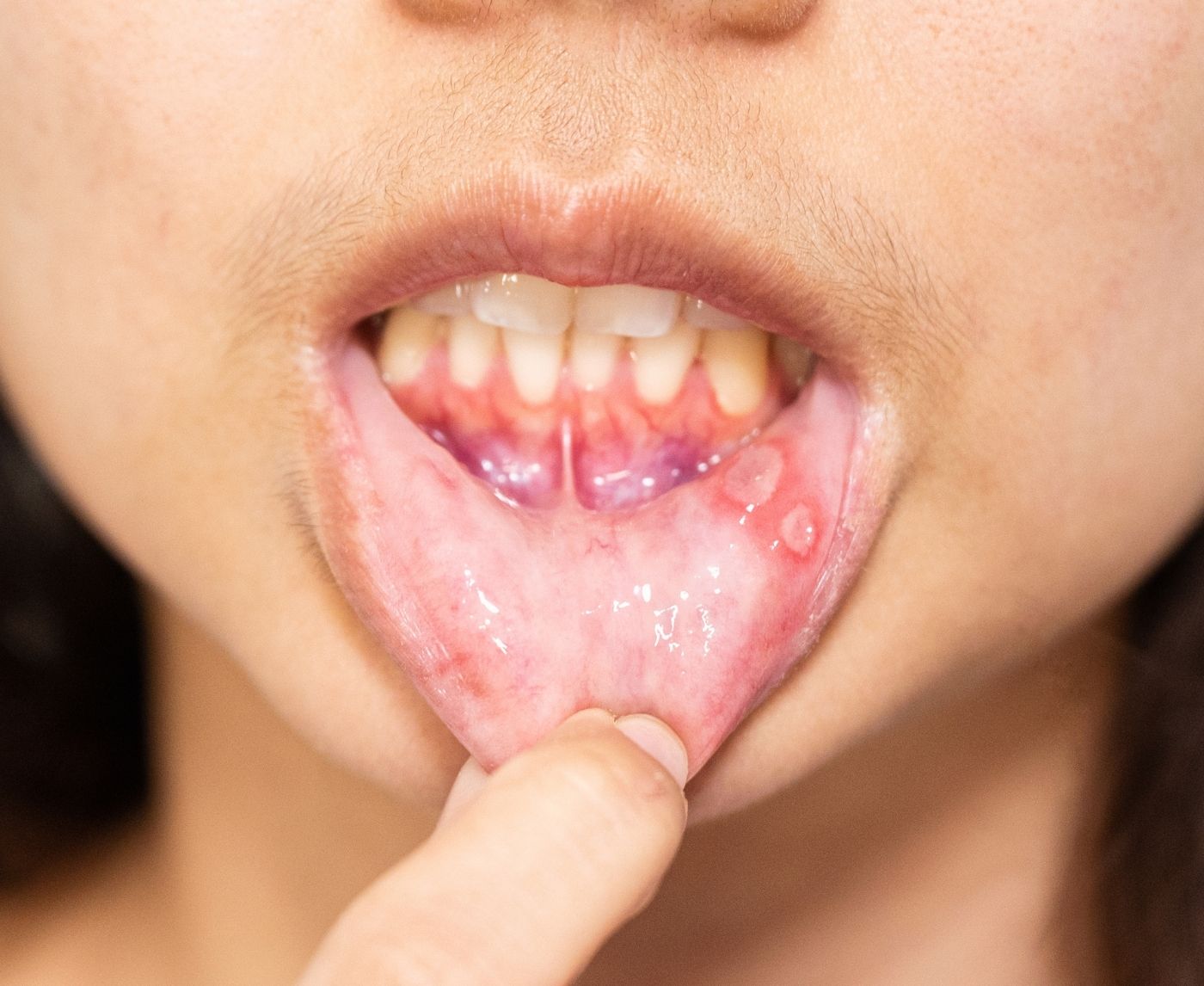
A classic canker sore is small, round or oval, and shallow. It usually has a white or yellow center with a red border. It forms on soft tissue, inside the lips, under the tongue, or along the inner cheeks. It hurts when you eat acidic food. It feels tender when your tongue brushes against it.
It does not start as a blister. It does not cluster. It does not appear on the outside of the lips. And it usually heals on its own within 7 to 14 days without scabbing.
One patient, Amina, told me, “It stings every time I drink orange juice, but it’s just one spot.” That detail matters. Single. Painful. Inside the mouth. Those are reassuring signs.
