Last updated: April 2026
Here's something the healthcare system doesn't make obvious: the biggest financial barrier to STD testing isn't always the cost of the test itself, it's the cost of not knowing your options. People put off testing because they assume it'll be expensive, when in reality they may have access to free or low-cost options they've never heard of, or affordable at-home kits that deliver results without a waiting room, a co-pay, or anything showing up on anyone else's insurance bill.
If cost or privacy has been the reason you haven't gotten tested, this article is for you. Let's break down every option, honestly.

People are also reading: Can You Get Affordable STD Testing Without Insurance in the US?
Why So Many People Skip STD Testing (And Why That's Understandable)
You had a hookup a few weeks ago. Nothing feels obviously wrong, but something is nagging at you. You open a browser and start looking up how much STD testing costs, and within five minutes, you've seen figures ranging from free to $730. You close the tab and tell yourself you'll deal with it later.
That's not a personal failing. That's an entirely rational response to a confusing system. According to research published by the CDC, a significant portion of sexually active young adults delay or skip STD testing because of concerns about cost, privacy, and what might show up on an insurance statement. These aren't excuses; they're real structural barriers that affect millions of Americans every year.
The good news: those barriers are more navigable than most people realize. The US has a genuine patchwork of free, low-cost, and transparent-price testing options, including at-home rapid kits that give results in minutes without involving a doctor, an insurance company, or anyone else. The trick is knowing what those options actually are and when each one makes sense for your situation.
According to provisional data from the CDC's 2024 STI Surveillance Report, more than 2.2 million cases of chlamydia, gonorrhea, and syphilis were reported in the US in 2024, and that figure represents only the infections that were actually tested and reported. The real number is higher because a significant share of infections go undetected simply because people didn't get tested. Cost and access are two of the leading reasons why.
The Real Cost of STD Testing in the US, No Sugarcoating
Before getting into where to go, it helps to understand what you're actually looking at price-wise. The range is enormous, and it's driven by a few key variables: where you go, how many infections you're testing for, and whether you're using insurance.
The hospital ER is never the right move for routine STD screening, not for cost reasons, not for any reason. ERs are designed for emergencies, and showing up there for a chlamydia test will result in a bill that could genuinely ruin your month. That column exists in the table only because people sometimes end up there out of desperation, and it's worth knowing upfront what that desperation costs.
The more relevant comparison for most people is the range between urgent care (expensive, somewhat transparent), public health clinics (cheap or free, but with trade-offs), and at-home testing (fixed price, private, fast), which is why a deeper clinic vs at-home STD testing cost comparison matters before you choose. Each of those options has a real use case depending on your situation, which is what the rest of this article covers.
Free and Low-Cost Clinic Options: What's Actually Available and What to Expect
There's a version of free STD testing in the US that most people don't know exists. It's not a myth, and it's not limited to major cities. The CDC operates a free testing locator at gettested.cdc.gov where you can enter your zip code and find nearby clinics offering free or low-cost STD, HIV, and hepatitis testing. It takes about 30 seconds to use and frequently surfaces options people had no idea were available to them.
Here's what you'll typically find through that tool and others like it:
Public health departments are often the single most affordable option for people without insurance who need affordable STD testing. Many county and city health departments offer STD testing on a sliding scale, meaning what you pay is based on your income. For people below a certain income threshold, testing can be genuinely free. For everyone else, costs are typically a fraction of what a private urgent care clinic would charge. The trade-off is that availability varies by location, and some departments have limited hours or require appointments scheduled in advance.
Planned Parenthood uses a sliding scale pricing model based on income and household size, which means the same panel that might cost $270 at a standard clinic could cost significantly less, or nothing at all, depending on your situation. It's worth calling your local Planned Parenthood directly to ask about self-pay STD testing and what to test for before assuming it's out of reach. The organization explicitly works to make testing accessible, and the conversation is usually more straightforward than people expect.
