Think You Have HIV? Why Testing Too Early Can Backfire
Quick Answer: The King County study shows syphilis is increasingly spreading among heterosexual adults, meaning anyone sexually active, regardless of orientation, should consider timely testing. At-home syphilis blood tests can detect infection during the antibody window period, typically becoming reliable about 3–6 weeks after exposure.
The study, published in Sexually Transmitted Diseases and available through the National Institutes of Health’s PubMed Central, documents a measurable epidemiologic shift. While syphilis rates among men who have sex with men remain high, heterosexual transmission in King County increased substantially over the study period, especially among women of reproductive age. That matters because untreated syphilis during pregnancy can lead to congenital infection, a preventable but devastating outcome.
This article builds on that research. We’re going to move beyond the headlines and into what this means for you: how syphilis spreads, what symptoms actually look like in real life, when to test after exposure, how window periods affect results, and how at-home testing fits into modern prevention. No moral panic. No shaming. Just clear steps.

People are also reading: Do Men and Women Need Different STD Tests? What Actually Changes (And What Doesn’t)
What Changed? The Epidemiology Is Shifting
For years, public health messaging around syphilis focused primarily on men who have sex with men. That focus was evidence-based at the time. But epidemics evolve. According to the King County data, heterosexual men and women, many without traditional “high-risk” labels, are now accounting for a growing share of early syphilis diagnoses.
The study identified increases in cases associated with methamphetamine use, opioid use, housing instability, and overlapping sexual networks. These are not fringe factors. They are social realities that shape risk across communities. The result is spillover transmission that affects people who may not perceive themselves at risk.
And here’s the uncomfortable truth: syphilis does not care about how you identify. It cares about exposure.
When an infection begins expanding into new demographic groups, it often spreads silently for a while. Syphilis is particularly good at that. Early symptoms can be painless. Secondary symptoms can mimic other illnesses. And latent stages can show no signs at all while the bacteria remain active in the body.
This is why relying on “I would know” is risky.
Syphilis Symptoms: Subtle, Staged, and Often Missed
Let’s talk about what syphilis actually feels like, not in textbooks, but in real life.
A person might notice a small sore after sex. It doesn’t hurt. It doesn’t itch. It looks almost harmless. That’s primary syphilis. The sore, called a chancre, can appear on the genitals, anus, mouth, or even inside the vagina where it’s not visible. It heals on its own in a few weeks. Many people never connect it to an STD.
Weeks later, they might develop a rash. Sometimes it appears on the palms of the hands or soles of the feet. Sometimes it’s faint and easy to dismiss. They might feel tired, slightly feverish, or swollen in the lymph nodes. Then that fades too.
The infection doesn’t disappear. It simply moves into a latent stage.
According to the Centers for Disease Control and Prevention, untreated syphilis can eventually damage the brain, nerves, eyes, heart, and other organs years later. But long before that, it can be transmitted to partners or passed during pregnancy.
The King County data underscore something important: many heterosexual adults diagnosed with syphilis did not present with dramatic symptoms. They were diagnosed through screening, pregnancy testing, or after a partner tested positive.
Which brings us to testing windows.
Window Periods and Why Timing Is Everything
Syphilis testing typically detects antibodies in the blood. That means your immune system has to respond before the test turns positive. If you test too early, you can receive a false negative, not because you’re fine, but because your body hasn’t produced enough detectable antibodies yet.
The antibody window period for syphilis is usually about 3 to 6 weeks after exposure. In some cases, detection may occur slightly earlier or later depending on immune response.
In the context of the accelerating heterosexual epidemic, this matters. If you had a new partner and feel fine two weeks later, that does not rule out infection. A negative result too early can create false reassurance.
This is where at-home blood-based rapid tests become powerful. They allow discreet screening without waiting weeks for a clinic appointment. If timing is borderline, you can retest at the optimal window without logistical barriers.
If your exposure was recent and your mind won’t settle, you can explore discreet options at STD Test Kits. For targeted screening, a dedicated syphilis rapid test kit provides private blood-based detection aligned with antibody timing.
How At-Home Syphilis Testing Fits Into a Changing Epidemic
When epidemiology shifts, access has to shift with it. The King County data show that heterosexual transmission is rising in populations that may not routinely seek STI screening. Some are working multiple jobs. Some are uninsured. Some assume syphilis “isn’t something straight people get.” That assumption is now outdated.
