Eye Infection After Sex: Can STDs Infect Your Eyes?
Quick Answer: Herpes in the eye (ocular HSV or herpes keratitis) usually causes a red, painful, light-sensitive eye with tearing and blurry vision. It is treatable with antiviral medication, but early care matters to prevent corneal scarring.
This Isn’t Just “Pink Eye”, And That’s the Problem
Ocular herpes most often shows up as herpes simplex keratitis, an infection of the cornea caused by the herpes simplex virus, usually HSV-1. The same virus that causes cold sores can travel along facial nerves and reactivate in the eye. According to the American Academy of Ophthalmology, HSV is one of the leading infectious causes of corneal blindness worldwide.
What makes this tricky is how ordinary it can look at first. Many people assume it’s allergies, dryness, or bacterial conjunctivitis. A little redness. Some irritation. Maybe mild swelling. It doesn’t announce itself with a neon sign that says “this is HSV.”
But there are differences. And they matter.
People are also reading: Do Men and Women Need Different STD Tests? What Actually Changes (And What Doesn’t)
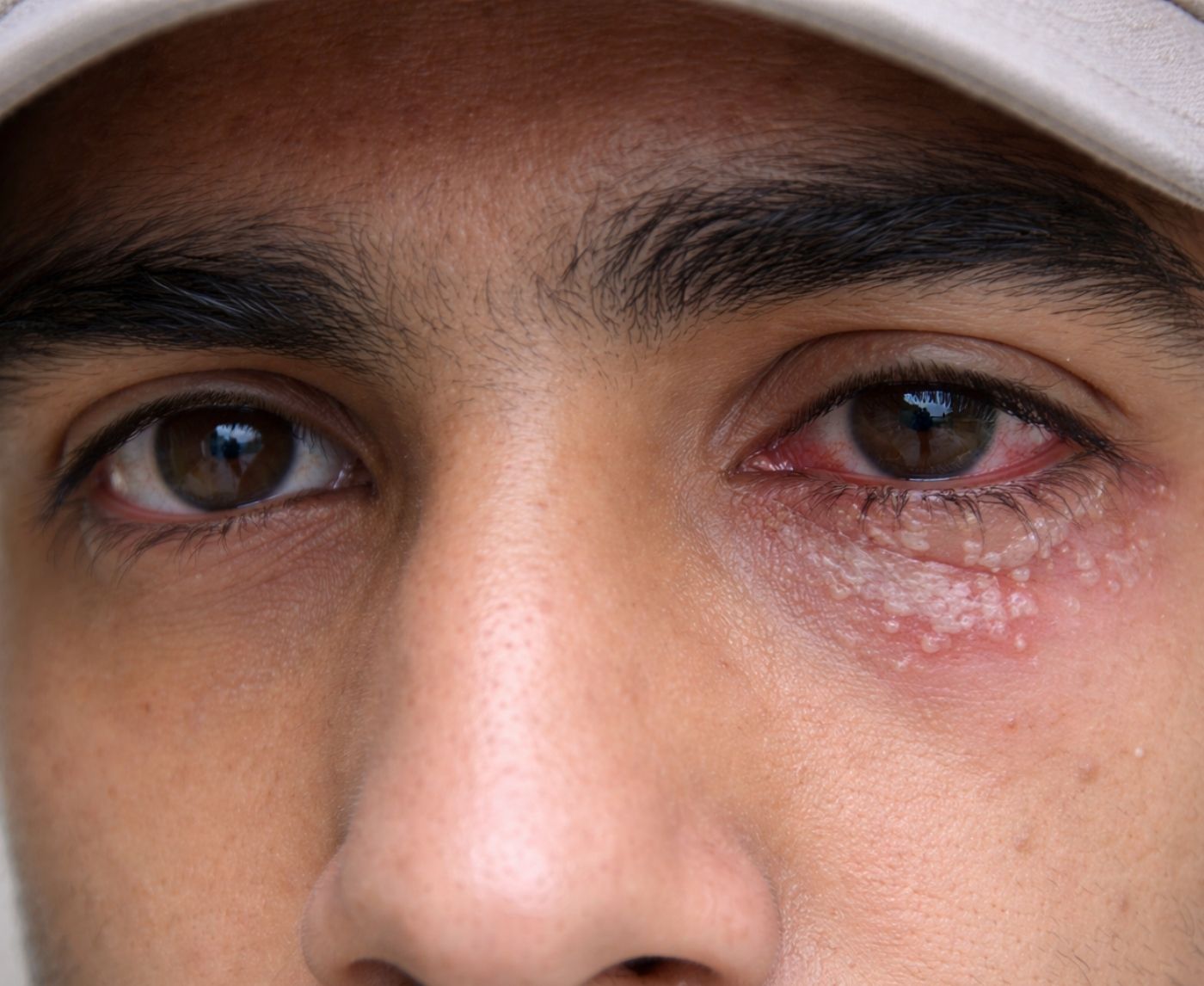
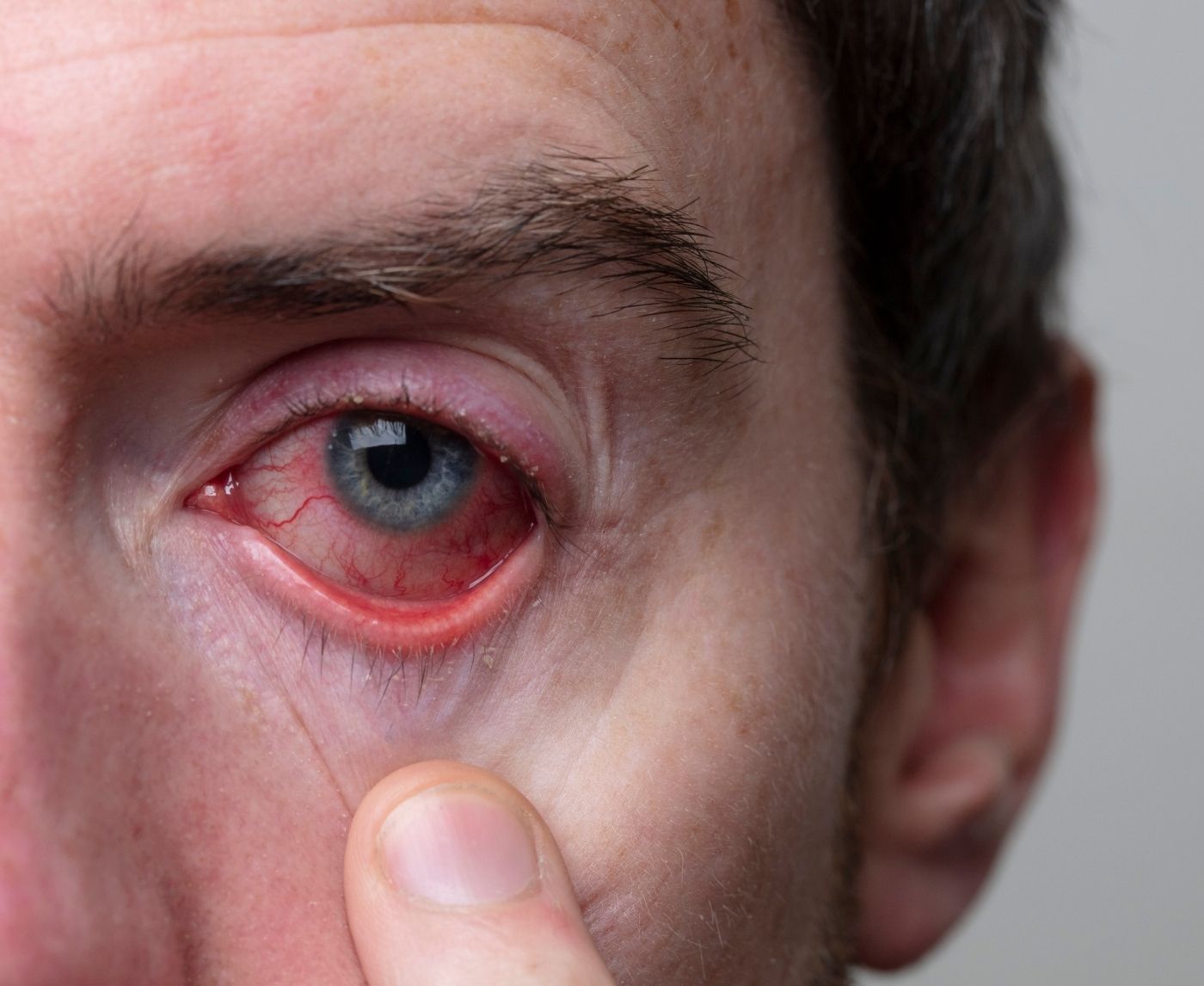
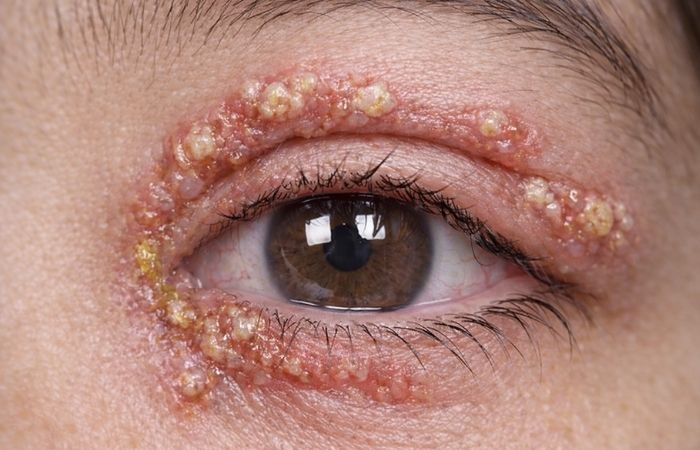
What Herpes in the Eye Actually Looks Like