Community health centers, including Federally Qualified Health Centers (FQHCs), receive federal funding specifically to provide care to uninsured and underinsured patients. These centers are required to offer services on a sliding scale, and in many cases their pricing for STD testing is lower than anywhere else in a given area. The Health Resources and Services Administration maintains a locator at findahealthcenter.hrsa.gov where you can search by zip code.
The honest caveat about free and sliding-scale clinic testing: it works well when you're not in a hurry and you're comfortable with the in-person experience. Wait times can be significant at high-demand locations. Hours are often limited. And some people, particularly young adults on a parent's insurance plan, people in smaller communities, or anyone who's anxious about the in-person dynamic, find the privacy calculus doesn't work in their favor. If any of those describe you, the next section matters more than this one.
The Insurance Privacy Problem: Why Some People Pay Out of Pocket Even When They Have Coverage
Here's something that doesn't get talked about enough: having health insurance doesn't automatically mean you'll use it for STD testing, and for a specific segment of people, using insurance can create a problem that's worse than the cost of paying out of pocket.
When you use insurance for any healthcare service, your insurance company generates a document called an Explanation of Benefits (EOB). This isn't a bill; it's a summary of what was charged and how your plan processed it. And if you're on someone else's insurance plan (a parent's, a spouse's, an employer's group plan), that EOB goes to the policyholder. It often includes the provider name and a description of the service.
Research published in the journal Sexually Transmitted Diseases found that confidentiality concerns around insurance billing are a genuine and documented barrier to STD testing, particularly among young adults who remain on a parent's plan until age 26. One CDC study found that 1 in 8 sexually active teenagers and young adults on a parent's insurance plan said they would avoid seeking sexual health services specifically because they feared their parents would find out.
This isn't paranoia. It's a real structural issue with how insurance billing works. And it explains why a significant number of people who technically have insurance coverage deliberately choose to pay out of pocket for STD testing, either at a cash-friendly clinic or through an at-home kit that bypasses the insurance system entirely. No claim is filed. No EOB is generated. No one else is notified.
If privacy is a factor in your situation, whether that's parents, a partner, or simply a preference to keep your sexual health separate from your employment records, paying out of pocket for a transparent-price option is often the smarter move, not just the more expensive one.
At-Home Rapid STD Test Kits: What They Actually Cost, How They Work, and When They Make Sense
Imagine this: it's 11 PM on a Tuesday, you're thinking about something that happened a few weeks ago, and you've spent the last 45 minutes reading conflicting information online. You don't want to call a clinic. You don't want to explain anything to anyone. You want an answer.
At-home rapid test kits exist precisely for that situation, and in the past several years, the technology behind them has caught up with the clinical setting in meaningful ways. Modern rapid tests use the same immunoassay detection technology used in many clinic-based screenings. When used correctly and within the right testing window, they deliver results that are clinically actionable, not just reassuring guesses.