At-home testing does not replace clinics. It expands reach. It lowers friction. It gives someone who feels exposed but embarrassed, or simply busy, the ability to test without navigating waiting rooms or insurance portals. In an accelerating epidemic, speed and privacy are not luxuries. They are containment tools.
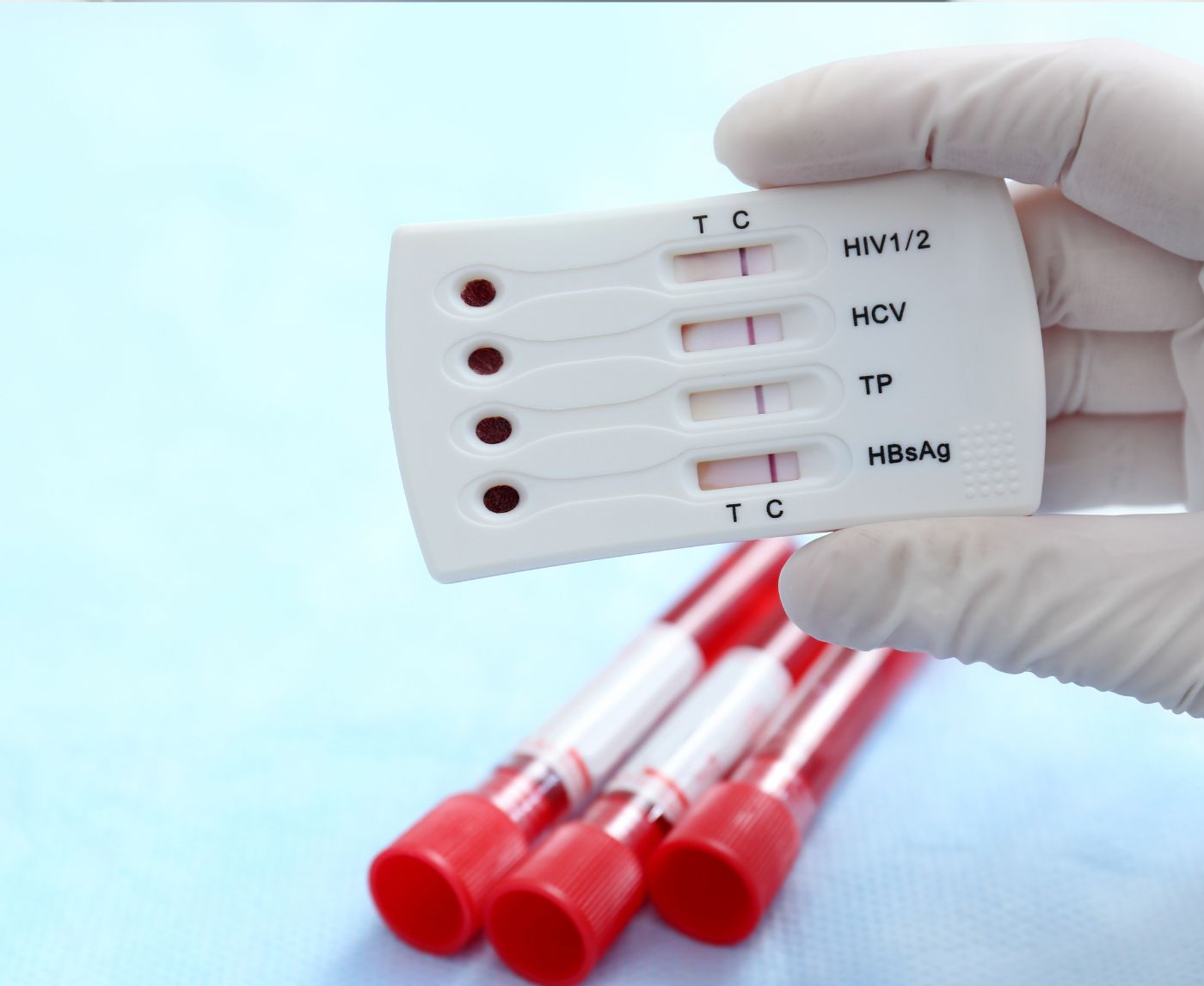
A rapid blood-based syphilis test detects antibodies using a small fingerstick sample. The process is similar to checking blood sugar. Results appear within minutes. While confirmatory lab testing may be recommended for positive results, rapid screening allows earlier identification than waiting months for routine checkups.