If you’re Googling “what does ocular herpes look like,” you’re probably scanning your reflection in your phone camera right now. So let’s get specific.
Ocular HSV often affects one eye at a time. The redness may look deeper and more concentrated than typical pink eye. The white of the eye can appear bloodshot, but the pain is often sharper, not just itchy, but gritty, burning, or stabbing.
Many people also describe an intense sensitivity to light. Walking outside feels overwhelming. Screens feel harsh. You may instinctively squint or keep the eye partially closed because light physically hurts.
Table 1. Key differences between ocular herpes and common conjunctivitis.
Another clue doctors look for is something you can’t see at home: a branching, tree-like pattern on the cornea called a dendritic ulcer. This is classic for herpes keratitis, and it’s visible under special dye during an eye exam.
The Symptom That Freaks People Out Most: Blurry Vision
When HSV infects the cornea, it can inflame or damage the surface layer. That’s where the fear ramps up. Because when your vision shifts, even slightly, your brain goes straight to permanence.
Blurry vision with ocular herpes is usually caused by corneal inflammation. In early or mild cases, it often improves with antiviral treatment. According to the Mayo Clinic and NHS guidance on herpes simplex eye infections, prompt antiviral therapy significantly reduces the risk of long-term scarring.
But here’s the part most people don’t hear: many cases resolve without permanent damage when treated early. The word “blindness” gets thrown around online, but severe vision loss is typically associated with repeated untreated recurrences or deep stromal involvement.
Translation? Early action changes outcomes.
How Does Herpes Even Get Into the Eye?
This is where shame tends to creep in. People imagine they “messed up.” They picture some dramatic transmission event. In reality, most ocular HSV cases come from HSV-1, the same virus responsible for oral cold sores, and it often spreads through routine facial contact.
Touch a cold sore. Rub your eye. The virus can transfer. Sometimes the initial infection happened years ago, and what you’re experiencing now is reactivation. HSV lives in nerve cells and can flare during stress, illness, sunlight exposure, or immune shifts.
That means you don’t have to be sexually reckless for this to happen. You don’t have to be promiscuous. You don’t even have to have an active cold sore at the moment of flare. The virus can reactivate silently.
And yes, technically HSV-2 (more commonly associated with genital herpes) can infect the eye, but HSV-1 is the far more common culprit in ocular cases.
Is Eye Herpes Contagious?