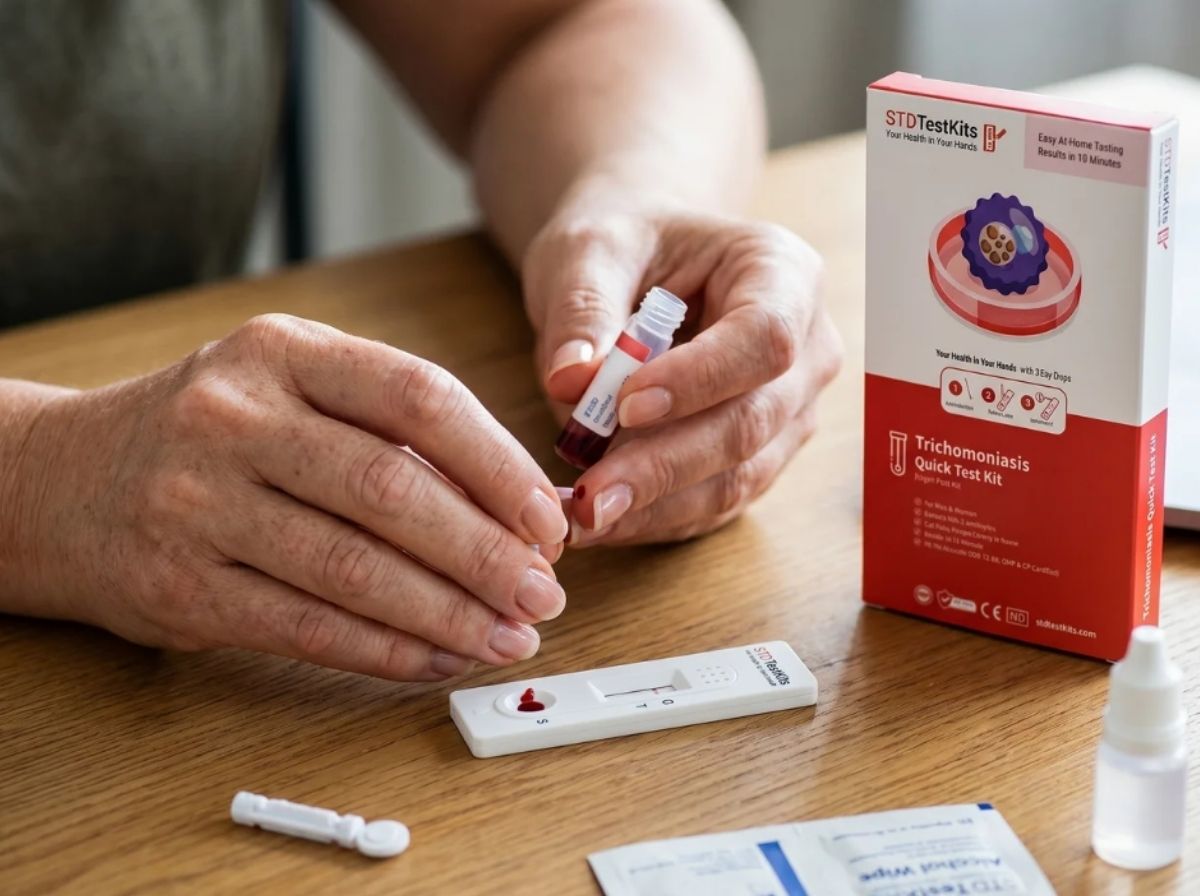
At STD Test Kits, the pricing is transparent and fixed. There are no office visit fees, no lab processing surcharges, and no bill going anywhere but to you. Here's how the kit lineup breaks down:
The pricing model here is fundamentally different from a clinic visit. With a clinic, you're paying for the test, plus the facility overhead, plus a consultation fee plus lab processing. With an at-home kit, you pay for the kit. That's it. No hidden line items, no surprise bill three weeks later, no co-pay ambiguity. For people who have been burned by unexpected medical bills before, that transparency has real value beyond just the dollar figure.
Testing at home also removes the waiting room entirely. The kit arrives in plain, discreet packaging. You collect the sample, follow the instructions, and get your result, often within minutes for rapid formats. No appointment. No time off work. No sitting in a shared space where you might run into someone you know. Taking control of your sexual health is supposed to feel empowering, not like an administrative ordeal.
People are also reading: STD Testing Window Periods: When to Test for Each
When to Test After Exposure: Getting the Timing Right on a Budget
One of the most important things to understand about STD testing, and something that budget-focused guides often skip over, is that the cost of a test matters far less than whether you're testing at the right time. Testing too early after an exposure can produce a false negative, not because the test is inaccurate, but because the infection hasn't yet reached detectable levels in your system. Every STD has what's called a window period, and testing before that window closes can give you a false sense of reassurance.