According to the World Health Organization, early detection and treatment of syphilis prevents long-term complications and reduces transmission risk. That includes preventing congenital infection. Every earlier diagnosis interrupts a chain.
If you're feeling unsure after getting a new partner, especially during the 3–6 week antibody window, a discreet at-home option can help. The Syphilis Test Kit lets you get tested in private at the right time, as advised. If you are at risk for more than one infection, a combo panel that tests for syphilis, HIV, chlamydia, and gonorrhea may be a good idea.
This isn’t alarmism. It’s adjustment.
Who Should Consider Testing Now?
Not everyone needs to panic. But certain scenarios deserve attention, especially in light of rising heterosexual transmission.
If you’ve had a new sexual partner in the past two months and haven’t tested, you fall into a reasonable screening window. If a condom broke. If you had oral sex without protection and noticed a painless sore afterward. If a partner tells you they tested positive for syphilis. If you’re pregnant or planning pregnancy. These are not fringe situations. They are ordinary human moments.
The King County study highlighted increased diagnoses among women of reproductive age. That intersects directly with congenital syphilis risk. According to the CDC treatment guidelines, syphilis during pregnancy can lead to miscarriage, stillbirth, or neonatal infection if untreated. Screening during pregnancy is standard because timing matters. Early treatment is highly effective.
But beyond pregnancy, heterosexual adults without symptoms are also testing positive. That is the subtle part of this shift. Many infections are detected during routine screening rather than symptom-driven visits.
Testing is not an accusation. It is maintenance.
Rapid Test vs Lab Test: Accuracy in Context
There’s a persistent misconception that at-home tests are inherently unreliable. That’s not accurate. What matters is test type, timing, and follow-up.
Traditional laboratory syphilis screening often uses a combination of treponemal and non-treponemal blood tests to confirm diagnosis. Rapid tests typically detect treponemal antibodies. When used within the appropriate window period, they demonstrate high sensitivity and specificity, though confirmatory testing is recommended after a positive result.
If you need immediate reassurance while waiting for a clinic appointment, a rapid test provides early screening data. If you test positive, confirmatory testing ensures staging and appropriate treatment. If negative but tested early, retesting at six weeks closes the window.
The accelerating heterosexual epidemic means more people outside traditional screening patterns may benefit from low-barrier testing access. When detection expands, transmission slows.
Why Congenital Syphilis Is Part of This Story
Another concern that people are worried about these days is not only an increase in heterosexual syphilis but also an increase in congenital syphilis. As syphilis continues to spread among women who are capable of bearing children, pregnancy outcomes are also being considered.
When congenital syphilis occurs, it means that the pregnant woman has infected her unborn baby. The effects of this may be premature birth, developmental problems, or even death. However, the good news is that it can be stopped in its tracks.
The King County study indicates that this increase is not occurring in isolation. It is part of other issues, including poor social support systems, housing instability, drug use, and poor prenatal care. Access to tests is not only about an individual’s health but also about the health of the entire community.
If you are pregnant, planning to become pregnant, or are sexually active but overdue for tests, tests should be seen as a form of protection, not punishment. Protection leads to treatment, which leads to prevention.

People are also reading: Herpes in the Eye: What Ocular HSV Really Looks Like
When to Test After Exposure , A Calm, Practical Timeline
You had sex. Maybe it was new. Maybe it was someone you trust. Maybe a condom broke. Maybe it didn’t. A few days later, your brain starts replaying it. You Google “syphilis symptoms in women” or “how long does syphilis take to show up.” You scroll. You spiral.
Let’s slow this down.
If exposure was within the last two weeks, testing today may not give you a definitive answer. The bacteria that causes syphilis, Treponema pallidum, triggers an antibody response that typically becomes detectable between three and six weeks after infection. Testing earlier can miss it.
That does not mean do nothing. It means plan.
If it has been three to six weeks since exposure, a blood-based test becomes increasingly reliable. If it has been six weeks or more, most screening tests reach high accuracy for detecting antibodies. If symptoms appear at any time, a painless sore, a rash on palms or soles, testing should not wait.