This question usually comes from two places: fear of spreading it to someone else, or fear of reinfecting yourself.
During an active outbreak, the virus can be present in tears and on the skin. That means good hygiene matters. Wash hands frequently. Avoid touching the affected eye. Don’t share towels, pillowcases, or makeup. According to public health guidance from the CDC and NHS, HSV spreads through direct contact with infected secretions.
But here’s what it’s not: it’s not airborne. You don’t spread ocular HSV by sitting in the same room. And once the infection is treated and inactive, the risk of transmission drops significantly.
The Part No One Talks About: Recurrence
Ocular herpes has a tendency to come back. Studies published in ophthalmology journals show recurrence rates can approach 30% within the first year after an initial episode. That statistic alone is enough to spike anxiety.
But recurrence doesn’t automatically mean worsening damage. Many recurrences are mild and manageable with antiviral medication. Some people with frequent episodes are placed on suppressive antiviral therapy to reduce flare frequency.
If you’re someone who already lives with oral or genital Herpes, this doesn’t mean you’re destined for eye complications. It means awareness and early care matter.
Where At-Home Testing Fits In
Here’s something important: there isn’t an at-home test specifically designed to diagnose herpes in the eye. Diagnosis typically involves an in-person eye exam, sometimes with laboratory confirmation.
However, if you’re unsure whether you carry HSV-1 or HSV-2 in general, knowing your status can provide context. Discreet at-home blood testing for Herpes antibodies can clarify whether the virus is present in your system. That doesn’t replace eye care, but it can reduce uncertainty.
If you’re navigating questions about HSV overall, you can explore confidential testing options at STD Test Kits. For broader screening, a Combo STD Home Test Kit offers discreet answers without a clinic visit.
Clarity lowers panic. And panic is not a treatment plan.
When to Seek Immediate Care
If you suspect herpes in the eye, this is not a “wait a week and see” situation. Eye infections involving the cornea deserve prompt evaluation by a healthcare provider, ideally an ophthalmologist.
Severe pain, increasing redness, vision changes, or light sensitivity are all signs to seek same-day care. Antiviral eye drops or oral antivirals are most effective when started early. Steroid drops, when appropriate and supervised, may also be used in certain deeper inflammatory cases, but never self-prescribe.
Your vision is not something to gamble with.
“I Thought It Was Allergies”, A Realistic Case Scenario
Rafael, 28, had a history of cold sores since high school. Nothing dramatic. One flare every couple of years during stressful seasons. When his right eye turned red after a long week at work, he blamed screen time and spring pollen.
“It just felt irritated,” he said. “Then two days later, I couldn’t look at my laptop without squinting. The light hurt. That’s when I knew it wasn’t normal.”
He almost waited it out. Almost bought over-the-counter pink eye drops. Instead, he saw an urgent care provider who referred him to an ophthalmologist the same day. Under fluorescent dye, they saw the telltale branching lesion on his cornea, classic herpes keratitis.
Within 24 hours of starting antiviral treatment, the pain began easing. Within two weeks, his vision stabilized. No scarring. No permanent damage. The difference wasn’t luck. It was timing.
How Doctors Diagnose Ocular HSV
If you’re worried about herpes in the eye, diagnosis isn’t guesswork. Eye specialists use specific tools designed to look directly at the cornea. One of the most important is fluorescein dye, a harmless orange stain placed in the eye that glows under blue light.
When HSV infects the surface layer of the cornea, it often creates a dendritic ulcer, a branching pattern that looks like a tiny tree. This is highly characteristic of epithelial herpes keratitis. According to the American Academy of Ophthalmology, this pattern is a key diagnostic feature.
In some cases, especially deeper infections (stromal keratitis), lab testing or PCR analysis may be used to confirm HSV involvement. But many cases are diagnosed clinically based on appearance and symptoms.
Table 2. Forms of ocular HSV and their clinical implications.
Treatment: What Actually Works
Ocular HSV is treated with antiviral medications. These may be topical (eye drops) such as trifluridine or ganciclovir gel, or oral antivirals like acyclovir or valacyclovir. The exact choice depends on severity, depth of infection, and provider judgment.