This is especially relevant for people trying to minimize costs. If you test too early and get a negative result, you may either stop worrying (incorrectly) or need to test again, paying twice when once would have been enough. Testing at the right time means one test, one clear answer.
Here are the exact window periods to use as your guide:
A practical note: if you're in the window period and genuinely anxious right now, that's understandable, but testing today won't give you a reliable answer. Mark the date when your window period closes, set a reminder, and test then. A clear result at the right time is worth far more than an inconclusive one taken too early. If you're experiencing symptoms in the meantime, that changes the picture; symptoms warrant a clinical evaluation regardless of the testing timeline.
Is At-Home Testing as Reliable as a Clinic? The Honest Answer
This is probably the question that holds more people back from at-home testing than the price ever does. And it deserves a direct answer rather than the defensive hedging that a lot of product pages retreat into.
At-home rapid tests use immunoassay technology, the same foundational method used in clinical settings for many common STD screenings. The accuracy figures for well-manufactured rapid tests are genuinely high. The STD Test Kits lineup, for example, runs at 98%–99%+ accuracy depending on the specific test. That's not a marketing number; it reflects the sensitivity and specificity of the underlying test format when used correctly.
The variable that most affects at-home test accuracy isn't the technology; it's sample collection. A swab collected incorrectly, a test administered before the window period closes, or a blood sample that's insufficient can all affect results. This is why reading the instructions carefully matters more than most people expect it to. The kit is doing its job correctly if you're doing your part correctly. Instructions exist for a reason.
The scenario where a clinical test has a meaningful accuracy advantage is in the detection of infections with more complex biological presentations, certain herpes cases, for instance, where a provider might use a swab of an active lesion combined with a blood test for the most complete picture. For most common STD screenings for people without active symptoms, a quality at-home rapid test gives you a reliable, clinically meaningful result.
What a positive result from an at-home kit means in practice: it's a strong signal that warrants follow-up with a healthcare provider for confirmatory testing and treatment. A positive result doesn't replace a clinical relationship; it starts the conversation with one. What it gives you first is clarity on whether that conversation is necessary.
How to Think About the Cost vs. the Cost of Not Testing
There's a financial argument for regular STD testing that almost never gets made clearly, so let's make it here.
Untreated chlamydia, the most commonly reported bacterial STD in the US, can progress to pelvic inflammatory disease (PID) in women, a condition that carries treatment costs measured in thousands of dollars and can result in lasting fertility complications. Untreated gonorrhea can cause epididymitis in men and PID in women, with similar downstream costs. Untreated syphilis progresses through stages that eventually become significantly more complex and expensive to manage than the antibiotic course that would have resolved it in the early stage.
The math here isn't subtle. A single-infection test that catches something early costs a fraction of what treatment for an advanced or complicated infection costs. And the non-financial costs, the health impact, the partner notification conversation, and the time lost, aren't minor either.
The CDC has explicitly identified expansion of at-home rapid testing as a public health priority precisely because access barriers, cost, clinic hours, embarrassment, and insurance concerns result in delayed detection that makes infections harder and more expensive to manage. Testing early, testing accurately, and testing at the right time after exposure is the cheapest version of STD healthcare that exists.
If cost is genuinely the barrier, the lowest-cost path forward is usually a targeted single-infection test if you have a specific exposure concern, or a combination kit if you want a broader picture without paying clinic prices for each individual test. Either way, the cost of testing is almost always less than the cost of not testing.

People are also reading: STD Risk Checker Quiz: Do You Need to Get Tested?
Practical Steps: How to Get Tested Based on Your Situation
Not every path to STD testing looks the same, and the right one for you depends on a few specific factors: how much privacy you need, how quickly you want results, what your actual budget looks like, and whether you have a specific infection concern or want a broader screening.