Here’s what this looks like in real life.
Daniel, 32, had a new partner while traveling for work. Two weeks later, he felt fine but couldn’t shake anxiety. He tested early and got a negative result. At week five, he retested. This time it was positive. Because he caught it in early stages, treatment was straightforward and highly effective.
Testing early isn’t foolish. It’s human. Just don’t let an early negative become your final answer if timing was premature.
What Happens If You Test Positive?
Syphilis can be cured. The treatment for syphilis in its early stages involves a single injection of benzathine penicillin G. This is according to the treatment guidelines provided by the CDC. The treatment for syphilis in its later stages involves additional injections. The issue here is not the patient’s shame or identity. The issue is the time of diagnosis.
If your rapid test for syphilis comes back positive, a confirmatory test will be necessary. This is not a failure of the rapid test. This is how all infectious disease tests work. A screening test identifies risk. A confirmatory test directs treatment.
You will be asked to notify recent sexual partners. This conversation can be as bad as the diagnosis. But notifying partners prevents reinfection and protects others from unwittingly spreading syphilis and infecting others. Many health departments provide anonymous partner services for those who find this conversation too overwhelming.
The sooner syphilis is treated, the lower the risk of complications. The complications of untreated syphilis can be severe. They can involve the nervous and cardiovascular systems and other organs. These complications are preventable.
If you are at home and receive a positive result for syphilis, do not just sit alone with this information. Use the data.
Retesting, Reinfection, and Ongoing Risk
After treatment, follow-up blood tests are typically recommended to confirm declining antibody titers over time. This is how clinicians verify treatment success. Retesting is not punishment, it’s documentation that the therapy worked.
If you remain in a network where exposure risk continues, multiple partners, overlapping relationships, or community clusters like those identified in the King County study, periodic screening may be appropriate. For some individuals, that might mean every three to six months.
Reinfection is possible. Treatment clears current infection, but it does not create immunity. This is a biological reality, not a moral one.
For individuals who want proactive monitoring without repeated clinic visits, discreet home-based options reduce barriers. Whether that means a single infection screen or a broader panel, accessible testing supports ongoing sexual health autonomy.
Breaking the “That’s Not My Risk Group” Myth
The most powerful takeaway from the King County data is not just that rates increased. It’s that perception lagged behind reality.
Many heterosexual adults diagnosed with syphilis did not view themselves as part of a high-risk population. Some were in long-term relationships. Some had few lifetime partners. Some had no symptoms at all. Epidemiology doesn’t follow stereotypes.
The phrase “can heterosexuals get syphilis?” is being searched more frequently for a reason. The answer is yes. Transmission depends on exposure to an infected partner, not sexual orientation. As sexual networks intersect, infections move.
This is not about labeling. It’s about updating mental models. If the epidemic is expanding, screening strategies must expand with it.
Why Early Detection Protects More Than Just You
Syphilis transmission often occurs during early stages when sores or rashes are present, but infection can also spread when symptoms are subtle or unnoticed. Identifying infection early interrupts transmission chains that might otherwise reach multiple partners.
In public health terms, early detection reduces reproductive number. In personal terms, it protects the people you care about.
Testing is not distrust. It’s stewardship.
If you’re weighing whether to test after a new exposure, especially in light of rising heterosexual transmission trends, consider proactive screening. A discreet at-home syphilis rapid test kit provides private results in minutes. If your risk profile spans multiple infections, broader panels are available. Your results are yours. Your timing is yours.
FAQs
1. Wait… I’m straight. How did syphilis even become my problem?
That’s the exact reaction many people in the King County study had. For years, public health messaging focused on specific groups, so a lot of heterosexual adults assumed they were outside the risk zone. But infections follow exposure, not identity labels. If someone in your sexual network is infected, even unknowingly, it can reach you. This isn’t about orientation. It’s about biology and timing.
2. If I only had one partner, do I really need to test?
One partner is enough if that partner was exposed. Many people with early syphilis don’t know they have it because symptoms can be mild or painless. Testing isn’t a statement about trust; it’s a way to remove uncertainty. Plenty of monogamous people discover infections through routine screening, not because someone cheated, but because someone didn’t know.