Canker sores are not contagious. They are not sexually transmitted. They are inflammatory, not infectious in the STD sense.
When an Oral Sore Might Be Herpes
Oral herpes often behaves differently. Instead of a single shallow ulcer appearing out of nowhere, herpes typically starts with tingling, itching, or burning before anything visible shows up. Then small fluid-filled blisters form. These blisters can cluster together before rupturing into painful sores.
Unlike canker sores, herpes lesions often occur on the border of the lips, what people call “cold sores.” They can also appear inside the mouth, especially during a first outbreak, but they tend to look like grouped lesions rather than one isolated crater.
Timing matters too. A first oral herpes outbreak often appears 2 to 12 days after exposure. It may come with fever, swollen lymph nodes, body aches, or general fatigue. If your sore appeared months after your last sexual encounter, it’s less likely to be a brand-new herpes infection and more likely to be a reactivation of a virus many adults already carry.
Yes, that’s another important piece: a huge portion of adults already have HSV-1, often acquired in childhood through non-sexual contact. Not every cold sore equals a recent sexual exposure.
When an Oral Sore Might Be Syphilis
Syphilis behaves differently from both canker sores and herpes. The first-stage lesion, called a chancre, is usually firm, round, and painless. That painless detail is the one people miss. It doesn’t sting like a canker sore. It doesn’t blister like herpes. It just sits there.
It may appear on the lips, tongue, or inside the mouth if the infection was transmitted through oral sex. It typically shows up about three weeks after exposure, though the window can range from 10 to 90 days.
Because it’s painless, many people ignore it. They assume it’s a minor irritation. Then it disappears on its own within a few weeks. That disappearance does not mean the infection is gone. Syphilis progresses internally without treatment.
If you have a single, firm ulcer that doesn’t hurt and you had unprotected oral sex in the past month or two, that is a moment to test, not panic, but test.
Side-by-Side Comparison: STD vs Non-STD Mouth Ulcers
Figure 1. Visual and symptom comparison of common oral ulcers.
What About Gonorrhea or Chlamydia in the Throat?
This is where Google can mislead you. Oral gonorrhea and chlamydia infections usually affect the throat, not the lips or inner cheeks. They often cause sore throat, mild redness, or no symptoms at all. They rarely cause visible ulcers.
So if you’re staring at a white ulcer on your tongue and spiraling, it’s unlikely to be throat gonorrhea. That infection tends to hide deeper in the pharynx and often requires a swab test to detect.
Still, if you had unprotected oral sex and are worried about “oral STD symptoms,” a throat swab test can provide clarity. Anxiety fades faster when you have real data.
Timing After Oral Sex: When to Actually Test
If your mouth sore appeared the very next morning after oral sex, it is almost certainly not a newly acquired STD. Most sexually transmitted infections have incubation periods measured in days or weeks, not hours.
Herpes usually appears within 2–12 days. Syphilis typically appears around 3 weeks after exposure. Gonorrhea and chlamydia throat infections can show up within a week, but again, they rarely cause ulcers.
If you’re inside those windows and something looks unusual, especially painless or blister-like lesions, testing is reasonable. If you’re far outside those windows and the sore looks classic for a canker ulcer, monitoring for 10–14 days is often appropriate.
And if you don’t want to sit in uncertainty, you can explore discreet testing options through STD Test Kits. Knowing beats guessing.
Red Flags That Warrant Immediate Medical Care
Most mouth ulcers are minor. But there are times when waiting is not the right move. If you have difficulty swallowing, high fever, rapidly spreading lesions, or sores that last longer than three weeks without healing, you need a clinician to look at it.
Also, if you notice rash on the palms or soles alongside a mouth sore, that combination can signal secondary syphilis. That is not a wait-and-see scenario. That is a test-and-treat scenario.
Your body is not trying to betray you. It’s signaling. The key is reading the signal correctly.
People are also reading: Can You Have an STD in Your Rectum Without Symptoms?
Why Your Brain Goes Straight to “STD” (Even When It’s Not)
Let’s talk about the psychology for a second. You have a new partner. Or a recent hookup. Or maybe just a moment that felt vulnerable. Then a sore appears. The human brain is wired to connect recent events to new symptoms. It tries to protect you by assuming the most threatening explanation.