If privacy is your top concern, an at-home rapid kit is the cleanest option. It arrives in plain packaging, the process happens entirely at home, and nothing is filed with any insurance company or shows up in any medical record. The STD Test Kits homepage walks through available options clearly, and you can select the panel that matches what you actually need to test for. Start with the combo kits if you want to test for the two most common infections together; the Chlamydia & Gonorrhea 2-in-1 is the logical entry point for most people with a general exposure concern.
If cost is the absolute top constraint, use the CDC's free clinic locator at gettested.cdc.gov to find public health department testing in your zip code. Call ahead to ask about sliding-scale pricing and whether you qualify. If you're a student, check whether your campus health center offers discounted or free STD testing, many do, and it's consistently underused. Planned Parenthood is also worth a call regardless of your income level; pricing is adjusted based on what you can actually pay.
If you want results fast and don't want the in-person experience, An at-home rapid test gives you results in minutes. There's no scheduling, no waiting room, no explaining yourself to anyone. If your window period has passed and you're in a position to test today, a kit ordered through STD Test Kits delivers to your door with everything needed to collect your sample and read your result without any additional steps or people involved.
If you're symptomatic: Symptoms change the equation. If you're experiencing discharge, sores, burning during urination, or other physical signs of a possible infection, a clinical evaluation is the appropriate first step, not because at-home testing is unreliable, but because symptoms sometimes require an in-person assessment to determine what's actually happening. Use gettested.cdc.gov to find an affordable local option, or contact a community health center about same-day or urgent appointments. An at-home test can still be useful in parallel, but a provider should see active symptoms.
FAQs
1. How much does STD testing cost without insurance?
It depends entirely on where you go and what you're testing for. A single-infection test at a public health clinic can be free or close to it on a sliding scale. The same test at a private urgent care clinic runs $80–$185 before any facility fees. A full panel at an urgent care center without insurance can reach $200–$400. At-home rapid kits offer fixed, transparent pricing with no surprise charges; what you pay is what you see before you order.
2. Will STD testing show up on my parents' insurance bill?
If you use your parents' insurance plan for any covered healthcare service, the insurance company typically sends an Explanation of Benefits (EOB) to the policyholder that details the service. The safest way to avoid this is to pay out of pocket, either at a cash-friendly clinic or through an at-home kit that bypasses the insurance system entirely. No claim, no EOB, no notification.
3. Are at-home STD tests as accurate as clinic tests?
For the most common bacterial infections, chlamydia, gonorrhea, and syphilis, quality at-home rapid tests deliver accuracy rates of 98%–99%+ when used correctly and within the right testing window. The main variable that affects home test accuracy is sample collection technique, not the technology itself. Following instructions carefully is the part that matters most.
4. Can I get free STD testing in the US?
Yes, genuinely. The CDC's GetTested tool at gettested.cdc.gov lists free and low-cost testing locations by zip code. Public health departments, community health centers, and many Planned Parenthood locations offer sliding-scale or free testing for people who qualify based on income. Free options are more widely available than most people realize; the barrier is usually awareness, not availability.
5. What's the cheapest STD test I can get for chlamydia specifically?
Chlamydia is one of the more affordable single-infection tests, whether you go through a clinic or test at home. At public health departments, it can be free or under $30 on a sliding scale. At-home single-infection chlamydia kits are similarly affordable and give results at home without any clinical visit involved. The key is testing from 14 days after exposure, earlier than that, and you risk a false negative regardless of which option you choose.
6. What happens if I test positive on an at-home STD kit?
A positive result means you need to follow up with a healthcare provider for confirmatory testing and to discuss treatment options. Most bacterial infections caught early respond well to treatment, and your provider can guide you through the next steps. An at-home positive result isn't a crisis; it's information, and information is what makes the next steps straightforward instead of complicated.
7. Can I use an HSA or FSA card to pay for at-home STD tests?
In many cases, yes. Health Savings Account (HSA) and Flexible Spending Account (FSA) funds can be used for medical testing products, including STD test kits. Check with your specific account provider to confirm eligibility for the product you're purchasing, as coverage can vary depending on plan type.