3. I had sex two weeks ago and I’m spiraling. Is it too early to test?
Two weeks is often early for a blood test to turn positive. Syphilis antibodies usually show up between three and six weeks after exposure. If you test now and it’s negative, that doesn’t automatically mean you’re clear, it may just mean your immune system hasn’t fully responded yet. A follow-up test around six weeks gives you a more confident answer.
4. What does early syphilis actually look like in real life?
Sometimes it’s dramatic. Often it’s not. A small sore that doesn’t hurt. A rash that looks like dry skin. Swollen glands you blame on stress. Then it fades. The quietness is what makes it tricky. Many people dismiss the first sign because it doesn’t feel urgent, and by the time they think about it again, the stage has changed.
5. If the sore went away, does that mean I’m fine?
Unfortunately, no. A disappearing sore can mean the infection moved to the next stage, not that it resolved. Syphilis is notorious for this. It enters a latent phase where you feel completely normal, but the bacteria are still present. That’s why testing matters even if symptoms came and went.
6. Are at-home syphilis tests legit, or am I playing doctor?
You’re not playing doctor. You’re screening. Rapid blood-based tests detect antibodies and are widely used in public health settings. The key is timing. Used within the proper window period, they provide meaningful information. If positive, you follow up for confirmation and treatment. Think of it as the first checkpoint, not the final verdict.
7. I’m pregnant. Should I be worried?
You should be proactive, not panicked. Rising rates among women of reproductive age are why prenatal screening is standard medical practice. Syphilis during pregnancy is treatable, and early treatment is highly effective at protecting the baby. If you’re pregnant and unsure of your status, testing is protective care, for both of you.
8. If I test positive, is this going to ruin my life?
No. That’s fear talking. Early-stage syphilis is treatable with antibiotics, and treatment is highly effective. What matters most is catching it and completing therapy. The emotional weight often feels heavier than the medical reality. Once treated, most people move forward without long-term health consequences.
9. How often should I test if I’m dating casually?
If you have new or multiple partners, every three to six months is a reasonable rhythm for many people. Some test after each new partner. There isn’t one universal rule. The better question is: what level of clarity helps you feel steady instead of guessing? Testing is about building a pattern of awareness, not reacting only when something feels wrong.
10. Why does this epidemic feel like it’s sneaking up on people?
Because perception takes time to catch up with data. The King County study showed transmission expanding before public awareness fully adjusted. Many heterosexual adults simply didn’t see themselves in previous messaging. Now the numbers are telling a broader story. When epidemics evolve, our assumptions have to evolve too.
This Isn’t Panic. It’s Prevention.
The King County study makes one thing clear: the syphilis epidemic is not frozen in time. It is moving through heterosexual networks, affecting women of reproductive age, intersecting with structural vulnerabilities, and reshaping who perceives themselves at risk. Ignoring that shift does not protect anyone. Adjusting to it does.
If you’ve had a recent exposure, if you’re unsure about a past partner, or if you simply want clarity in a changing landscape, testing is proactive care. Explore discreet screening options at STD Test Kits, or consider a focused Syphilis Test Kit for private, blood-based detection aligned with recommended timing. Early answers protect you, and the people connected to you.
How We Sourced This Article: This guide was built around the peer-reviewed study “The Syphilis Epidemic Among Heterosexuals Is Accelerating: Evidence From King County, Washington,” published in Sexually Transmitted Diseases and available through PubMed Central. We contextualized its findings using current CDC treatment guidelines, WHO fact sheets, and additional epidemiologic data on congenital syphilis trends. In total, approximately fifteen sources informed the writing; below are six key references selected for clarity, credibility, and public accessibility. All external links were checked for accuracy and open in a new tab for verification.
Sources
1. The Syphilis Epidemic Among Heterosexuals Is Accelerating: Evidence From King County, Washington
2. CDC – Syphilis Treatment Guidelines
3. World Health Organization – Syphilis Fact Sheet
4. CDC: Syphilis – STI Treatment Guidelines
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist who works on preventing, diagnosing, and treating STIs. He combines clinical accuracy with a direct, sex-positive approach and is dedicated to making sure that accurate testing information is available to people in many different communities..
Reviewed by: [Dr. Lauren Mitchell, MD] | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.