I’ve heard it countless times: “It has to be from that night.” But stress alone can trigger canker sores. So can lack of sleep. So can biting your lip during anxious dreaming. The mind fills in blanks when it feels guilt, fear, or uncertainty.
This doesn’t mean you’re irrational. It means you care. But caring works best when it’s paired with accurate information instead of shame spirals.
Less Common Causes of Mouth Ulcers That Aren’t STDs
There’s a long list of things that can inflame the lining of your mouth. Nutritional deficiencies, especially low vitamin B12, iron, or folate, are common culprits. So are autoimmune conditions like Behçet’s disease, though that’s rare and usually involves recurring ulcers plus other systemic symptoms.
Food sensitivities can create small, painful lesions. So can harsh toothpaste ingredients like sodium lauryl sulfate. Even dental braces or a rough tooth edge can repeatedly irritate the same spot until an ulcer forms.
If you get frequent mouth ulcers during periods of high stress, that pattern itself is diagnostic. Your immune system flares when you’re overwhelmed. It doesn’t mean infection. It means inflammation.
How Long Do STD-Related Mouth Sores Last?
This question shows up in search data constantly: “how long do STD mouth sores last?” The timeline can be clarifying.
A primary oral herpes outbreak can last two to three weeks, especially the first episode. Recurrent cold sores are usually shorter, often healing within 7 to 10 days. They scab over before fully resolving if located on the lips.
A syphilis chancre may linger for three to six weeks before disappearing, even without treatment. That disappearance can create false reassurance. The infection, however, continues progressing internally if untreated.
Canker sores typically heal within two weeks and do not leave scars. If your sore has been present for more than three weeks, regardless of STD concern, that alone warrants medical evaluation.
Decision Guide: Monitor or Test?
Figure 2. Practical decision framework for oral sores.
Testing Without Panic
Testing is not an admission of wrongdoing. It’s a data point. If you’re within the testing window and something feels off, clarity is empowering. You can explore discreet options at STD Test Kits, including combination panels that screen for common infections in one go.
For example, if your concern involves possible syphilis exposure after oral sex, a blood-based rapid test can provide preliminary answers quickly. If you’re concerned about herpes, understanding the difference between lesion swab testing and blood antibody testing matters, timing changes accuracy.
You don’t have to test for everything blindly. You test based on exposure type, symptom pattern, and timing. That’s informed action, not fear.
“I Thought It Was Herpes”
Javier, 27, came in convinced he had contracted herpes after a new relationship began. He noticed a small white ulcer under his tongue four days after oral sex. “It felt like punishment,” he told me. He hadn’t slept for two nights.
The lesion was singular, shallow, and painful to the touch. No blisters. No clusters. No fever. The timing was too fast for a new herpes infection. We monitored it. It healed in nine days. No scabbing. No recurrence.
He exhaled in my office like someone who had been holding their breath underwater. The ulcer wasn’t an STD. It was stress, the kind that shows up when vulnerability feels risky.
What If It Keeps Happening?
Recurring mouth sores can mean different things. Recurrent cold sores tend to appear in the same general location on the lip border and may flare during stress or illness. Canker sores can also recur, especially if you’re prone to them.
If ulcers appear frequently, consider tracking triggers: sleep deprivation, menstrual cycles, new foods, intense anxiety periods. Patterns tell stories that single episodes cannot.
And if outbreaks are frequent, severe, or accompanied by systemic symptoms like rash, joint pain, or eye irritation, that’s when a healthcare provider should evaluate for underlying conditions beyond STDs.
You’re Allowed to Ask This Question
There is nothing shameful about typing “mouth ulcer or STD” into a search bar. It means you’re paying attention. It means you want to protect yourself and your partners. That’s maturity, not guilt.
Sex-positive health care isn’t about assuming every symptom is sexually transmitted. It’s about recognizing that oral sex is common, kissing is intimate, and infections sometimes happen, and when they do, they’re medical conditions, not moral verdicts.
If your anxiety is louder than your logic right now, pause. Look at the characteristics. Look at the timing. Use the tables above. Then choose a plan: monitor, test, or see a clinician. Clarity beats catastrophizing every time.
If It’s an STD, What Happens Next?
Let’s say you test and it turns out to be something like herpes or syphilis. The first thing I want you to hear is this: both are manageable. One is treatable and curable with antibiotics. The other is manageable with antiviral medication. Neither is a life sentence of isolation.