8. How do I know which STD test kit is right for me?
Start with what you actually need to know. If you had a specific exposure and want to check for the two most common bacterial infections, the Chlamydia & Gonorrhea 2-in-1 kit is the logical starting point. If you want broader peace of mind after an encounter where you're unsure about risk, the 7-in-1 or 8-in-1 panel covers the most clinically relevant infections comprehensively. If you're a woman who wants the most complete screening available in one kit, the Women's 10-in-1 covers everything, including trichomoniasis and HPV.
9. Is it safe to test at home for HIV?
Yes. The HIV test in STD Test Kits' combo panels uses the same antibody/antigen detection approach used in clinical settings and delivers 99%+ accuracy after the 6-week window period. For HIV specifically, the window matters: test at 6 weeks for a first indicator, and retest at 12 weeks if you want a fully conclusive result. Testing too early, in the first few weeks after a potential exposure, is where false negatives happen, not because the test is inadequate but because the biology hasn't developed to a detectable level yet.
10. What if I can't afford to get tested at all right now?
Don't wait and hope for the best. Use gettested.cdc.gov to find free options near you. This is what that resource exists for, and it frequently lists options people had no idea were available in their area. Public health departments, LGBTQ+ health centers, university clinics, and community health centers all offer low-cost or free testing for people who genuinely can't pay. Getting tested for free is always better than not getting tested at all.
Get Tested on Your Terms, Without the Clinic Price Tag
Cost should never be the reason someone skips STD testing, but it is, for a significant number of people, every single day. The goal of this guide has been to make the actual landscape clearer: there are genuinely free options if you know where to look, there are sliding-scale clinics priced based on what you can actually pay, and there are at-home rapid kits that offer clinic-grade accuracy with complete privacy and no surprise billing.
If you're ready to test at home, the Chlamydia & Gonorrhea 2-in-1 At-Home STD Test Kit is the right starting point for most people dealing with a general bacterial exposure concern, the two infections it covers are the most commonly reported STDs in the US. For broader coverage, the 7-in-1 Complete At-Home STD Test Kit screens for seven of the most clinically relevant infections at a price point that's typically well below what a comparable panel would cost at an urgent care center. And for women who want the most comprehensive single-kit option available, the Women's 10-in-1 At-Home STD Test Kit covers ten infections including trichomoniasis and HPV strains 16 and 18.
All kits ship in discreet packaging, results are yours and no one else's, and pricing is fixed, no insurance required, no EOB generated, no waiting room involved. Visit STD Test Kits to find the right kit for your situation and take control of your sexual health on your own timeline.
How We Sourced This: Our article was constructed based on current advice from the most prominent public health and medical organizations, and then molded into simple language based on the situations that people actually experience, such as treatment, reinfection by a partner, no-symptom exposure, and the uncomfortable question of whether it "came back." In the background, our pool of research included more diverse public health advice, clinical advice, and medical references, but the following are the most pertinent and useful for readers who want to verify our claims for themselves.
Sources
1. CDC, Sexually Transmitted Infections Surveillance, 2024 (Provisional)
2. CDC, GetTested: HIV, STI & Viral Hepatitis Testing Locator
3. PMC / Sexually Transmitted Diseases, Insurance and Healthcare Access Barriers to STD Testing
4. Planned Parenthood, Does Getting Tested for STDs Cost Money?
5. PMC / NCBI, Updates on Testing, Treatment, and Prevention of STIs in the United States, 2025
6. HRSA, Federally Qualified Health Centers (FQHCs)
About the Author
Dr. F. David, MD is a board-certified infectious disease specialist focused on STI prevention, diagnosis, and treatment. He writes with a direct, sex-positive, stigma-free approach designed to help readers get clear answers without the panic spiral.
Reviewed by: STD Test Kits Medical Review Team | Last medically reviewed: April 2026
This article is for informational purposes and does not replace medical advice.