According to NHS and Mayo Clinic guidance, early antiviral therapy significantly reduces complications. Most uncomplicated epithelial infections improve within one to two weeks. Pain often decreases within several days.
Here’s what does not work: leftover antibiotic drops from a previous pink eye infection. HSV is viral. Antibiotics don’t touch it. Using steroid drops without supervision can actually worsen untreated epithelial HSV.
If inflammation extends deeper into the cornea, supervised steroid therapy may be added carefully alongside antivirals. This is not DIY medicine. This is precision care.
People are also reading: How a Cold Sore Kiss Nearly Blinded a Toddler, and What It Means for Herpes Testing
Can You Go Blind From Herpes in the Eye?
This is the Google search that keeps people awake at night. The honest answer is this: untreated or repeatedly recurrent ocular HSV can cause corneal scarring, which can impair vision. In severe global cases, it is a leading infectious cause of corneal blindness.
But that statistic needs context. In countries with access to antiviral treatment and ophthalmologic care, permanent severe vision loss from a single treated episode is uncommon. The highest risk comes from delayed treatment, repeated uncontrolled recurrences, or deep stromal disease.
So yes, it can be serious. No, it is not automatically catastrophic. The outcome curve bends dramatically with early care.
Why It Comes Back, The Recurrence Cycle
HSV is not eradicated from the body after the first infection. It becomes dormant in nerve cells, typically the trigeminal ganglion for facial infections, and can reactivate later.
Triggers may include stress, fever, illness, sunlight exposure, or immune suppression. Some people experience one ocular episode in their lifetime. Others may have periodic flares.
Long-term suppressive antiviral therapy can reduce recurrence frequency in individuals with repeated episodes. Clinical studies published in ophthalmology journals have shown prophylactic oral antivirals significantly lower recurrence risk during treatment periods.
Recurrence does not mean you did something wrong. It means the virus behaves the way viruses do.
Is This an STD If It’s in My Eye?
This question deserves nuance. Ocular HSV is most often caused by HSV-1, which commonly spreads through non-sexual contact such as kissing in childhood. While HSV is categorized as a sexually transmitted infection when it involves genital transmission, the virus itself is not exclusively sexual.
If you’re worried about whether you carry HSV systemically, blood testing can detect antibodies. That won’t diagnose the eye infection directly, but it can confirm prior exposure.
If you want clarity about your HSV status overall, discreet at-home options are available. You can review confidential testing kits through STD Test Kits, including broader screening like the 6‑in‑1 At‑Home STD Test Kit. Knowing your baseline status reduces guesswork.
How Long Does Ocular HSV Take to Heal?
For uncomplicated infections, symptoms may improve within 7 to 14 days, starting with pain, then redness, and finally, clarity of vision may take a bit longer to settle.
For more serious stromal infections, complete resolution may take weeks to months to achieve, and this may require close follow-up.
The common theme among all medical advice is that early intervention results in faster resolution and lower scarring potential.
What Not to Do If You Suspect Eye Herpes
Do not patch the eye. Do not use random leftover steroid drops. Do not rely solely on internet photos to self-diagnose. And do not ignore worsening light sensitivity or vision changes.
Your eye is not a place for trial-and-error medicine. If something feels deeper than routine irritation, get evaluated. Most urgent care centers can refer to ophthalmology if needed.
You deserve certainty. Not speculation.
How Herpes Spreads to the Eye in Real Life
Let’s make this practical. Most ocular HSV cases are not dramatic medical mysteries. They start with something ordinary. A cold sore. A hand that brushes the lip. A moment of rubbing your eye without thinking.
The herpes simplex virus travels through direct contact. If active viral particles are on your fingers and you touch the surface of your eye, transmission can occur. This is called autoinoculation. It sounds clinical, but it simply means self-transfer.
Sometimes there’s no obvious moment. HSV can reactivate internally along the trigeminal nerve and travel to the eye without you ever touching a cold sore. That’s why people are often confused. They search for the “mistake.” There isn’t always one.
Common Transmission Myths, And What’s Actually True
When fear takes over, myths multiply. So let’s clear the air.