If it’s oral herpes, antiviral medications can shorten outbreaks and reduce transmission risk. Many people live full, dating, kissing, relationship-filled lives with HSV. It becomes a health condition you manage, like migraines or eczema, not a definition of who you are.
If it’s syphilis, early treatment with antibiotics is highly effective. The key is catching it during early stages. That’s why painless oral sores that appear weeks after exposure deserve attention instead of dismissal.
And if it’s not an STD? You get to unclench your jaw. That relief matters too.
The Difference Between “Possible” and “Probable”
One of the most important distinctions in medicine is the gap between what is possible and what is probable. Yes, STDs can cause mouth sores. That is medically accurate. But probability depends on exposure type, timing, symptom pattern, and risk factors.
A single painful ulcer inside the cheek that appeared overnight with no systemic symptoms is possible as herpes, but not probable. A firm painless ulcer that appears a month after unprotected oral sex is both possible and more probable for syphilis.
Learning that difference prevents over-testing when unnecessary and under-testing when it matters.
When Kissing Is the Question
Another search that shows up constantly: “Can you get an STD from kissing?” The honest answer is nuanced.
Herpes (HSV-1) absolutely spreads through mouth-to-mouth contact. It does not require sexual intercourse. That’s why many people acquire it in childhood from relatives. So if you develop a cold sore after kissing someone, it may not even be new exposure, it could be reactivation.
Syphilis can spread through direct contact with a chancre, including during deep kissing if a lesion is present. That scenario is far less common than herpes transmission but biologically possible.
Gonorrhea and chlamydia are rarely transmitted through kissing alone. They typically require oral-genital contact.
So yes, transmission through kissing is possible in specific cases, but it’s not the universal threat the internet sometimes makes it sound like.

People are also reading: Is That a Pimple, Herpes, or a Genital Wart?
Reducing Anxiety While You Wait
Waiting for a sore to heal or for test results to return can feel unbearable. The mind invents outcomes. It replays encounters. It magnifies small details. That’s human.
Here’s something grounding: most STDs do not explode into catastrophic illness overnight. Even untreated syphilis progresses over months to years. That doesn’t mean ignore symptoms. It means you have time to respond rationally instead of reactively.
If testing would calm your nervous system, that’s a valid reason to test. You can explore discreet combination panels, including options that screen for syphilis and other common infections, through the STD Test Kits homepage. Your results are private. Your timeline is yours.
Practical Self-Check Before You Spiral
Before assuming the worst, pause and assess four variables: pain level, blistering pattern, timing after exposure, and duration so far. Those four clues tell more than fear ever will.
Is it painful? That leans toward canker sore or herpes. Is it painless and firm? That leans toward syphilis. Did it appear less than 24 hours after oral sex? That timing argues strongly against a newly acquired STD.
And most importantly: is it healing? Healing is reassuring. Progression, spreading, or systemic symptoms are signals to escalate care.
The Role of Testing Windows
If you decide to test, timing improves accuracy. Blood tests for syphilis are most reliable several weeks after exposure. Herpes blood antibody tests also require time for antibodies to develop. Testing too early can produce false reassurance.
This is where people get tripped up. They test at day three, see a negative result, and assume everything is fine. But certain infections need time to become detectable. If you’re inside the early window, a follow-up test may be recommended.
Testing isn’t just about the sore in front of you. It’s about matching the right test to the right timeline.
Stigma Makes Everything Louder
There’s a reason a tiny mouth ulcer can feel emotionally catastrophic. STDs carry social weight. They trigger fear of judgment, rejection, or self-blame. Even when the sore is unrelated, that stigma amplifies anxiety.
I want to be clear: getting an STD does not mean you were careless, reckless, or irresponsible. Oral sex is common. Kissing is intimate. Humans connect. Infections are biological events, not character flaws.
Separating symptom analysis from moral panic is one of the healthiest moves you can make.
If You’re Still Unsure
Uncertainty doesn’t make you weak. It makes you human. If your sore doesn’t clearly match the reassuring canker profile and it doesn’t clearly match classic herpes or syphilis patterns either, that gray zone is exactly what medical evaluation is for.
You can choose in-person care. Or you can begin with at-home screening to rule out common infections. For example, combination testing panels available through this at-home combo STD test kit can screen for multiple infections discreetly.
Clarity is empowering. Guessing is exhausting.
FAQs
1. I had oral sex and now I have a mouth ulcer. Be honest, how worried should I be?
Honest answer? It depends on timing and texture, not just the fact that sex happened. If the sore popped up the very next morning, that’s almost never how a new STD behaves. If it’s a single painful crater inside your cheek and it stings when you drink orange juice, that leans heavily toward a canker sore. If it’s a painless, firm ulcer that appeared weeks after unprotected oral sex, that’s when we move from “probably nothing” to “let’s test and be smart about this.”
2. What’s the one detail people miss when trying to tell herpes from a canker sore?
The blister phase. Herpes usually starts with tingling, then tiny fluid-filled blisters before they break open. Canker sores don’t blister first. They just show up as shallow ulcers. If you never saw blisters, and it’s inside the soft tissue of your mouth, that’s reassuring.
3. If it doesn’t hurt, is that better or worse?
Counterintuitive, but painless can be more concerning in specific situations. A syphilis chancre is often firm and painless. A canker sore, on the other hand, usually hurts. Pain alone doesn’t diagnose anything, but “completely painless and firm” plus recent exposure is a combination worth testing for syphilis.
4. Can stress really cause mouth ulcers, or is that just something doctors say?
It’s real. I’ve watched finals week, breakups, job interviews, and family drama show up as mouth ulcers more times than I can count. Stress alters immune signaling in the mouth. That doesn’t mean every sore is stress, but yes, your nervous system absolutely talks to your oral tissue.
5. If I already had HSV-1 as a kid, could this still be herpes?
Yes, but it wouldn’t be “new.” Many adults carry HSV-1 from childhood exposure. Stress, illness, or lack of sleep can reactivate it as a cold sore. That can feel scary if you recently kissed someone new, but the timing may be coincidence rather than fresh transmission.
6. Do throat STDs cause visible ulcers?
Usually no. Throat infections with gonorrhea or chlamydia often cause mild soreness or no symptoms at all. They don’t typically create dramatic white ulcers on your tongue. So if you’re staring at a visible sore in the mirror, that pattern doesn’t scream throat STD.
7. If the sore heals in a week, can I relax?
In many cases, yes. Canker sores heal within 7–14 days and disappear completely. Recurrent herpes lesions also heal, though they may come back later. The one exception is syphilis, where a sore can vanish without treatment while the infection continues internally. If exposure risk was real and the lesion matched that painless profile, testing still makes sense even if it healed.
8. Is it dramatic to test “just in case”?
Not at all. Testing isn’t drama. It’s data. If knowing your status will help you sleep tonight, that’s reason enough. The key is choosing the right test at the right time, not panic-testing on day two and assuming a negative means you’re bulletproof.
9. Why does this feel so emotionally intense over something so small?
Because mouth sores are visible. Because sex is vulnerable. Because STDs carry stigma. A tiny ulcer becomes symbolic. That doesn’t make you irrational. It makes you human. The goal is to separate biology from shame.
10. What’s the smartest next move if I’m still unsure?
Look at the pattern. Check the timeline. If something feels off, especially painless, persistent, or paired with other symptoms, test. If it looks and behaves like a classic canker sore, monitor it for two weeks. And if anxiety is louder than logic, get the data and reclaim your peace.
You Deserve Clarity, Not Catastrophe
A mouth ulcer is not a moral judgment. It is a symptom with a differential diagnosis. Most mouth ulcers are harmless, transient, and have nothing to do with STDs. Some require testing and treatment. The distinction is in pain distribution, time of onset, characteristics of the ulcer, and the patient's exposure history.
If you’re unsure, don’t let fear make the decision for you. Make it from a place of information. Explore discreet, medically guided options at this at-home combo STD test kit or browse resources at STD Test Kits. Your health is data-driven, not drama-driven.
How We Sourced This Article: The guide was developed based on existing clinical guidelines from the CDC, Mayo Clinic, and other peer-reviewed articles on infectious disease. We also used epidemiologic data on the transmission of oral herpes, stages of syphilis, and differential diagnoses for aphthous ulcers. We included narratives based on real-life experiences to mirror anxiety patterns while keeping the content accurate and evidence-based. There were about fifteen sources used for this article, and six of these key sources are listed below.
Sources
1. Mayo Clinic – Canker Sore Overview
4. Herpes simplex virus | World Health Organization
5. Canker sore - Symptoms and causes | Mayo Clinic
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works to stop, diagnose, and treat STIs. He uses a sex-positive, stigma-free approach along with clinical accuracy to help patients make smart choices about their health.
Reviewed by: L. Ramirez, PA-C | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.