Myth one: you can only get herpes in the eye from sexual contact. Not true. While HSV can be sexually transmitted, ocular HSV is most commonly linked to HSV-1, which many people acquire in childhood through non-sexual contact like kissing relatives.
Myth two: if you’ve never had a visible cold sore, you can’t have ocular herpes. Also false. Many people carry HSV-1 without ever developing noticeable lip lesions. The virus can remain silent for years before a flare.
Myth three: once you touch your eye during a cold sore, blindness is inevitable. That’s fear talking. Transmission risk exists, but immediate catastrophic damage is not the default outcome. Early treatment is protective.
Simple Prevention That Actually Works
Prevention isn’t about paranoia. It’s about routine hygiene during active outbreaks and general awareness if you carry HSV.
During a cold sore outbreak, wash your hands frequently. Avoid touching your eyes. Skip contact lenses if you’re having facial HSV symptoms. Replace eye makeup after an infection to reduce contamination risk.
If you experience recurrent ocular HSV, your provider may recommend suppressive oral antivirals. Clinical research has shown that daily antiviral therapy reduces recurrence frequency in high-risk individuals.
And if you wear contact lenses, be especially mindful. Contacts can irritate the cornea, and inserting or removing them increases hand-to-eye contact. During any suspected eye infection, switch to glasses until evaluated.
The Emotional Layer: Why Eye Symptoms Trigger Panic
Vision is primal. It’s how we navigate the world. When something threatens it, even slightly, the nervous system shifts into alarm mode.
Amina, 34, described it this way: “When my eye went blurry, I didn’t care about the word herpes anymore. I cared about whether I was going to see clearly again.”
That reaction is human. It doesn’t mean you’re dramatic. It means eyesight matters deeply to survival and identity. But panic can distort probabilities. The internet tends to spotlight rare worst-case outcomes instead of typical recovery patterns.
Most treated cases of epithelial herpes keratitis resolve without permanent vision loss. That sentence deserves to be louder online.

People are also reading: Latex Allergy or STD Rash? How to Tell After Sex
Can Ocular HSV Spread to the Other Eye?
It’s possible, but it’s not guaranteed. Good hygiene significantly reduces the chance of spreading infection between eyes. Avoid touching the infected eye and then the healthy one. Wash hands before and after applying medication.
Some people worry that blinking alone will spread it internally. That’s not how it works. Transmission requires viral particles contacting susceptible tissue. It’s not spontaneous migration.
Again, this is about mindful care, not hypervigilance.
Long-Term Management: What Living With It Looks Like
If you’ve had one episode, you may never have another. If you have recurrences, management becomes about reducing frequency and responding quickly when symptoms start.
Many ophthalmologists teach patients to recognize early warning signs: mild eye irritation, subtle redness, or light sensitivity before pain escalates. Starting antivirals early during recurrence can shorten duration.
For people with repeated stromal involvement, long-term suppressive antiviral therapy may be considered. This is especially relevant for individuals who have experienced corneal scarring or vision changes.
Living with HSV, whether oral, genital, or ocular, is about informed vigilance, not fear-based restriction.
When Symptoms Are Not Herpes at All
Not every red, painful eye is HSV. Bacterial conjunctivitis, adenoviral pink eye, allergic conjunctivitis, corneal abrasions, and even contact lens–related irritation can mimic aspects of ocular herpes.
That’s why self-diagnosis through photos is unreliable. The branching dendritic lesion that defines epithelial HSV isn’t visible without special staining.
If you’re unsure, let a professional examine it. Relief comes faster when you’re treating the right cause.
FAQs
1. Okay, but seriously, can herpes in the eye just clear up if I ignore it?
I get the temptation. Your schedule is packed. It’s “just” one eye. But this isn’t a paper cut. Ocular Herpes involves the cornea, and the cornea doesn’t love being inflamed. Some mild cases might calm down, but waiting increases the risk of scarring. If light hurts or your vision shifts even slightly, that’s your cue to get seen, not to tough it out.
2. How do I know it’s not just pink eye?
Great question. Pink eye usually feels itchy or mildly irritated. Ocular HSV often feels sharper, gritty, burning, like something is actually wrong. Light sensitivity is a big clue. If you find yourself squinting indoors or avoiding screens because it physically hurts, that’s not classic pink eye behavior. And blurry vision? That’s a “please get this checked” symptom.
3. I had a cold sore last week. Did I give this to myself?
Maybe. Maybe not. Touching an active cold sore and then rubbing your eye can transmit the virus, that’s called autoinoculation. But sometimes HSV reactivates internally along the facial nerves without you ever touching anything. This isn’t always about a mistake. It’s often just biology doing what biology does.
4. Am I contagious right now?
During an active outbreak, viral particles can be present in tears and on surrounding skin. So yes, there’s some risk. Wash your hands. Don’t share towels. Skip eye makeup. But you are not contagious through air or by sitting near someone. Once treated and healed, the risk drops dramatically.
5. Be honest, can I go blind from this?
Here’s the grounded truth. Untreated or repeatedly severe infections can cause corneal scarring that affects vision. But most people who receive early antiviral treatment recover without permanent vision loss. The internet loves extremes. Real-world medicine loves early intervention. Timing is the difference.
6. Why does this keep coming back?
HSV doesn’t leave the body after the first infection. It settles into nerve cells and can reactivate during stress, illness, or immune shifts. Some people have one episode ever. Others have recurrences. If flares are frequent, daily antiviral medication can significantly reduce how often they happen. Recurrence isn’t failure. It’s virology.
7. Can I still wear contact lenses?
Not during an active infection. Contacts can irritate the cornea and complicate healing. Switch to glasses until your provider clears you. Think of it as giving your eye a break while it repairs itself.
8. Is this considered an STD if it’s in my eye?
Ocular HSV is usually caused by HSV-1, which many people acquire through non-sexual contact in childhood. The virus can be sexually transmitted, but it isn’t exclusively sexual. If you’re unsure of your overall HSV status and want clarity, antibody testing can help, but it doesn’t replace an eye exam for active symptoms.
9. How long before I feel normal again? Many people notice pain easing within a few days of starting antivirals. Redness fades gradually. Vision often stabilizes within one to two weeks for surface infections. Deeper cases can take longer. Healing is not always instant, but it is usually steady with treatment.
10. What’s the one thing I shouldn’t do?
Self-prescribe steroid drops. Steroids can worsen untreated epithelial HSV if used incorrectly. If you suspect herpes in the eye, let a professional guide treatment. Your vision deserves precision, not experimentation.
Before You Spiral, Here’s What Actually Matters
Herpes in the eye sounds terrifying because vision feels sacred. But fear thrives in uncertainty. Ocular HSV is real, it can be serious, and it deserves prompt treatment, but it is also manageable in most cases when caught early.
If your eye is red, painful, or light-sensitive and something feels off, don’t wait. Get evaluated. If you’re unsure about your broader HSV status, get tested. You can explore discreet options through STD Test Kits, including the Essential 6-in-1 At-Home STD Test Kit for comprehensive screening.
How We Sourced This Article: This article will be a combination of clinical information from leading ophthalmological and infectious disease organizations, as well as peer-reviewed studies on herpes simplex keratitis outcomes and relapse rates. A total of fifteen sources were consulted for the creation of this article. The following are six of the most authoritative and accessible sources that were consulted for the creation of the medical claims presented in this article.
Sources
1. NHS – Herpes Simplex Eye Infections
2. What Causes HSV (Herpes Simplex Virus) Keratitis | CDC
3. Herpes Eye Infections: What is Herpes Keratitis? | American Academy of Ophthalmology
4. Herpes Simplex Virus Keratitis: A Treatment Guideline (2014) | American Academy of Ophthalmology
5. Ocular Herpes (Eye Herpes): Symptoms & Treatment | Cleveland Clinic
About the Author
Dr. F. David, an MD, is an infectious disease specialist who is board-certified in the prevention, diagnosis, and treatment of STIs. Dr. David combines accuracy with directness in the prevention, diagnosis, and treatment of STIs, while at the same time expanding access to sexual health information.
Reviewed by: Lauren E. Patel, OD | Last medically reviewed: February 2026
This article is for informational purposes and does not replace medical advice.